Hand Health
Tips for preventing and managing soft tissue disorders of the hands.
This course was published in the April 2011 issue and expires Apri 2014. The authors have no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- List possible causes of cumulative trauma disorders.
- Differentiate between de Quervain’s disease and Raynaud’s syndrome.
- Discuss treatment and management options for de Quervain’s disease.
- Identify possible risk factors associated with secondary Raynaud’s phenomenon.
- Detail management options for Raynaud’s phenomenon.
The frequently repeated movements so common to the practice of dental hygiene often lead to cumulative trauma disorders (CTDs).1,2 Additional behaviors specific to dental hygienists that increase their risk of CTDs include limited hand movements, use of vibrating instruments, and holding stressful body positions.3-5 The number of working hours, number of difficult patients treated, and years of practice also affect dental hygienists’ risk status.6 Mechanical stress caused by glove use and instrument design may also affect the well-being of practitioners.6 Typically, the upper extremities are more prone to CTDs when performing repetitive tasks.5
Carpal tunnel syndrome is the most common type of CTD experienced by dental hygienists.3 However, thoracic outlet syndrome, cubital and ulnar tunnel syndrome, extensor wad strain, and glove-induced injuries are also common among dental professionals.6 These CTDs have been extensively reviewed in the literature. However, two soft tissue disorders that affect the hands—de Quervain’s disease and Raynaud’s phenomenon—are not as frequently discussed but can have debilitating effects for dental hygienists.
ETIOLOGY OF DE QUEVAIN’S DISEASE
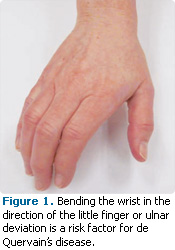
De Quervain’s disease is named for the Swiss surgeon, Fritz de Quervain, who first identified it in five women in 1895.7 The cause of de Quervain’s is idiopathic. However, repetitive motions, such as ulnar (bending the wrist in the direction of the little finger) and radial deviation of the wrist (bending the wrist in the direction of the thumb), are considered contributing factors (Figure 1).8
Dental hygiene procedures increase the probability of placing the wrist in ulnar deviation. To maintain health, dental hygienists must concentrate on keeping the wrist in neutral position during instrumentation. Reaching for dental instruments is another common cause of ulnar deviation.8 To avoid this, instruments should be placed within easy reach of the patient treatment area.
In de Quervain’s disease, the extensor pollicis brevis and the abductor pollicis longus tendons in the wrist at the base of the thumb become inflamed.7 Inflammation in these tendons of the thumb can cause pain that extends to the base of the wrist (tenosynovitis) and possibly into the forearm and shoulder.5,8 Thumb motion may be difficult and painful, particularly when twisting or pinching/grasping objects. The pain may increase with ulnar deviation of the wrist or if direct pressure is applied to the area. De Quervain’s affects middle-aged women eight to 10 times more frequently than men.7,9 Its onset can occur gradually or suddenly.
DIAGNOSIS AND TREATMENT
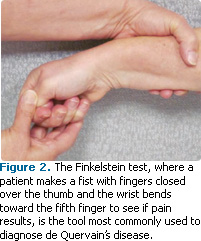
The Finkelstein test is most frequently used to diagnose de Quervain’s disease. When conducting this test, the patient makes a fist with fingers closed over the thumb and the wrist is bent toward the fifth (little) finger (Figure 2).5,8 When the wrist is bent toward the outside, the swollen tendons are pulled through the space in the wrist and stretched, which causes pain. A physical examination is also recommended to rule out any other possible conditions that could cause pain in the same area, such as osteoarthritis, scaphoid (navicular) bone disorders, disruption of the scapholunate ligament, and carpal tunnel syndrome.8
Initially, the patient continuously wears a spica splint for 4 weeks to 6 weeks (Figure 3).5,8,10,11 This not only immobilizes the affected area, but inhibits activities that may aggravate the condition. Ice may be applied to the affected area for 15 minutes to 20 minutes to reduce inflammation. The area should be warmed for 45 minutes before icing again. If symptoms continue, a physician may prescribe anti-inflammatory medications, such as naproxen or ibuprofen, or inject the area with corticosteroids to decrease pain and swelling.5,8,11 Management of de Quervain’s disease with corticosteroid injections is successful in approximately 50% to 80% of patients.11
If conservative medical treatment is not successful, outpatient surgery may be recommended. Surgery involves releasing the tendon sheath to relieve pressure or constriction around the tendon. This eliminates the friction that causes inflammation, thus restoring the tendon’s smooth gliding capability.11 Following surgery, physical/occupational therapy may be recommended to strengthen the thumb and wrist. Recovery times vary, depending on age, general health, and how long the symptoms have been present. Individuals whose disease has developed gradually may be more resistant to treatment.
The clinical management of any CTD is based on identifying and treating individual component pathologies. Referral to a knowledgeable physical/occupational therapist, with an understanding of ergonomic behavioral, postural, and workspace modification, is recommended.12 Prevention and management of the disease involves:
- Keeping hand/arm in neutral position during instrumentation, avoiding repetitive ulnar deviation of the wrist.
![]()
- Placing instruments within easy reach of patient treatment area to prevent ulnar deviation of the wrist.
- Practicing ergonomically correct positions.
RAYMAUD’S SYNDROME
Raynaud’s syndrome is named for the French physician, Maurice Raynaud, who first recognized the condition in 1862.13 Raynaud’s syndrome, sometimes referred to as a disease or phenomenon, is a type of vascular disease that affects the arteries. There is an interruption of blood flow to the fingers, toes, nose, and/or ears when a spasm occurs in the vessels of these areas. The hands are most commonly affected.14
Raynaud’s syndrome can occur alone or in association with other rheumatic diseases. When it occurs alone, it is referred to as Raynaud’s disease or primary Raynaud’s phenomenon. Primary Raynaud’s phenomenon is the most common form of the disorder and is not associated with any underlying disease or medical problem.
Secondary Raynaud’s typically accompanies connective tissues diseases such as scleroderma, systemic lupus erythematosus, Sjögren’s syndrome, rheumatoid arthritis, and polymyositis.14 Although secondary Raynaud’s is less common, it can be more serious. Signs of secondary Raynaud’s initially appear around age 40, whereas the primary form of Raynaud’s occurs indiscriminately.
CONTRIBUTING FACTORS
Arterial spasms from Raynaud’s syndrome are caused by exposure to cold or emotional stress. More important to dental hygienists, Raynaud’s also can be caused by repetitive trauma that damages the nerves supplying the blood vessels in the hands. Use of vibrating, hand-held power instruments over time can produce a type of secondary Raynaud’s phenomenon known as vibration white finger or hand-arm vibration syndrome (HAVS). HAVS is characterized by excessively reduced blood flow; blanching of the fingers; and limited supply of blood to the muscles, nerves, and tendons. Symptoms of HAVS include pain and/or tingling and numbness of the hand leading to loss of manual dexterity.
Vibrations also may cause injury to sympathetic (unmyelinated) fibers, leading to sympathetic overactivity. When the myelin sheath starts to degrade, nerve impulses are conducted improperly or lost completely, leading to tingling sensations or heat sensitivity. Signs of sympathetic overactivity include increased color changes (blue/red), sweating, and cold periphery with vasoconstriction. Additionally, occupational Raynaud’s phenomenon may be caused by thrombosis or clot of the ulnar artery. Raynaud’s phenomenon related to ulnar artery thrombosis is typically unilateral and associated with small blood clots.15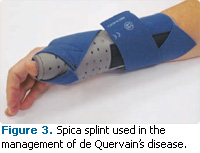
SYMPTOMS
Due to an imbalance of vasoconstriction and vasodilation in Raynaud’s disease, the affected area turns white, then blue, followed by bright red over the course of the attack (Figure 4). Skin discoloration occurs because an abnormal spasm of the blood vessels causes a diminished blood supply to the local tissues. In addition, there may be associated tingling, swelling, or painful throbbing. Chemotherapy is a risk factor for developing these symptoms, especially for patients being treated for ovarian cancer.16 Figure 4 shows the fingers of a dental hygienist, who is undergoing chemotherapy for ovarian cancer, experiencing Raynaud’s symptoms—red, white and blue fingers—when exposed to prolonged cold temperatures.
While there is no single blood test that identifies Raynaud’s, blood work can rule out the presence of autoimmune antibodies associated with scleroderma, lupus, mixed connective tissue disease, undifferentiated connective tissue disease, Sjögren’s syndrome, and other diseases that may have Raynaud’s as a possible component. Differential diagnostic tests include doppler ultrasound, nailfold capillaroscopy, antinuclear antibody test, and erythrocyte sedimentation rate.17
DISEASE MANAGEMENT
A physician may prescribe medication to relax the walls of the blood vessels to prevent smooth muscle contraction and arterial damage. Medications prescribed include topical nitroglycerin, angiotensin-converting enzyme (ACE) inhibitors, and calcium-channel blockers, especially nifidepine and sildenafil (Viagra).18,19 Transdermal, oral, or topical nitrates may cause adverse effects such as headaches, which can limit their use.14 Nondrug treatments and self-help measures can also decrease the severity of Raynaud’s attacks and promote overall well-being. Keeping the body, hands, and feet warm is helpful. Other measures include not smoking (constricts blood vessels), minimizing stress, exercising regularly, and having regular physical examinations.20 In addition, dental hygienists with Raynaud’s should limit their use of instruments that produce vibration.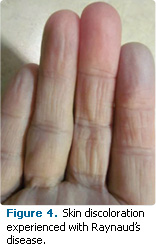
Lifestyle changes and supplements that encourage better circulation may be effective alternatives for managing Raynaud’s. Niacin, also known as vitamin B3, causes blood vessels to dilate, increasing blood flow to the skin.21 Although niacin supplements may be useful in treating Raynaud’s, they do cause flushing of the skin, most commonly in the face and trunk.21
Other complementary and alternative medicines used to treat Raynaud’s have been tested with positive results. In a double-blind, placebo-controlled study, the consumption of fish oil showed an increase in digital systolic pressure as well as the time of onset of symptoms after exposure to cold.22 In addition, evening primrose oil, which is a rich source of gamma-linolenic acid (GLA), demonstrated a decrease in the frequency of Raynaud’s attacks. GLA is an omega-6 essential fatty acid that cannot be made by the body and, therefore, must be obtained from food. Also known as a polyunsaturated fatty acid, GLA is found predominately in plant-based oils and is effective in reducing inflammation and stimulating skin growth.14 Before beginning complementary and alternative medicine treatments, a physician should be consulted.
PREVENTION
General exercise improves circulation and, therefore, may help prevent or minimize attacks of Raynaud’s syndrome. In addition, smoking should be eliminated since it impairs circulation. Recognizing and avoiding stressful situations may also help control the number and severity of attacks.23 Specific recommendations for dental hygienists are listed in Table 1.
CONCLUSION
Dental hygienists routinely use instruments that vibrate and perform hand-intensive, repetitive movements often in cramped conditions. Therefore, they can be at greater risk of developing hand disorders from lack of proper circulatory flow, pinched nerves, and compromised hand positions. Once symptoms develop, timely intervention is essential. A medical evaluation and diagnostic tests provide supplementary information to the physical examination and history. A comprehensive strategy for treatment and prevention is essential for a long career in dental hygiene.
REFERENCES
- Liskiewicz ST, Kerschbaum WE. Cumulative trauma disorders: an ergonomic approach for prevention. J Dent Hyg. 1997;4:162-167.
- Werner RA, Hamann C, Franzblau A, Rodgers PA. Prevalence of carpal tunnel syndrome and upper extremity tendinitis among dental hygienists. J Dent Hyg. 2002;2:126-132.
- Willard P. Patient reception and ergonomic practice. In: Wilkins EM. Clinical Practice of the Dental Hygienist. 10th ed. Philadelphia: Lippincott Williams & Wilkins; 2009:92.
- Carpal Tunnel Syndrome Health Center. Carpel Tunnel Syndrome. Available at: www.webmd.com/pain-management/carpal-tunnel/carpaltunnel-syndrome. Accessed March 23, 2011.
- Hamann C, Werner RA, Rhode N, Rodgers PA, Sullivan K. Upper extremity musculoskeletal disorders in dental hygiene: diagnosis and options for management. Contemporary Oral Hygiene. 2004;4:2-8.
- Tavoc T, Gutmann ME. Preventive strategies can keep practice pain-free and ensure a long career in clinical dental hygiene. Dimensions of Dental Hygiene. 2005;3(1):16-21.
- Lamphier TA, Long NG, Dennehy T. De Quervain’s disease an analysis of 52 cases. Ann Surg. 1953;6:832-841.
- Stitik TP, Conte M, Foye PM, Schoen D, Marini JS. An analysis of cumulative trauma disorders in dental hygienists. Journal of Practical Hygiene. 2000;9(2):19-25.
- Arthritis Health Center. De Quervain’s Disease—Topic Overview. Available at: http://arthritis.webmd.com/tc/de-quervainsdisease-topic-overview. Accessed March 23, 2011.
- Ilyas AM. Nonsurgical treatment for de Quervain’s tenosynovitis. J Hand Surg Am. 2009;5:928-929.
- Hazani R, Engineer NJ, Cooney D, Wilhelmi BJ. Anatomic landmarks for the first dorsal compartment. Eplasty. 2008;8:53.
- Chin DH, Jones NF. Repetitive motion hand disorders. J Calif Dent Assoc. 2002;2:149-160.
- Belch JJ. The phenomenon, syndrome and disease of Maurice Raynaud. Br J Rheumatol. 1990;3:162-165.
- Pope JE. The diagnosis and treatment of Raynaud’s phenomenon—a practical approach. Drugs. 2007;4:517-525.
- Al Qattan MM, Bowen V. Cumulative trauma disorders of the hand and wrist. Current Opinion in Orthopaedics. 1993;4(4):68-71.
- Matei D, Miller AM, Monahan P, et al. Chronic physical effects and health care utilization in long-term ovarian germ cell tumor survivors: a gynecologic oncology group study. J Clin Oncol. 2009;27:4142-4149.
- Kim SH, Kim HO, Jeong YG, et al. The diagnostic accuracy of power Doppler ultrasonography for differentiating secondary from primary Raynaud’s phenomenon in undifferentiated connective tissue disease. Clin Rheumatol.2008;6:783-786.
- Bakst R, Merola JF, Franks AG Jr, Sanchez M, Perelman RO. Raynaud’s phenomenon: pathogenesis and management. J Am Acad Dermatol. 2008;59:633-653.
- Olin JW. Other peripheral arterial diseases. In: Goldman L, Ausiello D, eds. Cecil Medicine. 23rd ed. Philadelphia: Saunders Elsevier; 2007:80.
- National Institute of Arthritis and Musculoskeletal and Skin Disease. Raynaud’s Phenomenon. Available at: www.niams.nih.gov/Health_Info/Raynauds_Phenomenon/default.asp#5. Accessed March 23, 2011.
- Mayo Clinic. Raynaud’s Disease. Available at: www.mayoclinic.com/health/raynaudsdisease/DS00433/DSECTION=alternativemedicine. Accessed March 23, 2011.
- DiGiacomo RA, Kremer JM, Shah DM. Fish-oil dietary supplementation in patients with Raynaud’s phenomenon: a double-blind, controlled, prospective study. Am J Med. 1989;2:164-185.
- NYU Langone Medical Center. Raynaud’s Disease and Phenonomen. Available at: www.med.nyu.edu/content?ChunkIID=11600. Accessed March 23, 2011.
From Dimensions of Dental Hygiene. April 2011; 9(4): 72-75.