Reduce White Spot Lesions
Patients undergoing orthodontic treatment are predisposed to early caries development. Here’s how to help your patients prevent incipient tooth decay.
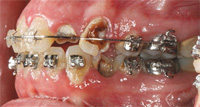
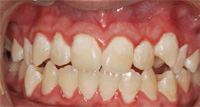
Orthodontic treatment can make tremendous improvements in a patient’s facial esthetics, in addition to increasing oral function. Treatment outcomes, however, can be marred by white spot lesions (Figure 1) or frank cavitation (Figure 2). Although excellent orthodontic results may be achieved, white spot lesions can cause severe esthetic problems that necessitate restorative care. White spot lesions frequently become smaller with time, but they may still be noticeable 12 years after debonding (Figure 3).1
INCREASED RISK DURING ORTHODONTIC TREATMENT
White spot lesions are incipient carious lesions that are visually apparent. They are caused by an imbalance in the remineralization/demineralization cycle that allows demineralization to predominate. This imbalance causes the tooth surface to become porous and rough but because the subsurface loss of minerals is blocked, the tooth surface partially reforms. This creates a change in the reflection of light on the tooth surface in comparison to noncarious enamel and thus, white spots become visible. When the rate of demineralization overcomes the rate of remineralization, the surface of the white spot lesion breaks down, producing frank caries.
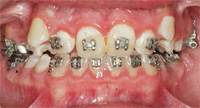
White spot lesions can form within 1 month of the start of orthodontic treatment because of the bacteria and debris that are retained around brackets and in the crevices between orthodontic bands and the enamel.2 Streptococcus mutans and lactobacilli increase dramatically in the biofilm once orthodontic appliances are placed, and contribute to the acidic milieu around the brackets. 3–5 The change in tooth structure encourages biofilm formation while the closure of space between teeth causes gingival tissue to bunch up—reducing access to the area and prohibiting effective cleaning. Biofilm also accumulates in the enlarged sulci. Tooth movement, called intrusion, also results in the massing of gingival tissue and deeper sulci. As the tissue shrinks to normal, white spot lesions are exposed. Brackets positioned close to the gingiva on erupting posterior teeth also make it difficult to clean those teeth, enhancing biofilm buildup. Various elastomeric materials used to hold wires to the brackets or to implement forces to close spaces encourage biofilm accumulation.
LOCATION AND SIZE
The size of the white spot depends on the severity of the carious assault. One study found that the average percentage of tooth surface involved in a white spot lesion was approximately 10% but could range from 0% to more than 50%.6 Robertson et al suggested that incisal edges were most frequently involved, but they did not account for pre-existing enamel opacities in the incisal edges that could be attributed to developmental hypomineralizations and not to carious demineralization.7
White spot lesions are usually found between the bracket and/or wire and the gingiva, suggesting that toothbrushing and interdental cleaning should be focused on these areas. One key to biofilm removal in orthodontic patients is teaching them to angle the brush into the maxillary and mandibular areas between the brackets and the gingiva and to disturb the plaque in those areas with short strokes. Patients should be able to “feel the toothbrush” on their gingiva but should not scrub hard enough to cause recession.
PREVALENCE
Studies report that as many as 37% to 97% of patients with fixed orthodontic appliances have at least one new white spot lesion after therapy.6,8 Considerable variation in the reported prevalence of white spot lesions on smooth surfaces exists because of the teeth examined in the study, the method of detection, and whether post-treatment status is compared to pretreatment status.6
Prevalence is also influenced by patient variables. As such, determining who is most vulnerable should help focus a prevention program. Younger patients tend to have more white spot lesions than older ones,6,9 possibly because young people are less concerned about oral hygiene than their older counterparts.
Some studies show that males have a higher incidence of and more severe cases of white spot lesions than females.6,9–11 Males have poorer oral health and clean their teeth less frequently than females.12 Thus, oral hygiene instructions should be particularly emphasized with male patients. Poor oral hygiene at the time of screening is also a predictor of white spot lesions.6 Dental professionals may want to determine whether orthodontic treatment is urgent or if it can wait until oral hygiene improves. Similarly, prior to placement of orthodontic appliances, the orthodontist should see evidence of continued good oral hygiene.
ORAL HYGIENE COMPLIANCE
Reversion to former bad habits may occur among those with initial poor oral hygiene.6 Therefore, orthodontic patients should frequently visit their general practice to reinforce good hygiene during treatment.6,9 Parents or caregivers of children should become involved in their oral hygiene instruction and should understand that good oral hygiene will minimize the risk of white spot lesions.
To reinforce oral health, one clinic required their patients to provide signed letters from their dental professionals proving they had good periodontal health and were caries-free in order to be accepted into orthodontic treatment.6 However, 36% of these patients still exhibited at least one new white spot lesion in their maxillary eight anterior teeth by the end of treatment. Thus, even patients who start with seemingly good oral health may not maintain it during their orthodontic treatment. Oral hygiene instruction should begin the first day the patient enters the orthodontic office.
Patients and parents should be told in writing and verbally at the beginning of treatment that continued lack of compliance will result in the end of treatment. Reiteration and documentation of this warning might be necessary throughout treatment. In some cases when poor oral hygiene is documented continually, wires can be removed and not reinserted. Patients and their parents are then told that at the next appointment certain expectations must be met in order to have the wires reinserted or debonding will occur.
Lack of compliance with oral hygiene is also associated with termination of treatment prior to achieving treatment goals, although some studies have not replicated this finding.6,13 Patients with white spot lesions are apt to miss more appointments, and treatment is longer than for those without white spot lesions, suggesting that these patients lack cooperation in many areas.6 Lack of compliance with factors such as keeping appointments, wearing the appliances, and oral hygiene all contribute to the deterioration of oral health. The risk of white spot lesions grows in direct response to longer treatment times, higher number of missed appointments, and greater incidence of poor compliance or poor oral hygiene.6,13
BIOFILM DISTURBANCE
Preventing white spot lesions is complex due to compliance problems. Because biofilm is a cause of white spot lesions, patient education should focus on effective means of preventing its formation. An effective patient education program will also consider patients’ finances and lifestyle.
Who is responsible for disturbing biofilm formation—the dental professional or the patient? It is not practical to think patients can keep weekly appointments due to cost and compliance. However, all orthodontic patients should be provided with appropriate oral hygiene instruction and self-care tools, which should be reinforced at each dental and orthodontic appointment. Patients should demonstrate to the dental professional that they can clean around the braces.
Recommendations for biofilm removal can be simple. Powered toothbrushes can be recommended and patients should be taught to pay special attention to areas most susceptible to demineralization, although the rest of the oral cavity must not ignored.14 Buccal surfaces of the canines, premolars, and central incisors may be most at risk, but more research is needed to determine this.2,6,15,16
FLUORIDE
Topical fluoride agents are frequently prescribed to prevent white spot lesions in orthodontic patients. Systematic reviews suggest that a daily fluoride mouthrinse is effective in reducing the incidence and severity of white spot lesions.17 Unfortunately, compliance, which is critical to the effectiveness of this method, is often low. In addition, the presence of fluoride in the environment is so ubiquitous that it is difficult to discern the effects of another form of fluoride delivery (eg, varnish, gels) on white spot lesion formation. More well-designed clinical research is needed to define the effectiveness of topical fluorides in orthodontic patients.18
Fluoride toothpaste is a widely available and is an effective anticaries agent.19,20 The rate of demineralization in orthodontic patients normally far exceeds the remineralization potential of the usual twice per day fluoride toothpaste application.21 To improve the efficacy of fluoride dentifrice in an orthodontic patient population, Al Mulla et al encouraged patients at each appointment to smear 1 gm of 1,450 ppm fluoride toothpaste (amount contained in most over-the-counter fluoride dentifrices) over all the teeth prior to brushing, brushing for 2 minutes, and then taking a small quantity of water into the mouth and swishing it between the teeth for 30 seconds before expectorating.21 Patients were instructed not to rinse with additional water or eat or drink for 2 hours. The control group had five times to six times more new carious lesions than the experimental group after 2 years of treatment. Within the treatment group, the individuals who complied more with the regimen had a lower caries incidence than those with poor compliance. The success of this method may be attributed to maintaining the salivary fluoride levels for a longer time period by swishing for the extra 30 seconds and to not rinsing, eating, or drinking following the toothpaste application. This technique may be particularly effective prior to bedtime because of the reduced salivary flow that occurs during sleeping.21 Using fluoride dentifrice in this manner is cost-effective and practical for most patients because it requires cleaning only twice per day and just using toothpaste.
Varnishes containing either fluoride or chlorhexidine are also recommended to minimize white spot lesions in orthodontic patents.22,23 Fluoride varnishes require minimal patient compliance because they are professionally applied during the appointment. Application is easy and the only objection is a transient discoloration depending on the varnish used.24 The efficacy of chlorhexidine varnishes in preventing decay appears to depend on its concentration and frequency.24 Similar to other chlorhexidine products, the staining of both the tongue and the teeth occur, as well as temporary dysgeusia.24
Various orthodontic materials are designed to minimize white spot lesions by releasing fluoride, which might help remineralize the enamel. Studies testing the clinical effect of these materials, such as bracket cements on white spot lesion formation, however, do not address biofilm formation.18 Similarly, clinical trials testing materials such as fluoridated vs nonfluoridated elastics analyze white spot lesions, not biofilm, as the final outcome.18 More research is needed to determine the benefits of these materials. Some evidence does show that the use of glass ionomer cement for bonding brackets is more effective in preventing white spot lesions than conventional composite cements.18
CONCLUSION
White spot lesions and caries remain a problem in orthodontic patients despite advances in caries prevention agents and continued education on the topic. These lesions are mainly associated with poor oral hygiene and should be preventable. Prevention of white spot lesions is the combined responsibility of dental professional, patients, and their parents or caregivers in the case of children. Dental professionals are responsible for explaining the caries process and its effects on oral health, how to prevent decay, and the tenets of a successful self-care regimen, while monitoring patients throughout treatment, but, ultimately, the task of ensuring good oral health rests with the patient.
REFERENCES
- Shungin D, Olsson AI, Persson M. Orthodontic treatment-related white spot lesions: a 14-year prospective quantitative follow-up, including bonding material assessment. Am J Orthod Dentofacial Orthop. 2010;138:136.e1–8.
- Ogaard B, Rolla G, Arends J. Orthodontic appliances and enamel demineralization. Part 1. Lesion development. Am J Orthod Dentofacial Orthop. 1988;94:68–73.
- Bloom RH, Brown LR Jr. A study of the effects of orthodontic appliances on the oral microbial flora.Oral Surg Oral Med Oral Pathol. 1964;17:658–667.
- Corbett J, Brown L, Keene H, Horton I. Comparison of Streptococcus mutans concentrations in non-banded and banded orthodontic patients. J Dent Res.
- Lundstrom F, Krasse B. Streptococcus mutans and lactobacilli frequency in orthodontic patients; the effect of chlorhexidine treatment. Eur J Orthod. 1987;9:109–116.
- Chapman JA, Roberts WE, Eckert GJ, Kula KS, Gonzalez-Cabezas C. Risk factors for incidence and severity of white spot lesions during treatment with fixed orthodontic appliances. Am J Orthod Dentofac Orthop. 2010;138:188–194.1981;60:1936–1942.
- Robertson MA, Kau CH, English JD, Lee RP, Powers J. MI Paste Plus to prevent demineralization in orthodontic patients: a prospective randomized controlled trial. Am J Orthod Dentofacial Orthop. 2011;140:660–668.
- Boersma JG, van der Veen MH, Lagerweij MD, Bokhout B, Prahl-Andersen B. Caries prevalence measured with QLF after treatment with fixed orthodontic appliances: influencing factors. Caries Res. 2005;39:41–47.
- Al Maaitah EF, Adeyemi AA, Higham SM, Pender N, Harrison JE. Factors affecting demineralization during orthodontic treatment: A post-hoc analysis of RCT recruits. Am J Orthod Dentofacial Orthop. 2011;139:181–191.
- Tufekci E, Dixon JS, Gunsolley JC, Lindauer SJ. Prevalence of white spot lesions during orthodontic treatment with fixed appliances. Angle Orthod. 2011;81:206–210.
- Yazdani R, Vehkalathi MM, Nouri M, Murtomaa H. Smoking, tooth brushing and oral cleanliness amont 15-year-olds in Tehran, Iran. Oral Health Prev Dent. 2008;6:45–51.
- Nanda RS, Kierl MJ. Prediction of cooperation in orthodontic treatment. Am J Orthod Dentofacial Orthop. 1992;102:15–21.
- Richter AE, Arruda AO, Peters MC, Sohn W. Incidence of caries lesions among patients treated with comprehensive orthodontics. Am J Orthod Dentofacial Orthop. 2011;139:657–664.
- Deery C, Heanue M, Deacon S, et al. The effectiveness of manual versus powered toothbrushes for dental health: a systematic review. J Dent. 2004;32:197–211.
- Lovrov S, Hartrich K, Hirschfelder U. Enamel Demineralization during Fixed Orthodontic Treatment – Incidence and Correlation to Various Oral-hygiene Parameters. J Orofac Orthop. 2007;68:353–363.
- Gorelick L, Geiger AM, Gwinnett AJ. Incidence of white spot formation after bonding and banding. Am J Orthod. 1982;81:93–98.
- Benson PE, Parkin N, Millett DT, Dyer F, Vine S, Shah A. Fluorides for the prevention of white spots on teeth during fixed brace treatment. Cochrane Database Syst Rev. 2004;(3):CD003809.
- Benson PE, Shah AA, Millett DT, Dyer F, Parkin N, Vine RS. Fluorides, orthodontics and demineralization: a systematic review. J Orthod. 2005;32:102–114.
- Marinho VC, Higgins JP, Sheiham A, Logan S. Fluoride toothpastes for preventing dental caries in children and adolescents. Cochrane Database Syst Rev. 2003;CD002278.
- Twetman S, Axelsson S, Dahlgren H, et al. Caries-preventive effect of fluoride toothpaste: a systematic review. Acta Odontol Scand. 2003;61:347–355.
- Al Mulla AH, Al Kharsa S, Birkhed D. Modified fluoride toothpaste technique reduces caries in orthodontic patients: A longitudinal, randomized clinical trial. Am J Orthod Dentofacial Orthop. 2010;138:285–291.
- Stecksen-Blicks C, Renfors G, Oscarson ND, Bergstrand F, Twetman S. Caries-preventive effectiveness of a fluoride varnish: a randomized controlled trial in adolescents with fixed orthodontic appliances. Caries Res. 2007;41:455–459.
- Ogaard B, Larsson E, Glans R, Henriksson T, Birkhed D. Antimicrobial effect of a chlorhexidine-thymol varnish (Cervitec) in orthodontic patients. A prospective, randomized clinical trial. J Orofac Orthop. 1997;58:206–213.
- Madlena M. The Importance and Possibilities of Proper Oral Hygiene in Orthodontic Patients. In: Orthodontics – Basic Aspects and Clinical Considerations. Rijeka, Croatia: InTech. 2012:69–110.
From Dimensions of Dental Hygiene. July 2012; 10(7): 28, 30, 32.

