Update on Ultrasonics
Ultrasonic instrumentation is integral to the success of periodontal therapy but its efficacy depends on the skills of the clinician.
For more than 4 decades, dental hygiene practice has benefited from powered instrumentation. It can achieve the same clinical outcomes as manual instrumentation, while reducing time and operator fatigue.1-4 However, the efficacy of powered instrumentation is dependent on the skill, technique, and knowledge of the clinician using it.
Historically, magnetostrictive ultrasonic devices have been the most popular in the United States, which has resulted in the term “ultrasonic scaling” being universally applied to all types of powered instrumentation. Reference to specific types of mechanized devices will be noted in this article; the term “ultrasonic” will refer only to instrumentation with a power driven device. Mechanized devices are classified by frequency and tip motion (Figure 1).
When is ultrasonic instrumentation appropriate?
For patients with supra- or subgingival plaque and/or calculus, ultrasonic instrumentation is effective, efficient, and can be more gentle on the gingival tissues, while also being less stressful for the clinician.1 If contraindications do not exist for ultrasonic use, the question is not when to use an ultrasonic device but rather what tip, what power, and what frequency should be used. Determining what proportion of time should be spent using ultrasonic instrumentation in combination with manual instrumentation in order to achieve optimum results is also an important factor.
What tip design is most appropriate?
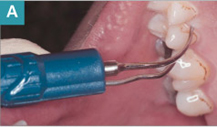
Choosing the correct tip design increases thoroughness, efficiency, and patient comfort. For patients with moderate to heavy supragingival or submarginal calculus, a standard tip insert design on medium to high power should be used (Figure 2). The standard inserts have enough bulk (mass/surface area) to remove the calculus with relative ease. Standard inserts include universal, triple-bend, beaver-tail, chisel, and periodontal probe-like tip designs (Figure 3). In addition to the tip design, the swivel design feature that is now available on the grip of the insert or on the base of the handpiece allows ease in rolling the insert to achieve improved insertion, angulation, and access without stopping instrumentation, removing the insert from the mouth, and rotating the insert to the desired position. The swivel feature also minimizes the drag from the handpiece cord, creating a more ergonomic instrument.
.gif)
Figure 1.Comparison of powered scaling devices.
|
|
|
For patients with light to heavy plaque and/or soft debris (either supra or subgingival) in the presence of inflammation or light supragingival calculus, a thin tipped insert on low to medium power is an appropriate choice (Figure 4a). The thin tips are also slim enough to access tight contacts and increase patient comfort when light deposits are subgingival.
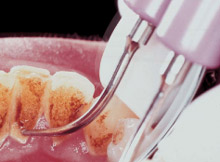
Candidates for scaling and root planing will require a variety of ultrasonic inserts and a specific sequence should be followed. Initially a standard insert on medium to high power is necessary to remove as much of the supra and subgingival calculus and debris as possible. Local anesthesia should be considered to allow access with the larger tips on high power along with the thinner insert tips and manual instruments so that the procedure can be comfortably tolerated by the patient. Thinner tip inserts are not designed or intended for removal of moderate to heavy calculus and should only be used after instrumenting with the bulkier standard inserts (Figure 5). After heavy deposits are removed, the entire subgingival surface should be explored and residual detectable deposits should be removed with slenderized periodontal tip insert designs (Figure 4b). The use of Gracey curets, mini-bladed curets, or Hirschfeld files should be considered if access is difficult even with thinner insert designs.
Several ultrasonic instruments offer specialized furcation tip designs. Studies show that hand instruments alone are not always adequate in debriding Class II and III furcations.1,5 As with the use of all ultrasonic tips, care must be taken not to create grooves in the root surface.
|
|
|
| Figure 4. Thin perio tip used on patient exhibiting plaque at the gumline (A) and with deep periodontal pockets (B). | |
What is the difference between manually-tuned and auto-tuned?
The first ultrasonic units for periodontal instrumentation were manually-tuned, meaning that the frequency could be controlled as well as the power and water. The majority of units today are auto-tuned, meaning that the frequency is adjusted automatically at maximum efficiency. Frequency translates to the number of times the tip vibrates each second. For example, when a magnetostrictive tip is marked 25 KHz or 30 KHz, this means the tip vibrates 25,000 cycles per second (cps) or 30,000 cps, respectively. Therefore, in manually-tuned units, the operator can control the number of times the tip contacts the calculus/debris. The more times the tip contacts the calculus/debris, the greater the chance for removal. In manually-tuned units, the frequency can be lowered for debridement and for when less tenacious calculus is present, maximizing patient comfort and potentially decreasing the undesirable effect of instrumentation on the root surface.
Previously, when preparing the ultrasonic device for patient care, the operator adjusted the water and power until a fine mist spray was achieved at the tip, creating aerosols. Today, a heavy drip or light mist-drip combination is recommended for light debris removal and deplaquing.6 This flow is still sufficient to allow for continuous irrigation, cooling, cavitation, and lavage while reducing aerosol water mist production.
 Figure 5. Thin tips from left to right: Piezo tips: ProDenTec UltraSlim® Right Curve tip; Satelec PerioFine PFR Right tip; EMS PL2 Right perio slim tip. Magnetostrictive tips: Hu-Friedy After Five® PLUS™ Right tip and Dentsply Cavitron SlimLine™ right tip. |
 Figure 6. Piezo tips from left to right: ProDenTec straight slim tip; Satelec #10 tip; and EMS PS tip. Magnetostrictive tips: Parkell Burnett Power tip; Dentsply Cavitron FSI #10 tip; and Hu-Friedy Satin Swivel #10 universal tip. |
How does amplitude affect ultrasonic instrumentation?
Clinicians often mistake frequency for power. The power behind ultrasonic instrumentation is not determined by frequency alone, but rather by a combination of frequency and amplitude. Where frequency controls the number of vibrations, amplitude determines the length of the stroke or the length of the vibration. The greater the amplitude, the further the tip travels. High power equals longer, more powerful strokes whereas low power equals shorter, less powerful strokes. An analogy of this concept is of a ball and crane preparing to demolish a building. If the ball were just a few feet away from the building prior to making contact, it would not be very powerful in knocking it down. The further the ball is away from the building prior to the swing, the more powerful it will be in its demolition. The power control knob on the ultrasonic unit adjusts the amplitude of the tip. When heavy and/or tenacious calculus is present, increasing the power will be more effective in its removal.
When selecting a powerful ultrasonic scaling device, attention must be given to not only high frequency, but also the amplitude range of the unit. The ideal device will have a wide amplitude range in order to adapt the power setting for various tasks.
Numerous systematic reviews have been published comparing magnetostrictive and piezoelectric units with conflicting results.1-3 Some studies conclude piezoelectric ultrasonics leave root surfaces smoother and increase patient comfort, while other studies have found rougher roots and increased patient discomfort with the equipment.1-3 Both magnetostrictive and piezoelectric units have a variety of inserts and tip designs available and appear to be equally effective in calculus removal (Figure 6).1,7
Piezoelectric ultrasonic units claim to produce less heat during instrumentation than magnetostrictive units. Although the water reduces friction at the tip and facilitates lavage, its flow can be minimized. Other claims include piezoelectric units are more efficient at calculus removal because the vibrations on the tooth surfaces are more powerful.7
Some piezoelectric units require a torque tool to secure and remove the tips from the handpiece. This requirement can be more disruptive than changing magnetostrictive tips during treatment. Piezoelectric units do not affect pacemakers because the energy is produced by ceramic crystals without generating a magnetic field. They are widely used in Europe and Asia.
The research group Clinical Research Associates is the Consumer Reports of dental products and techniques. A 2003 newsletter featured an evaluation of 11 ultrasonic scalers available in the United States.7 The report details the tips selected for best performance, trends in tip design, and ways to optimize scaler performance. Magnetostrictive scalers were recognized for their broad selection and interchangeable inserts between brands as long as the frequency is the same. Unit type—magnetostrictive vs piezoelectric—did not increase the occurrence of burnished tenacious calculus as such deposits were observed for some units in both groups. Performance recommendations include: tip replacement frequency consistent with use, use of larger diameter tips for tenacious deposit, and use of finer tips for improved tactile sensation and better access.
How can aerosols and splatter be reduced?
Regardless of which ultrasonic unit or insert is used, aerosols and splatter are produced, potentially transmitting pathogenic microorganisms and increasing airborne bacteria.1,8-11 Although documented transmission of disease has not been reported via aerosols when using ultrasonic devices, the potential is present, therefore the operator must try to reduce this risk. First, wearing a high filtering and properly fitting facemask greatly reduces the operator’s risk of inhaling contaminated aerosols.9-11 Second, the use of a preprocedural chlorhexidine or essential oil mouth rinse for approximately 1 minute prior to beginning treatment reduces the microbial content of aerosols during ultrasonic instrumentation.9-11 Finally, high volume evacuation has been shown to best reduce aerosols when using ultrasonics. It is the method recommended by the American Dental Association and the Centers for Disease Control and Prevention.9-11 The operator should position the evacuator tip near the teeth with one hand while scaling with the other hand.
However, high volume evacuation may not be a practical choice when the operator is working alone, therefore, a slow speed saliva ejector is often used because of its maneuverability and ease. Unfortunately, aerosols are not removed when only saliva ejectors are used.10 Studies have shown significant aerosol reduction with a high volume evacuation device that attaches to the ultrasonic handpiece and an extraoral evacuator tip positioning device.8-11 Also, there is a new device that isolates the quadrant and incorporates high volume evacuation and fiber optic light.
do other occupational risks exist?
Musculoskeletal and auditory damage are two other occupational risks in addition to aerosol contamination. The effects of solely ultrasonic instrumentation on the neurological and musculoskeletal health are difficult to isolate because dentists and dental hygienists alike use a variety of instruments that cause vibration. A reduction in strength and tactile sensitivity was observed in women dentists and dental hygienists when compared to women dental assistants and medical nurses who were not exposed to vibration.12 Other observations have shown impaired sensory perceptions in the dominant vs nondominant hands of dental personnel.13 Further research is necessary to confirm the effect of ultrasonic instrumentation on neurological and musculoskeletal function.
Tinnitus, an early sign of hearing loss, has been reported following ultrasonic use by both clinicians and patients.14 Empirical studies comparing tinnitus following a single episode of ultrasonic use report contradictory results with 0% to 50% of the subjects tested experiencing auditory symptoms. Overall, the hearing ability of dental personnel does not differ from that of nondental controls indicating that occupational exposure to ultrasonic instruments is not harmful to hearing.15
Why cover all subgingival tooth surfaces rather than just remove the detectable deposits?
Calculus deposits are certainly important to remove primarily because they are a haven for biofilm attachment. Pathogenic biofilms, which are found mainly in deep pockets (>4 mm), are not detectable and are highly resistant to antimicrobial agents and systemic antibiotics. The only way to totally disrupt the biofilm is through mechanical removal.16,17 Because we cannot see or feel a biofilm, we must assume it is present on every aspect of the tooth surfaces. Therefore, it is crucial when instrumenting to cover every square millimeter of subgingival tooth surfaces with continuous, methodical overlapping strokes, in closely spaced channels, to mechanically disrupt and remove the biofilm colonies. Ultrasonic instrumentation under low power is sufficient to accomplish this task but not to remove calculus.
Conversely, shallow pocket depths (<3 mm) in the absence of clinically detectable calculus may not require instrumentation at all. A systematic review of scaling and root planing outcomes clearly demonstrates that instrumentation of initially shallow sites may cause attachment loss.18 Shallow pockets in the absence of inflammation are likely colonized by beneficial flora and need not be disrupted.
Does antimicrobial irrigation make a clinical difference?
Many ultrasonic manufacturers offer units with self-contained irrigation devices so that antimicrobial agents can be incorporated during ultrasonic instrumentation. The advantages of using antimicrobial lavage instead of plain water have not been well-documented. Studies have not shown any marked difference in reduction of probe depths when antimicrobials are used versus water in mild to moderate pockets.1 Studies that have shown a statistical difference in probe depths after using an antimicrobial showed an overall improvement of only 0.5 mm and this improvement was found predominantly in severely deep pocket depths.1
The use of simultaneous ultrasonic instrumentation and antimicrobial irrigation with chlorhexidine has demonstrated only transient changes in the subgingival flora with no corresponding clinical benefit.19 Such findings are consistent with others that found that mature biofilm colonies have an enhanced resistance to antimicrobial agents and antibiotics.16,20 A rationale for this resistance is that antimicrobial agents fail to penetrate the full depth of the biofilm.21 While antibiotics are effective on single cell bacteria (planktonic), new research is showing they are not completely effective against biofilm colonies that cause periodontal disease.16,17,20-21
Is manual instrumentation necessary in addition to ultrasonic instrumentation?
Numerous studies have compared manual to ultrasonic instrumentation in regards to efficiency. In general, these studies indicate that manual instrumentation takes longer to achieve the same clinical results as ultrasonic instrumentation.4 Disregarding the time required to achieve clinical end-points, there is no significant difference between the efficacy of manual and ultrasonic instrumentation.4 Yet to achieve the desired clinical result, access is not always ideal with either manual or ultrasonic instruments, especially in anatomically difficult situations. A combined approach considering instrument access and personal preference with both manual and ultrasonic instruments must be used. Independent of instrument selection, effectively trained operators are crucial to thorough debridement. Less trained operators have been shown to attain lower levels of efficacy in debriding root surfaces regardless of instrument selection. Proficiency with both manual and ultrasonic instruments is just as important as the instrument of choice.22
Summary
Understanding the basic concepts of ultrasonic instrumentation will assist the practitioner in choosing the most appropriate inserts and knowing when best to use them. For the majority of patients undergoing treatment for routine prophylaxis, scaling and root planing, or periodontal maintenance therapy, ultrasonic instrumentation is an important treatment modality. When adapted to a patient’s individual periodontal needs and applied with sound professional skills and judgment, ultrasonic instrumentation can play a vital role in the success of periodontal therapy and the long-term maintenance of gingival health.
References
- Drisko CL, Cochran DL, Blieden T, et al. Position paper: sonic and ultrasonic scalers in periodontics. Research, Science and Therapy Committee of the American Academy of Periodontology. J Periodontol. 2000;71:1792-1801.
- Busslinger A, Lampe K, Beuchat M, Lehmann B. A comparative in vitro study of a magnetostrictive and a piezoelectric ultrasonic scaling instrument. J Clin Periodontol. 2001;28:642-649.
- Cross-Poline GN, Stach DJ, Newman SM. Effects of curet and ultrasonics on root surfaces. Am J Dent. 1995;8:131-133.
- Cobb CM. Clinical significance of non-surgical periodontal therapy: an evidence-based perspective of scaling and root planing. J Clin Periodontol. 2002;29(suppl):6-16.
- Sugaya T, Kawanami M, Kato H. Effects of debridement with an ultrasonic furcation tip in degree II furcation involvement of mandibular molars. J Int Acad Periodontol. 2002;4:138-142.
- Guignon AN. Expanding the role of ultrasonic scaling in clinical practice. Journal of Practical Hygiene. 2000; 9:30-33.
- Clinicians’ Guide to Dental Products and Techniques. Clinical Research Associates Newsletter. 2003;27:10.
- Rivera-Hidalgo F, Barnes JB, Harrel SK. Aerosol and splatter production by focused spray and standard ultrasonic inserts. J Periodontol. 1999;70:473-477.
- Klyn SL, Cummings DE, Richardson BW, Davis RD. Reduction of bacteria-containing spray produced during ultrasonic scaling. Gen Dent. 2001;49:648-652.
- Jacks ME. A laboratory comparison of evacuation devices on aerosol reduction. J Dent Hyg. 2002;76:202-206.
- Trenter SC, Walmsley AD. Ultrasonic dental scaler: associated hazards. J Clin Periodontol. 2003;30:95-101.
- Akesson I, Lundborg G, Horstmann V, Skerfving S. Neuropathy in female dental personnel exposed to high frequency vibrations. Occup Environ Med. 1995;52:116-123.
- Hjortsberg U, Rosen I, Orbaek P, Lundborg G, Balogh I. Finger receptor dysfunction in dental technicians exposed to high-frequency vibration. Scand J Work Environ Health. 1989;15:339-344.
- Coles RR, Hoare NW. Noise-induced hearing loss and the dentist. Br Dent J. 1985;159:209-218.
- Wilson CE, Vaidyanathan TK, Cinotti WR, Cohen SM, Wang SJ. Hearing-damage risk and communication interference in dental practice. J Dent Res. 1990;69:489-493.
- Chen C, Rich SK. Biofilm basics. Dimensions of Dental Hygiene. 2003;1(1):22-25.
- Matsuda SA. Instrumentation of biofilm. Dimensions of Dental Hygiene. 2003;1(1):26-30.
- Cobb CM. Non-surgical pocket therapy: mechanical. Ann Periodontol. 1996;1:443-490.
- Slots J. Selection of antimicrobial agents in periodontal therapy. J Periodontol Res. 2002;37:389-398.
- Costerton JW, Stewart PS, Greenberg EP. Bacterial biofilms: a common cause of persistent infections. Science. 1999;284:1318-1322.
- Gilbert P, Das J, Foley I. Biofilm susceptibility to antimicrobials. Adv Dent Res. 1997;11:160-167.
- Ruhling A, Schlemme H, König J, Kocher T, Schwahn C, Plagmann HC. Learning root debridement with curettes and power-driven instruments. Part I: a training program to increase effectivity. J Clin Periodontol. 2002;29:622-629.
From Dimensions of Dental Hygiene. May 2004;2(5):22, 24, 26, 28-29.