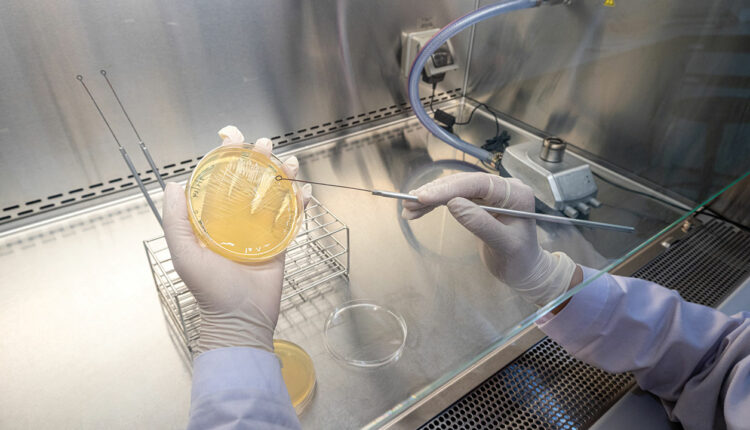
Local Anesthesia as an Antimicrobial Ally
The lesser-known antimicrobial properties of local anesthetics may help dental hygienists to optimize patient care beyond pain management.
This course was published in the June/July 2024 issue and expires July 2027. The authors have no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
AGD Subject Code: 340
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- Describe and differentiate the effectiveness of common local anesthetics in dentistry and their antimicrobial properties.
- Discuss factors that affect the bacterial inhibition of local anesthetics.
- Identify the implications of using local anesthetics for microbial inhibition in dental hygiene.
Local anesthesia has historically been used for analgesia (pain management) but it also has other benefits in dental care, such as the ability of vasoconstrictors to reduce bleeding at the injection site and decreased quantity of local anesthetics (LAs) in the bloodstream.1 A lesser known benefit is the bacterial inhibitory properties of LAs. With most state practice acts now allowing dental hygienists to administer local anesthesia,2 they need to be aware of LAs’ bacterial inhibitory properties that may help prevent and manage dental diseases.
Mechanism of Action
Currently, few studies investigate the mechanism of action of antimicrobial activity of LAs. However, local anesthesia functions by temporarily blocking sensory nerve impulses. The inhibitory effect of LA on bacterial growth may result from the disturbance of the cytoplasmic membrane or bacterial cell wall, leading to cell lysis and depletion of basic cell functioning.3 Depletion of basic cell functioning includes cellular respiration defects, permeability modification, structural changes, and DNA synthesis variation.3 The penetration of bacterial membranes occurs because of the electrostatic binding of anesthetic molecules and polar groups. This relates to the hydrophobic characteristics of anesthetics on the membrane surface.4 This mechanism of action is important because it contributes to the death of bacterial cells which, in turn, inhibits the growth of bacterial colonies in the area that the LA is administered.
Previous studies dating back to 1909 showed that LAs display not only an analgesic effect, but also an antimicrobial effect.5 Since then, studies have tested the antimicrobial effects of different LAs on many bacterial strains. However, limited studies focus on the bacteria found in the oral cavity as described in Table 1. In a study by Pelz et al,6 seven types of LAs were compared on bacterial inhibition efficacy. Articaine, bupivacaine, prilocaine, and lidocaine inhibited bacterial growth of a variety of bacterial strains found in the oral cavity. While all anesthetics tested showed antimicrobial activity, articaine inhibited all strains studied.6
Lidocaine
Since its introduction in 1948, lidocaine has become the most used dental anesthetic.7 Due to its potency, rapid onset, effectiveness, and superior safety profile in comparison to other anesthetics, lidocaine is the gold standard for dental local anesthesia for most dental procedures.7,8 In studies on the antimicrobial effect of lidocaine, it inhibited all strains studied except, Enterococcus faecalis, and Candida albicans.3,6,9-13 However, Morrow and Berry13 reported that topical lidocaine inhibited P. aeruginosa.
Overall, lidocaine resulted in a 73% to 100% decrease in bacterial colonies after exposure compared to controls without anesthetic.13 In a study by Schmidt and Rosenkranz,14 the antimicrobial activity of lidocaine and procaine were examined on 28 different bacterial strains including Streptococcus viridians, which causes dental caries.14,15 In Noda et al,16 the antimicrobial activity of lidocaine and bupivacaine were examined on three bacterial strains: Staphylococcus aureus, S. epidermidis, and P. aeruginosa.16 Both lidocaine and bupivacaine inhibited antimicrobial activity with all three bacterial strains, however, bupivacaine demonstrated greater antimicrobial activity than lidocaine.16
Articaine
Articaine, a newer LA synthesized in 1969, is a popular choice for use in local infiltrations.17 Pelz et al6 found that articaine was the most active LA when testing for bacterial inhibition with a minimal bactericidal concentration that was four times higher than the other LAs tested. It had the most prominent antimicrobial activity and was active against almost all bacteria tested except for P. aeruginosa and E. faecalis. More studies related to the antimicrobial effect of articaine are needed to further investigate its inhibitory properties.
Bupivacaine
Used in dentistry since 1957, bupivacaine is indicated for lengthy procedures due to its long-lasting properties.18,19 Rosenberg and Renkonen20 found that bupivacaine (5%) inhibited all tested bacterial strains except for P. aeruginosa. Grimmond and Brownridge21 demonstrated that bupivacaine’s antimicrobial inhibition increased with growing concentrations. The LA was able to inhibit eight of 10 microbial organisms tested, excluding P. aeruginosa and C. albicans.
In a study by Sakuragi et al,22 bupivacaine reduced the bacterial colony count by 99% after exposure to S. aureus for 24 hours. However, a study by Aydin et al23 showed that bupivacaine had poor antimicrobial effectiveness against S. aureus and other bacterial strains, such as E. coli, P. aeruginosa, and C. albicans. More evidence is needed to reconcile the conflicting claims.
Scope of Practice
Within the past 50 years, the dental hygiene process of care has expanded to include the administration of local anesthesia. Today, 47 states allow dental hygienists to administer local anesthesia.2 Dental hygienists often use LA for procedures such as scaling and root planing and restorative care.
During scaling and root planing, a diverse microbial community develops both supra- and subgingivally. In patients with periodontal diseases, specific strains of bacteria, such as Streptococcus spp. and S. aureus, are present.24,25 Table 1 (page 29) shows the bacteria present in the oral cavity in periodontal health and diseased states. More research is needed to test other bacterial strains in periodontal diseases.
Aside from the antimicrobial effects of local anesthesia by itself, other factors may increase LAs’ antimicrobial properties, such as delivery, greater concentration of LA, longer exposure of the anesthetic to bacteria, temperature, preservatives, and vasoconstrictors.4,9,26 Little evidence is available on the antimicrobial activity of added preservatives and vasoconstrictors; however, studies that did focus on it show conflicting results.6,27
Delivery
The antimicrobial effect of local anesthesia includes other delivery forms such as topical LAs. Sristajaluk et al9 suggested that 10% lidocaine topical spray can reduce bacteria found in the oral cavity by 60% to 95%. Morrow and Berry13 studied topical LA containing lidocaine and benzocaine and found that both lowered the bacterial population by 73% to 100% when compared to not using any LA. Other local anesthesia delivery methods, such as subgingival gels, have not yet been studied for their antimicrobial effects.
Concentration
Studies have shown that greater concentrations of LA increased bacterial inhibition in both Gram-positive and Gram-negative species.10,14 A study by Schmidt and Rosenkranz14 demonstrated that 80.1% of bacterial species were inhibited by 2.0% lidocaine in comparison to 0.5%, 1.0%, and 1.5%.
Parr et al10 found that lidocaine demonstrated a dose-dependent inhibition of bacterial growth for all strains tested. While more evidence on bupivacaine is needed, Rosenburg and Ronkonen20 tested bupivacaine at concentrations of 0.5%, 1.25%, 2.5% and 5%, against several bacterial strains. The 0.5% and 1.25% concentrations had no effect on bacterial inhibition, while the 2.5% concentration inhibited three of 10 bacterial strains, and the 5% concentration inhibited all bacterial strains except P. aeruginosa. Studies have shown efficacy in doses up to 10%.9
Time of Exposure
By increasing the time of exposure, bacterial inhibition was also increased when LA was administered. A study by Begec et al28 tested the antimicrobial effect of lidocaine on three organisms for different intervals. Inhibition was measured at baseline, after 3 hours, and after 6 hours. Lidocaine significantly inhibited the growth of bacteria after 6 hours compared to baseline and after 3 hours.
A study Srisatjaluk et al9 found that the antimicrobial effect of lidocaine topical spray was increased by exposure time. Six bacterial strains were exposed to lidocaine for 1, 2, and 3 minutes. The antimicrobial effect was highest after 3 minutes.
Another study showed lower bacterial colony counts of S. aureus were noted with longer exposure times.22 After 3 hours of exposure to lidocaine, the colony count was reduced by 60%, 70% after 6 hours, and 99% after 24 hours of exposure.
Tustin et al29 found a complete reduction in bacterial colonies after increasing lidocaine’s exposure time to the bacteria.
Temperature
Another factor that boosts the bacterial inhibition of LA is high temperature. In a study by Taki et al,12 bacterial strains were exposed to lidocaine at 37° C (98.6° F) and 40° C (104° F). The bacterial strains exposed to 40° C were more vulnerable to lidocaine than those exposed to 37° C.
James et al30 found that bupivacaine inhibited bacterial growth in S. epidermidis and Corynebacterium spp. at 37° C, but not at room temperature (20° to 22° C or 68° to 72° F) . Sakuragi et al27 showed that 0.5% bupivacaine had a stronger bacterial inhibitory effect at body temperature (37° C) than at room temperature (20° to 22° C).
Preservatives and Vasoconstrictors
The addition of preservatives and/or vasoconstrictors brings mixed results when it comes to their antimicrobial effects. In a study by Pelz et al,6 the antimicrobial activity of preservatives and vasoconstrictive components of LA was tested on methyl-4 hydroxybenzoate (preservative in lidocaine and mepivacaine), sodium disulfite (preservative in lidocaine), and epinephrine (vasoconstrictor in lidocaine).
Epinephrine had no effect on the bacteria tested. The preservatives, on the other hand, caused conflicting results.6 There were two instances in which the microbial count was lower against five bacterial species, indicating that the antimicrobial effect was a result of the preservative. However, there were 21 results where the pure LA showed greater antimicrobial effects compared to the LA with a preservative.
A study by Sakuragi et al27 suggested that the antimicrobial activity shown with bupivacaine may be due to the LA itself and not the added preservative.
Conclusion
While local anesthesia has been used for pain control for decades, these agents offer additional benefits including bacterial inhibition. The reduction of microbial activity is crucial for the prevention and management of oral diseases such as dental caries and periodontal diseases. Dental hygienists must be informed on the specific factors that affect bacterial inhibition. Also, dental hygienists should consider shifting to prioritizing both pain management and microbial inhibition at the injection site by increasing the frequency of LA delivery.
Practical implications may encompass patient education about the added benefits of utilizing LAs for more than just pain management. Specific LAs have been studied for their individual efficacy in control of microbial activity; however, more research is needed to identify the effects on bacteria present in the oral cavity.
References
- Bowen DM, Pieren JA. Darby and Walsh’s Dental Hygiene: Theory and Practice. 5th ed. Philadelphia: Elsevier; 2020.
- American Dental Hygienists’ Association. ADHA Practice Act Overview. Available at: adha.org/wp-content/uploads/2023/05/ADHA-Practice-Act-Overview-5-2023.pdf. Accessed May 6, 2024.
- Razavi BM, Fazly Bazzaz BS. A review and new insights to antimicrobial action of local anesthetics. Eur J Clin Microbiol Infect Dis. 2019;38:991–1002.
- Kaewjiaranai T, Srisatjaluk RL, Sakdajeyont W, Pairuchvej V, Wongsirichat N. The efficiency of topical anesthetics as antimicrobial agents: a review of use in dentistry. J Dent Anesth Pain Med. 2018;18:223–233.
- Jonnesco T. Remarks on general spinal analgesia. Br Med J. 1909;2:1396–1401.
- Pelz K, Wiedmann-Al-Ahmad M, Bogdan C, Otten JE. Analysis of the antimicrobial activity of local anaesthetics used for dental analgesia. J Med Microbiol. 2008;57:88–94.
- Bahar E, Yoon H. Lidocaine: a local anesthetic, its adverse effects and management. Medicina (Kaunas). 2021;57:782.
- Vishal G, Dandriyal R, Indra B N, Singh HP, Chaurasia A. Comparative study of the anaesthetic efficacy of 4% articaine versus 2% lidocaine with adrenaline during extraction of mandibular molars using an inferior alveolar nerve blocking technique. Br J Oral Maxillofac Surg. 2021;59:783–787.
- Srisatjaluk RL, Klongnoi B, Wongsirichat N. Antimicrobial effect of topical local anesthetic spray on oral microflora. J Dent Anesth Pain Med. 2016;16:17–24.
- Parr AM, Zoutman DE, Davidson JS. Antimicrobial activity of lidocaine against bacteria associated with nosocomial wound infection. Ann Plast Surg. 1999;43:239-245.
- Liu K, Ye L, Sun W, Hao L, Lou Y, Chen J. Does use of lidocaine affect culture of synovial fluid obtained to diagnose perioprosthetic joint infection? An in vitro study. Med Sci Monit. 2018;24:448-452.
- Taki Y, Seki K, Ikigai H, et al. Effect of temperature on antibacterial activity of lidocaine to Staphylococcus aureus and Pseudomonas aeruginosa. Microbiol Immunol. 1988;32:429–434.
- Morrow M, Berry C. Antimicrobial properties of topical anesthetic liquids. Anesth Prog. 1988;35:9–13.
- Schmidt RM, Rosenkranz HS. Antimicrobial activity of local anesthetics: lidocaine and procaine. J Infect Dis. 1970;12:597–607.
- Ahmed NM, Tariq P, Naim A. Viridans group streptococci and dental caries: an overview. Int J Biol Biotech. 2023;20:3-16.
- Noda H, Saionji K, Miyazaki T. Antibacterial activity of local anesthetics. Masui. 1990;39:994-1001.
- Luo W, Zheng K, Kuang H, Li Z, Wang J, Mei J. The potential of articaine as new generation of local anesthesia in dental clinics: areview. Medicine (Baltimore). 2022 ;101:e32089.
- Shafiei FT, McAllister RK, Lopez J. Bupivacaine. Treasure Island, Florida: StatPearls; 2023.
- Pandey C, Speedie A, Jaiswal R, Lanjewar S, Dondulkar Y. Role of bupivacaine in dentistry. J Int Oral Health. 2019;6:53-55.
- Rosenberg PH, Renkonen OV. Antimicrobial activity of bupivacaine and morphine. Anesthesiology. 1985;62:178-179.
- Grimmond TR, Brownridge P. Antimicrobial activity of bupivacaine and pethidine. Anaesth Intensive Care. 1986;14:418–420.
- Sakuragi T, Ishino H, Dan K. Bacterial activity of clinically used local anesthetics on Staphylococcus aureus. Reg Anesth. 1996;:239–242.
- Aydin ON, Eyigort M, Aydin N. Antimicrobial activity of ropivacaine and other local anaesthetics. Eur J Anaesthesiol. 2001;18:68-694.
- Dani S, Prabhu A, Chaitra KR, Desai NC, Patil SR, Rajeev R. Assessment of Streptococcus mutans in healthy versus gingivitis and chronic periodontitis: A clinico-microbiological study. Contemp Clin Dent. 2016;7:529–534.
- Rams TE, Feik D, Slots J. Staphylococci in human periodontal diseases. Oral Microbiol Immunol. 1990;5:29–32.
- Morrow ME, Berry CW. Antimicrobial properties of topical anesthetic liquids containing lidocaine or benzocaine. Anesth Prog. 1988;35:9-13.
- Sakuragi T, Ishino Ei, Dan K. Bactericidal activity of 0.5 % bupivacaine with preservatives on microorganisms in the human skin flora. Reg Anesth. 1997;22:178–184.
- Begec Z, Gulhas N, Toprak HI, Yetkin G, Kuzucu C, Ersoy MO. Comparison of the antibacterial activity of lidocaine 1% versus alkalinized lidocaine in vitro. Curr Ther Res Clin Exp. 2007;68:242–248.
- Tustin A, Kim SJ, Chomsky A, Hubbard GB, Sheng J. Antibacterial properties of 2% lidocaine and reduced rate of endophthalmitis after intravitreal injection. Retina. 2014;34:935–942.
- James FM, George RH, Naiem H, White GJ. Bacteriologic aspects of epidural analgesia. Anesth Analg. 1976;55:187–190.
- McCormack MG, Smith AJ, Akram AN, Jackson M, Robertson D, Edwards G. Staphylococcus aureus and the oral cavity: an overlooked source of carriage and infection? Am J Infect Control. 2015;43:35–37.
- Haslam DB, St. Geme JW. Viridians Streptococci, Abiotrophia and granulicatella species, and Streptococcus bovis group. Principles and Practice of Pediatric Infectious Disease. 6th ed. Philadelphia: Elsevier; 2023:748–751.
- Rivas Caldas R, Le Gall F, Revert K, et al. Pseudomonas aeruginosa and periodontal pathogens in the oral cavity and lungs of cystic fibrosis patients: a case-control study. J Clin Microbiol. 2015;53:1898–1907.
From Dimensions of Dental Hygiene. June/July 2024; 22(4):28-31



