 SUYASH.DWIVEDI, C, VIA WIKIMEDIA COMMONS
SUYASH.DWIVEDI, C, VIA WIKIMEDIA COMMONS
Managing High-Risk Patients With SDF
Silver Diamine Fluoride is safe, efficient, and effective, providing a helpful alternative in the caries management effort.
Dental hygienists provide care to diverse patient populations, some of whom are more difficult to treat than others. Children and adults at increased caries risk can pose challenges to even the most adept clinician. Arresting active caries lesions via silver diamine fluoride (SDF) provides an efficient nonsurgical alternative to traditional restorative dental treatment in young children, adolescents, patients with special needs, and aging adults that is appropriate in both private and public health settings.1,2
Appropriate Patient Populations
SDF halts the progression of caries lesions and is an excellent alternative for patients classified as high caries risk.1–4 These may include the following:
- Patients with special needs, such as severe cognitive and physical disabilities.1,3,4 These patients may not be able to sit for long appointment times. Challenges, such as sensory issues, food sensitivities, inadequate self-care, and adverse effects of medication use, may dramatically increase this patient population’s caries risk.
- Older adult patients who reside in nursing homes and assisted living facilities.1 Limited mobility; decreased access to care; and medical, behavioral, physical, and financial limitations all contribute to increased caries risk. The United States Centers for Disease Control and Prevention estimates that 1.4 million Americans reside in nursing homes and 1.2 million live in hospice.5
- Patients diagnosed with early childhood caries (ECC).The treatment of ECC is costly because the cooperative capacity of toddlers and preschool-aged children usually necessitates the use of general anesthesia.1,3,4
Nonsurgical SDF treatment can be easily applied to the site of infection and has fewer contraindications than other restorative treatment options, making it a game changer in the caries management arena.1
History of Use
SDF has been used safely around the world for more than 80 years. In fact, its use in dentistry can be traced back before the 20th century when it was used as a remedy for dentinal hypersensitivity and a caries inhibitor.6–8 However, it was not until 2014 that the US Food and Drug Administration approved it for treating dentin hypersensitivity in adults.9 The first commercial product became available for use in the US in 2015, and numerous clinical trials have established the effectiveness of SDF as a caries-arresting medicament.1–4 SDF also meets the six quality standards set by the US Institute of Medicine: safe, effective, efficient, timely, patient-centered, and equitable.9
Burden of Caries
Dental caries is a preventable chronic disease that continues to impact individuals across their lifespans. The prevalence of dental caries is the highest among children ages 6 to 11 and adolescents ages 12 to 19.10 Tooth decay is four times more common than asthma among those aged 14 to 17.10 Caries also affects adults older than age 19, with a 90% to 97% incidence rate of caries in at least one tooth.10,11
Dental caries is a multifactorial, behaviorally mediated, biofilm-based disease.12 An increased bacterial load or decreased salivary flow (xerostomia) hinder the body’s natural remineralization process and inhibit fluoride’s ability to prevent or arrest the caries process.13 Poor oral health affects systemic health, employment opportunities, job performance, self-esteem, and well-being.14,15 Poor oral health has long-term effects associated with severe illnesses, such as cardiovascular disease, diabetes, certain types of cancer, pneumonia, dementia, Alzheimer disease, and low birth weight.14,15
Untreated dental caries in children is often influenced by social determinants of health including income, ethnicity, cost, limited availability of providers, and access to oral health services.7,8,16,17 In low-income communities, dental caries often goes untreated, resulting in pain, missed school hours, poor academic performance, increased cost, and a decreased quality of life for affected children and their caregivers.7,8
Traditional restorative treatment can be challenging to provide to very young children with severe dental disease and those with special needs.16 SDF is faster to apply than sealants and less expensive.17 In fact, data from one of the largest school-based SDF programs suggest that it could eliminate 80% of caries among students while costing less than 20% of oral health spending from Medicaid.8,16,17
Benefits and Risks
The use of SDF offers many benefits, including ease of use, no need for anesthesia, instant and painless results, and preventing the need for invasive treatment among those who find it difficult to comply.16
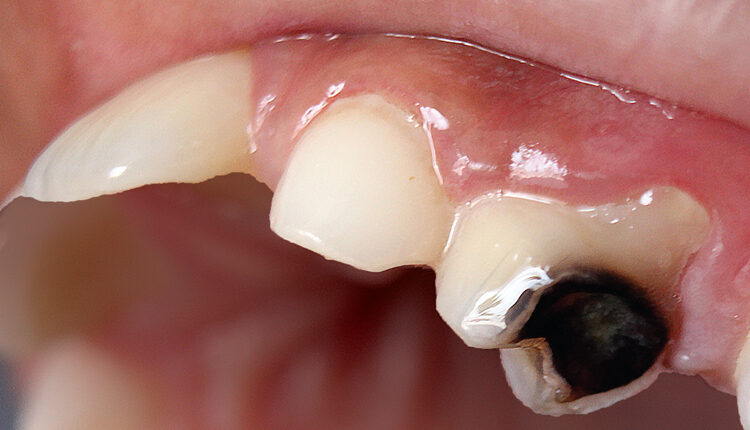
While SDF provides myriad benefits in certain populations, it does produce black or brown staining of the caries lesion. In addition, SDF temporarily stains skin, gingiva, clothes, and surfaces. Research suggests that the use of potassium iodide after SDF application may control or reverse the staining. Some commercial products with both SDF and potassium iodide are available. While staining on anterior teeth has raised some concerns among parents, the posterior teeth presented no issue with parental satisfaction. All patients must be informed of the benefits and contraindications and sign a consent for SDF placement.8,9,13,14
Clinical application
The clinical application of SDF on facial, lingual, and occlusal surfaces is simple.3,12
- Protect the lips with petroleum jelly or lip balm. Dental hygienists may prefer scented lip balm to mask the slight smell of ammonia.
- Isolate the tooth with cotton rolls.
- Clean the lesion of food debris with a microbrush or cotton pellet and then dry it.
- Paint SDF onto the clean lesion for 1 minute and allow to air dry.
- While post-operative rinsing with the air-water syringe after SDF application is not necessary, fluoride varnish should be applied to the treated tooth and the remainder of the dentition. The flavor of varnish is appealing and it keeps the SDF attached to the tooth surface. Fluoride varnish also remineralizes the rest of the dentition. It would be safe to assume that if a patient has one area of decay, other areas of demineralization may be present within the mouth.
- Evaluate the lesion for color change and hardness.
For proximal caries mesial and distal surfaces only:8
- Isolate the tooth with cotton rolls.
- Clean the lesion of food debris with floss.
- Place an SDF-coated soft pick into the proximal area for 1 minute and allow to air dry. The pick can be pulled gently in and out to agitate. The SDF then becomes absorbed into the proximal lesion.
- Dab additional SDF using a microbrush above the contact and in the buccal and lingual sluiceways. Blot any excess fluid and blood with a cotton roll, pellet, or swab. If there is radiographic evidence of a deeper decalcification or caries lesion, apply an additional 60-second insertion in the same manner.
- Paint fluoride varnish (5%) over the treatment area with the pick still in place and then withdraw the pick.
- Using radiography, note any changes in lesion 6-months post-application.
- Apply fluoride varnish to the remainder of the dentition.
Evidence-based research suggests that 38% SDF solution is the most effective.1–4 Application every 6 months is more effective than one annual application. Application times range from 1 minute to 3 minutes. Curing lights have been used by some clinicians to decrease set time.
Anterior teeth have higher rates of caries arrest than posterior teeth. Large occlusal lesions and those with visible biofilm have fewer chances of arrest. An annual application of SDF appears to be effective for the arrest and prevention of root caries in older adults who are capable of self-care. Multiple applications may benefit more dependent and at-risk older individuals. With all age groups, clinicians should use their best clinical judgment about application frequency based on individual caries risk factors, fluoride exposure, patient needs, and individual social determinants of health.3
Scope of Practice
According to the American Dental Hygienists’ Association’s “State Specific Information on Silver Diamine Fluoride,” all 50 states allow dental hygienists to administer SDF with either general or direct supervision.11
SDF is a preventive agent that has much to offer in reduction of the caries burden. It is safe, aerosol-free, and easy to apply. Oral health professionals should consider adding it to their caries-management armamentariums.
Acknowledgment
The author would like to thank Kim Attanasi, PhD, MS, RDH, for her assistance with this manuscript.
References
- Wright JT, White A. Silver diamine fluoride: changing the caries management paradigm and potential societal impact. N C Med J. 2017;78:394–397.
- Ruff RR, Niederman R. Silver diamine fluoride versus therapeutic sealants for the arrest and prevention of dental caries in low-income minority children: study protocol for a cluster randomized controlled trial. Trials. 2018;19:523.
- Use of silver diamine fluoride for dental caries management in children and adolescents, including those with special health care needs. Pediatr Dent. 2017;39:146–155.
- Use of silver diamine fluoride for dental caries management in children and adolescents, including those with special health care needs. Pediatr Dent. 2018;40:152–161.
- United States Centers for Disease Control and Prevention, National Center for Health Statistics . Oral Health Conditions. Available at: .cdc.gov/nchs/fastats/nursing-home-care.htm. Accessed June 14, 2022.
- Yee R, Holmgren C, Mulder J, Lama D, Walker D, van Palenstein Helderman W. Efficacy of silver diamine fluoride for arresting caries treatmentJ J Dent Res. 2009;88:644–647.
- Eslami NP, Chan DCN, Sadr A. Effect of silver diamine fluoride and glass ionomer on remineralisation of natural dentine caries. J Dent. 2021;106:103578.
- Croll TP, Berg J. Delivery methods of silver diamine fluoride to contacting proximal tooth surfaces and history of silver in dentistry. Compend Contin Educ Dent. 2020;41:84–89.
- Crystal YO, Niederman R. Silver diamine fluoride treatment considerations in children’s caries management. Pediatr Dent. 2016;38:466–471.
- United States Centers for Disease Control and Prevention, National Center for Health Statistics . Oral Health Conditions. Available at: cdc.gov/nchs/fastats/nursing-home-care.htm. Accessed June 14, 2022.
- American Dental Hygienists’ Association. Silver Diamine Fluoride State by State Information. Available adha.org/resources-docs/Silv_r_Diamine_Fluoride_State_by_State_Information.pdf. Accessed June 14, 2022.
- Seifo N, Robertson M, MacLean J, et al. The use of silver diamine fluoride (SDF) in dental practice. Br Dent J. 2020;228:75–81.
- Greenwall-Cohen J, Greenwall L, Barry S. Silver diamine fluoride —an overview of the literature and current clinical techniques. Br Dent J. 2020;228:831–838.
- Chu CH, Lo EC. Promoting caries arrest in children with silver diamine fluoride: a review. Oral Health Prev Dent. 2008;6:315–321.
- Twetman S. The evidence base for professional and self-care prevention—caries, erosion and sensitivity. BMC Oral Health. 2015;15 Suppl 1(Suppl 1):S4.
- Ruff RR, Niederman R. Comparative effectiveness of treatments to prevent dental caries given to rural children in school-based settings: protocol for a cluster randomised controlled trial. BMJ Open. 2018;8:e022646.
- Bridge G, Martel AS, Lomazzi. Silver diamine fluoride: transforming community dental caries program. Int Dent J. 2021;71:458–461.
From Dimensions of Dental Hygiene. July 2022; 20(7)22-24.

