Manage the Risk
How to provide oral health care safely to patients with a history of myocardial infarction.
This course was published in the July 2011 issue and expires July 2014. The author has no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- Describe the use of functional capacity in determining the risk of treating patients with a recent history of myocardial infarction (MI).
- Identify vital sign values that represent a medical emergency.
- Select the concentration of vasoconstrictor and number of local anesthetic cartridges that can be safely used when a recent MI is reported.
In the past, patients who had experienced myocardial infarction (MI) were advised to delay oral health care for 3 months to 6 months.1 In 2002, the recommended time delay was adjusted by the American College of Cardiology/ American Heart Association (ACC/AHA) Writing Committees to Establish Guidelines for Noncardiac Surgery.2 The updated guidelines specified that oral health care should be avoided for the first 30 days following MI because of the increased risk of an adverse cardiovascular event.2 The ACC/ AHA Writing Committees updated guidelines for noncardiac medical or dental procedures again in 2007. This version kept the 30-day restriction on oral health care and also stipulated that patients who score below a four on a metabolic equivalent (MET) evaluation should not receive oral health care services at all.3
Professional association guidelines are generally based on a systematic review of the evidence. The ACC/AHA Writing Committees performed a formal literature review, weighed the strength of evidence for or against a particular treatment, and included estimates of expected health outcomes where data existed. Patient-specific modifiers, comorbidities, and patient preferences that may influence the choice of particular tests or therapies were considered, as well as the frequency of follow-up and cost-effectiveness of treatment.3
The ACC/AHA guidelines were intended for physicians and nonphysician caregivers involved in the preoperative, operative, and post-operative care of patients undergoing noncardiac surgery or other health-related procedures, such as periodontal treatment. The goal was to provide a framework for considering cardiac risk of noncardiacrelated procedures in a variety of patient and surgical situations among patients with active cardiac conditions (eg, unstable angina, previous MI, decompensated heart failure, significant arrhythmia, and severe valvular disease).3
MI is considered active if it occurred less than 7 days prior and recent if more than 7 days, but less than 1 month, have passed.3 Angina is considered unstable or severe if not relieved by rest.3 Oral procedures of long duration or those expected to pose stress, such as heavy bleeding or pain, pose a risk to patients with active or recent cardiac conditions.
The guidelines recommend health care providers consult with the cardiovascular physician to determine the patient’s status and risk for adverse cardiac events. Written specifically for surgical procedures, including head and neck surgery, the guidelines include a category of “superficial procedures” that could encompass dental hygiene care.
FUNCTIONAL CAPACITY
Functional capacity of the patient, defined as the assessment of an individual’s capacity to perform common daily tasks (Table 1), is an important determinant of whether the provision of oral health care services is safe. The ACC/ AHA guidelines stress that the patient should be able to perform daily tasks equal to at least four METs to be at a low risk for adverse cardiovascular events.3 A MET is the amount of oxygen needed to perform a physical activity.
A patient classified as high risk because of advanced age or diagnosed coronary artery disease, but who is asymptomatic and can walk up two flights of stairs without stopping, needs no further evaluation.3 In contrast, a sedentary patient without a history of cardiovascular disease who cannot perform daily tasks to the four MET level may benefit from a more extensive preoperative evaluation before oral procedures are scheduled. Therefore, during the health history review, questions related to functional capacity should be asked.
RISK LEVEL FOR NONCARDIAC PROCEDURES
|
Various surgical procedures are classified as having low, intermediate, or high risk by the ACC/AHA guidelines. Oral surgery is labeled an intermediate risk procedure (cardiac risk less than 5%), and superficial procedures are noted as low risk (cardiac risk less than 1%).3 Procedures of long duration or that cause excessive blood loss increase cardiac risk. The patient who experienced an MI more than 30 days ago and scored well on a physician-administered
stress test does not indicate poor myocardial function, thus, the likelihood of reinfarction during oral procedures is low. If the patient scores at least a four on the MET level test, periodontal debridement can be scheduled for 5 weeks to 6 weeks after the MI. The decision to proceed with treatment should be made in consultation with the patient’s cardiologist.
The value of withholding emergency or elective surgery during the first 30 days after MI was supported by a 2005 study of sudden death in individuals who experienced MI and left ventricular dysfunction, heart failure, or both.4 This study of 14,609 patients revealed that 7% had a cardiovascular event a median of 180 days after MI, with 903 dying suddenly and 164 resuscitated after cardiac arrest. The risk was highest in the first 30 days following MI, where 19% of all sudden deaths or episodes of cardiac arrest occurred. The rate decreased to 0.14% per month after 2 years. The risk was highest among those with the lowest left ventricular ejection fraction.4 Although most patients cannot identify their level of left ventricular ejection fraction, this information is available from the cardiologist. Lowest left ventricular ejection fraction is a strong predictor of sudden cardiac death.
PHYSICAL ASSESSMENT
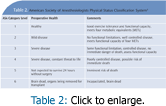
The American Society of Anesthesiologists (ASA) physical status classification system is used to assess patients’ physical well-being and their level of risk (Table 2).5 Patients with status levels one through three can receive oral care. Patients with status level four should not receive dental treatment until their condition is stabilized. The health of patients at status levels five and six would prohibit them from attending a dental appointment.5
A blood pressure value of ≥180/110 mm Hg is a reliable indicator of cardiovascular disease and equates to an ASA four risk classification. Patients at this level should not receive elective oral care, and they should be referred for medical evaluation to control blood pressure before treatment is considered safe.6 Blood pressure less than 90/50 mm Hg is considered a medical emergency.6 Pulse rates greater than 120 beats per minute (bpm) or less than 50 bpm are also considered emergencies.6
CARDIAC INTERVENTIONS AND THERAPIES
A vascular stent is used to treat unstable angina or MI due to thrombosis (blood clots). In February 2007, a new consensus was published about drug-eluting stents and antiplatelet therapy.7 The advisory states that health care providers who perform invasive or surgical procedures (dentists, specialists, dental hygienists) and are concerned about periprocedural and post-procedural bleeding should contact patients’ cardiologists regarding their antiplatelet regimen and risk of excessive bleeding. Because antiplatelet medications are taken in post-stent implantation to minimize the risk of stent thrombosis, the medications should not be discontinued prematurely. The current American Dental Association policy for anAssociationgents following stent placement recommends the continuation of antiplatelet therapy.8
For patients taking antihypertensive medication, blood pressure control should be monitored. Approximately 50% of individuals taking antihypertensive drugs have controlled blood pressure (<140/90 mm Hg) so the clinician should not fail to monitor blood pressure simply because medication is being taken.
LOCAL ANESTHESIA
Most local anesthetic (LA) agents used for periodontal care contain a vasoconstrictor to reduce bleeding during the procedure, while also providing pain control.10 Epinephrine is the vasoconstrictor most commonly used in dentistry. If epinephrine is inadvertently injected into the circulation, the risk of high blood pressure and rapid heart rate increases. In the absence of profound anesthesia, adrenalin-induced tachycardia with increased cardiac workload and oxygen requirements can precipitate coronary ischemia and angina pectoris. In some individuals, the event can progress to cardiac arrest.
Although some patients may fear injections, studies show that even though a transient increase in blood pressure may be produced during LA administration, it decreases when the syringe is removed from the mouth.11 The dose of vasoconstrictor for cardiac-involved patients is no more than two cartridges of 1:100,000 epinephrine (equivalent to 1:20,000 levonordefrin) or four cartridges of 1:200,000 epinephrine.6 For the patient taking a nonselective beta blocker, epinephrine should be limited to one or two cartridges of 1:100,000.12
A study investigated the heart rate and rhythm in individuals with cardiovascular disease who underwent minor oral surgery (tooth extraction, alveoloplasty, biopsy) under local anesthesia (2% lidocaine with 1:100,000 epinephrine or 0.5% bupivacaine with 1:200,000 epinephrine).13 Of the 40 study subjects, 20 were being treated for cardiovascular conditions (hypertension, angina, prior MI, conduction abnormalities, heart failure). Normal doses were given; they ranged from the equivalent of 1.0 ml to 7.9 ml of LA with 1:100,000 epinephrine. Although arrhythmias were detected in 17 subjects, they were benign in character. The incidence of arrhythmia did not differ between subjects with or without cardiovascular disease.
More rhythm disturbances occurred preoperatively and intra-operatively than during LA administration with epinephrine. This was attributed to anticipatory anxiety and the stress of surgery. Consequently, 4.5 ml of a local anesthetic agent with epinephrine 1:100,000 (two cartridges), or equivalent, can be administered safely when the functional capacity is four METs or greater.6 In addition, safe principles of injection technique (use of aspirating syringe, slow injection) should be used.
SUMMARY
Patients with a history of coronary artery disease who show no evidence of cardiac symptoms, are able to meet a four-MET demand during daily activities, and who have a systolic blood pressure reading of less than 180 mm Hg and a diastolic pressure less than 110 mm Hg with a normal pulse and rhythm, can undergo oral care with little to no risk of a cardiovascular event. Adequate pain control is essential to reducing cardiac workload and providing successful treatment.
For patients with a recent history of MI (more than 30 days) who have undergone a recent stress test that does not reveal poor myocardial function, the likelihood of reinfarction during noncardiac surgery or superficial oral procedures is low. With this medical history, delaying periodontal debridement for 4 weeks to 6 weeks after the MI is reasonable. In consultation with the patient’s cardiologist, the clinician should determine that the patient’s functional capacity meets a four-MET level before proceeding with oral procedures. Management of care should include a thorough physical evaluation and assessment of functional capacity, appropriate stress reduction, pain control, and conservative use of a vasoconstrictor if local anesthesia is administered, taking care to prevent intravascular injection.
Oral health care is an integral part of maintaining overall health. Patients with a history of cardiovascular problems can seek out professional dental care and dental professionals should feel confident providing services as long as certain parameters have been met.
REFERENCES
- Eagle KA, Brundage BH, Chaitman BR, et al.Guidelines for perioperative cardiovascular evaluation for noncardiac surgery. Report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. Committee on Perioperative Cardiovascular Evaluation for Noncardiac Surgery. Circulation. 1996;93:1278-1317.
- Eagle KA, Berger PB, Calkins H, et al. ACC/AHA guideline update for perioperative cardiovascular evaluation for noncardiac surgery—executive summary: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee to Update the 1996 Guidelines on Perioperative Cardiovascular Evaluation for Noncardiac Surgery). J Am Coll Cardiol. 2002;39:542-553.
- Fleisher LA, Beckman JA, Brown KA, et al. ACC/AHA 2007 Guidelines on Perioperative Cardiovascular Evaluation and Care for Noncardiac Surgery: A Report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol. 2007;50:159-241.
- Solomon SD, Zelenkofske S, McMurray JJ, et al. Sudden death in patients with myocardial infarction and left ventricular dysfunction, heart failure, or both. N Engl J Med. 2005;352: 2581-2588.
- American Society of Anesthesiologists Physical Status Classification System. 2011. Available at: www.asahq.org/clinical/physicalstatus.htm. Accessed July 1, 2011.
- Pickett F, Terezhalmy G. Dental Drug Reference with Clinical Implications. 2nd Ed. Baltimore, Md: Lippincott Williams & Wilkins; 2010:124-127.
- Grines CL, Bonow RO, Casey DE, et al. Prevention of premature discontinuation of dual antiplatelet therapy in patients with coronary artery stents. A science advisory from the American Heart Association, American College of Cardiology, Society for Cardiovascular Angiography and Interventions, American College of Surgeons, and American Dental Association, with representation from the American College of Physicians. Circulation. 2007;115:813-818.
- ADA Oral Health Topics. Prevent Early Discontinuation of Antiplatelet Medications in Patients with Coronary Artery Stents. Available at: www.ada.org/2959.aspx?currentTab=1. Accessed July 1, 2011.
- Chobanian AV, Bakris GL, Black HR, et al. The seventh report of the joint national committee on prevention, detection, evaluation and treatment of high blood pressure. National Heart, Lung and Blood Institute. J Am Med Assoc. 2003; 289:2560-2578.
- Pickett F, Terezhalmy G. Basic Principles of Pharmacology with Dental Hygiene Applications. Philadelphia: Lippincott Williams & Wilkins. 2009:78.
- Gortzak RAT, Oosting J, Abraham-Inpijn L. Blood pressure response to routine restorative dental treatment with and without local anesthesia. Oral Surg Oral Med Oral Pathol. 1992; 73:677-681.
- Little JW, Falace DA, Miller CS, Rhodus NL. Dental Management of the Medically Compromised Patient. 7th ed. St. Louis: Mosby Elsevier; 2008:DM-5, DM-3, 12.
- Campbell JH, Huizinga PJ, Das SK, et al. Incidence and significance of cardiac arrhythmia in geriatric oral surgery patients. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1996;82: 42-46.
From Dimensions of Dental Hygiene. July 2011; 9(7): 58-61.