
Details Make All The Difference
This comprehensive overview of the CDC’s infection control guidelines will help you practice safely.
In 1970 the Centers for Disease Control and Prevention (CDC) published the guidelines “Isolation Techniques for Use in Hospitals.” CDC updated these recommendations to meet the infection control challenges posed by newly identified pathogens. By 1983 the guidelines covered seven categories of isolation, but health care professionals still decided the level of protection and/or isolation necessary for specific techniques.1
UNIVERSAL PRECAUTIONS
In 1987, when the first comprehensive infection control guidelines for the dental setting were published, isolation techniques were replaced with universal precautions. Universal precautions are based on the concept that all blood and body fluids that might be contaminated with blood should be treated as infectious because patients with bloodborne infections can be asymptomatic or unaware they are infected.2 Preventive practices used under universal precautions to reduce blood exposures, particularly percutaneous exposures, include careful handling of sharp instruments; use of rubber dams to minimize blood splattering; handwashing; and use of protective barriers (eg, gloves, masks, protective eyewear, and gowns).
Advances in microbiologic and epidemiologic science provided a better understanding of bloodborne disease transmission in health care settings. There were documented cases of hepatitis B virus transmission in health care settings throughout the early 1980s.3 In December 1991 the Occupational Safety and Health Administration (OSHA) provided specific regulations to prevent the transmission of bloodborne pathogens, which stressed the importance of using universal precautions.
The CDC Oral Health Division outlined four infection control principles to minimize the transmission of bloodborne and infectious diseases in 1994 (Table 1). These principles are based on the level of anticipated contact with mucous membranes, blood, or saliva contaminated with blood.
TABLE 1. THE FOUR PRINCIPLES OF INFECTION CONTROL TO MINIMIZE THE TRANSMISSION OF BLOODBORNE AND INFECTIOUS DISEASES.
- Take action to stay healthy.
- Avoid contact with blood and other potentially infectious body substances.
- Make patient care items (instruments, devices, equipment) safe for use.
- Limit the spread of blood and other infectious body substances.
STANDARD PRECAUTIONS
In 1996 standard precautions were introduced in a CDC update to “Isolation and Transmission-based Precautions.”6 Standard precautions synthesize the major features of universal precautions (de signed to reduce the risk of transmission of bloodborne pathogens) and body substance isolation (designed to reduce the risk of pathogens from moist body substances) and apply them to all patients regardless of their diagnosis or presumed infection status.
Standard precautions apply to: blood; all body fluids, secretions, and excretions (except sweat), regardless of whether they contain blood; nonintact skin; and mucous membranes. The precautions are designed to reduce the risk of transmission of microorganisms from both recognized and unrecognized sources of infection.5
Elements of standard precautions include handwashing, use of appropriate personal protective equipment (PPE), management of patient care equipment, maintenance of environmental surfaces, and injury protection. Standard precautions are indicated in most dental health care settings.
This move from universal to standard precautions did not necessitate major changes to infection control protocol in the dental setting because saliva was labeled a bloodborne fluid in the 1987 CDC “Guidelines for Infection Control in Dentistry.”3 This designation was made because saliva has the potential to contain blood, especially during and after the performance of dental procedures.7
RESPIRATORY HYGIENEe
In 2007 CDC updated the isolation guidelines and added the respiratory hygiene (cough etiquette) to standard precautions (see Table 2). Cough etiquette is intended to reduce or eliminate the spread of respiratory secretions and is best if accompanied by simple signage that explains how to cover a cough, encourages the sanitary disposal of tissue (have a receptacle near the tissue box), how to perform effective hand hygiene, and how to use alcohol-based hand rubs. CDC created a poster about cough etiquette for health care providers to use in their offices (see Figure 1). It is available at the CDC website at no charge (www.cdc.gov).
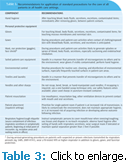
Reception area personnel should be trained to talk to patients when confirming appointments to determine whether they could spread infection. If a patient reports for an appointment with symptoms of infection, staff should ask him or her to wear a surgical mask and keep him or her isolated from other patients.8 Table 3 outlines the recommendations for applying standard precautions for the care of patients in all health care settings.
TABLE 2. RECOMMENDATIONS FOR INDIVIDUALS WITH SYMPTOMS OF RESPIRATORY INFECTION.
- Cover your mouth and nose with a tissue when coughing or sneezing.
- Have a waste receptacle in a convenient location for tissue disposal.
- Perform hand hygiene (eg, hand washing with nonantimicrobial soap and water, alcohol-based hand rub, or antiseptic handwash) after contact with respiratory secretions and contaminated objects/materials.
GUIDELINES FOR DENTISTRY
In 2003 CDC updated the infection control recommendations for dentistry. The updated guideline, “CDC Guidelines for Infection Control in Dental Health-Care Settings—2003,” emphasized standard precautions and provided evidence-based recommendations. The recommendations were consistent with other CDC guidelines for infection control in health care settings (for example, hand hygiene, environmental infection control, sterilization, and disinfection guidelines). CDC emphasizes that infection control recommendations apply to all health care settings—including dental offices—as basic measures to prevent transmission of infection.
Patients and dental health care personnel (DHCP) may be exposed to a variety of pathogens in the dental setting. CDC emphasizes that its goal is to prevent health care-associated infections among patients, and injuries and illnesses among personnel.7
The routes of exposure to patients and DHCP may be direct or indirect. During delivery of care and functions associated with care, DHCPs have contact with blood, oral and respiratory fluids, and contaminated instruments. Adherence to standard precautions and, when indicated, transmission-based precautions is critical to the safe delivery of oral health care, as well as the safety of those who receive and provide those services.
The 2003 guidelines state that organisms can be transmitted via:7
- Direct contact with blood, oral fluids, or other patient materials.
- indirect contact with contaminated objects.
- Contact with droplet-containing oralmucosal microorganisms.
- Inhalation of airborne microorganisms.
HIERARCHY OF CONTROLS
 For universal precautions, standard precautions, and transmission-based precautions, there are hierarchies of controls designed to reduce or eliminate transmission of pathogens in the dental setting. The hierarchy is based on the specific pathogen.
For universal precautions, standard precautions, and transmission-based precautions, there are hierarchies of controls designed to reduce or eliminate transmission of pathogens in the dental setting. The hierarchy is based on the specific pathogen.
There are three different types of controls: engineering controls, work practice controls, and PPE. Engineering controls encompass equipment, devices, or instruments that remove or contain a pathogen. Puncture-resistant containers for sharps disposal and hand hygiene are examples of engineering controls.
Work practice controls are changes to technique that limit or remove the risk of exposure by modifying the way a task is performed. These include guidelines, policies, and procedures that explain how to perform tasks safely.8 PPE provides a barrier to pathogens and helps protect both clinicians and patients.8
With bloodborne transmission, engineering controls are most important. Work practice controls may be the most critical with other transmission-based precautions. The point is to select the appropriate control as the first line of defense.9
TRANSMISSION-BASED PRECAUTIONS
Transmission-based precautions consist of infection prevention and control measures, in addition to standard precautions. The added measures are determined by the mode of transmission of the infectious agent. These modes include direct or indirect transmission via contact, droplet, or airborne transmission. Transmission-based precautions complement standard precautions when standard precautions are not enough to prevent or reduce the risk of transmission. They may be used for a limited time or indicated only for specific infections.9
While the hierarchy of universal and standard precautions begins with engineering controls, the hierarchy for transmission- based precautions begins with work practice controls designed to identify infectious patients, defer elective treatment, and refer for medical consult. Additional infection control precautions, such as respiratory hygiene/cough etiquette, safe injection practices, and personal respirator use, are other measures that can effectively decrease the risk of transmission.
Examples of conditions that require the use of transmission-based precautions include severe acute respiratory syndrome, influenza, H1N1 influenza, tuberculosis, and multidrug-resistant organisms/ methicillin-resistant staphylococcus aureus (MRSA). Transmission-based precautions are used with patients who have highly transmissible pathogens for which additional precautions are necessary.
Transmission-based precautions are not indicated for human immunodeficiency virus, hepatitis B virus, or hepatitis C virus; these can be managed with standard precautions.9
AIRBORNE PRECAUTIONS
Airborne precautions are designed for the following:
- Reduce risk of transmission of infectious agents that remain suspended in air over long distances.
- Reduce the risk of transmission from patients who are known or suspected to be infected with pathogens spread by an airborne route.
- Reduce the risk of pathogens spreading that are less than 5 microns in size.
These precautions are intended to protect health care workers and other staff as well as any patients in an area of potential exposure.
TABLE 4. CONTACT PRECAUTIONS THAT ARE IN ADDITION TO STANDARD PRECAUTIONS.
- Covering the infected area(s) with a clean, dry bandage.
- Wearing gloves and using aseptic technique to dispose of patient bandages.
- Cleaning skin with an appropriate skin disinfectant.
- Maintaining aseptic technique throughout a procedure.
CONTACT PRECAUTIONS
Contact precautions are intended to prevent the spread of microorganisms by direct or indirect contact with a patient or the patient’s environment. Patients may be colonized with specific organisms that can be transferred to other patients, providers, or surfaces. Contact precautions may include isolating the patient from others, putting on PPE before entering a treatment area, and ensuring appropriate cleaning and disinfection of patient care areas. Table 4 lists the contact precautions that are in addition to standard precautions. Conditions that require contact precautions include herpes zoster, varicella, and MRSA.
HERPES ZOSTER
When treating patients with herpes zoster (varicella-zoster or shingles), the location and status of the lesion(s) are important to treatment planning. A lesion is considered infectious until it is no longer draining. In dental health care settings, care should be taken to prevent manipulation or irritation of lesions. If the lesion(s) is in an area at risk of opening during the care, it may be prudent to postpone care until the lesion is no longer draining or at risk of draining.
The first line of prevention is immunity of health care personnel. CDC recommends all health care personnel know their immune status to herpes zoster. CDC further recommends that nonimmuno/susceptible personnel be immunized with the varicella vaccine. Until they are vaccinated, nonimmune/ susceptible health care personnel should not provide direct patient care.
VARICELLA
Patients with varicella (chickenpox) are considered contagious until the lesions are dry and crusted. Elective dental care should be postponed until the patient is no longer contagious. Susceptible health care personnel should not enter the operatory if immune caregivers are available. For susceptible personnel who are exposed to varicella, post-exposure prophylaxis is recommended. Post-exposure vaccine is recommended within 120 hours of the incident.
For susceptible health care professionals for whom vaccine is contraindicated (immunocompromised persons, pregnant women), varicella zoster immune globulin (VZIG), when available, is recommended within 96 hours. If VZIG is unavailable, the application of intravenous immunoglobulin is suggested. Susceptible health care workers should not work beginning 8 days after first exposure until 21 days after last exposure, or 28 days if VZIG was administered, regardless of post-exposure vaccination.10
MRSA
Standard precautions are recommended for most outpatient dental health care settings and they are considered adequate, in most circumstances, to prevent the transmission of MRSA.11 Open wounds or lesions should be aseptically covered to prevent seepage.
Droplet precautions include measures intended to interrupt transmission of pathogens that do not remain infectious over long distances and are spread through close respiratory or mucus membrane contact. Droplet precautions are used for patients known or suspected to be infected with large particle droplets greater than 5 microns. Droplets may be generated by coughing, sneezing, talking, or during an aerosol-generating procedure. Influenza is an example of an infection that is transmitted via droplets.
VACCINATIONS
care personnel play an important role in protecting public health. CDC and the Advisory Committee on Immunization Practices (ACIP) recommend that all health care personnel, including DHCP, get an annual flu vaccine. However, CDC estimates that less than 50% of health care personnel get an annual flu vaccine. Health care workers should be fully vaccinated to safely provide patient care. Not only do vaccinations protect patients and colleagues, studies show that higher vaccination rates among health care personnel can reduce influenzalike illness, and even deaths, in settings such as nursing homes.12
INFLUENZA
Educating patients about influenza prevention strategies is important. This can be accomplished by posting visual alerts (in appropriate languages) at the entrance to outpatient facilities such as dental offices; instructing patients and those who accompany them to inform health care personnel of symptoms of a respiratory infection when they first register for care; and to practice respiratory hygiene/cough etiquette.
During periods of increased respiratory infection activity in the community, CDC recommends that health care facilities offer masks to patients who are coughing. Either procedure masks (with ear loops) or surgical masks (with ties) may be used to contain respiratory secretions. When space permits, coughing patients should be encouraged to sit at least 3 feet away from others in waiting areas. Health care personnel should follow droplet precautions (eg, wearing a surgical or procedure mask for close contact, hand hygiene, cough etiquette), in addition to standard precautions, when examining a patient with symptoms of a respiratory infection, particularly if fever is present. These precautions should be maintained until it is determined that the cause of symptoms is not an infectious agent that requires droplet precautions.12
CDC recommends that aerosol-generating procedures only be performed on patients with suspected or confirmed influenza if they are medically necessary and cannot be postponed. Limit the number of health care personnel present during the procedure to only those essential for patient care and support, and who have received the influenza vaccine.13 In dental practice settings, elective dental treatment should be postponed until the patient is no longer contagious (eg, without symptoms and fever free without ffever-reducingmedications for at least 24 hours).
TUBERCULOSIS
Active pulmonary infection with Mycobacterium Tuberculosis (Mtb) is an infection that requires airborne precautions. Airborne infection control considerations include appropriate ventilation systems for aerosol-generating procedures. Most dental practice settings do not have the necessary ventilation systems, so aerosol-generating procedures are contraindicated for patients with tuberculosis.
Airborne infection isolation rooms should only be used to provide urgent dental treatment to patients with suspected or confirmed infectious tuberculosis (formerly known as a negative-pressure isolation rooms). Use of high-efficiency particulate air filters (HEPA) or ultraviolet germi cidal irradiation is indicated in areas with high volume of suspected or confirmed tuberculosis patients.
TABLE 5. DESCRIPTION OF RISK CATEGORIES FOR TUBERCULOSIS.
Low risk
- Persons with tuberculosis not expected to be encountered; exposure unlikely.
Medium risk
- Persons with tuberculosis not expected to be encountered; exposure unlikely.
Potential ongoing transmission
- Temporary classification for any settings with evidence of person-to-person transmission of M. tuberculosis.
Respiratory protection controls further reduce risk of exposure in special circumstances. CDC recommends use of respiratory protection that is at least a disposable N95 filtering face piece when providing urgent dental treatment to patients with suspected or confirmed tuberculosis. CDC further recommends developing a comprehensive respiratory protection program that includes personnel training, fit-testing for personnel who will wear N95 respirators, post-exposure evaluation, and medical evaluation and follow-up for personnel exposed to Mtb. Patients should be instructed in the proper cough/etiquette and respiratory hygiene (wear a surgical mask). The risk of Mtb transmission in the dental settings is low. To date there has been only one documented case of transmission by direct inoculation of the oral cavity. A potential transmission of multidrug resistant tuberculosis between two dental workers with HIV is cited in the literature. However, tuberculin skin test conversions among dental professionals are rare.14
CDC recommends that all health care settings establish measures to prevent the transmission of Mtb, including staff education and patient assessment. Because community Mtb risk assessments vary depending on location, CDC recommends that dental practices seek guidance regarding developing, maintaining, and implementing a written Mtb infection-control plan; managing a patient with suspected or active tuberculosis; completing a community risk-assessment to guide employe tuberculin skin tests or Mtb blood tests and follow-up; and managing DHCP with tuberculosis.14
All settings should perform risk classification to determine the need for and frequency of an Mtb screening and testing program for DHCP (see Table 5). The prevalence of Mtb in the community and the type of practice are important considerations. For example, if the population you treat is at higher risk of tuberculosis than the general population, the dental office may be at medium risk.15
TUBERCULOSIS TESTING
CDC personnel screening and testing recommendations include initial baseline Mtb testing to prevent misinterpreting boosted reactions for new infections (Table 6).
TABLE 6. PERSONNEL SCREENING TUBERCULIN SKIN TESTING FREQUENCY.
Risk Category Frequency
Low
- Baseline on hire; further testing not required unless exposure occurs.
Medium
- Baseline, then annually.
Potential ongoing transmission
- Baseline, then every 8-10 weeks until evidence of transmission has ceased.
CDC suggests that those who have not had a tuberculosis test should take a two-step test. If the first test is positive, the person is considered infected (likely a latent infection). Those who have a negative first test should be retested 1 week to 3 weeks after the first test was read. If the second test is positive, the person is either infected (boosted reaction of previous infection) or has had previous vaccination with bacillus calmette-guérin (BCG). If the second test is negative, the person is considered not infected. It is important to note that boosted tuberculosis skin test reactions are not new infections.
Dental practices, even those not equipped to treat patients with tuberculosis, need guidelines for handling an Mtb infected patient before he or she is transferred to another facility. For example, protocols should be developed that describe respiratory hygiene and cough etiquette procedures; evaluation procedures; and referral arrangements.13 At a minimum, practice protocols should include policies and procedures to: identify persons with symptoms of tuberculosis; isolate them from other patients and staff; defer nonurgent dental treatment; and refer for medical evaluation and treatment.
CONCLUSION
The principles of standard precautions and the addition of transmission-based precautions are adaptable to the current infection control challenges. These measures are proactive in order to face newly emerging or re-emerging infections. Oral health care professionals must become familiar with these precautions, understand their application, and adhere to them consistently. In so doing, dental health care providers will deliver care to their patients in a safe environment.
REFERENCES
- CDC Isolation Techniques for Use in Hospitals. 2nd ed. Washington, DC: US Department of Health and Human Resources; 1975:80-8314.
- Garner JS, Favero MS. CDC guideline for handwashing and hospital environmental control, 1985. Infect Control. 1986;7:231-243.
- Centers for Disease Control (CDC). Recommend – ations for prevention of HIV transmission in healthcare settings. MMWR Morb Mortal Wkly Rep. 1987; 36(Suppl):1S-18S.
- Summers, CJ, Gooch BF, Marianos DW, Malvits DM, Bond WW. Practical infection control in oral health surveys and screenings. J Am Dent Assoc. 1994;125:113-117.
- Garner JS, Hospital Infection Control Practices Advisory Committee. Guideline for isolation precautions in hospitals. Infect Control Hosp Epidemiol. 1996;17:53-80.
- Boylard EA, Tablan OC, Williams WW, Pearson ML, Shapiro CN, Deitchmann SD. Guideline for infection control in healthcare personnel, 1998. HICPAC. Infect Contr Hosp Epid. 1998:19407-19463.
- Kohn WG, Collins AS, Cleveland JL, et al. CDC Guidelines for infection control in dental health-care settings—2003. MMWR Recomm Rep. 2003; 52(RR- 17):1-61.
- McDonald M, Evans N. Infection control guidelines for healthcare professionals. Available at: www.nursingceu.com/courses/257/index_nceu.html. Accessed June 3, 2011.
- Siegel JD, Rhinehart E, Jackson M, CHiarello L, Healthcare Infection Control Practices Advisory Committee. 2007 guideline for isolation precautions: preventing transmission of infectious agents in healthcare settings. Am J Infect Control. 2007 Dec;35(10 Suppl 2):S65-164.
- Occupational Safety and Health Standards. Personal Protective Equipment: Respiratory Protection. Available at: www.osha.gov/pls/oshaweb/owadisp.show_document?p_id=12716&p_table=standards. Accessed May 31, 2011.
- Klevens RM, Gorwitz RJ, Collins AS. Methicillinresistant Staphylococcus aureus: a primer for dentists. J Am Dent Assoc. 2008;139:1328-1337.
- Influenza vaccination information for health care workers. Available at: www.flu.gov/professional/hospital/hcworkers_vaccine.html. Accessed May 31, 2011.
- Update: Recommendations of the Advisory Com – mittee on Immunization Practices (ACIP) regarding use of CSL seasonal influenza vaccine (Afluria) in the United States during 2010 Centers for Disease Control and Prevention (CDC). MMWR Morb Mortal Wkly Rep. 2010;13;59:989-992.
- Cleveland JL, Robison VA, Panlilio AL. Tuberculosis epidemiology, diagnosis and infection control recommendations for dental settings: An update on the Centers for Disease Control and Prevention guidelines. J Am Dent Assoc. 2009; 140: 1092–1099.
- CDC Guidelines for Preventing the Transmission of Mycobacterium Tuberculosis in Health-Care Settings, 2005. Available at: www.cdc.gov/mmwr/preview/mmwrhtml/rr5417a1.htm. Accessed May 31, 2011.
From Dimensions of Dental Hygiene. June 2011; 9(6): 46, 48, 50-55.


