 RUSLAN DASHINSKY/ ISTOCK/GETTY IMAGES PLUS
RUSLAN DASHINSKY/ ISTOCK/GETTY IMAGES PLUS
Supporting Oral Health in Pregnancy
Providing dental care to pregnant patients is both safe and necessary to ensure the health of both mothers and infants.
This course was published in the February 2017 issue and expires February 2020. The author has no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- List the factors that influence oral health during pregnancy, and those affecting patient comfort while receiving dental care.
- Identify common oral conditions experienced by pregnant patients, and the need for preventive care and treatment.
- Discuss the transmission of cariogenic bacteria from mother to child, and adjunctive methods for maintaining oral hygiene during pregnancy.
- Explain when national guidelines for oral health care during pregnancy were issued, and when medical clearance is needed before providing oral health services to this patient population.
INCREASED RISK FOR ORAL DISEASES
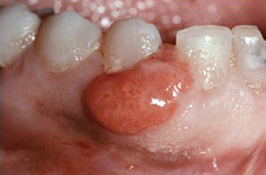
Pregnant women experience an increase in progesterone and estrogen, which exacerbates the inflammatory response to gingival irritants, such as plaque biofilm. Simultaneously, changes in the oral microflora favor the pathogens associated with gingivitis.1 As a result, pregnant women are more susceptible to gingivitis, pregnancy granuloma, periodontal diseases, and dental caries.
Gingivitis is a common oral condition that affects up to 75% of pregnant women.1,2Increased levels of estrogen and progesterone, changes in the oral flora, and a weakened immune system affect gingival tissue and cause inflammation. Poor oral hygiene and increased biofilm can exaggerate the gingival response. Pregnant women may experience gingivitis beginning in the second month and continuing throughout pregnancy. Although the severity may improve post-partum, most women who experience gingivitis during pregnancy will likely have some form of the disease after pregnancy.1,2
The hormonal changes that occur during pregnancy increase a women’s susceptibility to periodontal pathogens and reduce the body’s ability to repair oral soft tissues.3 Periodontal diseases have been associated with adverse pregnancy outcomes.4 Studies have shown an association between periodontal diseases and preterm birth, development of preeclampsia, and delivery of low-birth-weight infants.3,5–7
Poor periodontal health has been linked to chronic systemic conditions, including diabetes, cardiovascular diseases, and respiratory diseases.5,8 Pregnant women experience increases in cardiac output and blood volume, and changes in the respiratory system—all of which increase their risk for these diseases.7 For pregnant women with diabetes, excellent oral heath is critical because periodontal diseases can make diabetes more difficult to control.8 Furthermore, as the degree of uncontrolled diabetes increases, so does the risk for congenital anomalies in the fetus.9
Changes in the oral environment during pregnancy can increase the risk for caries.10 Pregnant women tend to crave a diet high in sugar and fermentable carbohydrates, increasing the risk for caries. In addition, many pregnant women experience nausea and vomiting, which can compromise oral hygiene efforts. Vomiting also increases acidity in the oral cavity. At later stages of pregnancy, the upward pressure from an expanding uterus may cause acid reflux.11 This type of acidic environment favors cariogenic bacteria and can also cause erosion. Additionally, cariogenic Streptococcus mutans passes from mother to infant through vertical transmission.11,12 The bacterium is transferred by sharing utensils or toothbrushes, kissing on the lips, cleaning a dropped pacifier by mouth, or the prechewing of food. Pregnant women with untreated caries have high levels of S. mutans in their saliva and are thus likely to pass the bacteria onto their offspring. Children who acquire the bacterium at an early age have a greater risk of developing early childhood caries.11,12
INTERPROFESSIONAL COLLABORATION
In 2006, the New York State Department of Health released evidence-based prenatal oral health guidelines.13 In 2010, the California Dental Association, together with the American College of Obstetricians and Gynecologists, revised their guidelines.11 In 2012, national guidelines were released in a collaboration between the federal Health Resources and Services Administration’s Maternal and Child Health Bureau, American College of Obstetricians and Gynecologists, and the American Dental Association.14 These guidelines, Oral Health Care During Pregnancy: A National Consensus Statement, provide information designed to improve oral health services to women during pregnancy. They clearly state that providing preventive, diagnostic, and restorative oral care during pregnancy is safe, effective, and recommended.14
The new guidelines seek to strengthen interprofessional collaboration between prenatal and oral health professionals. The prenatal health professional typically sees the pregnant patient first, and is often the only clinician to see the patient. During the first prenatal visit, women should be encouraged to schedule an oral examination. Prenatal practitioners should provide an oral assessment and make the necessary referrals to oral health care teams.
The success of any guidelines depends on consistent implementation and adherence by all clinicians, and an ongoing, collaborative relationship between prenatal and oral health professionals. Barring any significant health issues, there is no need to obtain medical clearance from a prenatal practitioner before providing oral care to a pregnant patient. In an effort to facilitate an easier referral process, however, prenatal health professionals can give patients a written “communication” form to bring to the dental office.11 This serves as both a referral form and tool to facilitate information sharing among all caregivers. After treatment is rendered, the form can be completed by the oral health care team and faxed back to the prenatal clinician. Click here to view a sample oral health clearance form for pregnant women.
BARRIERS TO CARE
Despite the importance of oral health during pregnancy, approximately 22% to 34% of women seek care during pregnancy.10 One reason is that the provision of oral health care during pregnancy is often misunderstood by patients, as well as prenatal and oral health professionals. As a result, medical practitioners may not refer patients for oral care. In addition, dental teams may choose to delay treatment until after delivery due to concerns about the safety of dental procedures.11,15 Kloetzel et al15 noted that less than half of the women surveyed about perceptions of dental care said their obstetricians had advised them to seek dental care during pregnancy.
Although the most common reason cited for not seeking care is lack of perceived need, research shows access to care also plays a role.11 The likelihood of low-income and uninsured women receiving such care is even lower. A California study found that fewer than one in five pregnant women enrolled in Medicaid received dental services.11 For many low-income women, pregnancy is the only time they may have dental coverage. Oral health coverage for pregnant women varies by state, although states must cover pregnancy-related services. This means Medicaid-eligible pregnant women must receive oral health services if the oral condition is exacerbated by the pregnancy or could negatively impact the pregnancy.16
Moreover, pregnancy is a time when women tend to be motivated to make healthy choices. Compared to uninformed patients, women who are educated about oral health needs during pregnancy are more likely to establish improved oral care habits for themselves and their offspring.16
Access to care may also be hindered by low oral health literacy and language barriers. All health professionals should ensure patients understand the information presented and are given the opportunity to ask questions.14
PROVIDING TREATMENT
The Oral Health Care During Pregnancy: A National Consensus Statement declares that comprehensive oral care—including necessary radiographs and use of approved local anesthesia—are beneficial during pregnancy and pose no fetal or maternal risk.14Furthermore, treatment can be safely rendered any time during pregnancy, although pregnant women may be most comfortable being treated in the second trimester. Pregnant women may experience nausea and vomiting in the first trimester and any manipulation of oral tissues may worsen the symptoms.
During the third trimester, women experience increased cardiac output, which, along with a growing uterus, may compress the inferior vena cava, especially when in the supine position.7 Consequently, pregnant patients may experience heart palpitations, dizziness, nausea, or hypotension, known as supine hypotension syndrome. To prevent supine hypotension syndrome, the clinician should keep the patient’s head at a higher level than her feet. Additionally, having the patient tilt slightly to her left and placing a pillow or rolled towel under her right hip can help prevent hypotension.7
As with any patient, a thorough medical and dental history should be taken, including the use of tobacco, alcohol, and drugs. Assessments should include a complete head, neck, and intraoral examination; caries risk assessment; and a periodontal exam. Radiographs should be taken when indicated, following the As Low As Reasonably Achievable principle of minimizing radiation exposure, and using a lead apron with a thyroid collar.14 Digital radiographs offer the least amount of radiation, which can be further reduced with a rectangular collimator.14 Based on the clinician’s assessment, a comprehensive treatment plan that includes preventive, restorative, and periodontal treatment can be formulated.
A tobacco cessation program should be offered to pregnant women who use tobacco. Women are more apt to quit smoking during pregnancy than during other times in their lives. Pregnant women who smoke may have an increased risk for ectopic pregnancy, spontaneous abortion, and low birth-weight/preterm babies. Infants exposed to second-hand smoke are at higher risk for respiratory illness, middle ear infections, asthma, and sudden infant death syndrome. A high incidence of caries in the primary dentition has also been associated with children who are exposed to second-hand smoke.17
A healthy diet rich in nutrients is necessary for both the pregnant woman and the fetus. Patients should be advised to eat a balanced diet rich in folate, protein, calcium, phosphorus, and vitamins A, B6, B12, C, and D.11,18 Pregnant women should be encouraged to take prenatal vitamins, including folic acid, to reduce the risk of birth defects, such as cleft lip and cleft palate.14 Clinicians should advise these patients to minimize their intake of sugary foods and starches. When sugary foods and starches are consumed, it is best to have them with a nutritious meal, as this will help buffer the acidity and decrease the likelihood of demineralization. Pregnant women should also be cautioned to limit their consumption of sweetened beverages, such as fruit juice, sports drinks, and soda, as these drinks can contribute to caries. Additionally, diet soda should be avoided, as the acidity could cause erosion and provides a favorable environment for cariogenic bacteria.
Pregnant women should have untreated caries restored because lesions will likely worsen. Additionally, caries control has the potential to reduce the mother’s cariogenic bacterial load, thereby preventing the transmission of pathogenic microorganisms from the mother to the infant. Dental materials—including amalgam, composite, and endodontic material—can be used safely and effectively.14 A rubber dam and high-speed evacuation should be used to prevent inhalation of dental material vapor, such as amalgam.14
Periodontal therapies, including scaling and root planing, are safe and effective during pregnancy.19 The American Academy of Periodontology recommends periodontal therapy be provided as early in the pregnancy as possible to reduce the pathogen load and prevent infections.19
ORAL HYGIENE INSTRUCTION
Good oral hygiene is essential during pregnancy. Women should be encouraged to brush twice daily with fluoride toothpaste, and use floss or an alternative interproximal cleaning method daily. In addition, pregnant women with high caries risk should use an alcohol-free, fluoride mouthrinse twice daily.14 Rinsing with an alcohol-free 0.12% chlorhexidine formula and 0.05% sodium fluoride reduces the cariogenic bacterial load. Using xylitol-containing products two to three times daily is also recommended.14 Although women should be encouraged to drink fluoridated water,14 systemic consumption of fluoridated water chiefly benefits the pregnant mother, as only trace amounts of fluoride reach the fetus.20
Patients who experience vomiting or gastric reflux should avoid brushing immediately after these incidents due to increased risk of erosion and caries. Pregnant women should rinse with a teaspoon of baking soda dissolved in a cup of water to neutralize the acids before brushing their teeth.10
IMPLEMENTING APPROPRIATE PAIN CONTROL MEASURES
Pregnant patients may experience increased anxiety, which may lower their pain threshold. Therefore, clinicians should manage pain with approved topical and local anesthetics (Table 1)14 and keep appointments short. A recent study by Hagai et al21 indicates the use of local dental anesthetics is safe and poses no risk to the fetus. Because of the risk for hypoxia, hypotension, and aspiration, however, consulting with the patient’s obstetrician is recommended prior using inhalation analgesics, such as nitrous oxide.14

CONCLUSION
Providing oral health care during pregnancy is safe and necessary for the mother and her developing fetus. Seeking care early will not only help prevent oral health problems, it can also reduce the risk of systemic diseases. Mothers who have received oral care during pregnancy are more likely to seek continued care for themselves and their infants.22 Modifying the attitudes and beliefs of patients and health care providers is essential in the effective promotion of preventive oral care.
REFERENCES
- Steinberg BJ. Women’s oral health issues. J Calif Dent Assoc. 2000;28:663–667.
- Steinberg BJ, Hilton IV, Iida H, Samelson R. Oral health and dental care during pregnancy. Dent Clin N Am. 2013;57:195–210.
- Boggess KA, Edelstein BL. Oral health in women during preconception and pregnancy: Implications for birth outcomes and infant oral health. Matern Child Health J. 2006;10(Suppl 1):169–174.
- Lieff S, Boggess KA, Murtha AP, et al. The oral conditions and pregnancy study: periodontal status of a cohort of pregnant women. J Periodontol. 2004;75:116–126.
- Boggess KA, Society for Maternal-Fetal Medicine Publications Committee. Maternal oral health in pregnancy. Obstet Gynecol. 2008;111:976–986.
- Han YW, Oral health and adverse pregnancy outcomes—What’s next? J Dent Res. 2011;90:289–293.
- López NJ, Gómez RA. Dental and medical comanagement of pregnancy. In: Periodontal Disease and Overall Health: A Clinician’s Guide. Genco RJ, Williams RC, eds. Yardley, Pa: Professional Audience Communication Inc; 2010:250–267.
- Allston A. Improving Women’s Health and Perinatal Outcomes: The Impact of Oral Diseases. Available at: jhsph.edu/research/centers-and-institutes/womens-and-childrens-health-policy-center/publications/oralbrief.pdf. Accessed January 23, 2017.
- Centers for Disease Control and Prevention. Check Your Knowledge: Diabetes and Pregnancy. Available at: cdc.gov/features/diabetespregnancy/. Accessed January 23, 2017.
- Silk H, Douglass AB, Douglass JM, Silk L. Oral health during pregnancy. Am Fam Physician. 2008;77:1139–1144.
- California Dental Association Foundation, American College of Obstetricians and Gynecologists, District IX. Oral health during pregnancy and early childhood: evidence-based guidelines for health professionals. J Calif Dent Assoc. 2010;38:391–403, 405–440.
- American Academy of Pediatric Dentistry. Guideline on Perinatal Oral Health Care. Available at: aapd.org/media/policies_guidelines/g_perinataloralhealthcare.pdf. Accessed January 23, 2017.
- New York State Department of Health. Oral Health Care During Pregnancy and Early Childhood: Practice Guidelines. Available at: health.ny.gov/publications/0824.pdf. Accessed January 23, 2017.
- Oral Health Care During Pregnancy Expert Workgroup. Oral Health Care During Pregnancy: A National Consensus Statement. Available at: mchoralhealth.org/PDFs/OralHealthPregnancyConsensus.pdf. Accessed January 23, 2017.
- Kloetzel MK, Huebner CE, Milgrom P. Referrals for dental care during pregnancy. J Midwifery Womens Health. 2011;56:110–117
- National Health Law Program. Dental Coverage for Low-Income Pregnant Women. 2012. Available at: healthlaw.org/issues/reproductive-health/dental-coverage-for-low-income-pregnant-women#.WIb1UoU41S4. Accessed January 23, 2017.
- American Academy of Pediatric Dentistry, Council on Clinical Affairs, Committee on the Adolescent. Guideline on oral health care for the pregnant adolescent. Pediatr Dent. 2012;34:153–159.
- U.S. Department of Health and Human Services, National Institutes of Health, Office of Dietary Supplements. Nutrient Recommendations: Dietary Reference Intakes (DRI). Available at: ods.od.nih.gov/Health_Information/Dietary_Reference_Intakes.aspx. Accessed January 23, 2017.
- Task Force on Periodontal Treatment of Pregnant Women. American Academy of Periodontology statement regarding periodontal management of the pregnant patient. J Periodontol. 2004;75:495.
- Patsouri K. Re-Examining the fluoride intake during pregnancy: A necessity or not for the incoming member. Int J Dent Med Res. 2015;1:150–156.
- Hagai A, Diav-Citrin O, Shechtman S, Ornoy A. Pregnancy outcome after in utero exposure to local anesthetics as part of dental treatment: A prospective comparative cohort study. J Am Dent Assoc. 2015;146:572–580.
- Curtis M, Silk HJ, Savageau JA. Prenatal oral health education in U.S. dental schools and obstetrics and gynecology residencies. J Dent Educ. 2013:77:1461–1468.
From Dimensions of Dental Hygiene. February 2017;15(2):46-49.



