Reduce Caries Risk with Topical Fluoride
Professionally applied topical fluorides are key to personalized caries prevention treatment planning.
Professional topical fluorides are an essential component of individualized treatment plans. In 2013, the American Dental Association (ADA) Council on Scientific Affairs published an executive summary that provided updated clinical recommendations for the evidence-based use of topical fluorides.1 In short, the summary supports the use of 2.26% fluoride varnish for patients younger than 6, and 2.26% fluoride varnish or 1.23% acidulated phosphate fluoride (APF) gel for patients older than 6 at least every 3 months to 6 months.
The recommendation of fluoride application should be tailored to each patient and based on caries risk. Only those at elevated caries risk should receive professionally applied topical fluorides. This article will discuss the types of professionally applied topical fluorides available (Table 1) in addition to providing a review of delivery methods and efficacy.1
ACIDULATED PHOSPHATE FLUORIDE
Acidulated phosphate fluoride (APF) 1.23% contains 12,300 ppm of fluoride ion,2 and comes in a foam and gel. However, the 2013 ADA Council on Scientific Affairs chairside recommendation’s advise against the use of 1.23% (APF) foam, as research has not demonstrated its efficacy for caries prevention.1 Benefits of using APF gel include storage, stability, acceptable taste, and tissue biocompatibility.2 Fluoride gels have been shown to reduce decayed, missing and filled tooth surfaces by 28% to 38%.1,3
Acidulated phosphate fluoride has a pH between 3.0 and 4.5. High concentration fluoride treatments provided at an acidic pH are more effective at promoting fluoride uptake in comparison to more alkaline formulations.4 However, the use of APF formulations can damage restorative materials via composite resin staining, softening, surface roughening, and decreased luster, due to their acidic pH.4–8
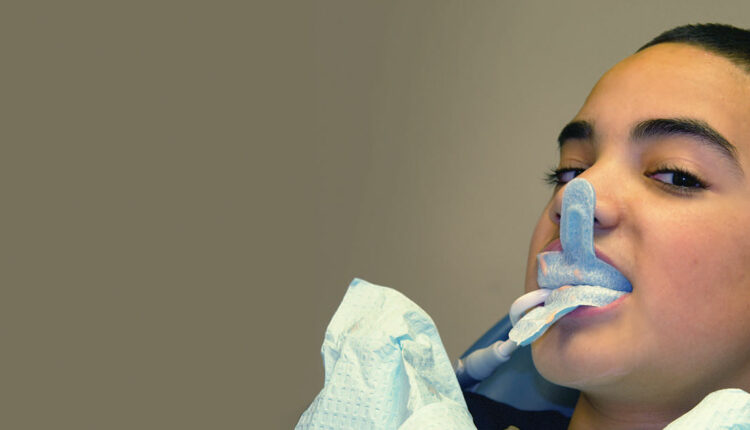
Applying an APF gel in a tray is safe and effective when used correctly. Patients should be seated upright to ensure minimal swallowing and an appropriate-sized tray should be used. Once the tray is loaded with fluoride and inserted, suction should be applied. Post-procedure, patients should be directed to avoid eating or drinking for 30 minutes because rinsing with water or cleaning the teeth immediately after the APF fluoride application reduces its ability to elevate plaque pH9 and decreases fluoride uptake. In addition, APF should be left in contact with the tooth for 4 minutes. Although most products still promote a 1-minute application process, most research supports a 4-minute application time.1 For children younger than 6, fluoride varnish is preferred over gel because it reduces the risk of excessive fluoride ingestion.1
![Topical fluoride agents]() NEUTRAL SODIUM FLUORIDE
NEUTRAL SODIUM FLUORIDE
Neutral sodium fluoride (NaF) 2.0% gel or foam was not included in the ADA Council on Scientific Affairs’ guidelines for caries prevention, but it is still available for professionally applied topical fluoride use. The gel or foam is available in a variety of flavors and has a pH of 7.0. A 2.0% sodium fluoride gel or foam contains 9,050 ppm of fluoride ion. Like APF, neutral sodium fluoride has good bioavailability, and acceptable taste.2 In contrast to APF, neutral sodium formulations are nonacidulated, so they do not cause roughening or pitting of restorative materials. The application method for NaF 2.0% gel mirrors the one outlined above for APF gels.
Fluoride varnish is a highly concentrated form of sodium fluoride. A 5% NaF varnish contains (2.26%) 22,600 ppm of fluoride ion.10 Fluoride varnish was initially approved by the United States Food and Drug Administration for the treatment of dentinal hypersensitivity but is used off-label for caries prevention. The anti-caries benefit of a 5% fluoride varnish is well established.11 A Cochrane review found that those treated with a fluoride varnish experienced an average reduction of 43% in decayed, missing, and filled tooth surfaces and when looking at the effect on newly erupted or deciduous teeth, a 37% reduction in decayed, missing, and filled surfaces was found.12
The delivery model of fluoride varnish enables the fluoride to have extended contact with the tooth. This reduces the risk of ingestion and prolongs contact time while decreasing the amount of product used in comparison to other treatments. For example, a fluoride varnish application uses approximately 7 mg compared with 30 mg of APF gel.2 Also, there is little evidence of adverse effects and patient nonacceptance.12
Fluoride varnish may be professionally applied two times to four times a year in the primary or permanent dentition.12 Patients who present with white spot lesions, especially those undergoing orthodontic treatment or those with poor self-care and high caries risk, may need to have fluoride varnish applied monthly for 6 months. The teeth are first dried and then the varnish is applied to each tooth. Patients are usually asked to refrain from hot liquids and hard or fibrous food, following the application. In addition, patients should avoid normal oral hygiene activities for several hours. Some fluoride varnish products also have a white to yellowish appearance that disappears when the product is removed.
SILVER DIAMINE FLUORIDE
Silver diamine fluoride (SDF) is a combination of sodium fluoride and silver nitrate. Silver nitrate has long been known as an effective antimicrobial agent and sodium fluoride has been used to reduce the incidence of dental caries.13 SDF has the ability to both arrest and prevent caries due to silver nitrate’s potent germicidal effect and fluoride’s ability to reduce decay.14 It is available in liquid form in a concentration of 38.3% to 43.2%.
SDF is approved as a dentinal hypersensitivity agent and also is used off-label for caries management. SDF is recommended to reverse or arrest noncavitated carious lesions.15 A systematic review by Chibiski et al16 showed that SDF was 89% more effective in controlling or arresting caries than other treatment or placebo in primary teeth and a literature review of primary and secondary preventive agents concluded that for primary prevention of root caries 38% SDF is preferred.17
A major disadvantage of SDF is that it causes dark staining of demineralized tooth surfaces, which can deter its acceptance.18 SDF is known to discolor areas of the tooth that are unsound or not intact. It is estimated that 40% to 90% of carious lesions can be arrested with a single application of SDF.19 Because single applications are not always adequate in arresting caries, SDF may need to be applied annually or every 6 months if areas are not restored. Practitioners should practice informed consent and explain potential side effects, and the need for follow-up to patients and caregivers.
SDF is easy to apply. Professionals should dry the teeth before applying the product, protect the patient’s eyes, avoid contact with skin or clothing, and minimize contact with mucous membranes. One drop applied with a microbrush is all that is needed for 4 teeth to 6 teeth and the area should be isolated before application. Excess solution should be removed from the microbrush prior to application. Apply for a minimum of 1 minute and allow to air dry. SDF application is contraindicated in those with ulcerative gingivitis or stomatitis. Pain on contact and increased absorption would be experienced in these individuals due to the disruption of the epithelial barrier seen with these conditions.13 Caution should be taken when a patient has a sensitivity to metals and a known silver allergy is a contraindication.13
CONCLUSION
The benefits of fluoride are well defined and there are many types of fluorides available. The oral health professional needs to be aware of the individual characteristics of fluoride types, the proper indication for use based on patient specificity, and also the governing practices for use of fluoride in their respective states.
REFERENCES
- Weyant RJ, Tracy SL, Anselmo TT, et al. Topical fluoride for caries prevention: executive summary of the updated clinical recommendations and supporting systematic review. J Am Dent Assoc. 2013;144:1279–1291.
- Wilkins E. Clinical Practice of the Dental Hygienist. 12th ed. Philadelphia: Wolters Kluwer; 2017.
- Marinho VC, Worthington HV, Walsh T, Chong LY. Fluoride gels for preventing dental caries in children and adolescents. Cochrane Database Syst Rev. 2015;6:CD002280.
- Mujeeb A, Mansuri S, Hussain SA, Ramaswamy K. In vitro evaluation of topical fluoride pH and their effect on surface hardness of composite resin-based restorative materials. J Contemp Dent Pract. 2014;15:190–194.
- Ozdemir-Ozenen D, Sungurtekin E, Issever H, Sandalli N. Surface roughness of fluoride-releasing restorative materials after topical fluoride application. Eur J Paediatr Dent Off J Eur Acad Paediatr Dent. 2013;14:68–72.
- Hosoya Y, Shiraishi T, Puppin-Rontani RM, Powers JM. Effects of acidulated phosphate fluoride gel application on surface roughness, gloss and colour of different type resin composites. J Dent. 2011;39:700–706.
- Hammad SM, Al-Wakeel EE, Gad E-S. Mechanical properties and surface characterization of translucent composite wire following topical fluoride treatment. Angle Orthod. 2012;82:8–13.
- Kim YJ, Jang K-T, García-Godoy F. Effect of acidulated phosphate fluoride (APF) gel on the adherence of cariogenic bacteria to resin composites. Am J Dent. 2005;18:91–94.
- Fatemeh M, Marjan S, Homa N, Maryam T, Mahsa S. Effect of water rinsing after acidulated phosphate fluoride gel on dental plaque acidity: an in situ study. Pediatr Dent. 2014;36:56–60.2012;46:31–37.
- Bonetti D, Clarkson JE. Fluoride varnish for caries prevention: efficacy and implementation. Caries Res. 2016;50Suppl 1:45–49.
- Arruda AO, Senthamarai Kannan R, Inglehart MR, Rezende CT, Sohn W. Effect of 5% fluoride varnish application on caries among school children in rural Brazil: a randomized controlled trial. Community Dent Oral Epidemiol. 2012;40:267–276.
- Marinho VC, Worthington HV, Walsh T, Clarkson JE. Fluoride varnishes for preventing dental caries in children and adolescents. Cochrane Database Syst Rev. 2013;7:CD002279.
- Horst JA, Ellenikiotis H, Milgrom PM. UCSF protocol for caries arrest using silver diamine fluoride: rationale, indications, and consent. J Calif Dent Assoc. 2016;44:16–28.
- Rosenblatt A, Stamford TCM, Niederman R. Silver diamine fluoride: a caries “silver-fluoride bullet.” J Dent Res. 2009;88:116–125.
- Slayton RL, Urquhart O, Araujo MWB, et al. Evidence-based clinical practice guideline on nonrestorative treatments for carious lesions: A report from the American Dental Association. J Am Dent Assoc. 2018;149:837–849.
- Chibinski AC, Wambier LM, Feltrin J, Loguercio AD, Wambier DS, Reis A. Silver diamine fluoride has efficacy in controlling caries progression in primary teeth: a systematic review and meta-analysis. Caries Res. 2017;51:527–541.
- Gluzman R, Katz RV, Frey BJ, McGowan R. Prevention of root caries: a literature review of primary and secondary preventive agents. Spec Care Dent Off Publ Am Assoc Hosp Dent Acad Dent Handicap Am Soc Geriatr Dent. 2013;33:133–140.
- Crystal YO, Janal MN, Hamilton DS, Niederman R. Parental perceptions and acceptance of silver diamine fluoride staining. J Am Dent Assoc. 2017;148:510–518.
From Dimensions of Dental Hygiene. April 2019;17(4):18, 21.



Just wanted to make a few additional notes to the article on Fluoride from the April 2019 edition… Related to Varnish, there are over 60 different products on the market. Not all of them require the teeth to be dry. Please read the instructions from each company that you purchase to make sure that you know how they suggest application. Some suggest having the teeth wet. Also there are some varnishes that are made with Rosin or Colophony and some that are synthetic. If you are concerned with any nut allergies, the synthetic or shellac options may be a better way to go. Check with the company you buy from…