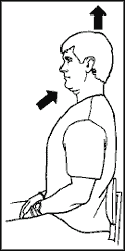
Improving Your Musculoskeletal Health
Postural, positioning, and stretching strategies for career longevity.
Day in and day out you educate your patients on the importance of prevention in their oral health regimen—brush, floss, and regular check-ups—because you know that structural damage to teeth or tissues can occur long before they actually experience pain. But what prevention strategies are you using to ensure your own musculoskeletal health and career longevity?
Work-related pain has become so endemic to dental hygiene that many hygienists tend to passively accept the inevitable partnership between their work and musculoskeletal pain. Indeed, a recent study revealed that five out of six hygienists experienced discomfort or pain in a 12-month period.1 Compared to the average woman worker, female dental professionals experience two to four times more musculoskeletal pain.2The neck and shoulders are the most problematic areas among hygienists.1-4
MULTIPLE RISK FACTORS
If you recently purchased a fine ergonomic chair or loupes, congratulations! You have taken the initiative and moved one step closer to practicing in comfort and preventing injuries.
What hygienists must realize is that effective injury prevention in dentistry involves addressing multiple risk factors.5-7 Just as you wouldn’t rely on root planing or antibiotics alone to prevent periodontal disease, you should not expect one strategy to effectively prevent work-related pain or injuries. Numerous factors contribute to work-related pain:
- Prolonged, awkward postures,
- Forceful, repetitive movements,
- Poor flexibility,
- Improper operator and patient positioning,
- Weak postural muscles,
- Poor equipment,
- Improper adjustment of ergonomic equipment,
- Infrequent breaks, and
- Stress.
MUSCULOSKELETAL DISORDERS
Prolonged exposure to these risk factors can result in painful musculoskeletal disorders (MSDs). Three of the most commonly diagnosed neck and shoulder disorders among hygienists include:1
- Tension neck syndrome (most common)
- Trapezius myalgia
- Thoracic outlet syndrome
Symptoms of tension neck syndrome include pain, tenderness, and stiffness in the neck and shoulder musculature, often with muscle spasms. Pain may radiate between the shoulder blades, down the arms, or up into the occiput. Headache is also a common symptom. Trapezius myalgia involves pain, tenderness, and trigger points in the upper trapezius muscle. Thoracic outlet syndrome is a neurovascular disorder, involving compression of the subclavian artery or brachial plexus nerve trunks. Symptoms include pain in the fingers, hand, arm, or shoulder. Numbness, weakness, coldness, and discoloration of the fingers are also symptoms. Thoracic outlet symptoms can easily be confused with a more common disorder of the hand/wrist—carpal tunnel syndrome. A physician should be consulted whenever neurological symptoms such as numbness, tingling, or weakness are experienced.
One word of caution when seeking treatment for pain or MSDs: therapies aimed at immediate relief usually yield temporary results. When the hygienist returns to work, the same postural, positioning, and ergonomic issues that led to the problem in the first place remain unchanged. Therefore, implement prevention and treatment first or concurrently with other therapies.
.gif)
POSTURE AND YOUR HEALTH
The spine is composed of three movable curves: the cervical lordosis, thoracic kyphosis, and lumbar lordosis. Preserving these curves is imperative in preventing neck and shoulder, as well as low back pain. When the curves are all present and centered along the line of gravity, the spine is supported by the bony vertebrae, and very little stress is placed on the muscle, ligaments, and surrounding soft tissue (Figure 1).
If, however, the low back curve is lost (Figure 2), the head projects forward, and the spine must depend largely on muscles for support. Hence, proper posture and healthy neck and shoulders are largely dependent on proper posture of the low back (ie, maintaining the low back curve). Maintaining these essential spinal curves is key to preventing neck and shoulder pain and injury.8
|
|
|
|
Figure 1. Posture where spinal curves are present and centered. |
Figure 2. Posture where low back curve is lost. |
POSTURAL STRATEGIES IN THE OPERATORY
Working with forward head posture (greater than 20°) is connected to neck pain and headaches.9 It contributes to such MSDs as tension neck syndrome and trapezius myalgia by causing sustained contraction and ischemia in the upper trapezius and levator scapula muscles. It can also result in thoracic outlet syndrome by creating tightness in the anterior neck muscles, weakness of the shoulder girdle stabilizers, and rounded shoulder posture resulting in compression of neurovascular structures. Be vigilant in the operatory to avoid harmful postures.
Neck and shoulder posture. Optimal neck and shoulder posture is ears-over-shoulders from a side view. An effective means to maintain the neck curve in dentistry is with magnification (Figure 1). Try several different types and work with the manufacturer to adjust the scopes to accommodate your optimal working posture. Poorly adjusted scopes can cause every bit as much neck pain as no scopes at all.10
Lumbar support. When the low back curve flattens, the head goes forward (Figure 2). Ensure that your chair is properly positioned to support your low back and maintain the lumbar lordosis. Check your operator chair to see if the lumbar support will adjust forward. Many hygienists don’t realize this feature is on most operator chairs.
Chin tuck and downward squeeze (Figures 3 and 4). These easy chairside exercises strengthen the neck and shoulder muscles, facilitate optimal operator posture, and can decrease neck and shoulder pain.11 Perform these frequently throughout the workday. Remember to never perform exercises in a painful range.
|
|
|
|
Figure 3. Chin tuck: sit tall and touch tips of fingers together behind lower neck (not shown) to maintain neck curve throughout exercise. Relax arms and elbows. Keeping eyes and chin level, pull chin up and backward. Hold five counts. Repeat five times. |
Figure 4. Downward squeeze: perform chin tuck and hold throughout exercise. Position fingers pointing up and palms forward. Roll shoulders back, squeezing shoulder blades together and downward. Hold one long breath cycle. Repeat five times. |
POSTURAL STRATEGIES AT HOME
Perform a simple postural check by asking someone to look at your postural alignment from the side. Stand relaxed, with arms at sides, in your everyday standing posture. You should be able to draw an imaginary line straight through the ear, shoulder, hip, and ankle. Check for excessive curvature of the low back, forward head, rounded shoulders, or protruding abdomen. If your body does not line up, chances are unnecessary strain is being placed on spinal muscles, ligaments, and joints. Postural awareness and strengthening exercise can help correct unbalanced posture.
Ideal standing posture:
• Stand with arms relaxed at sides, lift your chest toward the ceiling, and perform a chin tuck.
• Pull your tailbone forward underneath you, flattening your low back, and contracting your abdominals. Now push your tailbone backward, arching your low back. Alternate between these two postures several times. Now find the position that is halfway between and stabilize the spine by contracting your abdominals: pull your navel toward your spine (as though you were zipping up a pair of tight jeans).
• Roll your arms outward until palms face forward while rolling your shoulders backward and down.
• Without moving your shoulders, let your palms relax against the sides of your thighs, thumbs pointing forward.
Did you notice how easily your shoulders unrounded with rotating arms outward? You are now in an anatomically neutral posture, which you should strive to maintain with all activity. Remember to contract your abdominal muscles throughout the day to maintain this ideal posture. Your abs will become stronger, and this new posture will eventually become habit.
In order to develop sufficient strength in the postural muscles to maintain optimal postures throughout the workday, specific strengthening of the postural muscles of the trunk (transverse and oblique abdominals and multifidus muscles), interscapular muscles (primarily middle and lower trapezius), and specific muscles of the rotator cuff should be performed.8 Hygienists must have strong postural muscles of the trunk and shoulders to stabilize the body so the arms and hands can efficiently perform detailed tasks. When these postural muscles become fatigued, hygienists can slump into less than optimal posture, negatively affecting shoulder, arm, and hand position and setting the stage for injury.7
.jpg) |
Figure 5. Deep abdominal exercise: lying on your back, contract your navel toward the spine, holding throughout the exercise. Do not let your back arch up off the floor. Slowly alternate legs, extending one leg, then the other. Perform 10-20 repetitions as able. |
.jpg) |
Figure 6. Pointer dog exercise: position yourself on hands and knees. Contract the abdominals by pulling the navel toward the ceiling and hold throughout. Slowly extend one arm, hold five counts, then the other. Extend the legs, holding each for five counts. Perform five to 10 repetitions. |
There are dozens of exercises to strengthen these postural muscles. Make sure your program includes strengthening the transverse abdominal muscles (Figure 5), which stabilize the low back to help maintain the low back curve. The pointer dog exercise (Figure 6) strengthens most of the postural trunk and shoulder muscles in one exercise.
Exercising the neck, upper back, and shoulder muscles (especially strength training) reduces work-related neck and shoulder pain.11 Additionally, one study suggested that women dental operators who have poor shoulder muscle endurance may be more susceptible to pain in the neck and shoulders.12 Several resources provide instruction on using elastic exercise bands or free weights to strengthen these muscles easily at home.13-15
Exercise programs focused on postural strengthening, such as the Pilates method, are highly recommended for dental professionals. Additionally, the Swiss exercise ball provides a safe and effective means for mobilizing the spine, stretching muscles, and, by providing an unstable base of support, exercises the body’s deep postural stabilization muscles. Check into resources that focus on this specific work.15-18 As with all exercise, consult a physician before beginning a new exercise program.
POSITIONING STRATEGIES
There may be certain operatory features that hygienists can’t change like patient chairs and fixed bracket trays. The following strategies can be used in almost every setting and can mean the difference between no pain and pain at the end of the day.
Stay close to your patient. The patient’s head should be nearly against the operator’s abdomen, which can be problematic because of modesty issues or the inability to position knees under patient chair due to thick upper back and headrests. If you can’t gain close proximity to the patient, change positions or stand.
Correct height. Probably one of the biggest contributing factors to neck and shoulder pain in operatories is positioning the patient too high. This causes prolonged “chicken winging” of the arms. Operator forearms should be about parallel to the floor with upper arm relaxed against the trunk. When the operator and patient are optimally positioned in this manner, magnification is usually required due to the increased working distance.
Armrests. Armrests reduce strain in the upper trapezius muscle and allow the muscle to be replenished with oxygen and nutrients.19 By providing an elbow fulcrum from which to operate, armrests also improve instrument stability. Numerous types of armrests are available, however, be careful not to adjust armrests too far forward, as this encourages rounded shoulders.
Move. Although the benefits of good ergonomic equipment and operatory layout are numerous, certain layouts can be conducive to operating within a confined area. It is important to “work the clock” from the 8:00 to 3:00 positions in order to shift the workload from one group of neck and shoulder muscles to another. If operatories are too small or have fixed rear delivery systems that restrict the zone where the operator can work, it becomes imperative to perform chairside directional stretching throughout the day to prevent muscle imbalances.
 |
|
|
Figure 8. Tools for self-treatment of trigger points. |
|
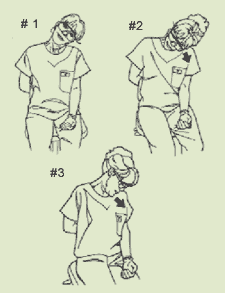
| Figure 7. Neck stretch sequence: anchor one hand behind your back or chair. Slowly bring the ear to shoulder (#1); slowly bring ear to armpit (#2), hold 2-4 breath cycles; and slowly bring chin to armpit (#3), hold 2-4 seconds. |
STRETCHING STRATEGIES
The body is designed to accommodate poor or awkward postures for brief periods of time. It is not designed for prolonged, static postures,20 as is so commonly seen in the hygiene profession.
Chairside stretching provides a break from these static postures and can prevent pain.21 In ideal postures, the deep postural stabilizing muscles are still statically contracted. When these muscles fatigue, poor posture can result, and it is back to the “hunched” posture again. Stretching provides a break for and replenishes these muscles with oxygen and nutrients.
It is not always possible to maintain “ideal” postures throughout the workday. Intermittently, when hygienists do find themselves in awkward postures, they are usually bent or leaning repeatedly in the same direction, which can result in tightness on one side of the body over the other. Directional stretching reverses the operator position, thereby improving flexibility and decreasing the likelihood of painful muscle imbalances, ischemic muscles, or trigger points.18
Stretches should be performed frequently throughout the day, both in and out of the operatory. If breaks are too far apart, the rate of damage will exceed rate of repair, ultimately resulting in breakdown of tissue. Frequent and brief micropauses are more beneficial than lengthy infrequent pauses.22
How to stretch safely:
- Breathe in deeply.
- Exhale slowly while moving into the stretch.
- Move into each stretch slowly (3-5 seconds) up to a point of mild discomfort.
- Hold the stretch for 10-20 seconds.
- Slowly release the stretch—come back to neutral position. Repeat.
- NEVER STRETCH IN A PAINFUL RANGE!
Perform the stretches (Figure 7) in both directions and determine which side is tightest. Perform the stretch primarily toward the tightest side throughout the workday.
TRIGGER POINTS
Oftentimes, hygienists experience pain that is not relieved with stretching, but is actually worsened by it. This pain may be caused by a small contraction inside the muscle tissue known as a trigger point, which feels like a hard knot. Trigger points neither allow the muscle to contract or relax, thereby effectively decreasing flexibility and range of motion. When firm pressure is applied, trigger points usually refer pain to another area, but pain may be felt locally as well. Although professional massage is most effective in treating trigger points, it is important to release the trigger point as soon as possible to prevent ischemia of muscle tissue. Operators can learn to manage upper back and neck pain caused by trigger points with self-treatment interventions.22
- Place a tennis ball or smaller hard rubber ball between your back and the wall. For harder to reach areas, use a Thera Cane (Figure 8) (www.theracane.com). Find the trigger point.
- Apply deep pressure for five slow counts, maintaining pressure till a release is felt, or alternate between deep pressure and slow massage for 1 minute per trigger point.
- Aim at a pain level that “hurts so good” (about six to seven on a scale of one to 10).
- Perform a gentle stretch to the area, holding 30-60 seconds.
- Treat the trigger point at least three to five times per day, or until pain decreases to a level of one to two on the pain scale.
The Trigger Point Therapy Workbook24 is an excellent resource for further study.
WHERE TO START?
Remember, your first line of defense when dealing with neck and shoulder pain is posture. Begin with the postural techniques, and then once they become habit, gradually add the other strategies.
As with periodontal disease, prevention of neck and shoulder problems is far easier than treatment of the musculoskeletal disorder that results once structural changes have occurred. Your dental hygiene career does not have to be plagued by pain and discomfort. You can learn to manage, control, and prevent work-related pain.
References
- Akesson I, Johnsson B, Rylander L, Moritz U, Skerfving S. Musculoskeletal disorders among female dental personnel—clinical examination and a 5-year follow-up study of symptoms. Int Arch Occup Environ Health. 1999;72:395-403.
- Akesson I, Schutz A, Horstmann V, Skerfving S, Moritz U. Musculoskeletal symptoms among dental personnel—lack of association with mercury and selenium status, overweight and smoking. Swed Dent J. 2000;24:23-28.
- Oberg T, Oberg U. Musculoskeletal complaints in dental hygiene: a survey study from a Swedish county. J Dent Hyg. 1993;67:257-261.
- Lalumandier JA, McPhee SD, Parrott CB, Vendemia M. Musculoskeletal pain: prevalence, prevention, and differences among dental office personnel. Gen Dent. 2001;49(2):160-166.
- Westgaard RH. Effects of physical and mental stressors on muscle pain. Scand J Work Environ Health. 1999;25:19-24.
- Lehto TU, Helenius HY, Alaranta HT. Musculoskeletal symptoms of dentists assessed by a multidisciplinary approach. Community Dent Oral Epidemiol. 1991;19:38-44.
- Murphy D. Ergonomics and the Dental Care Worker. Washington, DC: American Public Health Association; 1998:113-128,191, 344,350.
- Saunders HD, Saunders R. Evaluation, Treatment and Prevention of Musculoskeletal Disorders, Vol 1. 3rd ed. Chaska, Minn: Saunders Group; 1995:48,72,323-341.
- Ariens GA, Bongers PM, Douwes M, et al. Are neck flexion, neck rotation, and sitting at work risk factors for neck pain? Results of a prospective cohort study. Occup Environ Med. 2001;58(3):200-207.
- Chang BJ. Ergonomic benefits of surgical telescope systems: selection guidelines. J Calif Dent Assoc. 2002; 30:2:161-169.
- Vasseljen O Jr, Johansen BM, Westgaard RH. The effect of pain reduction on perceived tension and EMG-recorded trapezius muscle activity in workers with shoulder and neck pain. Scand J Rehabil Med. 1995;27(4):243-252.
- Rundcrantz B, Johnsson B, Moritz U. Occupational cervico-brachial disorders among dentists. Analysis of ergonomics and locomotor functions. Swed Dent J. 1991; 15:105-115.
- Creager CC. Therapeutic Exercises Using Resistive Bands. Berthoud, Colo: Executive Physical Therapy; 1998:1-366.
- Jesperson M, Potvin A, Jesperson M. The Great Stretch Tubing Handbook. Blaine, Wash: Fitness Products; 2000:1-64.
- Valachi B, Valachi K. Smart Moves for Dental Professionals on the Ball [videotape]. Portland, Ore: Posturedontics; 2002.
- Craig C. Pilates on the Ball. Rochester, Vt: Healing Arts Press; 2001:1-178.
- Posner-Mayer J. Swiss Ball Applications for Orthopedic and Sports Medicine. Denver: Ball Dynamics International; 1995:83-89, 109-120, 168-181.
- Valachi K, Valachi B. Position Yourself in 2003. Trends in Exercise and Injury Prevention. Dental Products Report. 2003;1:58-64.
- Parsell DE, Weber MD, Anderson BC, Cobb GW Jr. Evaluation of ergonomic dental stools through clinical simulation. Gen Dent. 2000;48(4):440-444.
- Sjogaard G. Intramuscular changes during long-term contraction. In: The Ergonomics of Working Postures: Models, Methods and Cases. Philadelphia: Taylor & Francis; 1986:136-143.
- McArdle W, Katch F, Katch V. Exercise Physiology: Energy, Nutrition and Human Performance. 3rd ed. Malvern, Pa: Lea & Febiger; 1991:488-489.
- Karwowski W, Marras W. The Occupational Ergonomics Handbook. Boca Raton, Fla: CRC Press LLC; 1999:256,835, 925.
- Hanten WP, Olson SL, Butts NL, Nowicki AL. Effectiveness of a home program of ischemic pressure followed by sustained stretch for treatment of myofascial trigger points. Phys Ther. 2000;80(10):997-1003.
- Davies C. The Trigger Point Therapy Workbook. Oakland, Calif: New Harbinger Publications Inc; 2001:15-207.
From Dimensions of Dental Hygiene. June / July 2003;1(3):20-22, 24, 26.

.jpg)
.jpg)