
Redefine Risk
Head and neck cancers associated with human papillomavirus affect many patients who don’t present with the traditional risk factors for oral cancer.
This course was published in the March 2013 issue and expires March 2016. The author has no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- Identify key differences between human papillomavirus (HPV)-positive and HPV-negative head and neck cancers.
- Differentiate between the various strains of HPV.
- Discuss the risk factors for HPV-associated oropharyngeal cancers.
- Suggest educational messages that could reduce the presence of HPV oral infection.
Early detection of head and neck cancers (HNCs) by dental hygienists can save lives. HNCs include cancers of both the oral cavity and the oropharyngeal regions. While many oral cavity cancers are found on the buccal mucosa, gingiva, front and ventral surfaces of the tongue, hard palate, and retromolar regions, human papillomavirus (HPV)-positive lesions are primarily found in the oropharyngeal region.
Oral cavity cancers were the most prevalent types of HNCs in the United States during the 1960s, 1970s, and 1980s.1 Over the past 20 years, the incidence of non-HPV oral cavity cancers has declined, while the rate of HPV-positive oropharyngeal cancers continues to rise. In fact, from 1988 to 2004, the rate of HPV-positive squamous cell carcinomas in the head and neck regions increased by 225%.1–3
Clear distinctions between HPV-negative oral cancers associated with tobacco and alcohol use and HPV-related oropharyngeal cancers also exist. The etiology, lesion location, risk factors, and affected populations for each condition vary.4,5 Given these differences and the impetus to implement evidence-based practice, dental hygienists may need to rethink their clinical and educational roles regarding the prevention of HNCs.
Over the past several decades, scientists have found that different sociodemographic variables and risks are associated with HPV-positive HNCs. The target population most vulnerable to HPV-positive cancers is white men under the age of 50, a group not typically associated with traditional oral cavity cancers.1 Oral cavity cancers were historically most prevalent among older black men. The male to female ratio for non-HPV-associated cancers is 6:1. When looking at HPV-positive HNCs, this ratio is cut in half to 3:1.6
LOCATION
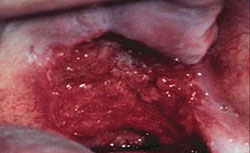
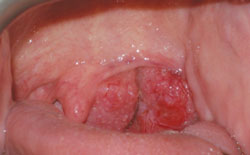
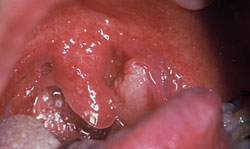
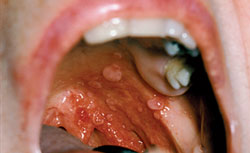
HPV-positive lesions are primarily found in the oropharyngeal region, eg, tonsillar areas, base of the tongue, and soft palate. Figure 1 through Figure 4 show examples of HNC lesions with varying appearances. Each of these lesions is easily visible with the naked eye. Because HPV lesions are predominant in this area, the oropharyngeal areas should be targeted during HNC screenings. Close examination of the soft palate and tonsillar regions is essential.
TRANSMISSION
More than 100 types of HPV strains exist. HPV 16 and 18 are the most virulent, and HPV 16 is related to almost all cervical cancers. HPV infection is the most prevalent sexually-transmitted disease in the US. Among American women, 42.5% have genital HPV infections.7 Despite this high rate of infection, 91% of those infected clear the virus within 1 year to 2 years. Thus, the number of cervical infections that transform into cervical cancers is relatively low.
Today, more than half of the oropharyngeal cancers diagnosed in the US are linked to HPV 16.2 Human sexual contact is strongly associated with HPV-positive HNCs.8,9 High-risk sexual behaviors heighten the potential risk of HPV-associated head and neck squamous cell carcinomas.10 Oral HPV infection most likely precedes the development of HPV-positive oropharyngeal cancers, similar to the cervical cancer model where HPV infection is present prior to the development of a cancerous neoplasm. Further, the risk factors for HPV infection and HPV-associated oropharyngeal cancers may be the same. However, the life cycle and clearance of oral HPV infection are not well understood.11
Because HPV 16 is implicated in both cervical and HNCs, understanding its mode of transmission is important. Several transmission routes for HPV exist but all are based on human-to-human contact, primarily sexual. Women with HPV-associated cervical cancer and dysplasia demonstrate a higher incidence of oral squamous cell carcinomas, as do their partners.12 Other transmission pathways include: from mother to child during cervical canal delivery (vertical transmission); from infected person to other family members, ie, to infants via breast milk (horizontal); and auto-inoculation through masturbation.13 Transmission may be heightened in the presence of certain behaviors, such as oral sex, penetrating sex, and open-mouthed kissing with salivary exchange. Studies show that more than six acts of oral sex increase the risk of HPV-positive oropharyngeal cancers, and that more than 26 lifetime genital sex partners, as well as early age at first intercourse, may facilitate the entry of HPV into the susceptible host.9 More recently, Gillison et al found that oral sex is the main culprit in HPV-positive oropharyngeal cancer development, and that more casual encounters, such as open-mouth kissing, may not be as related.5
While tobacco use is associated with 90% of oral cavity cancers, with excessive drinking additionally raising this risk, patients with HPV-positive cancers are typically nontobacco users and modest to nondrinkers. However, they may use marijuana, as cannabis is associated with HPV-positive cancers.8,9 Those with HPV-positive cancers are often college educated and earn substantial incomes.
OTHER FACTORS RELATED TO CANCER DEVELOPMENT
Chronic inflammation may also facilitate cancer growth as the risks of neoplastic development increase in the presence of chronic inflammation. For example, risks for pancreatic, cervical, and colon cancer are heightened among patients who have chronic pancreatitis, cervicitis, and irritable bowel syndrome, respectively. Tezal et al suggest that chronic oral inflammation, eg, chronic periodontal diseases, may influence the development of HPV-positive HNCs.14,15 Research also supports the involvement of saliva in carcinogenesis. Saliva metabolizes tobacco and alcohol into carcinogens; promotes viral transmission and replication; and interacts with shed viruses, bacteria, and other carcinogenic metabolites. More than 75% of oral cancers are found in saliva drainage sites.14 Bacteria also may be involved in the development of oral cavity cancers. Bacteria can induce changes in epithelium, are involved with genetic change, and can increase the magnitude of carcinogens. It remains unclear whether inflammation, rather than bacteria alone, is the true contributing source.
Comparisons of HPV with the herpes virus also have been made. When the herpes virus is present in the oral cavity, periodontal pockets contain more bacteria. Saliva in the presence of herpes is also associated with a high viral load, potentially increasing the risk of viral transmission. The same actions may take place in the presence of HPV. A pathology catalyzed by saliva, bacteria, shed viruses, and inflammation may enhance the development of HPV-positive oropharyngeal cancers. Based on these theories, Tezal et al suggest that an assault on chronic periodontal infection may be needed to reduce the potential for HPV-positive HNC development. Should further research support these theories, dental hygienists’ clinical interventions will become even more critical.14,15
TREATMENT
Treatment for patients with HPV-positive HNCs usually includes a combination of chemotherapy and radiation. Surgery is often required. The prognosis for HPV-positive HNCs seems to be more positive than for non-HPV head and neck neoplasms.16 Several explanations for this theory have been proposed. HPV-positive cancers appear to be more sensitive to treatment. Given that HPV-positive patients with HNC tend to be younger, they have had less time to acquire other comorbidities. Also, negative health behaviors are less entrenched among young patients.
BENIGN LESIONS
Other benign oral lesions related to HPV strains exist. These conditions are associated with less virulent strains of HPV, namely 2, 4, 6, 11, 13, 32, 40, 53, and 54. Oral condy lomas and papillomas are commonly associated with HPV 6 and 11. Oral warts, presenting as focal epithelial hyperplasia or Heck’s disease and oral verrucas (verruca vulgaris), are caused by HPV type 13 and 32, 2 and 4, and 6 and 40, respectively. Considered to be sexually-transmitted conditions, although they also may be spread through autoinoculation, oral condylomas are often found in patients with human immunodeficiency (HIV). Typically, condylomas appear as sessile pink or white coalescing nodules on the labial mucosa, lingual frenum, palate, and tongue. Despite removal, they often recur. Papillomas, as well as HPV-positive lesions, can be found in the uvulopalatal region, thus making biopsy essential. Oral warts are rare. They appear as small white keratinized lesions and may be spread by autoinoculation from warts on the skin.17,18
PROCESS OF CARE
The prevalence of HPV-associated HNCs necessitates examination of the dental hygiene process of care. Approaches to patient assessment may require reconsideration. Dental hygienists need to be aware of the broad-based population vulnerable to HPV-associated HNCs. Patient reports of symptoms, social histories, and prior health conditions associated with HPV must be considered and documented.
A head and neck exam must involve thorough investigation of the visible oropharyngeal areas. Patients must be supine when the oropharynx is examined to improve visibility of the oral cavity. Extraoral swellings may also be indicative of a neoplasm, so extraoral palpation is essential (Figure 5). Persistent coughing, difficulty swallowing, trismus, and headaches are associated with oral cavity cancers. Since these symptoms are similar to other common conditions, follow-up regarding their persistence is critical.
PATIENT EDUCATION
In addition to clinical protocols, dental hygienists intent on preventing HPV infection need to broaden their educational messages. Discussing prevention naturally flows into the topic of HPV-associated HNC. Educational messages that include tobacco prevention and cessation must address marijuana use as well. With the high prevalence of risky sexual practices among young adults, practitioners will need to make decisions as to whether they want to discuss sexual practices with patients, and accordingly, how and when they should do it. A recent data analysis found that 23% of girls and 21% of boys reported sexual intercourse by the age of 15; this rate increased to 78% and 84%, respectively, by age 20.19 In a survey of more than 13,000 subjects, oral sex was prevalent among 27% of 15-year-old boys and 23% of 15-year-old girls.10 Among teenagers age 15 to 19, 7% of girls and 9% of boys had experienced oral sex with an opposite-sex partner, but no vaginal intercourse.10 Historically, health care practitioners have avoided discussions related to sensitive topics.
Each dental hygienist will need to determine his or her comfort level and the practice philosophy.
VACCINATION
Dental hygienists are concerned with total patient well-being, thus, HPV vaccine information is relevant to share with adolescents and young adults and their parents. The link between HPV and certain HNCs fits right into this discussion. Two vaccines are currently available to consumers. One is quadrivalent and targets four strains of HPV while the other targets two high-risk viruses and genital warts. Patients need to understand that vaccination prevents infection, it does not treat it. Although recommendations for age of inoculation vary slightly, both male and female youth and young adults between the ages of 11 and 26 are appropriate candidates. Vaccines should be administered before the risk of HPV exposure via sexual practices.
CONCLUSION
Forecasts regarding the infectious spread of HPV are dire—future prevalence may be of epidemic proportions. By 2020, researchers estimate that HPV will cause more oropharyngeal cancers than cervical cancers in the US.2 The rise in HPV-positive HNCs raises an important question: what role should the dental hygienist play in preventing the spread of HPV and in discussing the risks associated with HPV-positive HNCs? Dental hygienists can be instrumental in preventing the development of oral HPV infection and decreasing the potential for oropharyngeal cancer development. During patient treatment, dental hygienists must be cognizant of patient risk factors and the unique characteristics of HPV-associated HNCs. With this knowledge, dental hygienists will be better prepared to save lives.
ACKNOWLEDGEMENTS
CREDIT : SCIEPRO/SCIENCE PHOTO LIBRARY
CREDIT : FIGURE 1. MICHAEL FINKELSTEIN, DDS, MS, AND GILBERT E. LILLY, DDS
CREDIT : FIGURES 2–4. MARTIN TYLER, DDS, MEd, AND PENWELL CORP
CREDIT : FIGURE 5. ANDREW R. SALAMA, DDS, MD, FACS
REFERENCES
- Chaturvedi AK, Engels EA, Pfeiffer RM, et al.Human papillomavirus and rising oropharyngeal cancer incidence in the United States. J Clin Oncol. 2011;29:4294–4301.
- American Cancer Society. Cancer Facts andFigures 2011. Atlanta: American Cancer Society;2011.
- Kreimer AR, Clifford GM, Boyle P, Franceschi S.Human papillomavirus types in head and neck squamous cell carcinomas worldwide: asystematic review. Cancer Epidemiol Biomarkers Prev. 2005;14:467–775.
- D’Souza G, Kreimer AR, Viscidi R, et al. Case control study of human papillomavirus and oropharyngeal cancer. N Engl J Med.2007;356:1944–1956.
- Gillison ML, Broutian T, Pickard RK, Tong Z,Weihong X. Prevalence of oral HPV infection in the United States, 2009-2010. JAMA. 2012;307:693–703.
- Centers for Disease Control and Prevention(CDC). Human papillomavirus-associated cancers—United States, 2004-2008. MMWR MorbMortal Wkly Rep. 2012;61:258–261.
- Hariri S, Unger ER, Sternberg M, et al.Prevalence of genital human papilloma virus among females in the United States, theNational Health and Nutrition Examination Survey, 2003–2006. J Infect Dis. 2011;204:566–573.
- Gillison ML. Human papillomavirus-related diseases: oropharynx cancers and potential implications for adolescent HPV vaccination. J Adolesc Health. 2008;43(Suppl):S52–S60.
- D’Souza G, Agrawal Y, Halpern J, Bodison S,Gillison ML. Oral sexual behaviors associated with prevalent oral human papilloma virus infection.J Infect Dis. 2009;199:1263–1269.
- Chandra A, Mosher WD, Copen C, Sionean C.Sexual behavior, sexual attraction, and sexual identity in the United States: data from the 2006-2008 National Survey of Family Growth. Natl Health Stat Report. 2011;36:1–36.
- Marur S, D’Souza G, Westra WH, Forastiere AA. HPV-associated head and neck cancer: a virus-related cancer epidemic. Lancet Oncol. 2010;11:781–789.
- Hemminki K, Dong C, Firsch M. Tonsillar andother upper aerodigestive tract cancers among cervical cancer patients and their husbands. Eur J Cancer Prev. 2000; 9:433–437.
- Yoshida K, Furumoto H, Abe A, et al. Thepossibility of vertical transmission of human papillomavirus through maternal milk. J Obstet Gynaecol. 2011;31:503–506.
- Tezal M, Sullivan Nasca M, Stoler DL, et al.Chronic periodontitis-human papillomavirus synergy in base of tongue cancers. Arch Otolaryngol Head Neck Surg. 2009;135:391–396.
- Tezal M. Interaction between chronic inflammation and oral HPV infection in the etiology of head and neck cancers. Int J Otolaryngol. 2012;2012:575242.
- Ang KK, Harris J, Wheeler R, et al. Human papilloma virus and survival of patients with oropharyngeal cancer. N Engl J Med.2010;336:24–35.
- Syrjänen S, Lodi G, von Bü?ltzingslöwen I, et al. Human papilloma viruses in oral carcinoma and oral potentially malignant disorders: a systematic review. Oral Dis. 2011;17(Suppl):58–72
- Lukes SM, Meneses MB. The dentalhygienist’s role in HPV recognition. Dimensions of Dental Hygiene. 2010;8(6):72–77.
- Abma JC, Martinez GM, Copen CE. Teenagersin the United States: sexual activity, contraceptive use, and childbearing, national survey of familyg rowth 2006-2008. Vital Health Stat 23.2010;30:1–47.
From Dimensions of Dental Hygiene. March 2013; 11(3): 46–49.



