How Saliva Supports Remineralization
An important consideration in caries risk assessment and remineralization therapy selection is saliva.

An important consideration in caries risk assessment and remineralization therapy selection is saliva. It is a critical biological and protective factor in the remineralization of enamel. Saliva’s buffering capacity and flow of secretion are directly related to the rate and extent of demineralization. Saliva can neutralize acids, form a protective membrane on tooth surfaces, and enhance remineralization by providing calcium, phosphate, and fluoride to enamel and dentin. The pH level of saliva directly affects remineralization through the amount of calcium and phosphate ions available to the enamel via saliva in times of acidic challenge. Saliva can act as a replenishing source and inhibit tooth demineralization during periods of low pH, while promoting tooth remineralization when the pH returns to a neutral state.
Photo Credit: SolStock / iStock / Getty Images Plus
Tipping the Scales Toward Demineralization
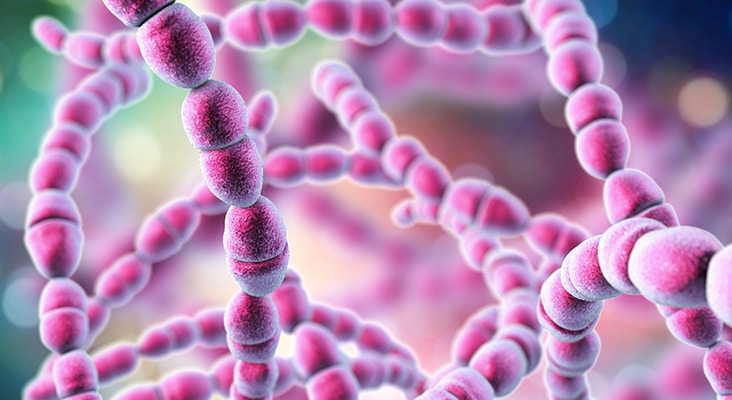
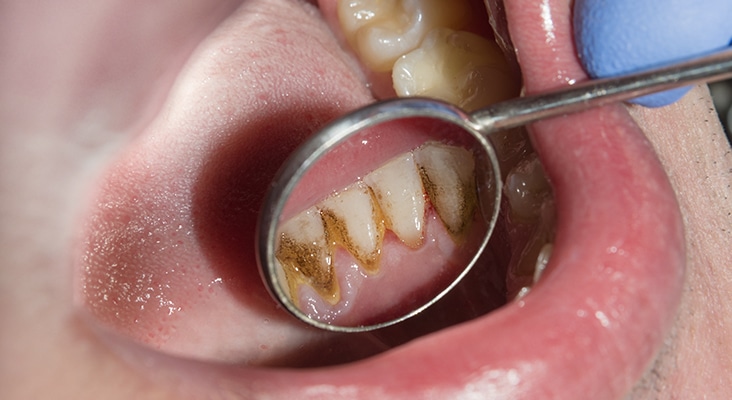
Demineralization is the process of removing mineral ions from hydroxyapatite crystals of hard tissues, such as enamel, and when unchecked, can result in caries development. Demineralization is a continuous, cyclical process that includes remineralization, during which saliva plays a key role. The demineralization process takes place on the tooth surface when biofilm—consisting of both bacterial plaque and the pellicle—is present on the enamel and dentin. When fermentable carbohydrates are ingested, Lactobacillus and Streptococcus bacteria in the biofilm metabolize the carbohydrates and produce acid. This acid is then able to diffuse across the tooth surfaces, dissolving the minerals in the enamel and dentin.
Photo Credit: Dr_Microbe / iStock / Getty Images Plus

Assisting the Remineralization Process
Patients with reduced salivary flow and/or compromised buffering potential need assistance with the remineralization piece of the cycle. While it is important to prevent early lesions, identifying caries lesions in the early stages of the demineralization process while the condition is still reversible is critical. Oral health professionals can intervene with preventive remineralization therapies before the process becomes irreversible.
Photo Credit: CarlaNichiata / iStock / Getty Images Plus

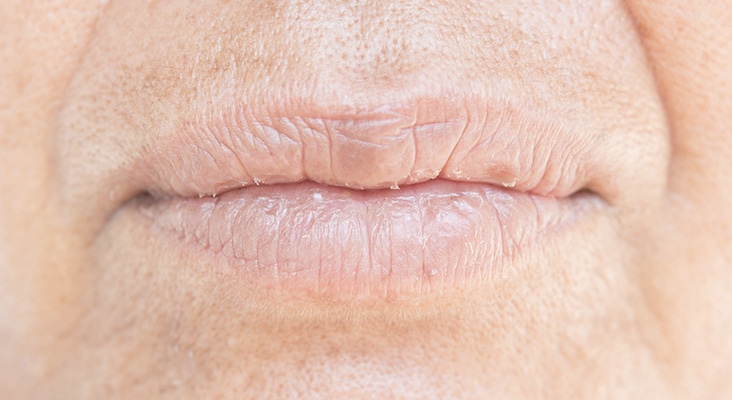
Hyposalivation
Hyposalivation and/or xerostomia is a decrease in salivary flow and is characterized by oral dryness. It can be caused by medications; autoimmune diseases, such as Sjögren syndrome; radiotherapy/chemotherapy; and hormone disorders. Approximately 30% of patients between the ages of 20 and 69 have xerostomia. Medications are the most common cause of dry mouth. As life expectancy grows, the prevalence of dry mouth increases, due to the number of medications prescribed for various health conditions.
Photo Credit: designer491 / iStock / Getty Images Plus
Determining Saliva Flow Rate
Assessment of salivary gland function should be included in routine dental visits, as it is essential in diagnosing salivary gland hypofunction as the cause of xerostomia. Clinicians generally use a subjective approach to identify and assess dry mouth, such as a patient’s response to a health questionnaire or medical history form. However, an objective measurement of qualitative or quantitative changes in saliva is ideal and best captured by collecting whole saliva or saliva from individual glands.
Photo Credit: Srisakorn / iStock / Getty Images Plus

Substitutes for Saliva
Several saliva substitutes and stimulants are available for patients with salivary gland hypofunction in the form of sprays, gels, oils, mouthrinses, and chewing gums. Each option differs with respect to the base substance, chemical composition, viscosity, and patient preference. Other treatment options directly impact the remineralization process. There is conflicting research as to whether one therapy is better than another. Certain salivary substitutes have reportedly increased demineralization by significantly decreasing intraoral pH. Patients with xerostomia may want to use high-viscous saliva substitutes and avoid saliva substitutes with low pH or citric acid.
Photo Credit: ValentynVolkov / iStock / Getty Images Plus

Fluoride Can Help
The use of professionally applied fluoride in combination with at-home fluoride products may enhance remineralization. Poor salivary contact and limited accessibility to interproximal surfaces make it difficult to manage incipient caries lesions. Songsiripradubboon et al investigated the remineralization properties of fluoride mouthrinses used at different times in conjunction with fluoride toothpaste on incipient caries lesions. Results showed that twice daily use of 0.05% sodium fluoride mouthrinse combined with twice daily use of fluoride toothpaste yielded the greatest remineralization of incipient caries.
Photo Credit: designer491 / iStock / Getty Images Plus
Calcium Phosphate Technologies
Fluoride, calcium, and phosphate are needed to aid in the remineralization process during a cariogenic attack. Amorphous calcium phosphate (ACP), a combination of soluble salts of calcium and phosphorous, may help to remineralize tooth structure. Peric et al evaluated the effect of casein phosphopeptide-ACP (CPP-ACP) and casein phosphopeptide-amorphous calcium fluoride phosphate (CPP-ACFP) pastes in patients with Sjögren syndrome. Results indicated that patients who used these pastes experienced a slight increase in salivary pH values, a significant rise in plaque pH values, and partial or complete occlusion of enamel defects. Other options used to support remineralization include calcium sodium phosphosilicate (NovaMin) and tricalcium phosphate.

