 PHOTO BY JON FRAZE
PHOTO BY JON FRAZE
Note the Signs of Sleep-Disordered Breathing in Children
Oral health professionals can support a child’s optimal growth and development by screening for sleep-related breathing disorders.
This course was published in the September 2018 issue and expires September 30, 2021. The authors have no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- Discuss sleep cycles and the importance of restful, quality sleep in a child’s health, growth, and development.
- Explain sleep-related breathing disorders and their potential impact on a child’s formative years.
- Describe clinical approaches to screening, and the signs and symptoms of sleep-related breathing disorders.
Sleep matters. At no time in medical history has this been clearer. During the critical formative years, making sure that children get the restful, quality sleep they need is vital. A normal sleep cycle includes rapid eye movement (REM) sleep and non-REM sleep. The latter involves three stages, progressing from light to deeper sleep. The human body and brain require all of these stages to achieve and sustain optimal health, growth, and development. When the airway is impeded, the brain sometimes cannot achieve REM and/or the deeper levels of non-REM sleep needed for proper parasympathetic function. Essentially, the body is spending large portions of the night focused on getting oxygen, which prevents it from reaching the deep, restorative phases of sleep.
Various behavioral symptoms can manifest when children do not get the quantity and quality of sleep they need; these include hyperactivity, behavior challenges, trouble focusing, bedwetting, learning disorders, and impaired growth. Because their brains are still developing, screening for sleep disorders is paramount for children, as any hindrance in adequate oxygenation, and therefore parasympathetic sleep, can have an immediate and lasting effect. Consequently, the American Dental Association has issued a statement advising dentists to screen for sleep-related breathing disorders because “proper recognition and treatment can help prolong the health and lives of our patients.”1
Research has examined the relationship between sleep, proper brain development2 and behavioral concerns in children.3 Nasal breathing and tongue position are crucial for proper jaw formation, as the tongue resting on the palate in a closed-mouth position acts as scaffolding for formation of the maxilla. During mouth breathing, the tongue tends to rest on the floor of the mouth rather than on the palate; consequently, the palate often forms a higher vault and a narrower arch form. The sequelae can produce various malocclusion phenotypes, such as anterior open bites or crowding of teeth, which, in turn, can contribute to persistent and worsening mouth breathing. By comparison, nose breathing promotes proper development of the craniofacial and respiratory complexes. Additional benefits include greater oxygenation of peripheral tissues and end-organ targets, and nitric oxide release from within the paranasal sinus complex. Beyond its role as an antioxidant and antimicrobial, nitric oxide acts as a vasodilator upon its release into the respiratory vasculature, thus promoting optimal pulmonary gas exchange.
AWARENESS IS KEY
Airway function disorders, SDB, and obstructive sleep disorders (OSDs) are characterized by conditions that limit airway function at multiple levels.4 Clinical symptoms range from obstructive sleep apnea (OSA) and upper airway resistance syndrome to primary snoring (PS).4,5 The risks of SDB have become more disconcerting, as studies indicate that even mild cases can have severe behavioral cognitive effects on children.4 Awareness is key when it comes to avoiding the detrimental effects of sleep disruption, especially due to OSA, which has been linked to somatic growth delay, cardiovascular and central nervous system diseases, and diminished quality of life.6
Research has shown the impact on cognitive health that is often seen in children with PS and SDB cannot be correlated directly to severity of the condition.4 Rather, individual vulnerability appears to be a much more compelling factor in determining the extent of impairment.4 This highlights the need to treat each pediatric sleep disorder case as a situation that cannot be handled with blanket-style care. Oral health professionals who provide services for children are in a prime position to perform validated airway disorder risk assessment through clinical observation of signs and symptoms, and by asking about behavioral traits known to be associated with increased SDB/OSA risk.
For children, the symptoms of SDB—including OSA and snoring—have been shown to negatively impact behavior and the ability to pay attention. Much was learned about this in the Avon Longitudinal Study of Parents and Children that examined the impact of mouth breathing, apnea, and snoring on behavior in a group of more than 11,000 subjects spanning from infancy to age 7. This study uncovered a litany of connections between SDB and heightened risk of attention deficit hyperactivity disorder, tendencies toward aggression, anxiety disorders, and behavior problems. The authors found that SDB symptoms occurring before age 5 were associated with a 40% greater chance of special education needs by age 8.2
In light of these data, it is clear that oral health professionals who see young patients regularly can make a significant difference by watching for symptoms of SDB. Suspect children can be directed toward treatment, such as an adenotonsillectomy, oral myofunctional therapy, orthodontia, or management with a continuous positive airway pressure device. There is evidence that when undertaken early in a child’s life, these interventions can be effective at preventing negative cardiovascular outcomes.7
SCREENING IN DENTAL PRACTICE
Historically, pediatric exams have involved caries evaluation and control, as well educating the patient and parent/caregiver about proper nutrition and oral hygiene. In today’s practice, screening children for SDB or airway disorders is every bit as important. Recognizing the signs of an airway disorder is a significant step toward a diagnosis that can help a child avoid a lifetime of challenges associated with poor sleep quality (including OSA). Research shows that craniofacial, respiratory, and neurological development—including behavior and learning—can be significantly affected by how well a child breathes, both during the day and while sleeping. Physically, evidence of SDB presents in myriad forms, such as a long and narrow face, habitual open-mouth posture, or venous pooling. Behavioral symptoms might include chronic mouth breathing, hyperactivity, snoring, or bedwetting. In addition, daytime irritability can stem from SDB and OSDs. A short lingual frenulum has also been implicated as a phenotype in pediatric sleep apnea, and has been associated with challenges in speech and sucking, as well as increased risk for maxillary hypoplasia.8,9
Parents and caregivers are invaluable in reporting these possible symptoms, as well as in helping to evaluate the quality of a child’s sleep.5 These developmental attributes are critical to brain development and mitigating cognitive deficiencies. The significance of involving an educated team of health care professionals becomes clear as providers attempt to prevent or treat various maladaptive conditions, and understand the nuances that impact learning, attention, memory, and behavior. Once screening reveals that a child may be at risk for airway issues, several approaches can be used to address them—and possibly provide immediate and long-lasting solutions. For example, dental hygienists, general dentists, pediatric dentists, and orthodontists can be trained to identify scientifically validated physical, behavioral, and birth history clues that might lead to definitive diagnosis of a child’s underlying disorder, thus opening the door to further investigation and appropriate intervention, if indicated.
When the signs of SDB are apparent, the child can be referred to specialists, including oral myofunctional therapists, orthodontists, pediatric dentists, child-focused general dentists, pediatricians, and pediatric ear, nose and throat (ENT) professionals. Oral appliances, orthodontia, and surgical treatment of the maxilla and mandible have also been used to reduce the effects of sleep apnea.10 Oral myofunctional therapists can help evaluate and remedy poor tongue postures or contributing habits, such mouth breathing and tongue thrusting. These therapists are trained to help children learn proper tongue positioning and optimal nasal breathing. Appropriately trained orthodontists, pediatric dentists, and general dental practitioners can help by expanding and protracting retrusive and constricted dental arches, which will result in redirection of impaired growth of both the maxilla and mandible. In addition, ENTs are helpful in evaluating the volume of the airway, and structures that may be impeding it, such as swollen nasal turbinates, tonsils, and/or adenoids. As noted, early intervention can improve a child’s airway during the critical formative years. Proper tongue positioning and eliminating harmful oral habits, ensuring adequate room for the tongue, and promoting nasal breathing can provide lifelong benefits for these patients.
A close examination of the symptoms and health effects apparent in sleep disruption reveals many disquieting conditions that could affect children into adulthood. Swallowing dysfunction has been observed in patients with OSA; this is indicated by abnormal swallowing that could be related to snoring-initiated neuromuscular injury.11 In addition, research suggests there is more to learn about how tongue thrusting, poor rest postures, and nonnutritive sucking behaviors relate to SDB. Oral breathing in young adults, for example, has exhibited an influence on head posture, which could prevent normalization of craniofacial dimensions during growth.12 Abnormalities, habits or issues that have the potential to compromise the upper airway are all suspect. Proper evaluation and diagnosis will benefit from an interprofessional, collaborative style of care. Removing the current silo model and replacing it with a carefully coordinated team of experts can mean the difference between a healthy child and one who grows into adulthood accommodating maladaptive physiological and biological impairments.
SEVEN SIGNS TO LOOK FOR
Armed with mounting evidence of the importance of early screening for sleep disorders and airway obstructions,2 oral health professionals can look for signs and symptoms using simple and scientifically validated checklists, such as the BEARS sleep screening questionnaire or Pediatric Sleep Questionnaire.13 Clinicians may find that instituting these supplemental actions strengthens their patient relationships and helps improve the patient’s oral and systemic health. For example, detecting and treating tongue tie in an infant or young child can promote proper nourishment and optimal development of dental arches and the posterior airway (Figure 1).9 Consistent with the American Academy of Pediatric Dentistry’s policy statement regarding the importance of establishing a dental home by age 1, welcoming newborns and infants into a practice allows oral health professionals to view the tongue position, which, in turn, could help prevent unnecessary developmental deficits. The following protocol is easily incorporated into clinicians’ clinical procedures. The seven common signs of SDB include:
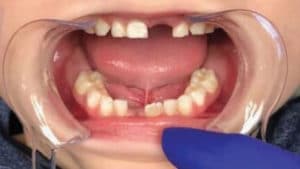
- High/narrow palatal vault9
- Mouth breathing12
- Clenching and grinding or tooth wear14
- Enlarged tonsils and adenoids15
- Allergic rhinitis or prevalence of allergy symptoms16
- Tongue tie and/or lip tie8
- Maxillary and mandibular deficiency8,9,12
If a clinician detects any of these symptoms, the next step would be to get the parents/caregivers involved. Key questions might include:
- Does the child snore, or make any noise while sleeping?
- Does he or she stop breathing for short periods during sleep?
- How rested does the child seem upon waking?
- Has he or she experienced behavior issues at home or school?
The last question deserves special attention, because sleep disorders and airway obstructions can lead to excessive fidgeting, emotional outbursts, and short attention spans. Assessing a child’s sleep habits can also help oral health professionals in treatment planning and educational efforts. The parent/caregiver should be asked not just how long a child sleeps, but also how well the child sleeps. Many adults will report their children sleep the whole night, which is usually a sign of adequate sleep quantity, but if the child shows signs of SDB, the adult should be suspicious of possible poor sleep quality. Asking the parent/caregiver to spend 20 minutes watching the child sleep may help answer the first question. How the clinician proceeds will vary based on relationships with other qualified health professionals, which, as previously noted, could include referrals to a pediatrician, ENT specialist, sleep physician, orthodontist, pediatric dentist, or oral myofunctional therapist experienced in treating malocclusion that might be comorbid with SDB and airway restriction. Utilizing a team approach will help optimize treatment for each patient.
Other actionable options include educating patients and/or parents/caregivers about the value of optimal sleep and airway disease prevention. Adults can be encouraged to help children develop habits that will make sleep patterns more regular. Small changes, such as putting away electronics at least an hour before bedtime17 and going to sleep at a regular time, can make a difference. Parents/caregivers should be aware of any new allergens in the child’s bedroom or bed, because rugs, carpet, pets, or stuffed animals that are seldom washed could lead to a mouth-breathing pattern associated with the detriments outlined above. One of the most important roles a parent/caregiver can play is seeking out health care providers who are competent in assessing and treating pediatric airway disorders.
IN SUMMARY
When loss of grey matter density,18 depressive disorders,19 and academic deficits15 are among the potential impacts of sleep disorders, any evidence-supported intervention is worth considering. Unhealthy sleep patterns have a whole-body effect on children that can influence performance in all aspects of education and development—thus negatively impacting health well into adulthood.
As a result, oral health professionals should routinely screen for SDB and other airway disorders. Dentistry can, and should, be the frontline defense for children vulnerable to sleep disruption. Incorporating a screening protocol that evaluates the child from a comprehensive and whole-body approach can help preemptively remove developmental obstacles affecting the quality of a child’s life into his or her adult years.
References
- Burger D. Sleep-related breathing disorder treatment outlined in new policy. ADA News. Available at: ada.org/en/publications/ada-news/2017-archive/october/sleep-related-breathing-disorder-treatment-outlined-in-new-policy. Accessed August 23, 2018.
- Bonuck K, Rao T, Xu L. Pediatric sleep disorders and special educational need at 8 years: A population-based cohort study. Pediatrics. 2012;130:634–642.
- Arali V, Namineni S, Sampath C. Pediatric obstructive sleep apnea syndrome: Time to Wake up. Int J Clin Pediatr Dent. 2012;5:54–60.
- Bourke R, Anderson V, Yang JS, et al. Cognitive and academic functions are impaired in children with all severities of sleep-disordered breathing. Sleep Med. 2011;12:489–496.
- de Serres LM, Derkay C, Sie K, et al. Impact of adenotonsillectomy on quality of life in children with obstructive sleep disorders. Arch Otolaryngol Head Neck Surg. 2002;128:489–496.
- Tan H, Alonso Alvarez M, Tsaoussoglou M, Weber S, Kaditis A. When and why to treat the child who snores? Pediatr Pulmonol. 2017;52:399–412.
- Arens R, Muzumdar H. Childhood obesity and obstructive sleep apnea syndrome. J Appl Physiol. 2010;108:436–444.
- Guilleminault C, Huseni S, Lo L. A frequent phenotype for paediatric sleep apnoea: Short lingual frenulum. ERJ Open Res. July 29, 2016. Epub ahead of print.
- Yoon AJ, Zaghi S, Ha S, Law CS, Guilleminault C, Liu SY. Ankyloglossia as a risk factor for maxillary hypoplasia and soft palate elongation: A functional-morphological study. Orthod Craniofac Res. 2017;20:237–244.
- Ruoff C, Guilleminault C. Orthodontics and sleep-disordered breathing. Sleep Breath. 2012;16:271–273.
- Valbuza J, Oliveira M, Zancanella E, et al. Swallowing dysfunction related to obstructive sleep apnea: A nasal fibroscopy pilot study. Sleep Breath. 2011;15:209–213.
- Cuccia A, Lotti M, Caradonna D. Oral breathing and head posture. Angle Orthod. 2008;78:77–82.
- Chervin RD, Hedger KM, Dillion JE, Pituch KJ. Pediatric Sleep Questionnaire (PSQ): validity and reliability of scales for sleep-disordered breathing, snoring, sleepiness, and behavioral problems. Sleep Med. 2000;1:21–32.
- Ng DK, Kwok KL, Poon G, Chau KW. Habitual snoring and sleep bruxism in a paediatric outpatient population in Hong Kong. Singapore Med J. 2002;43:554–556.
- Galland B, Spruyt K, Dawes P, Mcdowall P, Elder D, Schaughency E. Sleep disordered breathing and academic performance: a meta-analysis. Pediatrics. 2015;136:E934–E946.
- Oliveira L, Gomes C, Ferreira R. Allergy as a risk factor for sleep disordered breathing. Sleep Med. 2013;14 (Suppl 1):e36–e37.
- Lebourgeois M, Hale L, Chang A, Akacem L, Montgomery-Downs H, Buxton O. Digital media and sleep in childhood and adolescence. Pediatrics. 2017;140:S92–S96.
- Chan KC, Shi L, So HK, et al. Neurocognitive dysfunction and grey matter density deficit in children with obstructive sleep apnoea. Sleep Med. 2014;15:1055–1061.
- Chang CH, Chen SJ, Liu CY. Pediatric sleep apnea and depressive disorders risk: A population-based 15-year retrospective cohort study. PLoS ONE. 2017;12:E0181430.
From Dimensions of Dental Hygiene. September 2018;16(9):24–27.



