
A Modern Approach to Periodontal Debridement
Using both ultrasonic and manual instrumentation is the most effective treatment protocol when treating periodontal patients.
Blended instrumentation entails the use of both hand and ultrasonic instruments for efficacious scaling and root planing (SRP), as well as debridement procedures during periodontal maintenance. Hand instrumentation has been the accepted technique for the demanding task of root debridement since the introduction of the curet in 1916.1 The emergence of the ultrasonic scaler in 1958 should have impacted dental hygiene2 but widespread use of ultrasonics was slow to occur. Seven years following the original publications on ultrasonic scalers, Green and Sanderson described the many benefits of using ultrasonic debridement during patient care.3 They were the first to document less patient fatigue and discomfort while receiving ultrasonic debridement, as well as improved operator visualization.3
In the early 1990s, ultrasonic instrumentation became an accepted modality of SRP due primarily to an evolution in the size and shape of the ultrasonic tip. Technological improvements in the shape of ultrasonic tips have changed the practitioner’s approach in providing care to patients who require SRP and periodontal maintenance. A wide assortment of tips is available today, from thinner tips used in subgingival instrumentation to inserts that are safe to use on implants.
Potential Risks
One of the practitioner’s concerns during SRP is the risk of extensive root surface damage that can occur. The ultrasonic scaler used with a standard sized insert can damage the root surface more extensively than any other type of instrumentation.4 Standard sized inserts are appropriate for supragingival deposits but not for root surface debridement. Another potential consideration is the loss of attachment from instrumentation, known as critical probing depths.5 When scaling is completed in a sulcus depth that is less than 2 mm, loss of attachment can result.5 All of this information demonstrates the need for a sequenced approach to treatment. Using a combination of both hand and ultrasonic instruments will facilitate the achievement of the desired result.
Treating plaque-induced gingivitis
Plaque-induced gingivitis is the most common form of gingival disease seen by the dental hygienist. It is characterized by an inflammation of the gingiva as a result of bacterial biofilm at the gingival margin. Calculus may be present. Although the clinical signs of gingivitis may vary between patients, the key factor distinguishing gingivitis from periodontitis is the lack of attachment loss. Probing depth may be modest, ie, 2 mm-3 mm or significantly greater than 3 mm, due to gingival enlargement through edema or hypertrophy. No clinical or histologic evidence of apical migration of the epithelial attachment will exist. Radiographically, no bone loss is seen. 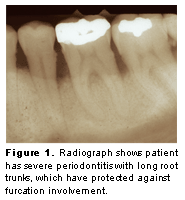
The treatment protocol for this type of disease may begin with ultrasonic instrumentation or hand instrumentation. If gross deposits exist, standard sized ultrasonic tips may be used. The tooth surfaces should then be evaluated with an instrument of the practitioner’s choice. An excellent choice is the Number 11-12 explorer, a probe, or curet. Moderate to light residual deposits should be removed with care using a variety of curets or fine ultrasonic tips. After deposit removal, a sickle scaler may be used to remove residual calculus or interproximal staining between the anterior teeth. If stain is still present, the final steps can include polishing followed by fluoride treatment.
Chronic periodontitis
Chronic periodontitis is a plaque-related disease, like gingivitis, but is defined by loss of attachment. The gingival tissues are usually red and swollen, but if the patient has fibrotic tissue, this may not be present. Chronic periodontitis was originally considered an age-related phenomenon, but is now known to involve host resistance factors in response to the periodontal pathogens present. If the patient has greater than 30% of sites with attachment loss, the patient has generalized disease. Attachment loss affecting less than 30% of sites is considered localized disease. Additionally, the amount of attachment loss can define the severity of periodontitis. Attachment loss of 4 mm indicates mild disease, 5 mm indicates moderate disease, and attachment loss of 6 mm or more indicates severe disease, according to Lindhe et al.5 Pocket depth cannot be used alone to determine the extent of the disease process because conditions like edema and hypertrophy can contribute to pocket depth but are not reflective of attachment loss.
Moderate to severe disease usually demonstrates bone loss radiographically. Furcation bone loss may also be noted. Furcation bone loss is not only dependent on the horizontal height of bone but also on the length of the root trunk. Root trunk length can be determined from radiographs, however, furcation involvement is best determined clinically with an instrument such as a Nabors probe. The horizontal depth of the furcation should be measured in millimeters and recorded. Clinical furcation involvement may or may not be noted radiographically. Figure 1 shows a patient with severe periodontitis and long root trunks. In this case, the long root trunks have protected against furcation involvement. The patient in Figure 2 has moderate probing depths but because of short root trunks, bone loss occurs in the furcation area. Furcation bone loss complicates the treatment and outcomes.
The average length of the root trunk from the CEJ to the entrance of the furcation on the maxillary first molars is 3 mm on the mesial, 4 mm on the facial, and 5 mm on the distal. On the mandibular first molar, the average length of the root trunk from the CEJ to the entrance of the furcation on the facial is 3 mm and 4 mm on the lingual.6 Early chronic periodontitis usually does not demonstrate furcation bone loss. Patients with periodontitis complicated by furcation involvement should be referred to a periodontal specialist as soon as possible. Surgical bone grafting is most successful for early furcation invasion.
Suggestions on Treatment Protocols
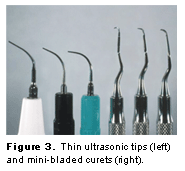
The treatment protocol for patients with chronic periodontitis can begin with ultrasonic instrumentation with standard sized tips for removal of any supragingival deposit. The next step should involve subgingival instrumentation with thinner tips used with sufficient power according to deposit characteristics. (Figure 3). When using power instrumentation, the preferred setting is the lowest power setting that still allows the deposit to be removed. Chapple et al7 showed that a half power setting is as effective as using the ultrasonic scaler at full power.
After thorough debridement with the thinner tips, the root surfaces should then be evaluated and debridement should be continued with hand instrumentation using area-specific curets. The selection of the curet is based on the topography of the pocket. Standard sized curets can be used in deep, wide pockets. Mini curets should be used in narrow pockets (Figure 3). A fine tipped explorer is useful at this point to evaluate the root surface. After final hand instrumentation for deposit removal, the thin ultrasonic tips can be used again on a low setting to remove any smear or sludge from the root surface and to smooth the root surface. Diamond files may be used by hand as the final finishing instrumentation to achieve a smooth root surface free of all deposit or smear layer. In a moderate or severe case, an antimicrobial agent can be used. Optional final steps are polishing the teeth and application of fluoride.
The more advanced the disease, the longer initial treatment will take. An early case of chronic periodontitis may only take the practitioner 11/2 hours of instrumentation. An efficient protocol for a moderate case is two visits, each lasting 11/2 to 2 hours. The right side of the mouth can be completed in one visit and then the left side can be completed at the next visit. In a severe case, three 2-hour or four 11/2-hour visits may be necessary. It is difficult, if not impossible, to establish absolute guidelines for how long a specific case may take to instrument well. Many variables exist, including tenacity of deposit, difficult access to the root surfaces due to root anatomy, pocket depth, existing over-contoured restorations, and degree of inflammation. Instrumentation continues until the root is as free of deposit as possible, given the local conditions, time available, and the clinician’s skill level.
Severe chronic periodontitis is the most difficult to treat. Often, several teeth may be lost. Referral to a periodontal specialist is the best treatment plan for the severe chronic periodontal patient.
Conclusion
Blended instrumentation is the modern approach to treatment. It allows for the gross removal of deposits supragingivally without damage to the root surface. In more advanced cases, thinner tips are used on root surfaces to remove deposits. Thinner tips with sufficient power can remove the most calculus with the least amount of root surface damage.4 The subsequent hand instrumentation step allows for adaptation into root flutes and irregular root surfaces. Advances in hand instrument design allow for better adaptation to the root surfaces.8 Finishing with irrigation using modified tips on a low setting removes debris remaining after hand instrumentation and smoothes the root surface. This blended instrumentation protocol can also be modified with the use of medicaments and/or other hand instruments. The goal is efficacious treatment and improvement of the periodontal health of our patients.
Acknowledgement
Thank you to Janet M. Guthmiller, RDH, DDS, PhD, of the University of Iowa School of Dentistry for her help with this article.
REFERENCES
- Mooney, M. Ultrasonics come of age. RDH . 1992;4:25-30.
- Ewen S, Tascher, P. Instrumentation in ultrasonic periodontal therapy. J Periodontol . 1958;29:45-49.
- Green GH, Sanderson AD. Ultrasonics and periodontal therapy—a review of clinical and biologic effects. J Periodontol . 1965;36:232-238.
- Dragoo MR. A clinical evaluation of hand and ultrasonic instruments on subgingival debridement. 1. With unmodified and modified ultrasonic inserts. Int J Periodontics Restorative Dent . 1992;12:311-323.
- Lindhe J, Ranney R, Lamster I, et al. Consensus report: chronic periodontitis. Ann Periodontol . 1999;4:1-112.
- Gher ME, Vernino AR. Root morphology—clinical significance in pathogenesis and treatment of periodontal disease. J Am Dent Assoc . 1980;101:627
- Chapple IL, Walmsley AD, Saxby MS, Moscrop H. Effect of instrument power setting during ultrasonic scaling upon treatment outcome. J Periodontol . 1995,66:756-760.
- Pattison A. Advancements in hand instruments. Dimensions of Dental Hygiene . 2006;4(5):26-29.
From Dimensions of Dental Hygiene. October 2006;4(10): 24-27.

