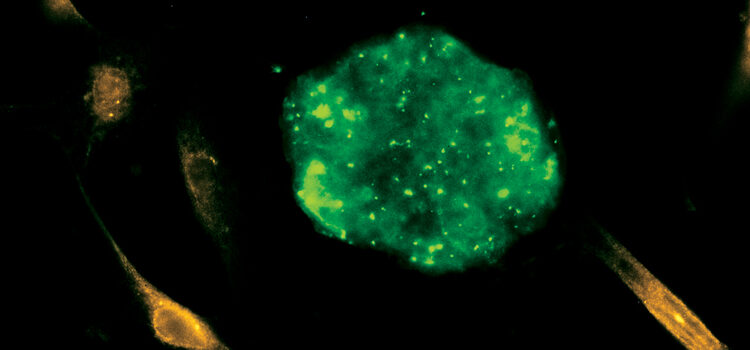
The Regenerative Process
Understanding stem cell research and its implications for the dental professional.
Part 2 of a two part series on stem cells. Part 1 appeared in the January 2009 issue and is available only by clicking here.
This course was published in the February 2009 issue and expires 2/28/12. The author has no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- Discuss the use of stem cells for tissue regeneration and repair.
- Identify oral soft tissue sources of adult stem cells.
- Describe the criteria used to select patients who are candidates for dental stem cell recovery.
- Identify various times during the course of an individual’s development when extracted teeth may be used to obtain dental stem cells for banking.
- Describe how the dental professional can educate patients about the benefits of recovering and storing dental stem cells for future use.
Adult stem cells have been identified in many types of adult tissues, including bone marrow, blood, skin, adipose, dental pulp, retina, skeletal muscle, and brain. Part 1 of this article, published in January 2009, explored these sources and types of human stem cells, including those found in dental pulp and other oral tissues. Dental stem cells are the most accessible adult stem cells and they can be isolated from a variety of oral tissues, including pulp, periodontal ligament, and bone.5,6 Very proliferative, multipotent, mesenchymal stem cells are found within dental pulp at the apex of developing teeth and in the follicular sac surrounding unerupted or impacted teeth.7,8
Mesenchymal stem cells found in the dental pulp of deciduous teeth, also known as SHED (stem cells from human exfoliated deciduous teeth), offer some distinct advantages over adult stem cells obtained from other tissues. SHED cells demonstrate greater plasticity and multiply more rapidly than stem cells taken from the pulp of fully developed permanent teeth.7 Stem cells in deciduous teeth begin to develop during the sixth week of embryonic life, very early in the differentiation process.
SHED cells go through fewer cell divisions than other types of adult stem cells, which may be the reason for their proliferate nature when grown in vitro. These unique characteristics and the immaturity of SHED cells, as compared to other adult stem cells found elsewhere in the body, suggest that stem cells from deciduous teeth show greater potential for differentiation into a wider array of tissue types.7 And, the opportunity to recover stem cells from deciduous teeth presents itself naturally during exfoliation, with little to no trauma to the child.
 Currently, there are no approved medical or dental therapies using dental stem cells, and the use of these future therapies is still years away from implementation into clinical practice. Indeed, dental professionals will play an important role in both the recovery and use of these stem cells for dental and medical regenerative therapies. However, in order to keep these stem cells as a form of bioinsurance for future use, dental professionals need to assist their patients with recovering and storing mesenchymal stem cells. Dental stem cells can be easily obtained during planned dental procedures from deciduous teeth, third molars, extracted permanent teeth with healthy pulp, and other accessible living tissues from the oral cavity. The opportunity to recover and bank dental stem cells is a service that can be offered now to pediatric, adolescent, and adult patients.
Currently, there are no approved medical or dental therapies using dental stem cells, and the use of these future therapies is still years away from implementation into clinical practice. Indeed, dental professionals will play an important role in both the recovery and use of these stem cells for dental and medical regenerative therapies. However, in order to keep these stem cells as a form of bioinsurance for future use, dental professionals need to assist their patients with recovering and storing mesenchymal stem cells. Dental stem cells can be easily obtained during planned dental procedures from deciduous teeth, third molars, extracted permanent teeth with healthy pulp, and other accessible living tissues from the oral cavity. The opportunity to recover and bank dental stem cells is a service that can be offered now to pediatric, adolescent, and adult patients.
Patient Selection Criteria
 Patients who are young and healthy are the best candidates for mesenchymal stem cell collection and storage, as they are more likely to be free from chronic diseases. The stem cells in young patients have undergone fewer cell divisions, and thus, there is less risk of somatic mutation.
Patients who are young and healthy are the best candidates for mesenchymal stem cell collection and storage, as they are more likely to be free from chronic diseases. The stem cells in young patients have undergone fewer cell divisions, and thus, there is less risk of somatic mutation.
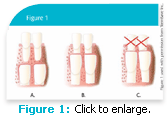
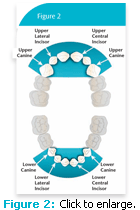
Exfoliating deciduous teeth are an excellent source of highly proliferative mesenchymal stem cells. In a child, dental stem cells become accessible naturally on several occasions, based on the resorption pattern of deciduous teeth. As stem cells are located diffusely throughout the pulpal chamber of the tooth, the ideal deciduous tooth for stem cell recovery still has a measurable amount of root structure that contains healthy pulp tissue (Figure 1). The best deciduous teeth from which to recover SHED cells are located in the area between the upper and lower canines and include moderately resorbed canines and incisors that still possess a healthy pulp (Figure 2).
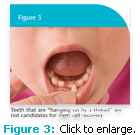 The pulp of the deciduous tooth receives nourishment from the collateral blood supply around the apex of the resorbing root. When the tooth becomes extremely mobile, the pulp becomes separated from its blood supply, which results in pulpal necrosis. The tooth may still maintain its gingival attachment and be retained for weeks in the mouth with a necrotic pulp. Teeth that are “hanging on by a thread” (Figure 3) or that naturally fall out on their own are not candidates for stem cell recovery. In order for stem cells to be recovered successfully from deciduous teeth, the dentist should remove the tooth when it is mobile but still attached with a good blood supply. Patients need to be educated about the benefits of banking these teeth as an alternative to simply discarding them or saving them as childhood mementos.
The pulp of the deciduous tooth receives nourishment from the collateral blood supply around the apex of the resorbing root. When the tooth becomes extremely mobile, the pulp becomes separated from its blood supply, which results in pulpal necrosis. The tooth may still maintain its gingival attachment and be retained for weeks in the mouth with a necrotic pulp. Teeth that are “hanging on by a thread” (Figure 3) or that naturally fall out on their own are not candidates for stem cell recovery. In order for stem cells to be recovered successfully from deciduous teeth, the dentist should remove the tooth when it is mobile but still attached with a good blood supply. Patients need to be educated about the benefits of banking these teeth as an alternative to simply discarding them or saving them as childhood mementos.
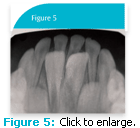
Anterior deciduous teeth are preferred over deciduous molar teeth when selecting teeth for stem cell recovery. Even though first and second deciduous molars possess a greater quantity of pulp as compared to anterior teeth, they are not typically candidates for stem cell recovery due to their irregular irregular patterns of resorption. It is difficult to predict the quantity of viable pulpal tissue at the time of natural exfoliation (Figure 4). However, deciduous molar teeth may be candidates when they are removed early for orthodontic treatment. In children, other sources of easily accessible stem cells include supranumerary teeth, mesodens, and overretained deciduous teeth (Figure 5).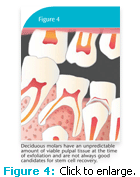
There are two excellent opportunities for adolescent patients to bank their dental stem cells: following extraction of bicuspid teeth for orthodontic treatment and partially developed third molars. Bicuspid teeth are not fully formed until between the ages of 12 and 14 years. The apex of the root is still developing and contains a concentrated area of stem cells that participate in the formation of the root and the supporting structures of the tooth, bone, and periodontal ligament. Typically, these teeth are extracted for orthodontic reasons before the roots are fully formed, which ensures a better chance for success of harvesting viable stem cells. The roots of the wisdom teeth are not fully formed until after the age of 18; extracting these teeth during the teenage years helps ensure the greatest abundance of proliferative stem cells.
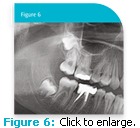
 The follicular sac of an unerupted tooth is also an excellent source of highly proliferative stem cells.7 The follicle is found around developing teeth and the coronal region of impacted teeth (Figure 6). This soft tissue lining is of ectomesenchymal origin, and is removed and discarded along with the impacted tooth.
The follicular sac of an unerupted tooth is also an excellent source of highly proliferative stem cells.7 The follicle is found around developing teeth and the coronal region of impacted teeth (Figure 6). This soft tissue lining is of ectomesenchymal origin, and is removed and discarded along with the impacted tooth.
Anatomically, the pulpal volume of the tooth is the greatest during the developmental stage. The size of the pulp chamber decreases in size as a person ages. All extracted teeth with healthy pulp should be considered candidates for stem cell collection. Common sources of dental stem cells in adult patients include any healthy teeth that require extraction, such as impacted third molars, orthodonticallyinvolved teeth, and supranumerary teeth. Teeth that have been traumatized or those that exhibit extensive caries, pulpal infection, and/or periodontal disease are not candidates.
Conclusions
Dental professionals can now assist their patients with recovering and banking their dental stem cells. Several companies offer collection and cryopreservation services for the dental professional community. Dental stem cells must be derived from living tissues, and these companies offer kits that are used to collect and transport harvested tissue samples from the dental office.
Companies that store stem cells procured in the dental office use similar protocols for the recovery and transport of tissue. During a regularly scheduled dental procedure, extracted teeth and tissue samples are placed into a special nutrient solution and thermal container to maintain their health during shipping to a regulated laboratory facility. Upon arrival at the facility, the stem cells are extracted and tested for viability. The cells are then cryopreserved at subzero temperatures to stop any cellular or biochemical activity, including cell growth as well as the mechanism that causes cell death.
Deciduous teeth that fall out on their own at home and are brought to the dental office are unlikely candidates for dental stem cell cryopreservation. This is especially important for parents of very small children to understand, who may not realize that they should bring their children in for evaluation when the deciduous teeth begin to develop mobility. Patients need to know about the availability of this service, so that collection can be planned later during a scheduled dental procedure. Research shows that stem cells from dental pulp of extracted third molars and from periodontal ligaments are viable following thawing after cryopreservation, and are able to differentiate into multiple cell types in vitro.9,10 This research suggests that dental stem cells can be safely stored for long periods of time via cryopreservation for later use.11 The time to offer patients this potentially life-saving service for future medical treatment is now.
References
- National Institutes of Health, United States Department of Health and Human Services. Clinical Trials. Available at: http://clinicaltrials.gov/ct/search?term=stem+cell&submit=Search. Accessed January 12, 2009.
- Barry FP, Murphy JM. Mesenchymal stem cells: clinical applications and biological characterization. Int J Biochem Cell Biol. 2004;36:568-584.
- National Institutes of Health, United States Department of Health and Human Services. Stem Cell Information. Available at: http://stemcells.nih.gov. Accessed January 12, 2009.
- Macchiarini P, Jungebluth P, Go T, et al. Clinical transplantation of a tissue-engineered airway. Lancet. 2008;13;372:2023-2030.
- Mao JJ, Giannobile WV, Helms JA, et al. Craniofacial tissue engineering by stem cells. J Dent Res. 2006;85:966-979.
- Gronthos S, Mankani M, Brahim J, Robey PG, Shi S. Postnatal human dental pulp stem cells (DPSCs) in vitro and in vivo. Proc Natl Acad Sci USA. 2000;97:13625-13630.
- Miura M, Gronthos S, Zhao M, et al. SHED: stem cells from human exfoliated deciduous teeth. Proc Natl Acad Sci USA. 2003;100:5807-5812.
- Gronthos S, Brahim J, Li W, et al. Stem cell properties of human dental pulp stem cells. J Dent Res. 2002;81:531-535.
- Zhang W, Walboomers XF, Shi S, Fan M, Jansen JA. Multilineage differentiation potential of stem cells derived from human dental pulp after cryopreservation. Tissue Eng. 2006;12:2813-2823.
- Seo BM, Miura M, Sonoyama W, Coppe C, Stanyon R, Shi S. Recovery of stem cells from cryopreserved periodontal ligament. J Dent Res. 2005;84:907-912.
- Papaccio G, Graziano A, d’Aquino R, et al. Long-term cryopreservation of dental pulp stem cells (SBPDPSCs) and their differentiated osteoblasts: a cell source for tissue repair. J Cell Physiol. 2006;208:319-325.
From Dimensions of Dental Hygiene. February 2009; 7(2):38-41.