 EDWARDOLIVE/ISTOCK/GETTY IMAGES PLUS
EDWARDOLIVE/ISTOCK/GETTY IMAGES PLUS
Ultrasonic Insert/Tip Selection for First Molar Teeth
Choosing the most appropriate ultrasonic inserts/tips for the task at hand is integral to effective ultrasonic instrumentation of this area of the dentition.
Thorough periodontal debridement, through hand and ultrasonic instrumentation, is essential for first molar teeth due to the stability and function they provide for a patient’s dentition. Often periodontitis is found in first molar teeth due to length of time since eruption, complex anatomy, and location in the oral cavity. Patient self-care and professional debridement are challenging for these reasons.
The root anatomy of first molar teeth was reviewed in the article, “Hand Instrumentation of First Molar Teeth,” published in the May issue of Dimensions of Dental Hygiene.1 Reflecting on the developmental concavities and potential furcation involvement is important for providing initial nonsurgical periodontal therapy. This therapy requires a robust armamentarium of ultrasonic inserts/tips, including varying shank diameters, lengths, and shapes.
ULTRASONIC INSERT/TIP SELECTION
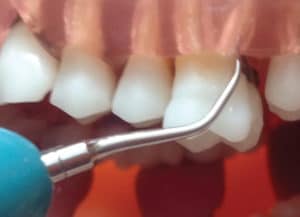
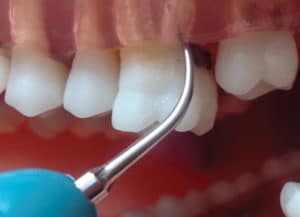
The size and tenaciousness of calculus deposits are key to selecting the appropriate ultrasonic insert/tip diameter. The location of the deposits within the probing depth and on the root’s anatomy is related to the length of the ultrasonic insert/tip. Moderate and large calculus deposits on first molars require a traditional ultrasonic insert/tip with a wide diameter such as a beavertail (#3), triple bend (#1000), or universal design (#10). Some clinicians use all three for general debridement for the first stage of initial nonsurgical periodontal therapy. Should the larger deposit be shallow (eg, 4 mm) within the periodontal pocket, a short length ultrasonic insert/tip can be chosen (Figure 1). If the heavy calculus is located 6 mm subgingivally, a wide diameter tip with a longer working end is needed (Figure 2).
It is tempting to apply a very thin ultrasonic insert/tip in deep pockets (5 mm or greater) to extend to the deposit to support patient comfort and to eliminate the need to change instruments during therapy. However, choosing a long thin insert (eg, #100 for magnetostrictive units and longer periodontal pocket microultrasonics) for this type of deposit will not be efficacious. The longest and thinnest ultrasonic inserts/tips are intended for use with low power and this, coupled with the thin diameter, can cause burnishing, interfering with the resolution of inflammation.
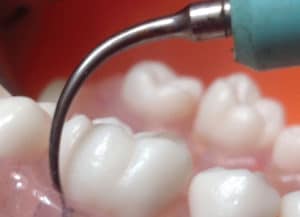
The large, tenacious deposits evident with initial therapy require an appropriate traditional insert, activated from the gingival margin toward the epithelial attachment because the working end can not always be adapted underneath the deposit when the periodontal pocket is full of calculus. In this situation, the point or point end of the tip is placed on the deposit to fracture it from the marginal to the apical portion. This situation is the only time it is recommended to use the point of the tip because the tip and its resultant energy are being placed on heavy calculus and not root surface structure. The point emits the greatest amount of energy, thus, it is not recommended for periodontal debridement on subgingival root surfaces because unwarranted damage can ensue.2,3 In the next stage, the active tip area is placed at the epithelial attachment to progress upward and remove deposit in an apical to marginal direction (Figure 3).
In the finishing stage of initial therapy, the suspected root anatomy will be encountered. Use of finer, longer, and tapered ultrasonic inserts/tips debride plaque biofilm and calculus. Examples include any periodontal debridement series intended for deep pockets and low to medium power settings. Curved and straight ultrasonic inserts/tips are needed because of the curvature of the tooth and the anatomical concavities in the root. It is not possible to adapt to all surface areas with one straight tip or even one curved tip. A study comparing a P10 to thin right and left inserts found both were able to debride the apical plaque biofilm border regardless of pocket depth, and there was no statistically significant difference in efficacy of debridement when both were compared. It was surmised, however, that shallow pockets were more effectively debrided with P10 inserts while deeper pockets were more effectively debrided with thin inserts.4 Although research has shown that dental hygienists know the importance of using multiple ultrasonic inserts/tips with patients with periodontitis (88%, N=44), a large percentage limited the number of tips used (37% used one tip: 42% used two tips).5
SURFACES OF FIRST MOLARS
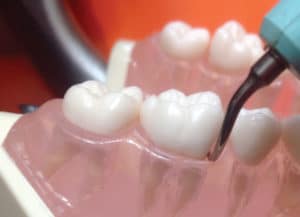
Finer deposits on the rounded buccal and lingual surfaces of molars are instrumented with curved ultrasonic inserts/tips. The easiest strategy is to adapt the curved tip just as a universal curet would be adapted. In other words, on the mandibular right buccal surface of the first molar, use the curved tip that points toward the mesial surface. This strategy allows negotiation of the concavity on the mesial surfaces of both the first molars with only slight rolling of the wrist (Figure 4). Some clinicians can adapt the curved designs exactly opposite of this concept. This latter method requires more wrist rolling and flexing than the first method and questions remain about appropriately adapting the tip into the proximal concavities. Microultrasonics may have difficulty accessing the area below the cementoenamel junction when the convex surface is adapted and this problem might be overcome by orienting the tip like hand curets.4
Any time a narrow periodontal pocket is encountered on the buccal or lingual surfaces, a straight ultrasonic insert/tip design is indicated with a vertical orientation (Figure 5). A thin straight tip will reach the depth of a narrow, deep periodontal pocket better than a curved design. Its limitation, however, is not adapting to the curvature of the remainder of the root at these depths. Therefore, the straight insert must be followed with a thin curved one to properly adapt to the root surfaces.
Ultrasonic inserts/tips with a small 0.8 mm ball end are designed for developmental concavities and furcation involvement. Use of these tips with an endoscope enables the clinician to assess effectiveness. They are not appropriate for use in the initial stages of periodontal debridement with heavier calculus deposits and they are recommended for use at low to medium power settings.
CONCLUSION
This article concentrated on ultrasonic insert/tip selection for first molar teeth during initial nonsurgical periodontal therapy. Effective ultrasonic instrumentation for these teeth depends on knowledge about anatomy, insert/tip designs, and technique. No longer is it acceptable to provide nonsurgical periodontal therapy with one or a few ultrasonic inserts/tips because so many options exist to match varying anatomical and patient conditions. Throughout initial therapy, ultrasonic instrumentation should be intertwined with hand instrumentation with explorers, files, and curets to improve effectiveness. The practitioner is responsible for providing efficacious care for prevention and maintenance of periodontitis, and molar teeth often provide the greatest challenge in doing so. A follow up article will focus on technique tips and ultrasonic therapy for furcation involvement on first molar teeth.
REFERENCES
- Hodges KO. Instrumenting first molars. Dimensions of Dental Hygiene. 2017;15:14–16.
- Flemmig TF, Petersilka GJ, Mehl A, Hickel R, Klaiber B. The effect of working parameters on root substance removal using a piezoelectric ultrasonic scaler in vitro. J Clin Periodontol. 1998;25:158–163.
- Flemmig TF, Petersilka GJ, Mehl A, Hickel R, Klaiber B. Working parameters of a magnetostrictive ultrasonic scaler influencing root substance removal in vitro. J Periodontol. 1998;69:547–553.
- Clifford LR, Needleman IG, Chan YK. Comparison of periodontal pocket penetration by conventional and microultrasonic inserts. J Clin Periodontol 1999;26:124–130.
- Alexander S, McConaughy F. Mentoring undergraduate dental hygiene students in research: Ultrasonic tip selection practices of dental hygienists. Abstract. J Dent Hyg. 2018;92(Suppl 1):38.
From Dimensions of Dental Hygiene. July 2018;16(7):46,48.

