Survey Recognize and Report
How to detect infectious outbreaks¯caused by terrorism or natural disease eruption and what to do if an outbreak occurs.
The opinions expressed in this paper are those of the authors and do not necessarily reflect those of the Department of Defense, United States Air Force, United States Navy, or the Defense Medical Standardization Board.
Click here for a list of contacts to report a suspected infection with a category agent.
With the advent of human-to-human transmission of the bird flu,1 health care professionals have a responsibility to ensure adequate disease surveillance to prevent another worldwide flu pandemic of epic proportions. In addition to naturally occurring diseases, we now live in a world where diseases may be deliberately spread by terrorists or cult members. Examples include the unsuccessful use of small homemade bombs to spread anthrax spores by Aum Shinrikyo cult members in Japan and the delivery of letters containing weaponized anthrax via the US Postal Service to members of congress and the media in the days immediately following the terrorist attacks on the New York World Trade Center and the Pentagon.2-4
SYNDROMIC SURVEILLANCE IN THE DENTAL SETTING
As members of the health care profession, dental hygienists have a shared responsibility to understand the threats posed by infectious diseases and to serve as a reliable source of accurate information for our patients and colleagues. Hygienists may also serve as lookouts to help public health authorities identify an outbreak of infectious approaches to outbreak detection as involving three major processes: 1) timely review and investigation of case reports; 2) use of analytic tools to recognize patterns of disease transmission early in the course of the outbreak; and 3) evaluation of indirect data including health care product purchases, signs, and symptoms seen by health care workers and absences from work or school.5,6
The use of nondiagnostic data to catch an outbreak in its earliest stages is known as syndromic surveillance. Syndromic surveillance is a process where health departments continuously monitor disease indicators to detect outbreaks earlier and more completely than is possible with conventional methods. This method uses indicator data types. These data sets are not diagnostic of a specific disease such as influenza or smallpox, but rather reflect changes in normal patterns of behavior or the unexpected appearance of unusual signs and symptoms in health care settings.6
Dental health care professionals can participate in several ways within this surveillance paradigm. Changes in dental appointment patterns may provide an early warning sign of the spread of an infectious disease. In many communities unexpected increase in the numbers of cancellations for dental appointments, especially if related to illness, may likewise signal the early onset of an outbreak of infectious disease. For dental offices to effectively participate, however, they need to become formally involved with local health departments as stakeholders.

RECOGNIZING AN OUTBREAK
In our uncertain world, it is important to understand what diseases pose major threats from terrorists and why. The why is relatively straightforward, diseases that can infect large segments of the population, simultaneously causing devastating economic and social impact, are keys to a successful bioterrorism attack. The most dangerous of these agents are deemed Category A biological agents by the CDC. These agents are easily disseminated or transmitted from person-to-person with a high death rate. Other characteristics that make a particular organism a good candidate for use in bioterrorism or biowarfare are weaponizability (can the agent be modified to make it more easily transmitted or more pathogenic?) and stability (can the agent resist heat/cold, chemicals, antibiotics, or extended storage?). With these criteria in mind, the CDC has defined the following as Category Agents: smallpox, anthrax, botulinum toxin, tularemia, and viral hemorrhagic fevers. Agents that present with signs or symptoms that may be first recognized by dental health care professionals include all of the diseases listed above with the exception of botulinum toxin.7
SMALLPOX
The variola virus causes smallpox. The last naturally occurring case of smallpox was reported in Somalia in 19777 so any occurrence should create high suspicion for an act of bioterrorism. A single case is a medical emergency.
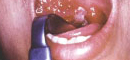
Smallpox is highly infectious with humanto-human transmission occurring easily. Humans are the only known reservoir of the virus. Transmission is via the respiratory route or contact with the pox lesion or infective material. The incubation period is 7-17 days until a rash or lesions appear. People are capable of spreading the disease once the pox lesions or rash appear. The pustules will scab over and begin to fall off after the second week. The patient is considered noncontagious only after all of the scabs have fallen off—usually after about 3 weeks. Oral lesions may be the initial manifestation of disease.7,8 Clusters of families presenting with oral lesions to the dental office should have smallpox included in the differential diagnosis (Figure 1).
The patient with smallpox will have a prodromal fever that may improve and then return after 2 days. Ulcers that appear on the buccal mucosa are painful. Lesions are symmetrical and, unlike other childhood pox viruses, have a distribution over the entire body, including the palms of hands and soles of feet. Treatment of smallpox is supportive with a case fatality rate of up to 30%. Vaccination may be effective if given within 7 days of exposure.10
ANTHRAX
Bacillus anthracis bacterium causes anthrax. The most common presentations of anthrax involve the skin (cutaneous anthrax), the respiratory system (inhalational anthrax), and the gastrointestinal system (gastrointestinal anthrax). Amore unusual variant of gastrointestinal anthrax that may be seen by dental health care professionals is oropharyngeal anthrax.
Human-to-human transmission is rarely seen. Anthrax is an excellent choice for biowarfare or terrorism because the bacillus forms very small spores that can be weaponized to improve dispersal. The spores are extremely hardy and may remain viable for decades in soil or as a component of a weapon. Most naturally occurring cases of anthrax are cutaneous and usually seen in people who work with livestock or handle wool or animal hide. The characteristic coal colored lesion gives both the bacteria and the disease its name. Cutaneous anthrax can be treated with antibiotics and is rarely fatal. If left untreated, about 20% of people with cutaneous infection will die.11
In contrast, untreated inhalational anthrax is almost invariably fatal. Early recognition is critical for survival.11 Of 11 cases of inhalational anthrax involved in the 2001 postal service attacks, five individuals died who were not identified early enough in the course of their disease to receive effective treatment.2,11,12 Natural cases of pulmonary anthrax are very rare in the United States with fewer than 20 cases reported between 1900 and 1976.11 The appearance of clusters of anthrax cases in nonagriculture related settings, as seen in the 2001 anthrax attacks, is an almost certain indication of a terrorist act.
Gastrointestinal and oropharyngeal anthrax result from ingestion of contaminated meat from infected animals. While all known uses of anthrax as a weapon have involved airborne transmission, contamination of food supplies is possible. In such a situation, dental offices might see an increase in dental visits for oral lesions, as the epidemiology is similar to the explosive outbreaks seen with food poisoning. The incubation period for oropharyngeal anthrax is very short, on the order of hours after exposure. In cases reported from Thailand, infections progressed to death within 33 hours.13
The dental hygienist may be the first to observe the clinical signs of oropharyngeal anthrax. The presentation includes severe sore throat or a local oral or tonsillar ulcer, usually associated with fever, toxicity, and swelling of the neck due to cervical or submandibular lymphadenitis or edema. Dysphagia and respiratory distress also may be present.13 See Figures 2 and 3.4
TULAREMIA
Francisella tularensis bacteria cause tularemia—also known as rabbit fever. Since tularemia generally occurs in rural areas and is associated with exposure to infected animals, an urban outbreak of tularemia would suggest a terrorist attack. The incubation period generally correlates with the virulence of the infecting strain. For biowarfare purposes, a highly virulent strain with a relatively short incubation period is most likely. Illness onsets generally occur 3 to 5 days after the initial release but can happen as soon as 1 day and up to 14 days later. Bioterrorism should be suspected if patients do not have risk factors for tularemia exposure, which include outdoor fieldwork or recent recreational activity, agricultural exposures, or exposure to infected arthropods or animals. The most likely form of intentional release for F tularensis would be via infectious aerosols.10,14
Oropharyngeal or gastrointestinal tularemia follows ingestion of the bacteria. Naturally occurring disease is a result of consuming undercooked meat from infected animals or direct inoculation from hand to mouth. Ingestion of the bacteria may occur secondary to inhalation of aerosolized bacteria. Pharyngitis occurs in up to 25% of tularemia patients. The pharynx may be erythematous or may present with petechiae, ecchymoses, ulcers, and/or exudates.14 Treatment consists of antibiotics with the drug of choice being streptomycin given intramuscularly. Gentamicin has also been used, given either intravenously or intramuscularly.10,14
VIRAL HEMORRHAGIC FEVERS
Viral hemorrhagic fevers are a diverse group of viruses from four different families. They include arenaviridae (Argentine, Bolivian, and Venezuelan hemorrhagic fevers and Lassa Fever); bunyaviridae (Congo-Crimea hemorrhagic fever, Rift Valley Fever); filoviridae (Ebola and Marburg viruses); and flaviviridae (dengue and yellow fever).15
Each of these virus families is distinctive epidemiologically. The arenaviridae and bunyaviridae are transmitted when humans come in contact with excretions from infected rodents.15 The filoviruses are transmitted human-to-human via contact with infected body fluids—often during health care procedures.5,6 Flaviviruses cause mosquito borne diseases including dengue and yellow fever. With the exception of dengue, the most likely mode of delivery in a terrorist attack would be via dispersed aerosols.10
The common symptoms of these viral illnesses are fever, myalgia, and prostration. Petechial hemorrhages are present and abnormal liver function tests are typical.10 For the dental community, fever and myalgia associated with gingival bleeding should alert the clinician to the possibility of viral hemorrhagic fever (Figure 4, page 11).9
With viral hemorrhagic fevers, control of bleeding is a priority and most patients will require treatment in an intensive care unit.10 The antiviral agent—ribavirin—may reduce morbidity and mortality and is most effective if begun early in the course of treatment.16
REPORTING
Early identification of an outbreak, whether from birds or bombs, is critical. Changes in dental appointment patterns may serve as an early warning sign of an impending epidemic or bio-terrorist event that may be incorporated into syndromic surveillance programs at the community level. Atypical oral diseases and disease patterns may be the earliest indicator of what type of an event may be occurring. The more informed dentists and dental hygienists become, the earlier detection will happen and containment with minimal damage can be assured.
The CDC and US Army Medical Research Institute for Infectious Disease response line personnel provide detailed instructions regarding necessary precautions and definitive treatment. The Federal Bureau of Investigation provides public health authorities instructions for collecting specimens and ensuring a proper chain of custody. Visit the web version of this article at www.dimensionsofdentalhygiene.com for a list of contacts for reporting a possible bioterrorism-related illness.
GET INVOLVED
Dental health care professionals who wish to become more involved in bioterrorism and pandemic disease preparedness should consider participating in community preparedness efforts. With proper training, dentists and dental hygienists can help extend care to affected populations if a disease outbreak should occur. Sponsored by the Office of the US Surgeon General, the Medical Reserve Corps (MRC) offers opportunities for volunteers from the health care professions to assist their communities during emergencies, such as an influenza epidemic, a chemical spill, or an act of terrorism. MRC units are community-based and function as a specialized component of Citizen Corps, a national network of volunteers dedicated to protecting communities from terrorism, crime, and disasters of all kinds. For more information about the MRC, visit www.medicalreservecorps.gov.
REFERENCES
- Brown H. WHO confirms human-to-human avian flu transmission. Lancet.2004;363:462.
- Estimating the impact of the next influenza pandemic: enhancing preparedness Geneva, 8 December 2004. 2005, World Health Organization. Available at: www.who.int/csr/disease/influenza/preparedness2004_12_08/en/print.html. Accessed March 6, 2005.
- Dewan PK, Fry AM, Laserson K, et al. Inhalational anthrax outbreak among postal workers, Washington, DC, 2001. Emerg Infect Dis. 2002;8:1066-1072.
- Keim P, Smith KL, Keys C, Takahashi H, Kurata T, Kaufmann A. Molecular investigation of the Aum Shinrikyo anthrax release in Kameido, Japan. J Clin Microbiol. 2001;39:4566-4567.
- Traeger MS, Wiersma ST, Rosentein NE, et al. First case of bioterrorism-related inhalational anthrax in the United States, Palm Beach County, Florida, 2001. Emerg Infect Dis. 2002;8:1029-1034.
- Buehler JW, Berkelman RL, Hartley DM, Peters CJ. Syndromic surveillance and bioterrorism-related epidemics. Emerg Infect Dis. 2003;9:1197-1204.
- Buehler JW, Hopkins RS, Overhage JM, Sosin DM, Tong V, CDC Working Group. Framework for evaluating public health surveillance systems for early detection of outbreaks: recommendations from the CDC Working Group. MMWR Recomm Rep. 2004;53(RR-5):1-11.
- Centers for Disease Control and Prevention. Emergency preparedness and response—biological agents/diseases 2004. Available at: www.bt.cdc.gov/agent/agentlist-category.asp#adef . Accessed March 6, 2005.
- Baron S. Smallpox: the main site of transmission is the oropharynx. J Dent Res. 2003;82:252.
- Centers for Disease Control and Prevention, Public Health Image Library, PHIL # 4360 (1969). Available at: http://phil.cdc.gov/phil/detail.asp?id=4360 . Accessed on March 6, 2005.
- Darling RG, Woods JB, eds. USAMRIID’s Medical Management of Biological Casualties Handbook. Fort Detrick, Md: US Army Medical Research Institute for Infectious Disease; 2004.
- Sternbach G. The history of anthrax. J Emerg Med. 2003;24:463-467.
- Spencer RC. Bacillus anthracis. J Clin Pathol.2003;56:182-187.
- Sirisanthana T, Brown AE. Anthrax of the gastrointestinal tract. Emerg Infect Dis. 2002;8:649-651.
- Dennis DT, Inglesby TV, Henderson DA, et al. Tularemia as a biological weapon: medical and public health management. J A M A. 2001;285:2763-2773.
- CDC Special Pathogens Branch, Disease Information. 2005, Centers for Disease Control and Prevention. Available at: www.cdc.gov/ncidod/dvrd/spb/mnpages/disinfo.htm . Accessed March 6, 2005.
- CDC Special Pathogens Branch, Lassa Fever. 2004, Centers for Disease Control and Prevention. Available at: www.cdc.gov/ncidod/dvrd/spb/mnpages/dispages/lassaf.htm . Accessed March 6, 2005.
From Dimensions of Dental Hygiene. May 2005;3(5):10-12.

