
Multifaceted Magnification
The same ergonomic tools used by dental hygienists to improve visual acuity may also help patients strengthen their self-care regimens.
The introduction of magnification and illumination has transformed dental hygiene by enabling clinicians to practice more ergonomically. These same aids may also help patients become more effective in their self-care regimens. The ergonomic benefits of using magnification while providing oral care are widely known.1–4 Several studies have been conducted on the use of loupes by dental and dental hygiene students while providing dental services, all of which found that their use provided significant ergonomic benefits—particularly in the maintenance of good posture.5–7 The outcomes of these studies suggest that requiring the use of magnifying lenses in educational programs may be justified, though additional studies are warranted. Nonetheless, the benefits of loupes and lighting are important components of an ergonomic approach to improving posture and reducing musculoskeletal disorders among oral health professionals— especially dental hygienists.1,3,8
The use of loupes with coaxial illumination assists clinicians with maintaining neutral posture—one of the primary ergonomic principles.8 Neutral posture for the upper body includes keeping the head upright, shoulders relaxed, elbows flexed at 90°, and wrists and back straight. Clinicians who use forward head flexion or awkward trunk postures can develop fatigue, rounded shoulders, and muscle disorders in the arms and hands.8,9 In addition to selecting comfortable loupes with a lightweight frame, the most important ergonomic factor to consider when using loupes is the declination angle, or the angle the eyes assume while looking into the oral cavity.1 Establishing this angle is crucial to mitigating neck and shoulder strain.
Coaxial illumination systems, or headlights, are frequently used in conjunction with loupes to improve the amount and direction of light in the clinician’s field of view. This type of headlight provides shadow-free illumination that, in turn, minimizes awkward positioning and excessive bending of the neck.1,3 Coaxial illumination produces light that is parallel to the clinician’s line of sight, thus minimizing the need to adjust the overhead light. Furthermore, headlight illumination can be especially helpful for dental professionals older than 40, who, like their older patients, may benefit from increased lighting when performing detailed tasks.10
PATIENT BENEFITS
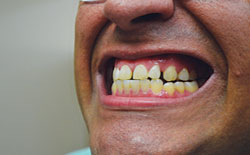
Clinicians aren’t the only ones who benefit both ergonomically and visually from magnification and illumination. There are also clear advantages for patients who utilize these modalities—namely, improved visual acuity when performing oral hygiene self-care. Visual enhancement is of special concern for the estimated 72 million to 79 million baby boomers (age 49 to 67) in the United States, who may see a decline in their ability to see as they age.10 Age-related decline in vision can affect patients’ abilities to perform everyday visually related tasks.11,12 The inability to see, read, and decipher words or images up close due to age is called presbyopia. This condition is one of the most common age-related vision disabilities, and often occurs around the age of 40.10 Figure 1 demonstrates the loss of intraoral clarity when a patient uses a typical bathroom mirror with no special lighting or magnification. However, when clinicians can help patients improve their ability to visualize plaque, bleeding, and inflammation through the use of enhanced lighting and magnification, patients becomes better equipped—and motivated—to improve their oral hygiene.
MAGNIFICATION MIRRORS
Magnifying mirrors—which work by enlarging an image in appearance but not actual size—may prove useful for patients who wish to improve their ability to perform oral hygiene tasks. Many patients may already own this helpful oral hygiene aid, which is commonly purchased for applying make-up or shaving.
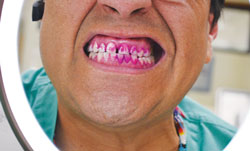
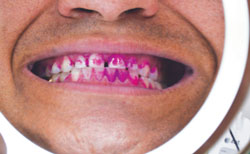
Typical magnification mirrors for consumer use range from 1x power to 15x power, though a modest amount of magnification is sufficient for most patients. In fact, patients should be cautioned not to over magnify the facial area, as increased magnification power results in a decreased field of view.1 Note how the field of view changes when 1x magnification is used (Figure 2) in comparison to a lighted mirror with 8x magnification (Figure 3). In addition to magnification power, patients should also consider their working distance or proximity to a magnifying mirror. For example, tall patients may need increased magnification to accommodate the greater distance from the mirror (depending on where it is placed within the home). When discussing these adjuncts for self-care with patients, clinicians should explain how the power of magnification can vary among products. Keep a few mirrors with different levels of magnification power on hand for patient demonstration. This will help patients discover the best power magnification for their specific needs.
Numerous types of lighted magnification mirrors are available. From adjustable wall-mounted mirrors to shower-mounted mirrors and table-top mirrors, patients should succeed in finding a magnification device suitable to their height and comfort. Higher-end models include special sensors that automatically light up as a face approaches. Cordless and travel models are also available. Ranging in price from $50 to $200, magnification mirrors can be purchased virtually anywhere.
LIGHTING
Light emitting diode (LED) technology is frequently used with loupes, and it may prove helpful to patients who use magnification mirrors during oral self-care. LED lighting provides a natural light source; produces less heat than bulbs with similar light output; and lasts longer than incandescent and fluorescent lighting.
LED technology is used in make-up magnifying mirrors, though small incandescent and compact fluorescent lamps are also available. The combination of illumination with magnification provides clinicians with an improved intraoral work site compared to typical operatory lighting. This is because the light projected into the clinician’s line of vision prevents shadows in the oral cavity. Ideally, the intraoral work site should also be at least 3x brighter than the background light.1 When compared to typical bathroom lighting, the illumination provided by a make-up mirror can improve lighting conditions—helping patients be more effective in plaque removal and oral hygiene self-assessment. While enhanced lighting may be beneficial for all patients looking to improve their plaque removal skills, it is baby boomers and older adults who most need an increase in light to perform detailed tasks. Clinicians may want to suggest that their patients evaluate and compare the different light and magnifying sources found in make-up mirrors before purchasing one to determine the best fit for visual acuity.
DISCLOSING SOLUTIONS
Regular and thorough plaque biofilm removal is a challenge for many patients and is dependent on their skill, technique, and ability to self-assess biofilm removal. A contributing factor may be that patients simply cannot visualize the gingival inflammation or plaque present in their mouths. Improved lighting conditions and magnification may advance patients’ abilities to detect the presence of plaque or signs of gingival inflammation and bleeding. The ability to visualize these conditions during oral self-care may be enhanced through the periodic use of plaque disclosing solutions. Figure 2 and Figure 3 demonstrate the combined use of disclosing solution with light and magnification to further improve patients’ abilities to self-assess their oral hygiene care.
OTHER EYE CONCERNS
The inability to see clearly at close distances is not the only obstacle experienced by older adults—a number of other vision concerns may be present among patients age 40 and older. If patients report a new vision problem, oral health professionals should encourage them to seek an evaluation from a medical provider or ophthalmologist. The American Optometric Association notes the following conditions may be of special concern for adult patients:10
- Chronic systemic conditions, such as diabetes or high blood pressure
- Family history of glaucoma or maculardegeneration
- Visually demanding job or eye-hazardous occupation
- High cholesterol, thyroid conditions,anxiety, arthritis, and related medications that have ocular side effects
CONCLUSION
Dental hygienists are the primary care providers of preventive oral health services.13 They are also well known for their creativity in helping patients accomplish effective oral health behaviors. The adage “what’s good for the goose is good for the gander” seems apropos when examining the benefits of light and magnification. If light and magnification improve clinicians’ visual acuity during clinical treatment, then perhaps adult patients can reap similar benefits from light and magnification to improve their oral health. Future research should address the use of these ergonomic tools in assisting patients with plaque detection and removal—thus improving oral health.
ACKNOWLEDGEMENT
The author would like to thank Nicholas Salomon for his assistance with the images for this article.
REFERENCES
- Chang BJ. Ergonomic benefits of surgical telescope systems: selection guidelines. J Calif Dental Assoc. 2002;30:161–169.
- Marsh L. Practicing ergonomically correct dental hygiene. Dimensions of Dental Hygiene. 2009;7(1):22–23.
- Branson B, Simmer-Beck M. Visual acuity without injury. Dimensions of Dental Hygiene.2009;7(9):46–49.
- Michaelides P, Stambaugh R. Zooming in on magnification. Dimensions of Dental Hygiene. 2007;5(4):16–21.
- Maillet JP, Millar AM, Burke JM, Maillet MA,Maillet WA, Neish NR. The effect of magnification loupes on dental hygiene student posture. J Dent Educ. 2008;72:33–44.
- Branson BG, Bray KK, Gadbury-Amyot C,et al. The effect of magnification lenses on student operatory posture. J Dent Educ.2004;68:384–389.
- Leknius C, Geissberger M. The effect of magnification on the performance of fixed prosthodontic procedures. J Calif Dental Assoc.1995;23:66–70.
- Sanders MJ, Michalak-Turcotte. Posture makes perfect. Dimensions of Dental Hygiene. 2011;9(11):30–35.
- Sanders MJ, Michalak-Turcotte. Preventing work related MSDs in dental hygienists. In: Sanders M, ed. Ergonomics and the Management of Musculoskeletal Disorders.2nd ed. St. Louis: Butterworth Heinemann; 2004:448–469.
- American Optometric Association. Adult vision: 41 to 60 years of age. Available at www.aoa.org/x9453.xml. Accessed October 13, 2013.
- Anderson GJ. Aging and vision: changes in function and performance from optics to perception. Wiley Interdiscip Rev Cogn Sci. 2012;3:403–410.
- Owsley C. Aging and vision. Vision Res.2011;51:1610–1622.
- Wilkins EM. Patient learning for health behavioral change. In: Wilkins EM, ed. Clinical Practice of the Dental Hygienist. 11th ed. Philadelphia: Lippincott Williams & Wilkins;2013:363–376.
From Dimensions of Dental Hygiene. November 2013;11(11):30,32,34.

