
Decision Making and Local Anesthesia
Selecting the most appropriate local anesthetic agent.
Clinicians must not become complacent in the selection of a local anesthetic—choosing an agent merely because “that’s what is available in the office” or “that’s what was set up on my tray.” Selecting the right drug is critical to the safe and effective administration of local anesthesia. The broad array of effective agents currently available creates a menu of options from which to choose, creating more opportunity for confusion.
A number of factors are important when selecting the most appropriate local anesthetic (LA) agent. Further, clinicians must be able to ascertain maximum recommended doses for each of the agents administered. Not only do we have a legal and ethical responsibility to choose the most appropriate anesthetic and dosage for each patient, but anything less is considered below today’s standard of care.
Questions to Consider
Before administering anesthesia on any patient, ask yourself, “have I considered?”
- The length of time required for both pulpal and soft tissue anesthesia,
- The procedure to be performed,
- The need for hemostasis, and
- The patient’s physical status, including potential drug interactions, based on information provided by the patient, either verbally or on the health history. To make an informed decision on each question, clinicians must have a strong background in the LA agents currently available.
The Agents
All five of the injectable local anesthetics currently used in the United States are on a level playing field. They prevent conduction of impulses to the central nervous system, they are chemically similar (all amides), and other than onset and duration of action, differences are subtle from a clinical standpoint. Additionally,evidence indicates all five are effective.1,2 The agents are: lidocaine (the first amide synthesized and considered the gold standard); mepivacaine (the least vasodilating agent); prilocaine (duration of action varies according to injection type, ie, infiltration vs block); articaine (the newest agent in the United States); and bupivacaine (the longest acting agent).
Vasoconstrictors
The choice of an LA agent is frequently related to which vasoconstrictor, if any, is most appropriate. Distinct advantages result from including a vasoconstrictor with anesthetic agents. For example, vasoconstrictors serve to prolong the duration of action of the anesthetic drug. Without a vasoconstrictor, an LA agent is very short acting. Decreasing blood flow in the area results in retention of the anesthetic solution at the injection site for a longer time period. Vasoconstrictors also delay the absorption of the LA into the bloodstream, thereby helping minimize the risk of toxicity. Additionally, vasoconstrictive action provides hemostasis in the area.
cardiovascular action. Besides useful vasoconstrictor (alpha receptor) properties, vasoconstrictors include beta receptor activities (vasodilation). The action of beta receptors found in the heart and skeletal muscle creates increased heart rate, cardiac muscle contraction, and blood pressure, as well as vasodilation of blood vessels. Consequently, when vasoconstrictors contact these receptors, potential for complications arise in patients with related health concerns and/or pharmacologic interactions.
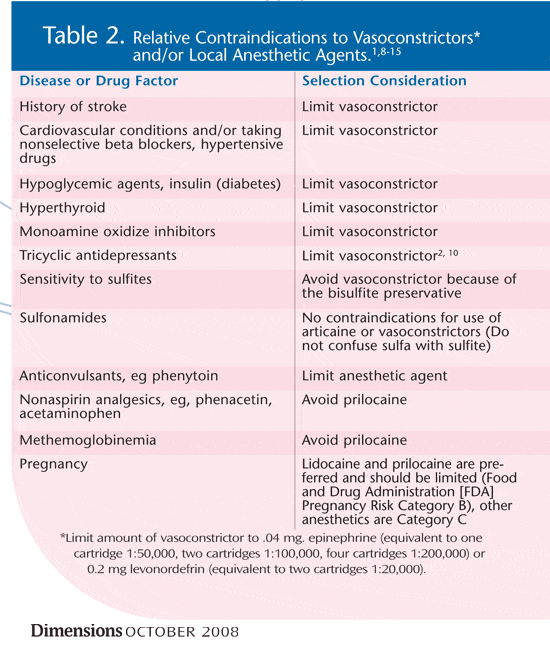
Monitoring blood pressure and heart rate pre-operatively is vital. In some situations, the amount of vasoconstrictor needs to be limited (or, infrequently, eliminated) and will be the drug that limits the amount of local anesthetic to be delivered to assure patient safety. Tables 1 and 2 provide a listing of broad categories of significant medical and drug history findings that limit either or both drugs. However, in normal dosages for the average healthy adult patient, the advantages of including vasoconstrictors far outweigh the risks.
Epinephrine and levonordefrin are the only two vasoconstrictors used in local anesthetic solutions in the United States. Three concentrations of epinephrine are available: 1:50,000, 1:100,000, and 1:200,000. Lidocaine is the only LA that contains a 1:50,000 concentration of epinephrine. This high concentration is needed predominantly when a clinician is trying to achieve hemostasis in a highly hemorrhagic localized area. Epinephrine 1:100,000 is found in lidocaine 2% and articaine 4%. Epinephrine 1:200,000 is found in articaine 4%, prilocaine 4%, and bupivacaine 0.5%. The maximum recommended dose for epinephrine is 0.2 mg per appointment for a healthy adult patient and .04 mg for patients requiring treatment modifications or the medically compromised. Levonordefrin (Neocobefrin®) is available in the United States only as a 1:20,000 concentration and is found only in the LA agent mepivacaine 2%. This vasoconstrictor is considered equivalent to epinephrine 1:100,000 although the ratio of its alpha and beta activities is somewhat dissimilar. Levonordefrin has less pressor potency than epinephrine, which might be useful for patients with cardiovascular disease. The maximum recommended dose for levonordefrin is 1.0 mg per appointment for a healthy adult patient and 0.2 mg for patients requiring treatment modifications or the medically compromised.
The preservative sodium bisulfite is added to LA solutions with vasoconstrictors to increase shelf life. Therefore, patients with sulfite allergies/ sensitivities should not receive an anesthetic with a vasoconstrictor. As a side note, many clinicians confuse “sulfite” with “sulfa” drugs and erroneously avoid the use of vasoconstrictors on patients with sulfonamide-related drug sensitivity. They are distinctly separate groups of drugs.
Duration Required
Duration of each agent varies for both pulpal and soft tissue anes thesia. Consideration should be given to the length of treatment time for both. Soft tissue anesthesia lasts longer than pulpal so the length of time required for pulpal anesthesia should be considered when selecting an appropriate drug. If short acting pulpal anesthesia is required (<20 minutes) and hemostasis is not a consideration, mepivacaine 3% (no vasoconstrictor) is a good selection. For longer appointments, a vasoconstrictor or a longer acting anesthetic, eg, prilocaine 4% plain for a nerve block, is necessary.
Duration times vary not only according to the drug’s biotransformation, but also according to type of injection administered (infiltration vs block), amount deposited, and available evidence. See Table 3 for the maximum recommended dosages and approximate duration times for each of the five available agents.1-6
Lidocaine
This anesthetic (trade name: Xylocaine®) is the shortest acting of all local anesthetics because it has greater vasodilating properties. Lidocaine is available without vasoconstrictor (lidocaine plain) or with a vasoconstrictor (1:50,000 or the more commonly used 1:100,000 epinephrine). In plain form, lidocaine’s duration is only 5-10 minutes for pulpal anesthesia and about 1-2 hours for soft tissue anesthesia. With the addition of epinephrine, its duration significantly increases to about 60-90 minutes for pulpal tissue and about 3-5 hours for soft tissue.
Mepivacaine
Like lidocaine, mepivacaine (trade names: Carbocaine ®, Polocaine®) is available with or without a vasoconstrictor. However, mepivacaine 3% (without a vasoconstrictor) produces longer duration of pulpal anesthesia (about 20-40 minutes) and soft tissue anesthesia of about 2-3 hours. With the addition of levonordefrin (Neocobefrin), pulpal anesthesia ranges from 60-90 minutes and soft tissue anesthesia from 3-5 hours.
Prilocaine
Prilocaine (trade name: Citanest®): Citanest Plain is without vasoconstrictor and Citanest Forte is with vasoconstrictor. Duration of anesthesia varies significantly based on the presence or absence of vasoconstrictor and type of injection administered. For prilocaine plain, an infiltration lasts about 5-10 minutes for pulpal anesthesia and 1-2 hours for soft tissue anesthesia. For a nerve block, pulpal anesthesia lasts approximately 40-60 minutes; soft tissue anesthesia lasts approximately 2-4 hours. With a vasoconstrictor, anesthesia may extend from 60-90 minutes of pulpal anesthesia and 3-8 hours1 of soft tissue anesthesia, regardless of type of injection. Because epinephrine is 1:200,000, prilocaine with epinephrine is a good choice for patients exhibiting cardiovascular disease or hyperthyroidism.
![]() Articaine
Articaine
Approved by the FDA for use in the United States in 2000, articaine (trade names: Zorcaine ™ and Septocaine®) 4% has a low risk of toxicity with effectiveness comparable to other local anesthetics. This anesthetic is only available with a vasoconstrictor. Zorcaine contains 1:100,000 epinephrine, and Septocaine is available with 1:100,000 or 1:200,000. Articaine is labeled as 1.7 ml of solution as compared to prilocaine’s 1.8 ml cartridge. Its duration of anesthesia for pulpal tissue is 45-75 minutes; soft tissue anesthesia is about 3-6 hours. Articaine’s high lipid solubility increases its diffusion, particularly on the maxilla, possibly eliminating the need for associated palatal injections. Because of increased lipid solubility leading to increased diffusion, fast onset, and lower toxicity, this anesthetic has gained popularity in the United States. Controversy exists regarding the use of articaine and increased incidents of paresthesia on the mandible. Early literature cautioned not to use this anesthetic on patients with sulfa-related drug allergy, however, later reports indicate there is no negative relationship between the use of articaine and sulfa allergy.7
Bupivacaine
Bupivacaine (trade name: Marcaine®), only available with a vasoconstrictor (epinephrine 1:200,000) is a long acting anesthetic with approximately four times the potency of other amides. It provides pulpal anesthesia from 1.5 to 5 hours and soft tissue anesthesia from 4-9 hours, thereby minimizing post-operative discomfort.
Procedure To Be Performed
In many offices, dental hygienists administer the injections for the dentist as well as their own patients. Obviously, extractions, surgical, and restorative procedures require extremely profound anesthesia, and if pain control is not profound throughout the procedure, extreme anxiety is created for everyone concerned. Types and amounts of anesthetics need to be customized for your particular practice. For example, a pediatric practice typically does not require the use of Marcaine, an anesthetic valuable in a periodontic or oral surgery practice.
To increase the comfort of patients, especially those with a fear of injections, a topical anesthetic can be administered first. Available in a variety of dispensing methods such as gels, sprays, patches, and subgingival delivery with blunt-tipped syringes, which would be used instead of an injection, a topical anesthetic can be used to numb the injection site before the local anesthetic is delivered. The amount of topical anesthetic used must be considered as part of the total amount of anesthesia provided. Dental hygienists need to be aware of the maximum recommended dosage for topicals. For more information on topical anesthetics, see “Safety First” by Kathy Bassett, RDH, MEd, and Arthur C. DiMarco, DMD, from the October 2007 issue.
Need for Hemostasis
Because LA agents have vasodilating properties, a vasoconstrictor should be included if hemostasis is a concern. Epinephrine is the vasoconstrictor of choice to control bleeding.1 Vasoconstriction is more effective for infiltration techniques in vascular sites than for blocks. Sometimes, supplementing mandibular blocks with infiltration-type injections is needed to achieve hemostasis.
Patient’s Physical Status
The health history must be updated thoroughly at each appointment to determine if any medical considerations or drug interactions contraindicate use of any agent. A few conditions indicate the need to reduce the amount of local anesthetic drug and several medical conditions may indicate the need for reduced dosage of the vasoconstrictor. Very few conditions or drug interactions absolutely contraindicate, ie, under no situation should the drug be administered, the use of either the anesthetic drug or vasoconstrictor.
Many patients may report having had a previous reaction or being sensitive to injections. Question the patient to establish if the reaction was related to the anesthetic or aresult of anxiety about the procedure/situation. Determine if the reaction was related to the anesthetic drug itself (very unlikely), the vasoconstrictor (somewhat unlikely), the sodium bisulfite preservative, an associated medical condition (somewhat likely), a drug interaction, or a “psychogenic” consideration (most likely).
With the growing number of people taking a larger number of pharmaceutical agents, reviewing their medications is paramount to avoiding potential complications. A drug reference should be readily available to review any unfamiliar drug the patient is taking prior to administering local anesthesia. Numerous websites supply information in a moment’s time, including www.rxlist .com and www.pdr.net.
Excellent articles and texts are available with information about indications and contraindications for various disease entities and/or potential drug interactions with LA agents. Naturally, conflicting opinions exist. Tables 1 and 2 present some broad categories of significant medical and drug history findings with implications for selecting an appropriate LA agent and vasoconstrictor, determining need to reduce dosage and contraindications. The information is presented from a practical standpoint. When information might be conflicting, the most conservative information is provided.1,8-15
Pediatric Patients
When administering local anesthesia on children, reviewing their health history and medication use with a parent/guardian and taking blood pressure is no less important than for adult patients. For example, many children take methylphenidate, methylin, or other drugs for attention deficit disorder or attention deficit hyperactivity disorder with risk of increased pulse or blood pressure. Calculation of the maximum dose for child patients is critical to prevent inadvertent toxicity.
![]() Anesthetics On Hand
Anesthetics On Hand
A well-supplied arsenal of LA agents should be available in dental practices. LA agents are reasonably priced so offices should be able to keep an assortment on hand. Consideration should be given to variety rather than quantity. When ordering LA agents for the office, keep in mind expiration dates so you do not over-order/stock any particular agent. LAs containing vasoconstrictors have a shelf life of approximately 1.5 years and those without vasoconstrictors are effective for about 4 years. Developing your own supply to have readily available is influenced by the particular practice setting, eg, pediatric versus periodontal practice, but might include at least one package of each of the categories summarized in Table 3 to cover nearly any eventuality.
Summary
Legal and ethical issues and the importance of safety during the administration of local anesthesia are crucial. Clinicians cannot afford complacency when choosing the appropriate anesthetic for a given patient or procedure. Selection should be carefully considered prior to use. By answering a few key questions, the choice can be simplified. Clinicians should have a variety of agents from which to choose and a thorough knowledge of each agent including recommended dosages and limitations.
References
- Malamed SF. Handbook of Local Anesthesia. 5th ed. St. Louis: Elsevier Mosby; 2004.
- Haas DA. An update on local anesthetics in dentistry. J Canadian Dent Assoc. 2002;68: 546-551.
- Moore PA, Boynes SG, Hersh EV, et al. The anesthetic efficacy of 4 percent articaine 1:200,000 epinephrine. J Am Dent Assoc. 2006;137:1572-1581.
- Rebolledo AS, Molina ED, Aytes LB, Escoda CG. Comparative study of the anesthetic efficacy of 4% articaine versus 2% lidocaine in inferior alveolar nerve block during surgical extraction of impacted lower third molars. Med Oral Patol Oral Cir Bucal. 2007;12:139-144.
- Becker DE, Reed KL. Essentials of local anesthetic pharmacology. Anesth Prog. 2006;53:98-109.
- Viana AM, deCampos AC, Morlin MT, Chin VKL. Plasma catecholamine concentrations and hemodynamic responses to vasoconstrictor during conventional or Gow-Gates mandibular anesthesia. Oral Surg Oral Med Oral Pathol Oral Radiol Endo. 2005;100:415-419.
- Overman PR. Articaine: a new alternative in dental hygiene pain control. J Dent Hyg. 2007;81:66.
- Pickett FA. The prescription pad and the dental office. Dimensions of Dental Hygiene, 2008;6(4):18-21.
- Spolarich AE. The top 20 most commonly prescribed medications for 2005. Access. 2006;20(10):39-48.
- Little JW, Fallace DA, Miller CS, Rhodus NL. Medical Management of the Medically Compromised Patient. 7th ed. St. Louis: Mosby Elsevier; 2008.
- Weyant R. There is minimal risk for adverse events in hypertensives associated with the use of epinephrine in local anesthetics. Review of systematic reviews. J Evid Base Dent Pract. 2007;7:60-61.
- Hersh EV, Giannakopoulos H, Levin LM, et al. The pharmacokinetics and cardiovascular effects of high-dose articaine with 1:100,000 and 1:200,000 epinephrine. J Am Dent Assoc. 2006;137:1562-1571.
- Paarmann C, Royer R. Pain Control for Dental Practitioners. Baltimore, Md: Wolters Kluwer/Lippincott Williams & Wilkins, 2008.
- Brown RS, Rhodus NL. Epinephrine and local anesthesia revisited. Oral Surg Oral Med Oral Pathol Oral Radiol Endo. 2005;100:401-408.
- Moore PA, Doll B, Delie RA, et al. Hemostatic and anesthetic efficacy of 4% articaine HCl with 1:200,000 epinephrine and 4% articaine HCl with 1:100,000 epinephrine when administered intraorally for periodontal surgery. J Periodontol. 2007;78:247-253.
From Dimensions of Dental Hygiene. October 2008; 6(10):24.

 Articaine
Articaine Anesthetics On Hand
Anesthetics On Hand