
Visual Acuity Without Injury
Reduce your risk of work-related musculoskeletal disorders with magnification loupes and co-axial illumination.
Due to the repetitive and precise nature of their work, dental hygienists are at a high risk of work-related musculoskeletal disorders (WMSDs). One of the main factors involved in WMSDs is poor working posture due to the need for clear visualization of the oral cavity, which often leads to excessive head tilt and awkward movement of the back.1 In order to increase visual acuity without inflicting injury, the proper selection of loupes and coaxial illumination is important.
Magnification Loupes
Studies show that the use of magnification loupes can help improve posture.2,3 However, the use of improperly selected or adjusted loupes can be further damaging to the musculoskeletal health of the clinician while increasing eye strain. Dental hygienists should be well-versed in basic magnification terminology when choosing loupes (see Figure 1).
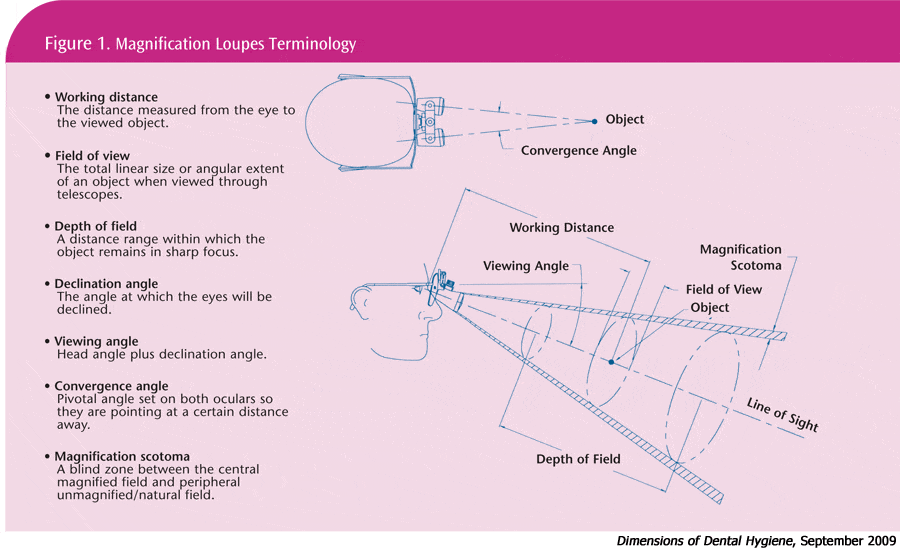 The working distance is the measurement between the plane of the eye and the surface being treated. The working range of magnification loupes is determined by the measurement between the closest and farthest distances where the object is kept in focus.1 Working distances typically range from 11 inches to 18 inches and are unique to the individual.4 The ideal working distance should be the middle point of the loupes’ working range.1
The working distance is the measurement between the plane of the eye and the surface being treated. The working range of magnification loupes is determined by the measurement between the closest and farthest distances where the object is kept in focus.1 Working distances typically range from 11 inches to 18 inches and are unique to the individual.4 The ideal working distance should be the middle point of the loupes’ working range.1
The size of the working area that can be viewed within the oral cavity is defined as the width of field or field of view. As magnification and image size increase, the width of the area that can be viewed through the loupes decreases. In other words, a pair of 2.0 x magnification loupes has a greater width of field than 2.5 x magnification loupes.5 Maintaining the ability to hold images in focus as the head moves is more difficult when the magnification power increases and the width of field decreases.1 Higher magnification levels also increase the blind spot between the magnified central view and the outside unmagnified view.6
Depth of field refers to the ability of the loupes to focus on objects near and far within the width of field without compensating with back and forth head movement. The greater the magnification, the less the depth of field. In other words, a pair of 2.0 x magnification loupes allows for approximately 5 inches of depth in the working area without movement of the clinician’s head. Thus, the lower magnification will result in greater latitude of clarity to the depth of field.7 The depth of field is dependent on each dental professional’s ability to adjust his or her vision, with older clinicians usually maintaining a shorter depth of field.1 Because the working distance changes for various procedures, the depth of field of magnification loupes should be large enough to use during many different tasks.1
 One of the most important factors to consider when choosing loupes is the declination angle, which is the angle that the eyes must assume to look downward into the oral cavity. Typically this can have a wide range of variation—from 15° to 44°.8 A correct measurement of this angle prior to purchase is important to prevent strain to the neck and shoulders. Figure 2 demonstrates the relationship between fatigue and head tilt angle. Too little of an angle causes clinicians to flex their head and neck forward in an awkward position. Too great of an angle causes eyestrain as clinicians must force the eyes downward to look through the severely angled lenses.5,8
One of the most important factors to consider when choosing loupes is the declination angle, which is the angle that the eyes must assume to look downward into the oral cavity. Typically this can have a wide range of variation—from 15° to 44°.8 A correct measurement of this angle prior to purchase is important to prevent strain to the neck and shoulders. Figure 2 demonstrates the relationship between fatigue and head tilt angle. Too little of an angle causes clinicians to flex their head and neck forward in an awkward position. Too great of an angle causes eyestrain as clinicians must force the eyes downward to look through the severely angled lenses.5,8
Types of Loupes
There are three types of loupes currently available: fixed through the lens (TTL), front-lensmounted (FLM) without vertical adjustment, and FLM with vertical adjustment. Fixed TTL loupes are permanently mounted in the eyeglass lenses. Their declination angle cannot be adjusted and vision correction must be built into the lenses. If a dental professional experiences vision changes, the loupes must be remade.9
FLM loupes without vertical adjustment typically allow the dental professional to adjust the interpupillary distance for different users but like TTL loupes, their declination angle cannot be adjusted. Some loupes allow the dental professional to adjust the convergence angle, which can create issues with alignment.1
FLM loupes with vertical adjustment provide the ability to set the declination angle for the most comfortable neck posture. This type of loupe has a mounting fixture with double hinges and a vertical slide that provides the ability to change the declination angle when performing different procedures.
Co-Axial Illumination
Often magnification loupes are accented by attached lighting devices called co-axial illumination systems. These systems not only add to the amount of light available in the working area but also help in the direction of light. Coaxial illumination systems deliver a direction of light that is parallel to the sight line. They are designed to provide shadow-free illumination and improve working posture.1
Understanding how light passes through the eye is integral to comprehending illumination. Light first enters through the clear cornea that covers the front of the eye and helps focus inward light. The light then flows through a watery fluid called the aqueous humor and through the colored part of the eye or iris. The iris dilates and constricts as light conditions change, controlling the amount of light allowed to enter the pupil of the eye. After light travels through the pupil, it enters the lens. The lens of the eye is responsible for focusing the light. It can change shape to facilitate focusing on distant or nearby objects. The amount of light impacting the iris plays a part in the ability of the eye to focus on an object. Therefore, by controlling the light in the working area with co-axial illumination, the clinician can improve visual acuity.1
1,10 Physical symptoms, such as vertigo, eye soreness, and poor posture, may be the result of improper lighting.
Often the dental office presents background and operatory lighting that is brighter than the intraoral work site, which creates glare. Ideal lighting requires the consideration of the ratio of target brightness to the brightness of the intraoral work site or the target-to-background brightness ratio (T/B ratio). The intraoral work site should be at least three times brighter than the background. Co-axial illumination systems allow the clinician to adjust the intraoral lighting to a level that contrasts comfortably with background light.1 Clinicians must also consider the T/B ratio when self-assessing for musculoskeletal discomfort.
Many co-axial headlights are available for dental applications. Important factors for selecting the most suitable headlight are adjustment of brightness, beam uniformity, and weight. The optimal brightness varies according to both the user’s age and the objects to be examined. In general, older people need more light. Therefore, the user should be able to precisely adjust the brightness for different procedures to achieve the maximum visibility and the maximum comfort for eyes.
References
- Chang BJ. Ergonomic benefits of surgical telescope systems: selection guidelines. J Calif Dent Assoc. 2002;30:161-169.
- Branson BG, Bray KK, Gadbury-Amyot C, et al. Effect of magnification lenses on student operator posture. J Dent Educ. 2004;68:384-389.
- Maillet JP, Millar AM, Burke JM, Maillet MA, Maillet WA, Neish NR. Effect of magnification loupes on dental hygiene student posture. J Dent Educ. 2008;72:33-44.
- Sunell S, Rucker L. Surgical magnification in dental hygiene practice. Int J Dent Hyg. 2004;2:26-35.
- Valachi B. Taking dental ergonomics to a new level: avoiding the ten common mistakes dental hygienists make. Contemporary Dent Hygiene. 2005;5:8-14.
- Rucker LM. Surgical telescopes: posture maker or posture beaker? In: Murphy D, ed. Ergonomics and the Dental Care Worker. Washington DC: American Public Health Association; 1998:191-216.
- Strassler HE, Syme SE, Serio F, Kaim JM. Enhanced visualization during dental practice using magnification systems. Compend Contin Educ Dent. 1998;19:595-612.
- Osuna T. Magnification in dental hygiene. Access. 2003;1:1-8.
- Michaelides P, Stambaugh R. Boosting your optical acumen. Dimensions of Dental Hygiene. 2005;(4):16-21.
- Smith G, Atchison DA. The Eye and Visual Optical Instrument. New York: Cambridge University Press; 1997.
From Dimensions of Dental Hygiene. September 2009; 7(9): 46, 48-49.

