
The Evolution of Sealants
With advancements in materials and methods, dental sealants remain one of the most important tools in the caries prevention armamentarium.
Dental sealants are part of the standard of care in the fight against dental caries.1 Since their introduction in the 1960s, sealant materials, methods of application, tooth selection criteria, and usage guidelines have changed.1,2 In 1955, Michael G. Buonocore, DMD, MS, of Rochester, NY, developed a new technique that used an acid etchant to mechanically bond an acrylic resin to the tooth. This created a barrier, which blocked the ability of food, such as fermentable carbohydrates, to reach the acid–creating bacteria located in pits and fissures—thereby preventing decay.3 This technique was the starting point for dental sealants, as well as other applications in cosmetic dentistry.4 However, 20 years passed before dental sealants became a commonly used prevention strategy in the United States.2
CHANGES IN DIAGNOSTIC METHODS
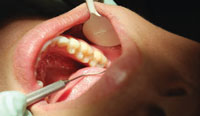
For years, occlusal decay was diagnosed by inserting the tip of the explorer into the pit and fissure5 to see if it would “stick” in the tooth surface (Figure 1). Today, more sophisticated caries detection technologies are available. Most are light–based diagnostic techniques that rely on the visual appearance of enamel. These devices measure different types of light in relation to the tooth surface. Reflectant light technologies measure the light that is reflected by the tooth surface.
Luminescent modalities measure the level of glow and heat after a laser light is applied to the tooth surface. Other tools measure light transmission or fluorescence or use electrical impedance to assess a tooth’s health. Evidence varies on the efficacy of these devices. Products measuring fluoresence are highly sensitive, but they may also produce false positives.6 Reflectant light tools are effective but may not be specific enough to detect early carious lesions.7 Luminescent technologies are able to successfully detect caries on occlusal surfaces.8 These devices can all contribute to the caries diagnostic process, especially when combined with visual and radiographic examinations.5
ADVANCES IN MATERIALS
Dental sealants have improved with advancements in the materials used. Improvements in the viscosity and the ability to resist flow have contributed to ease of use.2 Some sealants can now be applied in a moist environment, which has led to easier placement and improved adhesion.2 Self–etching adhesives are also available, which reduce the time needed for placement.
Sealants are classified into three types: unfilled, filled, and fluoride–releasing. Unfilled sealants naturally abrade within 24 hours to 48 hours, and thus require no occlusal adjustment. Unfilled sealants are less viscous so they may flow more easily into pits and fissures.9 Filled sealants contain additives that create bulk in order to boost bond strength and help the material resist abrasion and wear.10 They typically require a longer time to cure.11 Glass ionomer sealants release fluoride and are hydrophilic, however, their retention is not typically as long as traditional sealants. They are best applied in patients who have poor oral selfcare or when tooth isolation is impossible. The giomer sealant, a new fluoride–releasing material that contains surface pre–reacted glass ionomer filler particles, is now available. It contains a self–etching primer that eliminates the need for acid etching.12
Dental sealants are manufactured in colors including clear, tinted, and opaque. Some change color after polymerization to improve monitoring, but this has no effect on retention.10
TOOTH SELECTION
The decision to seal a tooth is based on tooth morphology, status of the eruption, caries history, and future caries risk. Placing sealants on the permanent molars of children is an effective caries prevention strategy.13 Also, the placement of sealants over an early carious lesion can help prevent it from progressing into decay, thus reducing the need for restorative care.14 Caries risk assessment should be conducted routinely and treatment planning should be adjusted accordingly.
Dental sealants should not be considered if proximal decay is detected radiographically.10 Also, occlusal surfaces with well coalesced pits and fissures are most likely at low caries risk and need not be sealed.10
SAFETY
Bisphenol–A (BPA), an organic compound, is contained in some sealant materials and the risks related to exposure are not well understood. BPA imitates the hormone estrogen and exposure may initiate hormone responses in the body. The derivatives of BPA may cause problems in the prostate and urinary tracts. Fleisch et al found that BPA remains in children’s mouths up to 3 hours after sealant placement.15 The authors assert that the benefits gained from sealant placement combined with the brief level of exposure support the continued use of sealants in caries prevention, but suggest that pregnant patients postpone placement of dental sealants until after delivery.15 There are sealant materials available without BPA. Clinicians can also rub the surface of the sealant with pumice to remove any residual BPA. Rinsing the sealant with water for 30 seconds immediately after light curing also provides further removal of the BPA layer.15
OBSTACLES
Dental sealants are woefully underutilized in private practice, despite their proven efficacy. Factors that interfere with implementation include the perception that dental sealants may inadvertently seal incipient caries into the tooth surface, questions about their efficacy, and low or no reimbursement from third party payers.16 Dental sealants placed within school–based and government–funded programs have made significant reductions in dental caries, which providing extensive savings in health care expenditures due to a reduced need for restorative care.17 Cost effectiveness relies on sealant retention.5 Factors that lead to sealant failure include: placement problems with partially erupted teeth, poor isolation, patient behavioral problems, enamel morphology, and defects. Re–evaluation of sealants should be done periodically and lost sealants should be replaced.3
FUTURE OF SEALANTS
The United States Centers for Disease Control and Prevention has identified dental sealants as a key element in the fight to prevent dental caries in primary teeth and improve overall oral and systemic health among Americans.1 As the prevention experts, dental hygienists can play a significant role in improving the usage of sealants among their patients and helping to ensure their long–term retention.
REFERENCES
- United States Department of Health and HumanServices. Healthy People 2020. Available at: www.healthypeople.gov/ 2020/ topics objectives 2020/ overview.aspx?topicid=8. Accessed October 8, 2012.
- Gjermo P. Chlorhexidene and related compounds. J Dent Res.1989;68:102.
- Banks V. The sealant story: A look at the evolution of the dental sealant. Dimensions ofDental Hygiene. 2009;7(7):28—31.
- Buonocore M. A simple method of increasing the adhesion of acrylic filling materials to enamel surfaces. J Dent Res. 1955;34:849—853.
- Kugel G, Ferrari M. The science of bonding:From first to sixth generation. J Am Dent Assoc.2000;131:205–255.
- Strassler H, Porter J. Success with pit and fissure sealants. Dent Today. 2005;24:124—30.
- Ferreira Zandoná AG, Analoui M, Beiswanger BB,et al. An in vitro comparison between laser fluorescence and visual examination for detection of demineralization in occlusal pits and fissures.Caries Res. 1998;32:210—218.
- Amaechi B. Emerging technologies for diagnosisof dental caries: the road so far. J Appl Phys.2009;105:102047.
- Jeon RJ, Hellen A, Matvienko A, et al. In vitro detection and quantification of enamel and root caries using infrared photothermal radiometry and modulated luminescence. J Biomed Optics. 2008;13:034025–034011.
- Feigal RJ, Donly KJ. The use of pit and fissure sealants. Pediatr Dent. 2006;28:143—150.
- Wyche C. Sealants. In: Wilkins EW. ClinicalPractice of the Dental Hygienist. 11th ed. St. Louis: Lippincott Williams and Wilkins; 2012:542—550.
- Yue C, Tantbirojn D, Grothe RL, Versluis A,Hodges JS, Feigal RJ. The depth of cure of clear versus opaque sealants as influenced by curing regimens. J Am Dent Assoc. 2009;140:331—338.
- Burgess JO. Material revolution. Dimensions of Dental Hygiene. 2012;10(10):41—44.
- Sasa I, Donly KJ. Sealants: a review of thematerials and utilization. J Calif Dent Assoc.2010;38:730–734.
- Oong EM, Griffin SO, Kohn W, Gooch BF,Caufield P. The effect of dental sealants on bacteria levels in caries lesions: a review of the evidence. J Am Dent Assoc. 2008;139:271–278.
- Fleisch AF, Sheffield PE, Chinn C, Edelstein BL,Landrigan PJ. Bisphenol A and related compound sin dental materials. Pediatrics. 2010;126:760—768.
- Siegal M, Farquhar CL, Bouchard JM. PublicHealth Rep. 1997;112:98—106.
- Bertness J, Holt K. Dental Sealant Resource Guide.2nd ed. Washington, DC: National Maternal andChild Oral Health Resource Center; 2006.
From Dimensions of Dental Hygiene. November 2012; 10(11): 30,32.

