
Mistaken Identity
While gingival cancers can be difficult to detect, survival rates depend on early treatment.
The establishment of a mutually respectful and collaborative relationship between dentists and dental hygienists is key to the provision of high-quality dental care. One of the most crucial collaborative efforts is performing a thorough head and neck exam. Dentists rely on dental hygienists to perform a systematic examination of the oral cavity and the entire head and neck complex. Additionally, dental hygienists are instrumental in educating patients about oral cancer, and they are often the first clinicians to note any variations from normal within the oral cavity. Even with this systematic approach, some gingival cancers may be challenging to identify when inflammatory components are involved, and their initial presentation appears as a dental abscess, trauma, or periodontal disease.1–3 Gingival cancers are rare, and their initial presentation may be missed due to their location. Unfortunately, a delay in early intervention may adversely affect survival rates.
This article outlines a gingival cancer that initially presented with features of periodontal disease and, thus, hindered a definitive diagnosis that delayed treatment.
CASE STUDY
An 85-year-old woman was seen for comprehensive care in a dental residency clinic. The patient was hypertensive and reported occasional alcohol consumption and no tobacco use. After an initial examination, she was diagnosed with generalized moderate periodontitis and localized severe periodontitis in the mandibular left quadrant. Pocket depths ranged from 6 mm for teeth #20 and #21 to 9 mm for teeth #18 and #19. Scaling and root planing was performed, along with extractions of teeth #18 and #19 due to their severe attachment loss and mobility.
The treatment plan included a mandibular removable partial denture to replace teeth #18 and #19. The patient returned within 2 weeks for study models. The healing of the extractions sites was favorable. A final impression for the mandibular removable partial denture was obtained 1 week later. The patient returned for a 6-week reevaluation of the scaling and root planing therapy. The tissue response was favorable for the maxillary arch and mandibular right quadrant; however, there was moderate plaque accumulation and severe inflammation of the gingival tissue in the mandibular left quadrant on tooth #20 and slightly distal on the edentulous segment. Pocket depths ranged from 3 mm to 4 mm. As the nature of the lesion aroused suspicion, the clinic’s oral surgeon was summoned to evaluate the site. The oral surgeon thought the inflammation was caused by the accumulation of plaque and residual subgingival calculus, and the patient admitted to avoiding brushing the area after extractions of teeth #18 and #19. The area was scaled again, and the patient was reinstructed on proper oral hygiene care. A mandibular partial denture was inserted at this visit, and the patient received instructions on its care.
The patient was scheduled 2 weeks later for a follow-up of the removable partial denture and evaluation of the mandibular left quadrant. At the second evaluation visit, the tissue in the mandibular left quadrant was very inflamed and erythematous, and the texture had changed with noticeable white specks and a pebbly appearance distal to tooth #20. The patient complained of moderate pain, which was due to irritation and inflammation caused by the partial denture. The pressure spots were relieved on the partial denture; however, the severe erythema and dramatic change of the gingiva prompted a referral to an oral surgeon for a second opinion. The oral surgeon biopsied the lesion, and the pathology report noted verrucous carcinoma—a type of squamous cell carcinoma, as the definitive diagnosis.
Typically, a suspicious lesion is recommended for biopsy after it has been present for 2 weeks or longer. With this patient, in the 2-week interval after the extractions and initial scaling and root planing, the tissue response had been favorable. At the 6-week reevaluation, however, the tissue revealed severe inflammation, moderate plaque, and residual subgingival calculus, which led the oral surgeon to suspect periodontal disease—not gingival cancer. To compound the issue, the pressure spots from the removable partial denture contributed to the inflammation and misdiagnosis. The appearance of the lesion changed more dramatically the following 2 weeks, at which point the referral for biopsy was made. This case reinforces the need to review oral pathology—particularly gingival cancer.
SQUAMOUS CELL CARCINOMA
More than 90% of oral cancers present as squamous cell carcinoma.4 Lesions range from a white plaque-like appearance to a red and white exophytic appearance that can develop anywhere in the mouth, but most frequently occurs on the tongue, tonsils, oropharynx, and floor of the mouth.4 Vigorous examination of these specific areas may lead to missing gingival lesions entirely when an inflammatory component and an initial impression of periodontal disease are present. The emphasis should be placed on evaluating gingival and inflammatory lesions more closely for the possibility of gingival cancers. The patient may be asymptomatic in the early stages, but with progression of the gingival cancer, symptoms can include a swelling or mass, pain, and mobility of teeth due to destruction of underlying bone.5 At late stages, the prognosis is poor.
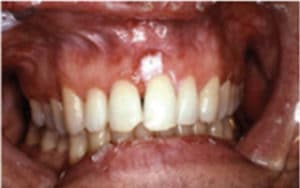 FIGURE 1. This image depicts an aspirin burn caused by the patient applying the pain reliever directly to the gingival tissue instead of consuming it orally. COURTESY OF SOL SILVERMAN, JR, MA, DDS.
FIGURE 1. This image depicts an aspirin burn caused by the patient applying the pain reliever directly to the gingival tissue instead of consuming it orally. COURTESY OF SOL SILVERMAN, JR, MA, DDS.
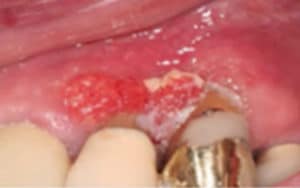 FIGURE 2. This squamous cell carcinoma of the gingiva was present for quite some time before a diagnosis was achieved.
FIGURE 2. This squamous cell carcinoma of the gingiva was present for quite some time before a diagnosis was achieved.
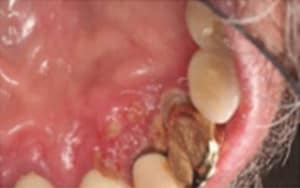 FIGURE 3. Squamous cell carcinoma of the gingiva, as pictured here, was not detected in its earliest stages. COURTESY OF DARREN COX, DDS, MBA
FIGURE 3. Squamous cell carcinoma of the gingiva, as pictured here, was not detected in its earliest stages. COURTESY OF DARREN COX, DDS, MBA
Squamous cell carcinoma of the gingiva may be difficult to diagnose in its early stages when inflammatory components and bone loss are present.6 Lesions can range from white, mixed white and red, or red in appearance. White lesions are usually recognized more readily. Figure 1 demonstrates a white plaque-like lesion on the facial of tooth #9, which was caused by an aspirin burn. Figure 2 and Figure 3 demonstrate white plaque-like lesions with erythematous components on the facial and palatal gingival margins of teeth #9, #10, and #11. When evaluating lesions with this clinical presentation, clinicians should ask a series of questions to aid in a definitive diagnosis. For instance, if trauma or a chemical burn is suspected, the following series of questions should be asked.
- Have you noticed the change in color of your gingiva in this area?
- If so, how long has this lesion been present?
- Does it hurt?
- Did you place aspirin in the area of discomfort?
Some patients erroneously think that direct topical application of a pain reliever will be more effective than taking it orally. This is precisely what the patient did in Figure 1. Most dental professionals would recommend the patient return in 2 weeks to reevaluate the area; in the absence of resolution, a referral for a biopsy would be indicated. This is the ideal scenario but often not the case. Prime examples are illustrated in Figure 2 and Figure 3, where the lesion had been present for some time before a definitive diagnosis of squamous cell carcinoma of the gingiva was confirmed through a biopsy. This lesion presented at an advanced stage of cancer that is now more challenging to treat.
Figure 4 through Figure 6 demonstrate various forms of squamous cell carcinoma that may be initially mistaken for frictional keratosis or pyogenic granuloma. Any suspicious lesion or ulcerated tissue should be followed up with another evaluation within 2 weeks of presentation. If a lesion persists, and/or is nonhealing, then a referral to an oral surgeon or oral pathologist is indicated. Good documentation regarding the color, location, size, and texture of the lesion will make it easier to evaluate at the second visit.
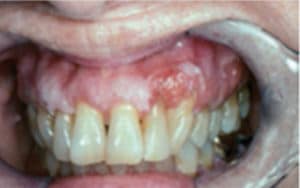 FIGURE 4. This patient was diagnosed with leukoplakia on the gingival site of tooth #7 and #9, and squamous cell carcinoma on the gingiva between tooth #10 and #11. COURTESY OF SOL SILVERMAN, JR, MA, DDS.
FIGURE 4. This patient was diagnosed with leukoplakia on the gingival site of tooth #7 and #9, and squamous cell carcinoma on the gingiva between tooth #10 and #11. COURTESY OF SOL SILVERMAN, JR, MA, DDS.
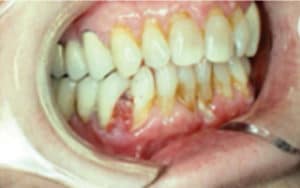 FIGURE 5. A squamous cell carcinoma, this lesion was mistaken for pyogenic granuloma. COURTESY OF SOL SILVERMAN, JR, MA, DDS.
FIGURE 5. A squamous cell carcinoma, this lesion was mistaken for pyogenic granuloma. COURTESY OF SOL SILVERMAN, JR, MA, DDS.
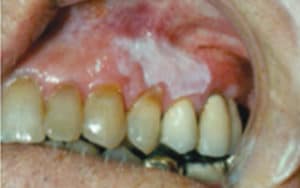 FIGURE 6. Moderate to severe epithelial dysplasia is present in this patient with squamous cell carcinoma. COURTESY OF SOL SILVERMAN, JR, MA, DDS.
FIGURE 6. Moderate to severe epithelial dysplasia is present in this patient with squamous cell carcinoma. COURTESY OF SOL SILVERMAN, JR, MA, DDS.
Taking a photograph of the initial lesion is recommended. If dental practitioners routinely take photos of oral lesions, a helpful library of images can be developed that may prove invaluable to oral pathologists, dentists, and dental hygienists. If a biopsy is indicated, the picture can be forwarded to the oral pathologist to aid in the diagnosis. Asking questions is crucial and may trigger the patient’s memory, providing information helpful to arriving at a diagnosis.
ORAL VERRUCOUS HYPERPLASIA AND CARCINOMA
Oral verrucous hyperplasia presents as a white, plaque-like lesion. It is difficult to distinguish from oral verrucous carcinoma and tends to precede verrucous carcinoma.7 People who use smokeless tobacco and drink one or more alcoholic beverages per month are predisposed to verrucous hyperplasia.7 For this reason, these lesions should be closely evaluated and not dismissed as benign.
Oral verrucous carcinoma is a form of squamous cell carcinoma with a variable appearance and unknown etiology.7 It may present as a white, plaque-like lesion or a mixed white-red lesion with a pebbly, wart-like surface.7 Figure 7 illustrates a more advanced form of verrucous carcinoma. It occurs more frequently in the mandibular posterior alveolar ridge and retromolar region, but can also present in the buccal mucosa, palate, floor of the mouth, and lip.7
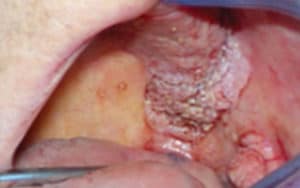
The case study patient had a partial denture and the site of the verrucous carcinoma occurred on the gingiva distal to tooth #20 and on the alveolar ridge. In partially edentulous patients, areas of concern include the gingival tissue of the abutment teeth retaining the removable appliance and the alveolar ridge area. Patients with removable partial dentures or full dentures should be scrutinized closely for these types of lesions. While it is true that some of the lesions associated with removable appliances are due to pressure spots or ill-fitting dentures, various precancerous or cancerous lesions may present similarly.
CONCLUSION
The gingival cancer in this case study initially presented as periodontal disease with local etiologic factors of inflammation, bone loss, and subgingival calculus. No risk factors for gingival cancer were present. An accurate diagnosis was delayed, as completion of periodontal therapy and reevaluation of treatment took an average of 2 months to 3 months. This case illustrates the need to be highly diligent when evaluating gingival lesions. Dental hygienists see patients on a regular basis, and their skill in identifying areas of concern in the oral cavity is invaluable. If the lesion is still present after 2 weeks, the patient should be referred to an oral surgeon or oral pathologist for biopsy. Early detection of cancer is crucial to an increased survival rate. It behooves both dentists and dental hygienists to promptly refer when gingival lesions are unresponsive to the usual treatment modalities.
REFERENCES
- Seoane J, Varela-Centelles PI, Walsh TF, Lopez-Cedrun JL, Vazquez I. Gingival squamous cell carcinoma: diagnostic delay or rapid invasion? J Periodontol. 2006;77:122–133.
- Lee JJ, Cheng SJ, Lin SK, Chiang CP, Yu CH, Kok SH. Gingival squamous cell carcinoma mimicking a dentoalveolar abscess: report of a case. J Endod. 2007:33:177–180.
- Cox D. Introduction to a Diagnostic Approach to Oral and Maxillofacial Pathology: A Programmed Text [iBook]. 2012. Based on: Rovin S, Sabes WR, Howell RM. The Programmed Textbook of Oral Pathology. 2nd ed. Lexington, Kentucky: OP Enterprises; 1973.
- Oral Cancer Foundation. Oral Cancer Facts. Available at: oralcancerfoundation.org. Accessed November 21, 2014.
- Daneshi M, Beylin S, Zemnick C, Emde K. Misdiagnosis of gingival squamous cell carcinoma presenting as a periodontal lesion of the anterior palate. Columbia Dental Review. 2009/2010;14(6):12–15.
- Fitzpatrick SG, Neuman AN, Cohen DM, Bhattacharyya I. The clinical and histologic presentation of gingival squamous cell carcinoma: a study of 519 cases. Oral Surg Oral Med Oral Pathol Oral Radiol. 2012;114:509–515.
- Alkan A, Bulut E, Gunhan O, Ozden B. Oral verrucous carcinoma: a study of 12 cases. Eur J Dent. 2010;4:202–207.
From Dimensions of Dental Hygiene. December 2014;12(12):27–29.

