
Reducing Kids’ Risk with Blood Pressure Monitoring
Frieda Atherton Pickett, RDH, MS, and David Charles Kaelber, MD, PhD, MPH, FAAP, discuss the need for monitoring pediatric blood pressure in the dental office.
The views expressed in this interview are the authors’.
Q. In 2004 the National High Blood Pressure Education Program Working Group on High Blood Pressure in Children and Adolescents updated its guidelines on the assessment of prehypertension and hypertension (HTN) in children in the “Fourth Report on the Diagnosis, Evaluation, and Treatment of High Blood Pressure in Children and Adolescents.” What were the major changes in the updated guidelines for blood pressure values in the pediatric population?
Pickett: The major changes in the 2004 report compared to the last update in 1996 included replacing the former designation of high normal blood pressure values with a new category of prehypertension and defined levels of HTN into stage 1 HTN and stage 2 HTN.1 The report recommends that blood pressure be monitored in pediatric patients older than age 3 and that blood pressure monitoring become part of the health care visit in all health facilities, rather than just within the medical office. The report features tables that identify elevated blood pressure values which require ascertaining a child’s height percentile from among seven different levels in order to identify elevated blood pressure values. There is a table for girls and a table for boys with blood pressure values identified as normal (50th percentile), prehypertensive (90th percentile), stage one HTN (95th percentile), or stage two HTN (99th percentile) according to the age of the child.1
Q. Is the height percentile requirement an obstacle to effectively using the tables, particularly in the dental setting?
Kaelber: Yes, determining a child’s height percentile requires the clinician to first know the child’s height, as well as age and gender, and then to use a graph or equation to determine the height percentile. Although this approach is the most accurate, in many settings determining the height and then the height percentile can be time consuming.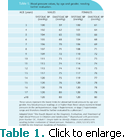
Pickett: In order to resolve this issue, Dr. Kaelber and I have created a simplified table (Table 1).2 When blood pressure values equal or are higher than the values listed in the simplified table for the child’s sex and age, the child should be referred for medical evaluation of blood pressure.
THE SIMPLIFIED TABLE
Q.What are the advantages of the simplified table, as well as its limitations?
Pickett: The simplified table is based only on gender and age, identifies only one threshold value of abnormal systolic and diastolic blood pressure, and has 100% sensitivity. However, it can produce false positive values in some children in higher height percentile (taller) categories. The table identifies the blood pressure values for boys and girls—based on the age—that should be referred for medical evaluation.
Kaelber: We do not see the potential false positive rate in children in higher height percentile categories as a significant issue since the precision of blood pressure measurements is relatively low and can vary up to 10 mmHg to 15 mmHg for systolic and 5 mmHg to 10 mmHg for diastolic blood pressures based on time of day of the blood pressure measurement, if automatic versus manual blood pressure measurement is used, office versus ambulatory readings, and the competence of who is doing the manual measurement. This variation in the precision of the blood pressure measurement is equal to or greater than the difference in cut-off blood pressure values for the 5% height percentile and the 95% height percentile, which vary between 6 mmHg to 9 mmHg for systolic blood pressures and 3 mmHg to 5 mmHg for diastolic blood pressures.
Q. How was the simplified table developed?
Pickett: A cohort study of electronic medical records in Ohio including 14,187 children, ages 3 years to 18 years, reported that blood pressure assessment within a medical facility did not identify 74% of hypertensive blood pressures or 89% of prehypertensive blood pressures.3 The publication of this study led me to contact one of the study authors, Dr. Kaelber, to express my opinion that the difficulty of using the seven height percentiles in the original report’s tables was the reason for this high level of misdiagnoses. I was reasonably sure dentistry would have problems finding the height percentile information and the study results indicated that even physicians found it difficult. Dr. Kaelber responded, agreeing with me that the tables in the report needed to be simplified for clinical use. Our development of the simple table followed.
As most dental hygienists know, hypertension is not diagnosed based on one blood pressure evaluation; at least two and often three measurements made at different appointments are needed to diagnose prehypertension or HTN. Dr. Kaelber rightly determined that it was not the role of oral health care professionals to diagnose HTN in children, but rather to comply with the report recommendations identifying the role of oral health care professionals in the screening process. The clinical application is that when blood pressure values equal or are higher than the values for the sex and age listed in the simple table we developed, the pediatric patient should be referred for medical evaluation of blood pressure. At this time our table has not been pilot tested to determine the degree of usefulness leading to a diagnosis of prehypertension or HTN. A study design for this purpose is currently in process with Caren Barnes, RDH, MS at the University of Nebraska Medical Center College of Dentistry in Omaha.
PREVALENCE OF HYPERTENSION AMONG CHILDREN
Q. How prevalent is pediatric hypertension in the United States and what is the clinical significance?
Pickett: Epidemiologic studies indicate that 2% to 4% of the pediatric population4 and between 15% and 30% of obese children have HTN,5-8 which can lead to chronic diseases including cardiovascular disease, type 2 diabetes mellitus, and fatty liver disease.1,9,10 The report describes evidence of early target-organ damage in children and adolescents, and further studies verify vascular damage.11,12 On the basis of developing evidence, primary HTN is detectable in the young, the risk for long-term chronic diseases is substantial, and measures must be taken now to reduce this risk.
In fact African-American children with primary hypertension (PHTN) are nearly twice as likely to have left ventricular hypertrophy (prevalence 42%) as children from other racial backgrounds with PHTN (prevalence 37%).12 This study concluded that African-American children with HTN, as a special group, may be at particularly high risk for cardiovascular disease as they age and health care professionals should follow them very closely. Left ventricular hypertrophy in adults is a marker of increased cardiovascular morbidity and mortality. If children with elevated BP levels are monitored closely signs of cardiovascular disease can be detected early and possibly treatment can reduce their development.
THE PARAMETERS OF DIAGNOSIS
Q. How many blood pressure measurements should be obtained to confidently classify a child as normotensive, prehypertensive, or hypertensive?
Kaelber: At least three blood pressures taken during different visits and at different times are needed in the prehypertensive or hypertensive range for the patient to carry one of these diagnoses. For example, let’s say the following readings were taken from a child who had six blood pressure readings without any interventions:
- Visit one—hypertensive blood pressure
- Visit two—normotensive blood pressure
- Visit three—hypertensive blood pressure
- Visit four—hypertensive blood pressure
- Visit five—normotensive blood pressure
- Visit six—normotensive blood pressure.
Does this child have hypertension? According to the strict definition, yes. In my opinion, I would not say this person had chronic hypertension at the sixth visit. Hopefully, future guidelines will help clarify this. The equivalent guidelines for adults, Joint National Commission Seventh Report of Hypertension in Adults, uses the criteria: “The average of two or more properly measured, seated, blood pressure readings on each of two or more office visits.”13
Q.What is the proper technique for taking blood pressure measurements from children?
Kaelber: Cuff size is very important for taking a blood pressure measurement from a child. The “Fourth Report” states: “By convention, an appropriate cuff size is a cuff with an inflatable bladder width that is at least 40% of the arm circumference at a point midway between the olecranon (the curved bony eminence of the forearm that presents behind the elbow) and the acromion (on the shoulder blade). For such a cuff to be optimal for an arm, the cuff bladder length should cover 80% to 100% of the circumference of the arm. Such a requirement demands that the bladder width-to-length ratio be at least 1:2.”14,15 The report also includes a table outlining typical sizes based on age range. The National Kidney Foundation also has a detailed description of this approach with figures on its website at www.kidney.org/professionals/kdoqi/guidelines_ bp/guide_13.htm.
Q. Are automated blood pressure measurements reliable?
Kaelber: I agree with the report, which states “An elevated BP reading obtained with an oscillometric device [determines blood pressure with a cuff that measures the oscillations of blood flow] should be repeated by using auscultation [blood pressure taken with a cuff hooked up to a mercury manometer and the use of a stethoscope].” Depending on the type of office blood pressure measurement (manual versus automatic), systolic blood pressure can vary by 4.39 mmHg to 4.82 mmHg and diastolic blood pressure by 4.61 mmHg to 9.35 mmHg.16
REFERENCES
- National High Blood Pressure Education Program working Group on High Blood Pressure in Children and Adolescents. The fourth report on the diagnosis, evaluation, and treatment of high blood pressure in children and adolescents. Pediatrics. 2004;114(suppl):555-576.
- Kaelber DC, Pickett F. Simple table to identify children and adolescents needing further evaluation of blood pressure. Pediatrics. 2009;123:e972-974.
- Hansen ML, Gunn PW, Kaelber DC. Underdiagnosis of hypertension in children and adolescents. JAMA. 2007;298:874-879.
- Sorof JM, Turner J, Martin DS, et al. Cardiovascular risk factors and sequelae in hypertensive children identified by referral versus school-based screening. Hypertension. 2004;43:214-218.
- Boyd G, Koenigsberg J, Falkner B, et al. Effect of obesity and high blood pressure on plasma lipid levels in children and adolescents. Pediatrics. 2005;116:442-446.
- Manzoli L, Ripari P, Rotolo S, et al. Prevalence of obesity, overweight and hypertension in children and adolescents from Abruzzo, Italy. Ann Ig. 2005;17:419-431. D
- Falkner B, Gidding SS, Ramirez-Garnica G, et al. The relationship of body mass index and blood pressure in primary care pediatric patients. J Pediatr. 2006;148:195-200.
- Angelopoulos P, Milionis H, Moschonis G, et al. Relations between obesity and hypertension: preliminary data from a cross-sectional study in primary schoolchildren. The Children Study. Eur J Clin Nutr. 2006;60:1226- 1234.
- Denney-Wilson E, Hardy LL, Dobbins T, et al. Body mass index, waist circumference, and chronic disease risk factors in Australian adolescents. Arch Pediatr Adolesc Med. 2008;162:566-573.
- Urbina EM, Kimball TR, McCoy CE, et al. Youth with obesity-related type 2 diabetes mellitus demonstrate abnormalities in carotid structure and function. Circulation. 2009;119:2913-2919.
- DelGiorno C, Damaso L, Bird K, et al. Simple obesity without features of the metabolic syndrome is associated with increased cardiovascular risk even before the onset of puberty in children. Available at: www.medscape.com/viewarticle/704463. Accessed January 18, 2010.
- Pruette CS. PAS 2009: Black Children With Primary Hypertension Have High Risk for Ventricular Hypertrophy. Available at: www.medscape.com/viewarticle/702520. Accessed January 18, 2010.
- Chobanian AV, Bakris GL, Black HR, et al. The seventh report of the joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure: the JNC 7 report. JAMA. 2003;289:2560–2572.
- Gomez-Marin O, Prineas RJ, Rastam L. Cuff bladder width and blood pressure measurement in children and adolescents. J Hypertens. 1992;10: 1235–1241.
- American Heart Association. Home monitoring of high blood pressure. Available at: www.americanheart.org/presenter.jhtml?identifier=576. Accessed January 18, 2010.
- Wong SN, Tz Sung RY, Leung LC. Validation of three oscillometric blood pressure devices against auscultatory mercury sphygmomanometer in children. Blood Press Monit. 2006;11:281–291.
From Dimensions of Dental Hygiene. February 2010; 8(2): 20, 22, 24-25.

