
Strategies for Managing Erosive Tooth Wear
Erosive tooth wear can be effectively addressed with minimally invasive dentistry if diagnosed in its early stages.
This course was published in the November 2019 issue and expires November 2022. The authors have no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- Explain the concept of erosive tooth wear, as well as its etiology, clinical manifestations, prevention, and management.
- Discuss clinical considerations when treating dental erosion.
- List treatment strategies for restoring teeth in patients diagnosed with erosive tooth wear.
Erosive tooth wear is a multifactorial condition comprising various clinical terms. To help lend insights into this concept, this article will examine risk factors and management of dental erosion. In 1970, Pindborg1 defined dental erosion as the irreversible loss of tooth structure by a chemical process that does not involve bacteria. Recently, the term biocorrosion has been suggested as more appropriate because it embraces a degradation of tooth substance caused by endogenous and exogenous acids.2 This process, in combination with mechanical wear, such as abrasion and attrition, is collectively known as erosive tooth wear, and it is a public health concern. One study examined 17,061 children, and among those aged 5 and 6, 25% of the primary dentition exhibited erosive tooth wear that involved dentin exposure.3 Diagnosis at an early stage may decrease the risk of wear reaching a pathological state that requires restorative intervention.4
In a carious process, enamel and root dentin begin to decalcify at pH values of 5.2 to 5.5 and 6.7.5,6 However, in an erosive process, decalcification is more complex, as the ionic content (calcium, phosphate, and hydroxyl ions) of saliva and plaque fluid needs to be considered.7 Depending on the salivary concentrations of calcium and phosphate, the critical pH of erosion may range from 5.5 to 6.5.8 In plaque fluid, concentrations of calcium and phosphate are much higher than in saliva, so the critical pH for erosion may be as low as 5.1.7
In broad terms, there are two chief causes of dental erosion: intrinsic and extrinsic. The intrinsic type results from gastric acids entering the oral cavity, most often due to gastroesophageal reflux disease (GERD) or vomiting from eating disorders. The extrinsic type is mainly due to the ingestion of an acidic diet. A thorough medical history is essential to identify the causative factors, and treatment should never be initiated until the factors at play are under control.
INTRINSIC CAUSES
The intrinsic causes are mainly from gastric acids, which can reach a pH value of less than 1. The prevalence of GERD in the adult United States population ranges from 6% to 10%.9 Clinical symptoms of GERD include heartburn, noncardiac chest pain, chronic cough, and hoarseness. Dental erosion is the primary oral clinical manifestation of this condition.9 Early diagnosis and suppression of refluxed acid through lifestyle changes and medications may prevent further damage and potential tooth loss. Systematic reviews have reported the prevalence of dental erosion among GERD-positive patients to range from 32.5% to 48%—with severity correlated to the presence of the GERD symptoms.10,11 Patients receiving a GERD diagnosis should therefore be examined for dental erosion, and interdisciplinary collaboration is imperative when treating these patients.12
Eating disorders, such as anorexia nervosa and bulimia, may also cause dental erosion.13 Patients with eating disorders restrict food intake and/or have episodes of binge eating and vomiting, leading to weight loss, amenorrhea, and a distorted concept of body image. In addition to eroding the teeth, excessive vomiting leads to dehydration and reduced salivary flow. Often, these patients consume acidic drinks to stimulate salivary flow and counteract the bad taste—which adds to the erosive effect.14 Primarily seen on lingual, palatal, and posterior occlusal surfaces, perimolysis is a clinical manifestation of dental erosion; coupled with intrinsic acids, it is often exacerbated by movements of the tongue.15
EXTRINSIC CAUSES
Extrinsic erosion is due to acidic dietary habits. Beverages, such as citrus juice, carbonated drinks, tea, wine, and designer drinks (eg, sparkling juice beverages), have been shown to be erosive. The erosive potential of beverages is not only related to their pH value, as beverage composition and titratable acidity can be even more important.16 Noncola beverages can therefore be far more aggressive than cola-based drinks.16 Commercially available teas can be about as erosive as orange juice (pH = 3.73),17 and several white wines are equally or more erosive than orange juice.18 Designer drinks may pose a considerable erosion problem.19 Sports drinks and energy drinks have even lower pH values and higher titratable acidity than orange juice and soda.20,21

A case report was presented on a patient who used to eat three apples a day, and her maxillary incisors experienced considerable loss of tooth structure.22 Several fruits and vegetables have acidic pH values, and acidic medications are also an extrinsic risk.23 Furthermore, approximately 63% of the most commonly prescribed medications in the US have the potential to cause xerostomia.24 Saliva creates a protective pellicle on the tooth surface that reduces the erosive potential of acidic agents.25 As a result, patients with reduced salivary flow face increased risk of erosion.26,27 The preferred treatment for dry mouth is the use of oral moisturizers to alleviate symptoms, but certain moisturizers can potentially be erosive,28 as some have been shown to have pH values below the critical pH of enamel and dentin.29 Another solution is the use of oral rinses, but a recent study demonstrated the erosive potential of select products due to their acidic pH;30 thus, clinicians are advised to recommend rinses for dry mouth that are pH neutral.
The erosive potential of an acidic diet depends on the habits of consumption. The method of drinking, time to clear the erosive agents, protective salivary capacity, and amount of residual acids can reduce the erosive effect up to 50%.25 The initial erosive effect occurs within the first 3 minutes of exposure, after which the salivary capacity reverses the effect. After swallowing and clearing, a residual amount of acid will be left in the mouth in limited contact with teeth, most likely in the sulcus, where crevicular fluid plays a protective role.31
Upon diagnosis of extrinsic erosion, the causes must be determined. A dietary analysis is a useful tool, and should include at least 4 days—including weekdays and a weekend. A one-to-one dietary intervention is an excellent way to show patients objectively what they are consuming, the frequency of consumption, and provide advice regarding alternatives.32,33
CLINICAL SIGNS
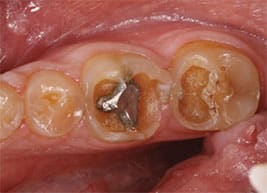
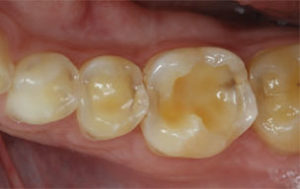
The three main clinical signs of erosion are cupping of cusps, restorations standing proud or alone, and the absence of anatomical features (Figure 1 through Figure 4). The location of these clinical signs must be determined to understand the cause. Intrinsic erosion usually occurs on palatal surfaces of anterior maxillary teeth, facial surfaces of mandibular anterior teeth, and occlusal surfaces of mandibular molars, which is consistent with the pathway of the gastric acids. Extrinsic erosion is generally seen on labial, buccal, and occlusal surfaces. Often the cause is multifactorial, resulting in a more generalized appearance that necessitates a thorough health history and dietary analysis.
The Basic Erosive Wear Examination (BEWE) is the most widely used index.34 In this system, surfaces are scored based on signs of dental erosion, with either a 0 (no signs of erosive wear), 1 (initial loss of surface texture), 2 (distinct defect, with hard tissue loss < 50% of the surface area), or 3 (hard tissue loss of ≥ 50% of the surface area). Only the most severely affected surface of each sextant is scored. The total scores of the sextants are then added and the subject is graded as having no (< 2), low (3–8), medium (9–13), or high (≥ 14) risk level, based on the patient’s total BEWE score. This system is simple and allows clinicians to record and track progression of the condition. Repeated measurements are suggested at 2-year intervals for low-risk patients, and 6-month to 12-month intervals for patients at medium or high risk.

PREVENTION AND MANAGEMENT
When a patient is diagnosed with dental erosion, the clinician should identify whether it is from intrinsic or extrinsic sources, or both. If the condition involves an eating disorder, open communication between the patient and provider must be established using a nonjudgmental approach.13 Multidisciplinary care is the key to treating these individuals, and the role of the oral health professional is to assess the case and make the appropriate referral to a psychologist, nutritionist, and/or physician. Bear in mind that oral health professionals are often the first health care providers to identify these situations, and if they are to help the patient, he or she must admit the problem. If this is not the case, only minor and/or palliative treatment should be considered, as definitive therapy should be postponed until the patient is actively engaged in treatment.
In the case of extrinsic erosion, the patient should be educated about the nature of the condition and encouraged to adjust his or her dietary habits to a less erosive pattern. Acidic consumption should be reduced, with emphasis on reducing the frequency of acid attacks. Highly acidic beverages should be substituted with water or milk ideally, or the mouth at least rinsed with water, fluoride, or bicarbonate after consuming acidic drinks.
Hyposalivation is diagnosed when salivary production drops below 0.1 ml/minute for unstimulated salivary flow or 0.7 ml/minute for stimulated salivary flow.5,35 If salivary production is low, xylitol-containing chewing gum is a readily available adjunct to stimulate salivary flow. In addition to the gum stimulating saliva secretion, xylitol has been shown to be effective in preventing root caries in adults.36 Encouraging adequate hydration is also important. Mouthrinses and oral moisturizers can also be of benefit in alleviating symptoms and aiding remineralization.
When tooth structure is compromised by wear to the point dentin is exposed, remineralization should be encouraged. For example, 5,000-ppm fluoride toothpaste should be prescribed, especially if the patient presents with active caries lesions. Fluoride varnishes remineralize the tooth structure, reduce the critical pH for demineralization by substituting hydroxyapatite with fluorapatite, and can decrease sensitivity where dentin has been exposed.37,38 An additional benefit of fluoride varnishes is that efficacy does not rely on patient compliance.
Abrasion is often a cofactor in erosive tooth wear. Patients should be instructed in nonabrasive oral hygiene methods and preferably delay brushing for 30 minutes to 60 minutes after an acid exposure. Several whitening dentifrices have large abrasive particles to more effectively remove surface stains, so patients should be encouraged to use toothpastes that are relatively nonabrasive, along with soft brushes.39 Lastly, parafunctional habits should be controlled whenever possible; for example, hard or soft occlusal guards should be prescribed if there is evidence of bruxism or clenching.
TREATMENT
The primary focus of the restorative dentist should always be to preserve the remaining dentition. If the patient does not have major esthetic or functional problems, and other causative factors in erosive tooth wear are kept at bay, sealing dentinal exposures on occlusal, facial, or palatal surfaces can go a long way in preserving the remaining dentition.
If functional or esthetic problems are such that greater restorative intervention is needed, modern conservative dentistry dictates that an additive approach should be employed (whenever possible) to preserve tooth structure.40,41 Historical treatment of severe tooth wear was often by means of full-mouth rehabilitation with crowns, a treatment modality often causing more massive tooth structure loss than the causative factors themselves.42 We propose additive adhesive dentistry to affected teeth to simultaneously protect them from further wear, while improving patient-perceived esthetics.
Wear patients may seek dental treatment due to chipped, thin, or short maxillary front teeth. In some cases, there may be inadequate space to build up these teeth, which have often eroded and worn on the palatal surfaces. Two easy approaches are available: If the posterior teeth are relatively unaffected by erosion, the front teeth can be built up with composite resin, either freehand or with the aid of a wax-up and silicone stent. This will temporarily open the occlusion posteriorly. Through a combination of supra-eruption of the posterior teeth and intrusion of the anterior teeth, the teeth will come in to occlusion again, usually over 4 months to 6 months.43 This has been termed the Dahl principle, which was first proposed to gain restorative space in cases with anterior attrition by placing a removable cast appliance on the palatal surfaces on the upper anterior teeth for 4 months to 6 months.44 The same effect can be obtained by using composite resin and doing the anterior buildups directly. If the labial surfaces of the upper maxillary teeth are also affected by erosion, either direct or indirect veneers are the most conservative method of restoring function and esthetics after the proper occlusal relationship has been restored.45
If the posterior teeth are affected by erosive tooth wear, the vertical occlusal relationship can be raised with either direct composite resin or bonded onlays on the affected teeth, thus gaining space to restore the anterior dentition adhesively. Evidence now supports the use of bonded ceramic onlays that defy traditional retention and resistance form, providing a favorable treatment modality for eroded teeth.46 While long-term clinical evidence is still being established, short- to medium-term studies have shown promising results. Numerous case reports have been published in which erosive tooth wear has been successfully restored in a minimally invasive manner using bonded ceramic onlays, palatal, and facial veneers and direct composite, preserving precious tooth structure.
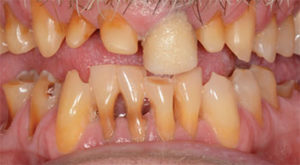
For more severe cases (Figure 5), full-coverage restorations may be the most reasonable treatment. Still, the clinician’s goal should always be to delay invasive treatment for as long as possible—and, whenever possible, detect this condition early and employ preventive measures and minimally invasive treatment modalities to protect what is remaining.
Acknowledgement: The authors would like to thank Terence Donovan, DDS, for his devoted guidance and enthusiastic passion on this topic.
REFERENCES
- Pindborg J. Pathology of Dental Hard Tissues. Philidelphia: Saunders Company; 1970:443.
- Grippo JO, Simring M, Coleman TA. Abfraction, abrasion, biocorrosion, and the enigma of noncarious cervical lesions: a 20-year perspective. J Esthet Restor Dent. 2012;24:10–23.
- Downer MC. The 1993 national survey of children’s dental health. Br Dent J. 1995;178:407–412.
- Amaechi BT, Higham SM, Edgar WM. Influence of abrasion in clinical manifestation of human dental erosion. J Oral Rehabil. 2003;30:407–413.
- Lofgren CD, Wickstrom C, Sonesson M, Lagunas PT, Christersson C. A systematic review of methods to diagnose oral dryness and salivary gland function. BMC Oral Health. 2012;12:29.
- Shay K. The evolving impact of aging America on dental practice. J Contemp Dent Pract. 2004;5:101–110.
- Dawes C. What is the critical pH and why does a tooth dissolve in acid? J Can Dent Assoc. 2003;69:722–724.
- Ericsson Y. Enamel-apatite solubility. Investigations into the calcium phosphate equilibrium between enamel and saliva and its relation to dental caries. Acta Odontol Scand. 1949;8(Suppl 3):1–139.
- Barron RP, Carmichael RP, Marcon MA, Sàndor GK. Dental erosion in gastroesophageal reflux disease. J Can Dent Assoc. 2003;69:84–89.
- Pace F, Pallotta S, Tonini M, Vakil N, Bianchi Porro G. Systematic review: gastro-oesophageal reflux disease and dental lesions. Aliment Pharmacol Ther. 2008;27:1179–1186.
- Milosevic A. Gastro-oesophageal reflux and dental erosion. Evid Based Dent. 2008;9:54.
- Benages A, Muñoz JV, Sanchiz V, Mora F, Minguez M. Dental erosion as extraoesophageal manifestation of gastro-oesophageal reflux. Gut. 2006;55:1050–1051.
- Hazelton LR, Faine MP. Diagnosis and dental management of eating disorder patients. Int J Prosthodont. 1996;9:65–73.
- Hellström I. Oral complications in anorexia nervosa. Scand J Dent Res. 1977;85:71–86.
- House RC, Grisius R, Bliziotes MM, Licht JH. Perimolysis: unveiling the surreptitious vomiter. Oral Surg Oral Med Oral Pathol. 1981;51:152–155.
- von Fraunhofer JA, Rogers MM. Dissolution of dental enamel in soft drinks. Gen Dent. 2004;52:308–312.
- Phelan J, Rees J. The erosive potential of some herbal teas. J Dent. 2003;31:241–246.
- Rees J, Hughes J, Innes C. An in vitro assessment of the erosive potential of some white wines. Eur J Prosthodont Restor Dent. 2002;10:37–42.
- Rees JS, Davis FJ. An in vitro assessment of the erosive potential of some designer drinks. Eur J Prosthodont Restor Dent. 2000;8:149–152.
- von Fraunhofer JA, Rogers MM. Effects of sports drinks and other beverages on dental enamel. Gen Dent. 2005;53:28–31.
- Noble WH, Donovan TE, Geissberger M. Sports drinks and dental erosion. J Calif Dent Assoc. 2011;39:233–238.
- Olafsson VG, Boushell, L.W. Pragmatic esthetics: severe labial erosion corrected with direct composite resin veneers. J Cosmetic Dent. 2014;30:82–90.
- Gandara BK, Truelove EL. Diagnosis and management of dental erosion. J Contemp Dent Pract. 1999;1:16–23.
- Sreebny LM, Schwartz SS. A reference guide to drugs and dry mouth — 2nd edition. Gerodontology. 1997;14:33–47.
- Jensdottir T, Holbrook P, Nauntofte B, Buchwald C, Bardow A. Immediate erosive potential of cola drinks and orange juices. J Dent Res. 2006;85:226–230.
- Plemons JM, Al-Hashimi I, Marek CL, American Dental Association Council on Scientific Affairs. Managing xerostomia and salivary gland hypofunction: Executive summary of a report from the American Dental Association Council on Scientific Affairs. J Am Dent Assoc. 2014;145:867–873.
- Winston AE, Bhaskar SN. Caries prevention in the 21st century. J Am Dent Assoc. 1998;129:1579–1587.
- Delgado AJ, Olafsson VG, Donovan TE. pH and erosive potential of commonly used oral moisturizers. J Prosthodont. 2016;25:39–43.
- Delgado AJ, Olafsson VG. Acidic oral moisturizers with pH below 6.7 may be harmful to teeth depending on formulation: a short report. Clin Cosmet Investig Dent. 2017;9:81–83.
- Delgado AJ, Dias Ribeiro AP, Quesada A, et al. Potential erosive effect of mouthrinses on enamel and dentin. Gen Dent. 2018;66:75–79.
- Lagerlof F, Dawes C. The volume of saliva in the mouth before and after swallowing. J Dent Res. 1984;63:618–621.
- Kidd EA. The use of diet analysis and advice in the management of dental caries in adult patients. Oper Dent. 1995;20:86–93.
- Harris R, Gamboa A, Dailey Y, Ashcroft A. One-to-one dietary interventions undertaken in a dental setting to change dietary behaviour. Cochrane Database Syst Rev. 2012:CD006540.
- Bartlett D, Ganss C, Lussi A. Basic Erosive Wear Examination (BEWE): a new scoring system for scientific and clinical needs. Clin Oral Investig. 2008;12(Suppl 1):65–68.
- Scully C, Felix DH. Oral medicine — update for the dental practitioner: dry mouth and disorders of salivation. Br Dent J. 2005;199:423–427.
- Ritter AV, Bader JD, Leo MC, et al. Tooth-surface-specific effects of xylitol: randomized trial results. J Dent Res. 2013;92:512–517.
- American Dental Association Council on Scientific Affairs. Professionally applied topical fluoride: Evidence-based clinical recommendations. J Am Dent Assoc. 2006;137:1151–1159.
- Weyant RJ, Tracy SL, Anselmo TT, et al. Topical fluoride for caries prevention: executive summary of the updated clinical recommendations and supporting systematic review. J Am Dent Assoc. 2013;144:1279–1291.
- Dzakovich JJ, Oslak RR. In vitro reproduction of noncarious cervical lesions. J Prosthet Dent. 2008;100:1–10.
- Dietschi D, Argente A. A comprehensive and conservative approach for the restoration of abrasion and erosion. Part I: concepts and clinical rationale for early intervention using adhesive techniques. Eur J Esthet Dent. 2011;6:20–33.
- Dietschi D, Argente A. A comprehensive and conservative approach for the restoration of abrasion and erosion. Part II: clinical procedures and case report. Eur J Esthet Dent. 2011;6:142–159.
- Burke FJ, Kelleher MG, Wilson N, Bishop K. Introducing the concept of pragmatic esthetics, with special reference to the treatment of tooth wear. J Esthet Restor Dent. 2011;23:277–293.
- Dahl BL, Krogstad O. The effect of a partial bite raising splint on the occlusal face height. An X-ray cephalometric study in human adults. Acta Odontol Scand. 1982;40:17–24.
- Dahl BL, Krogstad O, Karlsen K. An alternative treatment in cases with advanced localized attrition. J Oral Rehabil. 1975;2:209–214.
- Magne P, Magne M, Belser UC. Adhesive restorations, centric relation, and the Dahl principle: minimally invasive approaches to localized anterior tooth erosion. Eur J Esthet Dent. 2007;2:260–273.
- Politano G, Van Meerbeek B, Peumans M. Nonretentive bonded ceramic partial crowns: concept and simplified protocol for long-lasting dental restorations. J Adhes Dent. 2018;20:495–510.
From Dimensions of Dental Hygiene. November 2019;17(10):34—36,39.



