
Promote Remineralization
Here are strategies to expand your caries management protocol.
Gone are the days of managing dental caries by only surgical and restorative intervention. With increased understanding of the caries process, more effective therapeutic modalities have become available that not only intervene when lesions are in their earliest stages, but also contribute to their reversal by promoting remineralization.1
Dental caries is a dynamic, multi-factorial process that starts in the biofilm. The first goal in caries management is to prevent disease progression by ending the ongoing process, followed by prevention and repair through remineralization. Effective caries management is based on the early detection of visible changes in tooth tissues, with meticulous documentation of severity, extent, and activity of the lesion, in addition to other factors, such as patient history. Documenting the lesion’s activity is crucial to diagnosis. Initial risk assessment and subsequent recare appointments are part of an effective continuum of care. Remineralization of active, noncavitated lesions is the ultimate goal.
REMINERALIZATION THERAPY
Acid-producing bacteria in dental biofilm cause the minerals in tooth tissues to dissolve. Frequently switching demineralization/remineralization cycles at the tooth surface are normal physiologic occurrences that occur numerous times per day. In a healthy mouth, these cycles are in balance, with saliva providing a constant supply of calcium, phosphate, and fluoride minerals to assist remineralization of the partly dissolved apatite crystals.2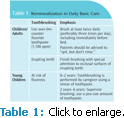
In a caries-inducing oral environment, however, this balance tilts toward demineralization, leading to subsurface porosities. If these conditions are allowed to continue, the incipient, noncavitated lesion will progress until the surface collapses and a cavity is created. The constant battle between mineral dissolution (demineralization) and mineral uptake (remineralization) at the tooth-biofilm interface consists of continual ion-exchange across this interface. This demineralization/remineralization process takes place both at external tooth surfaces (enamel and root surface) and internally in the dentin (cavitated lesions, caries associated with restorations). Bioactive restorative materials can also induce remineralization.
Generally, carious lesions do not develop rapidly (other than in erupting teeth or in the case of hyposalivation). Lesions may take 3 years to 4 years to become cavitated, providing clinicians with unique opportunities for successful intervention during the initial phase of lesion formation. Remineralization therapy in this phase leads to uptake of minerals in the tissues, resulting not only in repair and strengthening of the porous tooth structure, but also in increased acid resistance. The subtle rearrangement of crystals and redeposition of dissolved minerals in the subsurface lesion parts make the remineralized tooth surface less susceptible to renewed caries attacks. Most of the remineralization occurs at the surface, leaving a sealed porous subsurface underneath.3
Contemporary management strategies are based on interpretation of lesion activity and future caries risk. Early detection is crucial for successful, noninvasive lesion management.4 Focused clinical assessment and diagnosis of early lesions might be time-consuming, but they are rewarded with positive results.
More recent treatment strategies include calcium-based technologies. These technologies need additional study, but the body of evidence supporting their efficacy continues to grow. Insufficient evidence does not necessarily mean that the intervention does not work. Rather, a lack of evidence may be related to an insufficient number of well-designed clinical studies investigating the intervention or, for example, when efficacy has only been shown for a specific subset of the population.1
Overtreatment of remineralized, white, or brown “tissue scars” should be avoided. These arrested, nonactive lesions do not need management. Their surface layer is more acidresistant than sound enamel. Greater awareness of this phenomenon will help reduce the perceived need for remineralization intervention and avoid therapeutic overtreatment.
ENCOURAGING REMINERALIZATION
The dental professional’s goal is to assist the natural, daily demineralization/remineralization cycles to shift toward remineralization activity and reverse early carious lesions. Because caries is an infectious disease, the process can be interrupted and arrested by modifying the biofilm through changes in local or oral environment. Basic prevention (Table 1) includes plaque-removal and plaque-reducing strategies, and stimulation of salivary flow (sugarfree, polyol-containing chewing gum). These cleaning strategies expose the tooth surface to a healthy amount of saliva, which delivers minerals to the tooth surface, thus promoting local remineralization.
Reduction in bacterial acid production will influence the local dynamics of ion-exchange at the tooth surface, and encourage remineralization. Patients should be advised to brush at least twice per day, regardless of age or health status. Daily toothbrushing with fluoride toothpaste keeps plaque build-up under control while delivering additional fluoride ions to the exposed clean surface (Table 1). Elevated levels of fluoride in the oral environment should be considered active chemical treatment for carious tissues. Daily cleaning with fluoride toothpaste will help convert active carious lesions in enamel and dentin into inactive lesions. The positive effects of simple oral hygiene measures should be emphasized to at-risk patients (Table 2).5,6
Little or no exposure to fluoride constitutes an elevated risk of caries. The use of fluoride toothpaste is a cost-effective way to control caries.7 This strategy enhances plaque removal while facilitating remineralization of the tooth surface. Frequent presence of small amounts of fluoride at the tooth surface promotes effective remineralization. This prompts the “Spit, but don’t rinse” recommendation. After excess toothpaste has been spit, the remainder will continue to facilitate remineralization, and may result in up to a 26% reduction in the incidence of approximal caries.9 This is particularly important for erupting teeth. After eruption into the oral cavity, local conditions, in combination with saliva, modify the composition of the enamel surface and lead to enamel maturation. The matured tooth surface is then less soluble and more resistant to caries challenges.10–13
Exposing dentin surfaces to the oral environment results in a similar maturation effect. After gingival recession, the cementum is rapidly worn away, exposing the dentin surface to similar demineralization/remineralization cycles. This creates a root surface augmented with minerals, which significantly reduces permeability and caries susceptibility. Rigorous cleaning with fluoride toothpaste may revert active root dentin lesions into hard, leathery, inactive lesions.6 Likewise, caries-affected dentin in cavitated lesions can arrest and remineralize when the local cariogenic conditions change. For example, an open, advanced lesion that has lost its walls will expose the dentin to the self-cleansing actions of chewing and saliva. Because the biofilms are no longer able to accumulate for significant amounts of time, the now-exposed dentin lesions will remineralize and arrest. Another example is the alternative nonrestorative caries management strategy of “opening of contact areas” among patients with rampant caries in the deciduous dentition.14
A different approach to arrest lesions and protect tooth surfaces from demineralization is sealing of the surface through the application of a resin sealant. Sealants provide an impenetrable barrier, completely blocking off the biofilm from the tooth. The effectiveness of sealants in managing noncavitated and cavitated caries lesions is overwhelming: sealants resulted in caries reduction of about 71% up to 5 years after placement.15 Both sealing of the caries process and sealing of restorations appear to be highly effective in conserving sound tooth tissue and providing protection of hard tooth tissues against caries progression.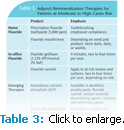
A glass ionomer sealant encourages remineralization and maturation of the underlying enamel. Among noncompliant patients with moderate to high caries risk, sealant application may be the preferred option. Once a resin sealant is applied to the lesion, however, the protected tooth surface can no longer be remineralized. This is also true for resin-infiltrated lesions. The protective resin film inhibits the ion-exchange with saliva and biofilm fluids in both directions—not only shielding the enamel from bacterial acid challenge, but concurrently barring the potential for remineralization.
Additional caries reduction can be achieved when fluoride toothpaste is combined (either at home or via in-office application) with other topical fluorides, such as mouthrinses, gels, and varnish.11 These are essential parts of any caries control program (Table 3).
High concentration prescription fluoride toothpaste and fluoride mouthrinses may benefit adults with active caries who have difficulty cleaning their teeth adequately. For patients with hyposalivation and/or burning mouth syndrome, alcohol-free products should be recommended.12
Fluoride levels should be kept elevated as often as possible, thus the daily addition of a third fluoride boost through extra brushing with high-concentration fluoride toothpaste, fluoride mouthrinse, or other applications (eg, tablets, gels), may be indicated. Strong evidence13 supports professional application of topical fluorides as an effective caries control measure. Fluoride gel and foam should be applied for 4 minutes to gain the full effect.
Fluoride varnish should be applied two to four times per year among moderate to high caries risk patients.16 Complementary preventive strategies, such as sealants, fluoride varnish, and toothbrushing, are also indicated. Currently, the evidence to support fluoride varnish is strong and mounting. Due to ease of application and eliminating the need for at-home compliance, fluoride varnish may soon be the preferred mode of adjunct fluoride delivery instead of gels and foams.
CALCIUM-BASED TECHNOLOGIES
Calcium-based products for the remineralization of caries show considerable promise. In addition to fluoride, calcium and phosphate ions are needed to achieve remineralization. The calcium and phosphates in saliva are the primary source for recrystallizing minerals while fluoride facilitates and assists the remineralization process. With hyposalivation, however, supplementing fluorides with home applications of bioactive calcium phosphate complexes may greatly assist remineralization.
Amorphous calcium phosphates (ACP), casein phosphopeptides (CPP)-ACP, calcium sodium phosphosilicate, and tri-calcium phosphate have shown potential benefits. They may serve as effective adjuncts to fluoride treatment in the noninvasive management of early carious lesions. Many are currently used to treat dentinal hypersensitivity, though additional research is needed to validate their efficacy in caries management.17,18
A recent clinical study reported an alternative therapy for treating incipient proximal lesions.19 The study used a simple, low-cost, noninvasive method to deliver supplemental minerals. Using orthodontic elastics to separate and open approximal contacts, glass ionomer cement (GIC) was applied directly to carious lesions. The study demonstrated that the application of GIC to early noncavitated proximal carious lesions inhibited the progression and enhanced the regression of the lesions. Application of GIC to proximal lesions is a viable method in cases where home use of remineralizing products is not feasible, or where poor patient compliance is anticipated. Further studies, however, will be necessary to define the long-term clinical effects of GIC on the progression of initial proximal caries.
DENTAL EROSION
Dental erosion is characterized by the irreversible loss of tooth structure due to chemical dissolution by acids not of bacterial origin. Remineralization requires the presence of partly demineralized apatite crystals that grow back to their original size. Entirely new crystals are rarely formed.20 At eroded surfaces, the enamel is etched away layer by layer, and crystals are lost layer by layer. As such, erosion lesions are not likely to remineralize, even when exposed to mineral-saturated saliva for long periods of time. Though fluoride does not contribute to the remineralization of eroded surfaces, there is convincing evidence that it can strengthen teeth against erosive acid damage.
Oral hygiene measures influence the progress of erosive lesions. When erosion is a problem, patients should avoid toothbrushing immediately after an erosive challenge. Instead, patients should be encouraged to brush before the acid challenge, using a soft toothbrush and low abrasive toothpaste. This procedure does not completely remove the pellicle, and the pellicle is thus able to continue its protective function when the erosive attack follows.21 After acid intake (eg, soft drinks, wine), patients can stimulate saliva flow by chewing gum or lozenges and postponing toothbrushing. Periodic use of fluoride mouthrinse and concentrated topical fluoride are advised. Fluoride toothpastes, high-concentration fluoride agents, and/or frequent fluoride applications are potentially effective approaches in preventing dental erosion.22
MINERAL ADDITIONS TO WHITENING GELS
Over the past decade, tooth whitening products have become widely available in the United States, and vital tooth whitening has become a common procedure in daily clinical practice. Whitening agents use active ingredients, such as carbamide peroxide and hydrogen peroxide, to effectively whiten teeth. Tooth whitening, however, may cause side effects, such as dentinal hypersensitivity and morphological and chemical alterations of the enamel surface (eg, decrease in calcium and fluoride content, reduced microhardness, and increased surface roughness).
Enamel is susceptible to mineral changes during whitening treatment. The recent addition of fluoride, calcium, and phosphate to whitening agents is designed to minimize mineral loss in the enamel and dentin. The use of remineralizing gels after whitening can significantly enhance the naturally occurring remineralization by saliva, rapidly enhance microhardness, and reduce roughness of the whitened enamel.27
HIGH-RISK PATIENTS
Patients require individually-tailored management to effectively prevent and manage the caries disease process. Patients at high risk of caries include: children with erupting teeth and immature enamel; patients with appliances (fixed and removable orthodontics, removable partial dentures); patients with newly exposed root surfaces after periodontal surgery; older adults with root caries; and all individuals who suffer from hyposalivation (due to medication, xerostomia, radiation, etc).
Among high caries risk patients, the saliva and thus the biofilm fluids should be saturated with minerals that will tip the balance toward remineralization when cariogenic conditions arise. Both at-home and professional applications might be advised (Table 4). More frequent fluoride boosters (eg, applying fluoride varnish four times per year) will benefit these patients.
STRATEGY OVERVIEW
Caries activity and risk assessment are vital to the development of an effective caries management strategy. Once the correct strategy has been decided, patient compliance is key to a successful longterm outcome. Encouraging communication and monitoring compliance are integral parts of effective caries management and maintenance plan. If compliance or monitoring is problematic, sealants are strongly recommended for all at-risk surfaces. Fluoride remains the most widely used agent for managing the remineralization process, but adjunct calcium and phosphate technologies may also help enhance remineralization.
REFERENCES
- Peters MC. Strategies for noninvasive demineralized tissue repair. Dent Clin North Am. 2010;54:507–525.
- González-Cabezas C. The chemistry of caries: remineralization and demineralization events with direct clinical relevance. Dent Clin North Am. 2010;54:469–478.
- Larsen MJ, Fejerskov O. Chemical and structural challenges in remineralization of dental enamel lesions. Scand J Dent Res. 1989;97:285–296.
- Pitts NB. Review of the ICW-CCT meeting, the importance of early detection and the philosophy/approach of ICDAS. In: Stookey GK, ed. Early Detection of Dental Caries. Indianapolis: Indiana University School of Dentistry; 2003:1–17.
- Ekstrand KR, Christiansen ME. Outcomes of a non-operative caries treatment programme for children and adolescents. Caries Res. 2005;39:455–467.
- Nyvad B, Fejerskov O. Active root surface caries converted into inactive caries as a response to oral hygiene. Scand J Dent Res. 1986;94:281–284.
- Wong MC, Clarkson J, Glenny AM, Lo EC, Marinho VC, Tsang BW, Walsh T, Worthington HV. Cochrane reviews on the benefits/risks of fluoride toothpastes. J Dent Res. 2011;90:573–579.
- Marinho VC. Cochrane reviews of randomized trials of fluoride therapies for preventing dental caries. Eur Arch Paediatr Dent. 2009;10:183–191.
- Sjögren K, Birkhed D, Rangmar B. Effect of a modified toothpaste technique on approximal caries in preschool children. Caries Res. 1995;29:435–441.
- Marinho VC, Higgins JP, Sheiham A, et al. One topical fluoride (toothpastes, or mouthrinses, or gels, or varnishes) versus another for preventing dental caries in children and adolescents. Cochrane Database Syst Rev. 2004;1:CD002780.
- Adair SM. Evidence-based use of fluoride in contemporary pediatric dental practice. Pediatr Dent. 2006;28:133–142.
- NIH-NIDCR Fact Sheet: Burning Mouth Syndrome. Available at: www.nidcr.nih.gov/OralHealth/Topics/Burning/BurningMouthSyndrome.htm. Accessed September 26, 2011.
- American Dental Association Council on Scientific Affairs. Professionally applied topical fluoride: Evidence-based clinical recommendations. J AmDent Assoc. 2006;137:1151–1159.
- Peretz B, Gluck G. Early childhood caries (ECC): a preventive-conservative treatment mode during a 12-month period. J Clin Pediatr Dent. 2006;30:191–194.
- Griffin SO, Oong E, Kohn W, et al. The effectiveness of sealants in managing caries lesions. J Dent Res. 2008;87:169–174.
- Azarpazhooh A, Main PA. Fluoride varnish in the prevention of dental caries in children and adolescents: a systematic review. J Can Dent Assoc. 2008;74:73–79.
- Zero DT. Recaldent—evidence for clinical activity. Adv Dent Res. 2009;21:30–34.
- Azarpazhooh A, Limeback H. Clinical efficacy of casein derivatives: a systematic review of the literature. J Am Dent Assoc. 2008;139:915–924.
- Trairatvorakul C, Itsaraviriyakul S, Wiboonchan W. Effect of glassionomer cement on the progression of proximal caries. J Dent Res. 2011;90:99–103.
- Ten Cate JM, Larsen MJ, Pearce EIF, Fejerskov O. In: Fejerskov O, Kidd EAM, eds. Dental Caries: the Disease and its Clinical Management. 2nd ed. Oxford, England: Blackwell Munksgaard; 2008:49–68.
- Joiner J, Schwarz A, Philpotts CJ, Cox TF, Huber K, Hannig M. The protective nature of pellicle towards toothpaste abrasion on enamel and dentine. J Dent. 2008;36:360–368.
- Magalhães AC, Wiegand A, Rios D, Buzalaf MA, Lussi A. Fluoride in dental erosion. Monogr Oral Sci. 2011;22:158–170.
- Magalhães AC, Moraes SM, Rios D, Buzalaf MA. Effect of ion supplementation of a commercial soft drink on tooth enamel erosion. Food Addit Contam Part A Chem Anal Control Expo Risk Assess. 2009;26:152–156v
- Manton DJ, Cai F, Yuan Y, Walker GD, Cochrane NJ, Reynolds C, Brearley- Messer LJ, Reynolds EC. Effect of casein phosphopeptide-amorphous calcium phosphate added to acidic beverages on enamel erosion in vitro. Aust Dent J. 2010;55:275–279.
- Pinheiro HB, Cardoso PEC. Influence of five home whitening gels and a remineralizing gel on the human enamel and dentin ultrastructure and hardness. Am J Dent. 2011;24:131–137.
- Cavalli V, Rodrigues LK, Paes-Leme AF, Brancalion ML, Arruda MA, Berger SB, Giannini M. Effects of bleaching agents containing fluoride and calcium on human enamel. Quintessence Int. 2010;41:157–165.
- Borges AB, Samezima LY, Fonseca LP, Yui KC, Borges AL, Torres CR. Influence of potentially remineralizing agents on bleached enamel microhardness. Oper Dent. 2009;34:593–597.
From Dimensions of Dental Hygiene. October 2011; 9(10): 42-47.

