Prevent Digital Radiography Pitfalls
How to avoid common mistakes When taking digital X-rays.
While the benefits of digital radiography, including reduced radiation exposure and improved efficiency, are numerous, the use of digital sensors and photostimuable phosphor plates (PSPs) can present challenges for clinicians who are accustomed to taking film X-rays. Here are three common mistakes when using digital sensors and PSPs, and strategies for avoiding them.
MISSING IMPORTANT ANATOMY
Digital sensors and PSPs have smaller recording dimensions, which can lead to radiographs that are missing important anatomy, thus increasing the need for additional exposures.
As all clinicians are bound to the “as low as reasonably achievable” (ALARA) principle of reducing patients’ exposure to radiation, unnecessary retakes should be avoided. To prevent missing important anatomy due to the smaller dimensions of the sensor or PSP, the vertical or horizontal angulation of the X-ray beam can be altered to project the desired area onto the image receptor (Figure 1). The apices of the teeth can also get cut off when periapical X-rays are taken. To prevent this, the vertical and horizontal angulations should be directed toward the image receptor, which enables the recording of anatomy that appears beyond the dimensions of the sensor. However, the angulation should not shift more than 15° away from perpendicular.
Recording the distal edge of the canines during bitewing radiographs can also be challenging. By positioning the anterior edge of the digital sensor away from the lingual surfaces of the teeth, the distal edges of the canines can be recorded. In order to prevent an overlap error, the sensor should be placed toward the middle of the oral cavity with the anterior edge of the sensor positioned forward, closer to the canine on the opposite side (Figure 2).
HORIZONTAL OVERLAP

The maxillary first molars, maxillary second molars, and distal edges of the canines with the premolars are at the greatest risk for overlap error in digital radiography. Overlap is common because the size of the digital sensors can interfere with the precise placement needed to image the teeth’s embrasures.
The large rhomboid shape of the maxillary first molar increases the overlap risk. To prevent this problem, the image receptor should be placed as if taking a premolar radiograph (Figure 3). The image receptor should be positioned away from the lingual surface of the premolar. Overlap errors of the distal edge of the canine with the first premolar are affected by anatomy, as well. The first premolar’s wide dimension can superimpose the lingual cusp onto the image of the canine. To avoid this overlap, the horizontal angulation of the tube head should be positioned so the X-ray beam intersects the canine from a slightly distomesial position. Little to no overlap of the canine and premolar contact will occur if the tube head shift is less than 15.º
IMAGE CONTRAST
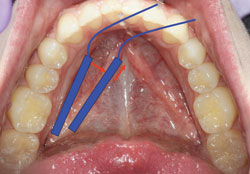
Image contrast is a critical characteristic of a diagnostic quality dental radiograph. Accurate diagnoses depend on the ability of the image to discriminate between different levels of gray. The human eye can generally distinguish between 32 gray levels, while computer monitors display a maximum of 256 gray levels.
However, some digital imaging systems are capable of recording up to 65,536 levels of gray.1 One of the advantages of digital imaging is the ability to tease out and highlight additional information captured by the sensor. To take full advantage of this capability, clinicians need to evaluate X-ray-generating equipment for optimum compatibility with the digital system and determine the appropriate exposure settings prior to capturing the image. Failing to update X-ray generating equipment when necessary and making mistakes in choosing an exposure setting can result in two distinct problems: low contrast images that cannot be corrected with software, and images that appear to be of normal density, but that may be unnecessarily exposing the patient to radiation.
Research has indicated that using precise electronic exposure timers capable of regulating exposures in 1/100 of a second intervals and direct current X-ray generators with low kVp (60 or 65) and low mA (5 or 7) settings are ideally suited to producing high-quality diagnostic digital images.2,3 When switching from film-based imaging, it is sometimes recommended to refit older X-ray generators with an electronic timer.
Because digital imaging systems offer contrast manipulation to enhance the image, the practitioner may be lulled into careless attention to exposure settings. Especially common when switching from film-based radiography to digital imaging, reducing radiation exposure to a drastically low level may produce electronic noise, the equivalent of film-fog, which produces a severely low contrast image.

These low contrast images cannot be corrected by software as readily as images that are overexposed.2 Manufacturers of digital imaging systems provide exposure setting suggestions to assist in avoiding mistakes.However, these guidelines may be based on conditions, such as preset kVp and mA settings and a position indicating device or focal-spot-to-object length, that does not match the equipment used by the practice, setting up a situation of trial-and-error experimentation to determine the best exposure settings. Clinicians need to know how to adjust the exposure recommendations to match the equipment used in practice.
Clinicians who need to refresh their knowledge of coordinating and matching exposure variables may benefit from consulting a dental hygiene radiology textbook for a review of the calculations used to adjust the factors affecting the radiographic image. When using PSP digital systems, determining the precise exposure settings to avoid
unnecessary radiation exposure to patients is critical. PSP plated sensors have what’s called a “wide latitude of exposure.” This characteristic allows for self-adjustment so that the image does not exhibit the typical increased density that would ordinarily alert the practitioner to a radiation overdose potential.4
Careful attention to correct exposure settings can assist in avoiding images with low contrast and increased electronic noise, and in preventing routine use of software to correct overexposed images at the patient’s expense.
CONCLUSION
Keeping up-to-date on digital radiography technique is imperative to the safe and effective use of this modality. Clinicians can improve their skills by reviewing radiography textbooks, attending high-quality continuing education courses, and reading the literature. By honing these skills, clinicians will be better able to avoid mistakes while obtaining high-quality diagnostic images.
- Farman AG, Farman TT. A comparison of 18 different x-ray detectors currently used in dentistry. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2005;99:485–489.
- Iannucci JM, Howerton LJ. Dental Radiography. Principles and Techniques. 4th ed. St. Louis: Elsevier Saunders; 2012:303.
- Thomson EM, Johnson ON. Essentials of Dental Radiography for Dental Assistants and Hygienists. 9th ed. Upper Saddle River, NJ: Pearson Education; 2012:104.
- Van der Stelt PF. Better imaging: the advantages of digital radiographs. J Am Dent Assoc. 2008;139:7S–13S.
From Dimensions of Dental Hygiene. June 2013; 11(6): 45–46.

