 PRAWEENA/ISTOCK/GETTY IMAGES PLUS
PRAWEENA/ISTOCK/GETTY IMAGES PLUS
Air Polishing for Today’s Dental Hygienist
A new addition to the biofilm management armamentarium, air polishing offers significant benefits to both patients and clinicians.
This course was published in the October 2018 issue and expires October 2021. The authors have no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- Identify the role of biofilm management in periodontal health.
- Compare and contrast conventional supragingival air polishing with subgingival air polishing.
- Discuss the type of equipment needed in air polishing.
- List strategies for implementing air polishing into the dental hygiene process of care.
One of the greatest challenges for achieving and maintaining a healthy periodontium is biofilm management. Plaque biofilm is the primary etiology for gingival diseases; therefore, disruption and removal slow down progression of the inflammatory process. Most subgingival biofilm within pockets cannot be reached by conventional toothbrushes, floss, interdental aids, or mouthrinses.
Professional removal of biofilm is an integral aspect of nonsurgical periodontal therapy and the preventive services provided by oral health professionals. Goals of periodontal debridement include removal of calculus and biofilm, elimination of inflammation, removal of infection, and maintenance of a healthy periodontium.1 Traditionally, biofilm management has been professionally disrupted using ultrasonic instrumentation, hand instrumentation, and rubber cup polishing. The use of air polishing can also provide benefits to both patients and clinicians.
CONVENTIONAL SUPRAGINGIVAL AIR POLISHING
Conventional supragingival air polishing uses a combination of air, water, and abrasive powders. Indications for use include removal of biofilm and stain on enamel surfaces, and cleaning of pits and fissures prior to sealant placement. Supragingival air polishing is technique sensitive but offers an alternative to traditional rubber cup polishing for removal of biofilm and extrinsic stain.
The traditional supragingival air polishing powder is sodium bicarbonate. Sodium bicarbonate is nontoxic and water soluble, thus making it ideal for intraoral use.2 Aluminum trihydroxide is an alternative type of low abrasive powder that may also be used for supragingival air polishing, but it is not water soluble. Table 1 lists the contraindications for sodium bicarbonate air polishing powder. Advantages include safe and efficient removal of extrinsic plaque and stains on intact enamel surfaces. Research also shows that sodium bicarbonate air polishing is approximately one-third less time consuming when compared with hand instrumentation and rubber cup polishing.2–10 Disadvantages include salty taste, large particle size, aerosol production, unpleasant stinging sensation, potential for soft tissue trauma, and contraindicated for use on root surfaces, demineralized surfaces, and restorative materials. In addition, sodium bicarbonate air polishing can lead to erosion or dulling effects of filling materials.2,3,11–15
Research has shown that air polishing using sodium bicarbonate led to root structure loss and, therefore, cannot be recommended in patients with exposed root surfaces.16 This is a particular concern for patients with periodontal disease, as there is a high incidence of coexisting gingival recession in these patients.2,17,18 While benefits exist for the use of conventional sodium bicarbonate air polishing, studies have shown that it is not possible to adjust the working field to be safe for effective debridement of biofilm from root surfaces or subgingival surfaces.
BENEFITS OF SUBGINGIVAL AIR POLISHING
New technology has expanded the traditional method of biofilm and stain removal from only supragingival removal to include subgingival surfaces. When used effectively, subgingival air polishing can safely remove biofilm from enamel and root surfaces, and within the periodontal pocket. New technologies have now been created for subgingival polishing with glycine powder as the main polishing agent. Glycine is a nonessential amino acid and the substance is significantly smaller in particle size when compared to sodium bicarbonate powders.
The benefits of using glycine powder are twofold: it provides a safe alternative to sodium bicarbonate for effective removal of biofilm and stain, and it allows for subgingival removal of biofilm without risk of harming oral tissues such as dentin and cementum.16 Research on subgingival air polishing supports its use for better outcomes in nonsurgical periodontal therapy.19
Glycine powder air polishing is safe and causes decreased gingival trauma when compared with hand instrumentation and sodium bicarbonate powder.20–23 Subgingival air polishing uses a low abrasive glycine powder, which is 80% less abrasive than sodium bicarbonate.24 Glycine air polishing powder can also be safely used on restorative materials, dental implants, and debridement of periodontal pockets up to 5 mm.25,26 In one study, glycine powder resulted in improved access to pits and fissures, demonstrated rapid removal of biofilm and debris, and indicated no recognizable change in plastic brackets when tested.27 Research evaluating the effect of glycine powder used on enamel, composite, and glass ionomer cement found a reduced amount of change in surface characterization compared to certain sodium bicarbonate and aluminum trihydroxide powders.28 Patients also tolerated the sweet taste compared to the salt-based sodium bicarbonate powder.
Other advantages of glycine powder subgingival air polishing include time efficiency, less operator fatigue, no heat production for dental surfaces, and more effective removal of biofilm in pits and fissures. When compared to sodium bicarbonate, glycine powder has fewer contraindications for use (Table 2). One limitation of using the glycine air polishing device is that additional clinical training is recommended for proper subgingival biofilm removal techniques. Glycine powder is not as effective at removing tenacious stain when compared with traditional sodium bicarbonate powder.
While manual instrumentation is limited in its ability to effectively remove subgingival biofilm,29 glycine can also be used for subgingival biofilm removal to enhance treatment of periodontitis, peri-implant mucositis, peri-implantitis, and periodontal maintenance.30 During the 2015 EuroPerio Consensus Conference, recommendations on the clinical application of air polishing for the management of peri-implant mucositis and peri-implantitis were discussed and published.31 Nine consensus statements were developed on the effects of subgingival air polishing with glycine powder:
- Safe for use on implants and implant-supported restorations
- Safe for treatment of both peri-implant mucositis and peri-implantitis
- Results in clinical improvements, such as reduction in bleeding on probing
- Demonstrates effective biofilm disruption
A systematic review of nonsurgical treatment for peri-implantitis showed that the use of glycine was successful in reducing bleeding on probing when compared with hand instrumentation.32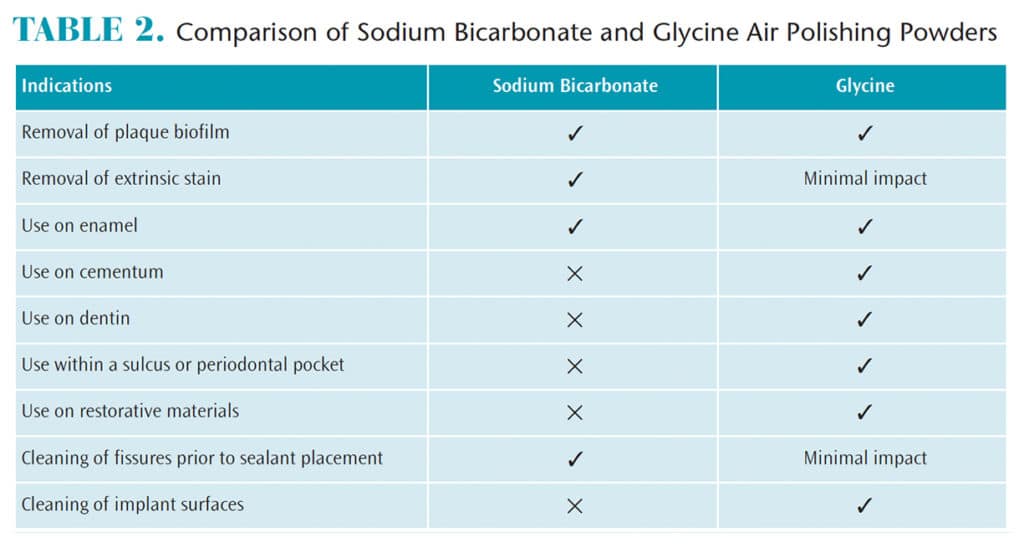
EQUIPMENT
Several companies make air polishing devices that offer subgingival technologies. One design includes a combination of a piezoelectric ultrasonic scaler with a supra- and subgingival air polisher. This unit offers the clinician flexibility in technique by allowing for both supra- and subgingival air polishing for a variety of patient needs. Another design is a portable hand unit that can be interchangeable and attached to the air compression lines of a dental unit. When using a standard nozzle, both of these units are used for supragingival biofilm removal and subgingival biofilm removal in normal sulci or shallow pockets up to 4 mm. The units include a site-specific periodontal nozzle tip for reaching periodontal pockets greater than 4 mm.
INTEGRATING THE TECHNIQUE INTO PRACTICE
Integration of air polishing affords the oral health professional new options and an enhanced approach to patient care. When determining the most effective technologies for individualized care, consideration must include evidence of oral disease, presence and level of biofilm and stain, and overall health status. Healthy individuals with stain may be better candidates for traditional supragingival air polishing using sodium bicarbonate. On the other hand, patients with gingival disease may be better served by subgingival air polishing using glycine. Research has indicated the use of subgingival air polishing prior to calculus removal has an advantageous approach to the dental hygiene process of care (Table 3).33
Clinicians skilled in the use of glycine powder air polishing recommend air polishing first, followed by periodontal instrumentation. Benefits of this approach include increased time efficiency, decreased clinician fatigue, better patient acceptance, and enhanced efficacy. Subgingival air polishing with glycine powder has been shown to be more effective in removing subgingival biofilm vs hand instrumentation, which leads to increased patient comfort.34 With the goals of periodontal debridement at the forefront of dental hygiene care, the use of subgingival air polishing technology can assist in achieving better patient outcomes by providing alternative options to achieving the goals of periodontal therapy.
CONCLUSION
Oral health professionals must stay abreast of new technologies that offer enhanced patient outcomes. Clinicians may feel limited by the initial cost or a new learning curve with new technologies. However, the benefits of implementing and using evidence-based technologies offer great advantages to both the patient and clinician. Air polishing procedures offer advantages when compared with conventional biofilm removing procedures. By understanding the benefits of air polishing, the clinician is better equipped to provide optimal patient care.
REFERENCES
- Francis B, Fleming D. Powered instrumentation in periodontal debridement. In: Daniel S, Harfst S, Wilder R, eds. Dental Hygiene Concepts, Cases and Competencies. 2nd ed. St. Louis: Elsevier, 2008.
- Petersilka GJ. Subgingival air-polishing in the treatment of periodontal biofilm infections. Periodontol 2000. 2011;55:124–142.
- Barnes CM, Russell CM, Gerbo LR, Wells BR, Barnes DW. Effects of an air-powder polishing system on orthodontically bracketed and banded teeth. Am J Orthod Dentofacial Orthop. 1990:97:74–81.
- Berkstein S, Reiff RL, McKinney JF, Killoy WJ. Supragingival root surface removal during maintenance procedures utilizing an air-powder abrasive system or hand scaling. An in vitro study. J Periodontol. 1987:58:327–330.
- Horning GM, Cobb CM, Killoy WJ. Effect of an air-powder abrasive system on root surfaces in periodontal surgery. J Clin Periodontol. 1987:14:213–220.
- Kontturi-Narhi V, Markkanen S, Markkanen H. Effects of airpolishing on dental plaque removal and hard tissues as evaluated by scanning electron microscopy. J Periodontol. 1990:61:334–338.
- Kovacevic R. Monitoring the depth of abrasive waterjet penetration. Int J Mach Tools and Manuf. 1992:32:725– 736.
- Mahlendorff M. Evaluation of the relationships between abrasion and surface alterations after professional tooth cleaning. Dtsch Zahnarztl Z. 1989:44:203–204.
- Atkinson DR, Cobb CM, Killoy WJ. The effect of an air-powder abrasive system on in vitro root surfaces. J Periodontol. 1984;55:13-18.
- Weaks LM, Lescher NB, Barnes CM, Holroyd SV. Clinical evaluation of the Prophy-Jet as an instrument for routine removal of tooth stain and plaque. J Periodontol. 1984:55:486–488.
- Castagnola L, Wirz J, Garberoglio R. Die Reinigung der Schmelzoberfla ̈che von Plaque und starken Verfa ̈r- bungen mit dem Prophy-Jet. Quintessenz. 1983:34:963–972.
- Cooley RL, Lubow RM, Patrissi GA. The effect of an air- powder abrasive instrument on composite resin. J Am Dent Assoc. 1986:112:362–364.
- Hu ̈ gelmeyer T. Oberfla ̈ chenvera ̈ nderung von Zahnsch- melz, Wurzelzement, Amalgam und Kunststoff nach Behandlung mit verschiedenen Reinigungsinstrumenten. Quintessenz. 1989:40:683–693.
- Jost-Brinkmann PG. The influence of air polishers on tooth enamel. An in-vitro study. J Orofac Orthop. 1998:59:1–16.
- Lubow RM, Cooley RL. Effect of air-powder abrasive instrument on restorative materials. J Prosthet Dent. 1986:55:462–465.
- Sahrmann P, Rony V, Schmidlin PR, Attin T, Paque F. Three-dimensional defect evaluation of air polishing on extracted human roots. J Periodontol. 2014:85:1107–1114.
- Holtfreter B, Schwahn C, Biffar R, Kocher T. Epidemiology of periodontal diseases in the Study of Health in Pomerania. J Clin Periodontol. 2009:36:114–123.
- Hugoson A, Sjodin B, Norderyd O. Trends over 30 years, 1973–2003, in the prevalence and severity of periodontal disease. J Clin Periodontol. 2008:35:405–414.
- Petersilka GJ, Bell M, Haberlein I, Mehl A, Hickel R, Flemmig TF. In vitro evaluation of novel low abrasive air polishing powders. J Clin Periodontol. 2003;30:9–13.
- Petersilka GJ, Haberlein I, Barakos K, et al. Subgingival plaque removal at buccal and lingual using a novel low abrasive air polishing powder. J Clin Periodontol. 2003;30:328–333.
- Flemmig TF, Hetzel M, Topoll H, et al. Subgingival debridement efficacy of glycine powder air-polishing. J Periodontol. 2007;78:1002–1010.
- Petersilka GJ, Faggion Jr MC, Stratmann U, et al. Effect of glycine powder air-polishing on gingiva. J Clin Periodontol. 2008;35:324–332.
- Simon CJ, Vekatech PML, Chickanna R. Efficacy of glycine powder air polishing in comparison to sodium bicarbonate air polishing and ultrasonic scaling: a double-blind clinico-histopatholigic study. Int J Dent Hyg. 2015;13:177–183.
- Petersilka GJ, Bell M, Mehl A, Hickel R, Flemmig TF. Root defects following air polishing. J Clin Periodontol. 2003:30:165–170.
- Tastepe CS, Lin X, Donnet M, Wismeijer D, Liu Y. Parameters that improve cleaning efficiency of subgingival air polishing on titanium implant surfaces: an in vitro study. J Periodontol. 2017;88:407–414.
- Petersilka GJ, Steinmann D, Häberlein I, Heinecke A, Flemmig TF. Subgingival plaque removal in buccal and lingual sites using a novel low abrasive air–polishing powder. J Clin Periodontol. 2003;30:328–333.
- Wilmes B, Vali S, Drescher D. In vitro study of surface changes in fixed orthodontic appliances following air polishing with Clinpro Prophy and Air–Flow. J Orofac Orthop. 2009;70:371–384.
- Barnes CM, Hayes EF, Leinfelder KF. Effects of an airabrasive polishing system on restored surfaces. Gen Dent. 1987;35:186–189.
- Gutmann ME. Air polishing: a comprehensive review of the literature. J Dent Hyg. 1998;72:47–56.
- Sahm N, Becker J, Santel T, Schwarz F. Non–surgical treatment of peri–implantitis using an air–abrasive device or mechanical debridement and local application of chlorhexidine: a prospective, randomized, controlled clinical study. J Clin Periodontal. 2011;38:872–878.
- Schwarz F, Becker K, Bastendorf KD, et al. Recommendations on the clinical application of air polishing for the management of peri-implant mucositis and peri-implantitis. Quintessence Int. 2016;47:293–296.
- Muthukuru M, Zainvi A, Esplugues EO, Flemmig TF. Non-surgical therapy for the management of peri-implantitis: a systemic review. Clin Oral Implants Res. 2012;23(6 Suppl):77–83.
- Davis K. Biofilm removal with air polishing and subgingival air polishing. Available at: ineedce.com/courses/2507/PDF/1309cei_davis_web.pdf. Accessed September 24, 2018.
- Cobb CM, Daubert DM, Davis K, et al. Consensus conference on supra- and subgingival air-polishing. Compend Contin Educ Dent. 2017;38:1–8.
From Dimensions of Dental Hygiene. October 2018;16(10):35–38.



