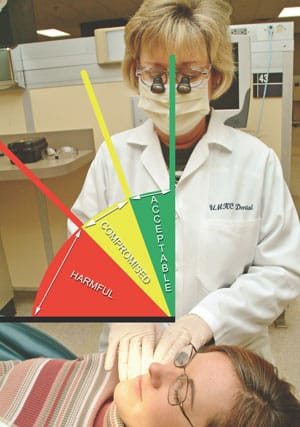
Posture Perfect
Noting harmful chair side postures through assessment and observation and making necessary adjustments can make the difference in maintaining a healthy career in dental hygiene.
The high rate of musculoskeletal disorders (MSDs) reported by dental hygienists is no secret.1-3 In 2001, 65% of registered dental hygienists reported having carpel tunnel syndrome (CTS) that required days away from work and 79% of dental hygienists reported days away from work due to repetitive motion exposure.4 The rate of MSDs among dental hygiene practitioners is higher than that of the general population.4 Despite these alarming numbers, dental hygiene educational programs continue to better prepare dental hygienists for needle stick prevention than for maintaining their musculoskeletal health.5
Work-related musculoskeletal disorders (WMSDs) result in a loss of income, increased medical expenses, rising workers’ compensation claims, and often require days off work, permanently decreasing the number of days worked or ultimately resulting in a career change. Proper education in ergonomics for the workplace can alleviate some of these problems.
THE DEVELOPMENT OF CTS
The objective of ergonomics is to fit the physical workplace to the worker. This concept sounds quite simple, yet proves to be extremely complex. Experimental and epidemiological research acknowledges the origin of a WMSD as multifactorial.6 A conceptual framework (Figure 2) for developing a WMSD has been developed by the National Research Council. In this model, the work environment, organizational factors, and social context are influenced by physical and psychological factors and nonwork-related activities.
The development of CTS results from compression of the median nerve. The median nerve begins in the brachial plexus of the spine where the neck meets the shoulder. It runs the length of the arm next to the brachial artery through the carpal tunnel canal of the wrist and into the hand to supply feeling to the thumb, index finger, middle finger, and half of the ring finger.7 Dental hygienists need to be conscious of the signs and symptoms of CTS.
Recent studies that analyzed the relationship between clinical CTS symptoms and nerve conduction tests concluded that the major symptom of CTS is pain at night,8 along with numbness and tingling. Minor symptoms of CTS are pain, weakness, and clumsiness.9,10 The origin of hand pain may not be in the hand and could possibly relate to other aspects of operator posture.
Dental hygienists are subject to many risk factors that increase the chance of developing WMSDs. The most significant non modifiable risk factors include wrist-hand ratio and history of musculoskeletal disorder within the past 5 years.8 Others include female gender, age, the number of patients seen per day, body mass index, diabetes or other endocrine disorders, hypo or hyperthyroidism, pregnancy, obesity, and menopause.1,2,9,11 Modifiable risk factors,include activities, such as hobbies, that require repetitive use of the hands, the use of heavy pinch grip forces, non-neutral positions,awkward posture and positioning,localized pressure and use of repetitive motions, poorly fitted gloves, cold temperatures,vibrations, and work organization also significantly contribute to the development of CTS.2,9,12,13
SITTING POSTURE
Maintaining a neutral posture while sitting may aid dental hygienists in the prevention of WMSDs and hand problems.13,14 Dental hygienists often work in the same position for long periods of time, performing tasks repeatedly, and bending or twisting the back in awkward positions.1 Often there is a misconception that a simple change in instrument selection or wearing a splint at night will prevent CTS. These alterations are beneficial, however, due to the interdependent nature of the many factors necessary to develop CTS,focus should not be limited to hands and arms alone.6 Dental hygienists must also consider the important role that sitting posture plays in physical factors related to MSDs.
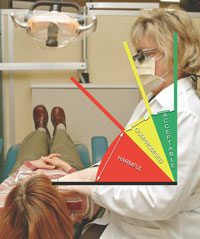
An on-the-job assessment of posture is critical to determining posture weaknesses. In order to accomplish this assessment, dental hygienists need to understand the parameters of correct posture. Educational programs typically instruct dental hygiene students on the ideal sitting posture.5 This instruction includes holding the head, trunk, arms, and hips in neutral positions, typically at an angle of slightly less than 90°.15 This is often not practical in the clinical setting and movement beyond the limits of neutral posture frequently occurs. However, the limits to which an operator can move beyond neutral are not well-established nor are they commonly recognized by clinicians.
ASSESSMENT
Practicing dental hygienists can use an assessment instrument to examine posture. This examination can be a self-assessment but is more ideally used by a trained observer examining the clinician in real time. The Branson’sPosture Assessment Index (BPAI)16 is a validated instrument that calls for an observer to examine various posture check points and determine how far the body part is angled off the 90° axis. The nature of dental treatment requires that the hygienist adopt postures in angulations away from neutral. WMSDs occur when the angulations are excessive or held for long periods of time. Evaluation of these limits is important in understanding the levels to which a clinician’s posture is harmful.
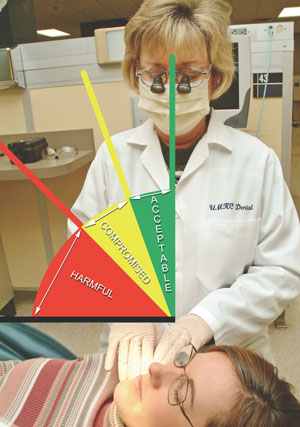
The BPAI (Figure 1) incorporates a grading scale for posture. The scale examines the clinician’s posture at three check points over a 5 minute time period and rates the overall posture as either acceptable, compromised,or harmful. The clinician’s hips, trunk, head/neck, shoulders, and wrists are evaluated. The final BPAI numerical score is a result of a mathematical calculation that multiplies values for each category at each time interval to determine a final sum. Posture scores that range from 10 to 40 are considered acceptable, scores ranging from 41 to 80 are compromised, and scores ranging from 81-194 are harmful. This instrument is designed to be administered by trained evaluators during real-time observation.
Click here for Figure 1 – Branson’s Posture Assessment Instrument (BPAI)
OBSERVATION
In the dental office, the assessment instrument is best used if several team members are familiar with the use of the evaluation system. Team members can take turns doing evaluations of each other. These evaluations should take place at different times throughout the work day. Other information needs to be collected by the observer to thoroughly examine posture (Figure 3). For example, if the most compromised/harmful postures occur while sitting at the 10:00 position while using thin handled scalers on the buccal surfaces of the upper left quadrant, then the operator needs to make modifications while treating this area.
While real time observation is the most ideal method of evaluation, video taping may be an alternative method for self-observation. Applying the same self-assessment strategies mentioned above can be used when reviewing video tapes. The evaluator examines the posture of the individual using BPAI and also applies assessment principles. Some information may be lost in the video-taping but the dental hygienist can still make generalizations as to the weak areas in positioning and posture.
INTERVENTION
Once posture weaknesses are identified, the hygienist needs to consider evidence-based interventions and ergonomic devices, such as loupes and ergonomically designed chairs and instruments, that will address the problem areas.
Magnification loupes are common devices used to prevent posture problems. The value of loupes is largely based on self-reports and focus groups; few studies exist to definitively outline the benefits. However, a recent study used video tape analysis to determine the effect magnification loupes had on operator posture of student dental hygienists. The study used trained observers and concluded that the posture of dental hygiene students was more acceptable when magnification loupes were worn than when traditional safety glasses were used.18
Musculoskeletal disorders are caused by many factors and are experienced by most dental hygienists at some point. Early ergonomics education and prevention are important in avoiding the negative impact of WMSDson a dental hygiene career. Dental hygienists need to be aware of compromised and harmful chair-side postures. Ergonomic devices such as magnification loupes have proven useful in keeping the head, neck, and trunk in less stressful postures. Dental hygienists should be on the alert for opportunities to self-assess and incorporate ergonomic strategies into the dental office environment.
REFERENCES
- Anton D, Rosecrance J, Merlino L, Cook T. Prevalence of musculoskeletal symptoms and carpal tunnel syndrome among dental hygienists. Am J Ind Med. 2002;42:248-257.
- Lalumandier JA, McPhee SD. Prevalence and risk factors of hand problems and carpal tunnel syndrome among dental hygienists. J Dent Hyg. 2001;75:130-134.
- Akesson I, Hansson GA, Balogh I, Moritz U, Skerfving S. Quantifying work load in neck, shoulders and wrists in female dentists. Int Arch Occup Environ Health.997;69:461-474.
- US Department of Labor. Special Report. Washington, DC: US Bureau of Labor Statistics; June 28, 2004.
- Beach JC, DeBiase CB. Assessment of ergonomic education in dental hygiene curricula.J Dent Ed. 1998;62:421-425.
- National Research Council. Work Related Musculoskeletal Disorders: A Review of the Evidence. Washington, DC: National Academy Press; 1998.
- Interactive Hand Therapy Edition [CD-ROM]. Version 1.1. London: Primal Pictures; 2001.
- You H, Simmons Z, Freivalds A, Kothari MJ, Naidu SH. Relationships between clinical symptom severity scales and nerve conduction measure in carpal tunnel syndrome. Muscle Nerve. 1999;22:497-501.
- You H, Simmons Z, Freivalds A, Kothari MJ, Naidu S, Young R. The development of risk assessment models for carpal tunnel syndrome: a case-referent study. Ergonomics. 2004;47:688-709.
- Bland JD. The value of the history in the diagnosis of carpal tunnel syndrome.J Hand Surg [BR]. 2000; 25:445-450.
- Michalak-Turcotte C. Controlling dental hygiene work-related musculoskeletal disorders: the ergonomic process. J Dent Hyg. 2000;74:41-48.
- Keyserling WM. Workplace risk factors and occupational musculoskeletal disorders,Part 2: A review of biomechanical and psychophysical research on risk factors associated with upper extremity disorders. AIHAJ. 2000;61:231-243.
- Sanders MA, Turcotte CM. Strategies to reduce work-related musculoskeletal disorders in dental hygienists: two case studies. J Hand Ther. 2002;15:363-374.
- Meador HL. The biocentric technique: a guide to avoiding occupational pain. J Dent Hyg. 1993;67:38-51.
- Nield JS. Fundamentals of Periodontal Instrumentation and Advanced Root Instrumentation. 5th ed. Philadelphia: Lippincott Williams & Wilkins; 2004:14-21.
- Branson BG, Williams KB, Bray KK, McIlnay SL, Dickey D. Validity and reliability of a dental operator posture assessment instrument (PAI). J Dent Hyg.2002;76:255-261.
- Spielholz P, Silverstein B, Morgan M, Checkoway H, Kaufman J. Comparison of self-report, video observation and direct measurement methods for upper extremity musculoskeletal disorder physical risk factors. Ergonomics. 2001;44:588-613.
- Branson BG, Bray KK, Gadbury-Amyot C, et al. Effect of magnification lenses on student operator posture. J Dental Educ. 2004;68:384-389.
From Dimensions of Dental Hygiene. May 2005;3(5):14, 16-19.

