Heart Safe Dental Care
Ensure the safety of patients with cardiovascular disease by keeping up-to-date on the guidelines for prophylaxis.
This course was published in the November 2011 issue and expires November 2014. The authors have no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- Detail the recommendations included in the 2007 American Heart Association Prevention of Infective Endocarditis Guidelines.
- Identify the medical conditions and devices at risk of infection from bacteremia due to dental procedures.
- Discuss the oral cavity as a source of infective endocarditis.
The American Heart Association (AHA) first introduced recommendations for the use of antibiotic prophylaxis before routine dental treatment in order to prevent infective endocarditis (IE) in 1955.1 Much has changed since their inaugural release, and several updates have been issued. Due to the emergence of additional scientific evidence, the 2007 guidelines have significantly limited the use of antibiotic prophylaxis.2 Dental professionals, particularly those treating patient populations with high levels of cardiovascular disease (Table 1), need to update their own practice policies to reflect these new guidelines.3
What the Evidence Says
It is clear that oral bacteria cause some cases of IE, but any association between invasive dental procedures and endocarditis remains debatable.4 In fact, there is no conclusive proof that antibiotic prophylaxis is effective in reducing the incidence of IE.2,5,6 Many large clinical studies have demonstrated that antibiotic prophylaxis reduces the incidence and duration of bacteremia (bacteria getting into the blood stream) following dental procedures,2,4 but none show that dental procedures specifically cause IE.
Bacteremia caused by routine activities, such as toothbrushing, is far more common than dental procedure-related bacteremia.4 Evidence suggests that people with compromised oral health experience higher rates of bacteremia than those with good oral health.7 As such, patients at risk of IE should receive consistent professional oral health care and perform effective self-care regimens in order to maintain optimal oral health. The clinical importance of bacteremia caused by dental procedures, and the use of antibiotic prophylaxis to prevent it, may be less important.
Oral Cavity as a Source of Distant Site Infection
Valvular abnormalities and turbulent blood flow are the primary risk factors for IE. Oral hygiene and gingival disease, however, may be the next most important risk factors in the development of primary oral flora-related IE.2 Strong evidence supports the idea that the gingival crevice around the teeth is the main source and portal of entry for the oral bacterial species that causes more than 40% of IE cases. The best evidence for this relationship is the frequent presence of oral bacteria in the blood of patients with IE and data from studies of bacteremia following dental procedures.4,8 The origin of many IE cases is probably transient bacteremia entering the blood from oral bacterial pathogens around the teeth. Bacteremia has also occurred following dental procedures in patients with healthy periodontia.9–11
Role of Antibiotic Prophylaxis
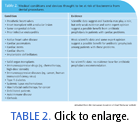
Antibiotic prophylaxis is designed to kill bacteria before they can adhere. For patients with cardiovascular disease, it may inhibit bacterial attachment to the endothelium of the heart. Antibiotic prophylaxis has been recommended for more than 25 patient populations because of an increased risk of infection (Table 2).5
Antibiotic prophylaxis, however, has its own set of risks. As a result, the 2007 AHA guidelines greatly reduced the number of cardiac conditions indicated for antibiotic prophylaxis (Table 3).2
Risks of Antibiotic Prophylaxis
Prior to 2007, the AHA guidelines placed patients with heart disease into three categories: low, moderate, and high risk of negative outcomes caused by IE.8 Antibiotic prophylaxis was not recommended for patients at low risk. The 2007 guidelines eliminated the antibiotic prophylaxis recommendation for the moderate risk group, which comprises almost 90% of the patients who were recommended to receive it under the 1997 guidelines.12
The AHA revised these guidelines for several reasons. Although IE still has a high morbidity and mortality rate, insufficient evidence exists to support the efficacy of antibiotic prophylaxis to prevent cardiac infection when used prior to dental procedures. There are also risks associated with the widespread use of antibiotics in the population as a whole, such: as allergic reactions (including anaphylaxis); risk of developing resistant and more infectious strains of bacteria; changes in the normal microbiological flora; gastrointestinal disturbance (eg, amoxicillin) or pseudo-membranous colitis (eg, clindamycin); and drug interactions. Finally, the financial cost of administering antibiotic prophylaxis to patients in the moderate risk category is significant.
The current guidelines still advise that the four highest risk cardiac populations receive prophylaxis, which include those with prosthetic cardiac valves, previous IE patients, some congenital heart disease patients, and some cardiac transplantation patients.
Current AHA guidelines acknowledge that few, if any, cases of IE are caused by invasive dental procedures and point out that IE from oral flora is most often caused by bacteremia from routine daily activities. England has abandoned antibiotic prophylaxis altogether and the incidence of IE has not increased.13,14
Recommendations for Patients with Cardiovascular Disease
The 2007 AHA guidelines for antibiotic prophylaxis were written by experts in cardiology, infectious diseases, dentistry, epidemiology, and other specialties. It is the most authoritative document in the United States on this topic, and the guidelines are used by many countries throughout the world. These experts conclude there is currently no proven association or causal relationship between dental procedures and the development of IE.
Table 4 shows the most recent dosage guidelines. Amoxicillin is the most frequently prescribed antibiotic, although several alternatives exist for patients who are allergic, including clindamycin and cephalexin. A single dose should be administered approximately 1 hour before dental treatment begins. If the patient has not taken the correct dose at the right time, it may be administered up to 2 hours after the procedure. If a patient is already taking antibiotics for another infection, an antibiotic from a different class should be chosen in order to reduce the risk of creating resistant microbial forms.
Another major change to the 2007 guidelines is the listing of dental procedures that should be avoided by patients at high risk of IE. The 2007 guidelines do not provide a lengthy list of procedures to be avoided, but rather, they advise avoiding procedures that manipulate the gingival tissue, periapical region of the teeth, or perforation of the oral mucosa (Table 3).
Table 1. Cardiovascular disease risk factors.3
- Male
- Older than 65 years of age
- Genetic predisposition
- Smoking
- High cholesterol
- High blood pressure
- Sedentary lifestyle
- Overweight and obesity
- Diabetes
- High stress levels
- Poor diet
- Heavy alcohol use
Clinical Relevance
Some patients, physicians, and dental professionals may disagree with the 2007 guidelines, which can put dental hygienists in a difficult position because they are ultimately responsible for the treatment provided. The overall goal should be to encourage all health care providers to reach a consensus on the issue of antibiotic prophylaxis. Clear communication among all parties and a presentation of the scientific evidences should facilitate the reaching of an agreement. Dental hygienists play an important role as liaisons between patients and their dentists.
Conclusion
There is no strong scientific evidence that dental procedures cause IE, nor that antibiotic prophylaxis reduces the risk of IE among patients with cardiovascular diseases.7 The AHA guidelines stress that dental professionals and patients should focus on routine preventive care and oral health as the primary means of reducing the risk of IE.
Current Thinking About Antibiotic Prophylaxis and the Risk of Infective Endocarditis
What We Know:
- A high percentage of Viridans Group Streptococci (VGS) exist in the mouth.• Invasive dental procedures and toothbrushing increase the risk of VGS-associated bacteremia.
- Oral bacteria can cause infective endocarditis and other distant site infections, such as brain abscess.
- Compliance with established guidelines for antibiotic prophylaxis is poor.
- Antibiotic prophylaxis does not always prevent infective endocarditis.
What We Think We Know:
- Antibiotic prophylaxis kills bacteria before they adhere, inhibits bacterial attachment to the endothelium of the heart, and kills or inhibits growth in early vegetations of bacteria.
- There is little drug resistance in the population from a single dose of antibiotics.
- Bacteremia incidence, duration, and nature (species) are related to some invasive dental procedures and toothbrushing.
What We Don’t Know:
- Whether patients at risk of distant site infections can be identified.
- If dental procedures cause infective endocarditis.
- Whether antibiotic prophylaxis prevents distant site infection.
- The magnitude of bacteremia following dental procedures or routine daily events, such as toothbrushing or chewing food.
- Whether bacteremia surrogate measures are relevant (eg, incidence, duration, nature, and magnitude of bacteremia)
- If an association exists between the invasiveness of a procedure and the risk of bacteremia/distant site infection.
- Whether the benefits of antibiotic prophylaxis outweigh the risks.
- Whether poor oral hygiene and oral disease are risk factors for distant site infection.
- If antibacterial mouthrinses decrease bacteremia and prevent distant site infection.
- If oral bleeding is an indicator of bacteremia risk.
REFERENCES
- Jones TD, Baumgartner L, Bellows MT, et al. Prevention of rheumatic fever and bacterial endocarditis through control of streptococcal infections. Circulation. 1955;11:317–320.
- Wilson W, Taubert KA, Gewitz M, et al. Prevention of infective endocarditis: guidelines from the American Heart Association: a guideline from the American Heart Association Rheumatic Fever, Endocarditis, and Kawasaki Disease Committee, Council on Cardiovascular Disease in the Young, and the Council on Clinical Cardiology, Council on Cardiovascular Surgery and Anesthesia, and the Quality of Care and Outcomes Research Interdisciplinary Working Group. Circulation. 2007;116:1736–1754.
- Understand Your Risk of Heart Attack. American Heart Association. Available at: www.heart.org/HEARTORG/Conditions/HeartAttack/UnderstandYourRiskofHeartAttack/Understand-Your-Risk-of-Heart-Attack_UCM_002040_Article.jsp#.TqWmYc1OgtU. Accessed October 24, 2011.
- Lockhart PB, Brennan MT, Sasser HC, Fox PC, Paster BJ, Bahrani-Mougeot FK. Bacteremia associated with toothbrushing and dental extraction. Circulation. 2008;117:3118–3125.
- Lockhart PB, Loven B, Brennan MT, Fox PC. The evidence base for the efficacy of antibiotic prophylaxis in dental practice. J Am Dent Assoc. 2007;138:458–474.
- Oliver R, Roberts GJ, Hooper L, Worthington HV. Antibiotics for the prophylaxis of bacterial endocarditis in dentistry. Cochrane Database Syst Rev. 2008;4:CD003813.
- Lockhart PB, Brennan MT, Thornhill M, et al. Poor oral hygiene as a risk factor for infective endocarditis-related bacteremia. J Am Dent Assoc. 2009;140:1238–1244.
- Bahrani-Mougeot FK, Paster BJ, Coleman S, Ashar J, Barbuto S, Lockhart PB. Diverse and novel oral bacterial species in blood following dental procedures. J Clin Microbiol. 2008;46:2129–2132.
- Lockhart PB, Brennan MT, Kent ML, Norton HJ, Weinrib DA. Impact of amoxicillin prophylaxis on the incidence, nature, and duration of bacteremia in children after intubation and dental procedures. Circulation. 2004;109:2878–2884.
- Roberts GJ, Gardner P, Simmons NA. Optimum sampling time for detection of dental bacteraemia in children. Int J Cardiol. 1992;35:311–315.
- Lockhart PB. An analysis of bacteremias during dental extractions: a double-blind, placebo-controlled study of chlorhexidine. Arch Intern Med. 1996;156:513–520.
- Dajani AS, Taubert KA, Wilson W, et al. Prevention of bacterial endocarditis: recommendations by the American Heart Association. JAMA. 1997;277:1794–1801.
- Prophylaxis against infective endocarditis: antimicrobial prophylaxis against infective endocarditis in adults and children undergoing interventional procedures. NICE Clinical Guideline No 64. London: National Institute for Health and Clinical Excellence; 2008.
- Thornhill MH, Dayer MJ, Forde JM, et al. Impact of the NICE guideline recommending cessation of antibiotic prophylaxis for prevention of infective endocarditis: before and after study. BMJ. 2011;342:2392.
From Dimensions of Dental Hygiene. November 2011; 9(11): 72, 75-77.