Are Handheld Dental X-Ray Devices Convenient or a Hidden Safety Risk?
As these handy devices become more common in dentistry, updated safety protocols and proper technique are critical to minimizing radiation exposure and protecting both clinicians and patients.
First introduced in the 1990s, handheld portable X-ray devices are used in a variety of settings, from schools to mobile clinics. While not intended to replace the traditional wall units seen in most dental offices, handheld devices are becoming ubiquitous in dentistry.1,2 Traditional wall-mounted units are installed with structural shielding and protective barriers to protect operators from ionizing radiation in a controlled setting. In contrast, handheld units are typically used in noncontrolled environments, where the standard protective barriers associated with wall-mounted units are not present. Handheld devices are not designed to replace the traditional wall-unit but rather serve as a supplement.3,4
Handheld X-ray devices are frequently found in military settings, nursing homes, facilities for individuals with special needs, remote or underdeveloped regions lacking dental clinics, community outreach clinics, patients receiving treatment under general anesthesia, and in forensic dentistry.1,3
Radiation Safety for Dental Hygienists
Oral health professionals must always adhere to the “as low as reasonably achievable” (ALARA) principle when using ionizing radiation. Any exposure to radiation can increase the risk of adverse health effects; however, the exposure encountered in the dental setting is low.5
The National Council on Radiation Protection and Measurements (NCRP), a United States-based scientific advisory organization, provides guidance for dental radiographic procedures in NCRP Report No. 177: Radiation Protection in Dentistry and Oral and Maxillofacial Imaging.5 The maximum permissible dose (MPD) for occupational exposure is set at 50 mSv per year; however, oral health professionals receive an average annual dose of just 0.06 mSv, approximately 6% of this limit.5
Studies evaluating handheld X-ray devices report even lower operator exposure levels, averaging 0.0453 mSv, or about 0.9% of the annual limit.⁶ These values can vary depending on factors such as device type, operator hand positioning, and handling technique.6
The NCRP has made the following recommendations for oral health professionals who use handheld devices.2,3,6
- All handheld devices must be approved by the US Food and Drug Administration (FDA).2,3,6
- Approved units must be equipped with a backscatter shield that is at least 0.25 mm lead/lead equivalent, clear, and not removable from the device.3 The backscatter shield protects oral health professionals by blocking radiation scattered from the patient and surrounding objects. Research shows that with the backscatter shield in place, operator exposures are well within the maximum permissible dose for occupationally exposed individuals.3
- Rectangular collimation should be used whenever possible. Rectangular collimation reduces the patient-absorbed dose by 50% and also decreases scatter radiation.1,2
- Operators of handheld devices must be able to hold the device in place for multiple exposures.
- Handheld radiographic equipment must be securely stored.
- When handheld devices are used, all individuals at risk of exposure need to be protected.
- The operator of an FDA-cleared device is not required to wear a personal radiation protective garment.
Although exposure rates are low, many oral health professionals would prefer to see additional safety protocols implemented. Current studies recommend that operators use lead aprons with thyroid collars, dosimeters, and lead gloves as added protection.4,6,7 The potential areas of risk to exposure are the eyes, hands, thyroid, and gonads; due to the close proximity to the source of ionizing radiation.6,7 Future research is needed focusing on the cumulative exposures and to strengthen safety protocols.
Clinical Protocols for Safe Use
To ensure operator safety, correct positioning must be implemented during use. Several manufacturers recommend that the operator’s arms be fully extended and the device held parallel to the patient and perpendicular to the floor.4
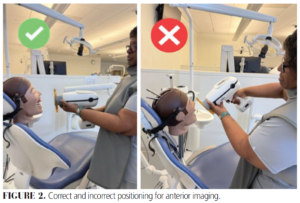
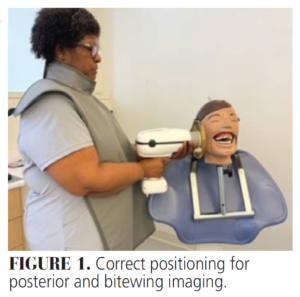 Proper positioning will provide a maximum safety zone of protection for the operator. Figure 1 shows the correct positioning when exposing a posterior and bitewing dental image. Figure 2 shows both correct and incorrect positioning of the device.
Proper positioning will provide a maximum safety zone of protection for the operator. Figure 1 shows the correct positioning when exposing a posterior and bitewing dental image. Figure 2 shows both correct and incorrect positioning of the device.
The handheld device should have the backscatter shield at the outer edge of the positioning indicator device (PID) close to the subject. For additional safety, dental staff and patients should stand at least 6 feet away from the primary beam when barrier protection is not available.5
Handling the machine with both hands helps with maintaining correct positioning. Due to the weight of the machine, operator arm fatigue over multiple exposures can compromise the ability to keep the device parallel.2 In Figure 3, the device is supported with two hands. One hand is held underneath the PID stabilizing the device, while the other is on the exposure button.
 The use of beam alignment devices helps clinicians adhere to the ALARA principle by minimizing technique errors and reducing dose exposure. The beam alignment device used for handheld units is different than the one used with the traditional wall-mounted unit. The indicator extension rod used for the handheld device is shorter. The shorter rod helps keep the backscatter shield as close as possible to the patient. Figure 4 shows a comparison of the regular beam alignment indicator extension rod compared to the beam alignment indicator extension rod used for the handheld device.
The use of beam alignment devices helps clinicians adhere to the ALARA principle by minimizing technique errors and reducing dose exposure. The beam alignment device used for handheld units is different than the one used with the traditional wall-mounted unit. The indicator extension rod used for the handheld device is shorter. The shorter rod helps keep the backscatter shield as close as possible to the patient. Figure 4 shows a comparison of the regular beam alignment indicator extension rod compared to the beam alignment indicator extension rod used for the handheld device.
Although the NCRP no longer recommends the use of lead aprons, manufacturers continue to suggest they may be helpful. In some cases, patient positioning may limit proper operator placement, and altering device positioning can compromise the protective zone. The lead apron is an added safety measure for operator protection.
Operators who face exposure beyond the annual limit of 1 mSv, should consider using a dosimeter, a personal safety device used to measure an individual’s cumulative exposure to ionizing radiation (X-rays, gamma rays, beta particles) over time.5 Pregnant operators should adhere to shielding procedures as stated in the facility’s radiation protection protocol in addition to using a dosimeter.5
Proper Handling , Storage, and Infection Control
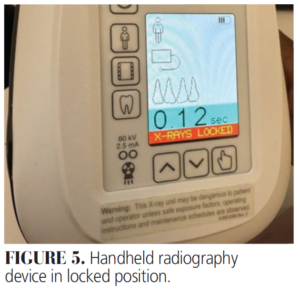
Due to the design and weight of the handheld device, operators should be careful about how they are handled. The devices can be placed in a cart or laid flat on the counter to prevent damage. The device should remain in the locked position until ready for use to prevent accidental discharge of radiation (Figure 5). Units should be stored securely and kept out of each to prevent unauthorized use.5
 Handheld X-ray devices are disinfected with a nonacetone disinfectant. Only the exterior surfaces and unplugged charger should be wiped down; the device surfaces should never be sprayed. The unit can also be covered with a plastic barrier for added infection control protection.
Handheld X-ray devices are disinfected with a nonacetone disinfectant. Only the exterior surfaces and unplugged charger should be wiped down; the device surfaces should never be sprayed. The unit can also be covered with a plastic barrier for added infection control protection.
Quality Assurance
All dental offices need to have a protocol for the use of handheld X-ray devices. Only trained personnel should be using the device. The NCRP states that special training for the operation of the handheld devices is needed for all clinicians and that the manufacturers are responsible for the training.3 Certification may be required before operating a handheld device.
In addition to NCRP recommendations, oral health professionals should know their state regulations and requirements. Information on state radiology regulations is available at the American Society of Radiologic Technologists’ website: asrt.org.8
Conclusion
Handheld dental radiation devices offer valuable flexibility in modern dental care, particularly in places where the traditional unit is not possible. As the dental hygiene profession continues to expand to meet the needs of individuals outside of the traditional dental office, dental hygienists must have a working knowledge of how to properly use the equipment safely and limit risks to themselves and their patients.
References
- Almeida FT, Majeed M, Fossen A, Pacheco-Pereira C. Exploring hand-held dental X-ray devices and their impact on digital dentistry: rationale and best practices. Can J Dent Hyg. 2026;60:64-68.
- Lurie AG, Kantor ML. Contemporary radiation protection in dentistry: Recommendations of National Council on Radiation Protection and Measurements Report No. 177. J Am Dent Assoc. 2020;151:716-719.
- Geist JR. Handheld intraoral dental x-ray devices should supplement but not replace conventional radiographic equipment. Oral Surg Oral Med Oral Pathol Oral Radiol. 2021;132:257-259.
- Martins GC, Rocha TG, de Lima Azeredo T, de Castro Domingos A, Visconti MA, Villoria EM. Hand-held dental X-ray device: Attention to correct use. Imaging Sci Dent. 2023;53:265-266.
- Benavides E, Krecioch JR, Connolly RT, et al. Optimizing radiation safety in dentistry: Clinical recommendations and regulatory considerations. J Am Dent Assoc. 2024;155:280-293.
- Altındağ A, Eren H, Orhan K, Görgün S. Evaluation of operator and patient doses after irradiation with handheld x-ray devices. Appl Sci. 2023;13:10414.
- Abubakr RI, Hajee SI. Occupational radiation exposure from handheld dental x‐ray devices: A quantitative dosimetric study. J Appl Clin Med Phys. 2025;26:e70375.
- American Society of Radiologic Technologists. ASRT States that Regulate. Available at asrt.org/main/standards-and-regulations/legislation-regulations-and-advocacy/states-that-regulate. Accessed April 21, 2026.
From Dimensions of Dental Hygiene. May/June 2026; 24(3):10-13