 © MICHAELA NGUYEN, RDH, BSDH, MS
© MICHAELA NGUYEN, RDH, BSDH, MS
Improve Nonsurgical Periodontal Therapy With Appropriate Instrument Choice
Mini- and micro-mini-bladed Gracey curets enable access and maximize calculus removal.
Successful nonsurgical periodontal therapy depends on eliminating biofilm and calculus to prevent the progression of periodontal diseases.1 Incomplete removal of these deposits enables biofilm to accumulate, causing inflammation that may lead to the destruction of surrounding tissue and bone. This is especially true for difficult-to-reach tooth surfaces with challenging root morphology. Calculus deposits left behind can lead to periodontal pockets that are laborious to manage.2 As such, securing access and removing all deposits are key to successful outcomes.
Instrument selection is integral to accessing difficult root morphology and reaching the base of the pocket. Assessing the tissue tone, clinical attachment loss, root morphology, and accessibility determines which instruments are suitable to accomplish complete root debridement. Terminal shank length and instrument blade thickness should be considered in order to access the pocket and tissue. The use of standard thick- and large-bladed instruments can cause trauma to the soft tissue when forced into the pocket. If the blade is too thick or too long to safely insert subgingivally, accessing the base of a pocket becomes impossible.
Mini-bladed Gracey curets and micro-mini-bladed Gracey curets are good alternatives to the standard Gracey instrument. Their thinner blades provide access to the pocket and ensure debridement for this type of tissue without trauma. A recent microscopic analysis study showed that mini-bladed, area-specific curets were optimal for root instrumentation in terms of both calculus removal and surface alterations when compared to standard area-specific and power instruments.3
DESIGN CHARACTERISTICS
Both mini- and micro-mini-bladed Gracey curet designs have a terminal shank 3 mm longer than the standard Gracey curet for deep access into pockets. In addition, the blade on the mini-bladed Gracey curet is 50% smaller in length and width than that of a standard Gracey. The micro-mini-bladed curets are 20% smaller than the mini-bladed Gracey curet, therefore, 70% smaller in length and width than a standard Gracey curet blade (Figure 1). The shorter, thinner blades and extended shanks enable them to reach deeper and improve access in periodontal pockets than any other hand instruments, while also reducing tissue distension and easing subgingival insertion.
Mini- and micro-mini-bladed Gracey curets were developed to adapt well to contours of the tooth including the cementoenamel junctions (CEJ), line angles, root depressions, concavities, furcations, and narrow pocketing.4 In the past, the only solution to access these difficult areas was to use the Gracey curet with a toe-down horizontal stroke. Mini- and micro-mini-bladed Gracey curet instruments now allow access to areas that previously were extremely challenging to reach with complete root coverage using multidirectional strokes.

micro-mini-bladed Gracey curets.© Michaela Nguyen, RDH, BSDH, MS
INSTRUMENT USE
Both mini- and micro-mini-bladed Gracey curets are particularly useful in debriding root and tooth surfaces in areas of narrow, deep periodontal pocketing. It is physically impossible to insert a long, regular-sized blade directly into the deepest area of a pocket in a transverse position using vertical strokes.5 In addition, the use of mini- and micro-mini-bladed Gracey curets eases the challenge of accessing the interradicular root furcation surfaces.
In comparison to modified slim ultrasonic insert/tips, mini- and micro-mini-bladed Gracey curets allow for unprecedented access and effectiveness for root debridement because they provide excellent adaptation with better tactile sensitivity in areas of line angles; furcations; and narrow, curved, and facial or palatal root surfaces, especially when tissue is tight.4
STROKE DIRECTION
Vertical strokes with mini- or micro-mini-bladed Gracey curets are generally used straight with the toe directed in the mesial or distal direction. These types of strokes are effective on rounded concavities going into and out of root depressions and furcations, and around line angles under the CEJ. Oblique or horizontal strokes can be used; however, due to the shortness of the blade, these strokes may not extend far enough subgingivally unless tissue is retractable.4
Horizontal strokes with the toe directed toward the junctional epithelium with mini- or micro-mini-bladed Gracey curets are most effective when used at the CEJ or in developmental depressions just below it.4 However, due to the nature of a shorter blade, using a horizontal stroke is difficult to reach deep periodontal pockets with developmental depressions.
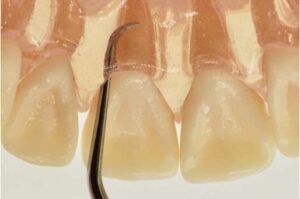
along the palatal surface of maxillary anterior roots with vertical strokes. © Michaela Nguyen, RDH, BSDH, MS
PALATALS OF MAXILLARY ANTERIOR TEETH
Palatogingival grooves are developmental anomalies involving lingual surfaces of the maxillary incisors. They are inconspicuous, funnel-shaped, and extend for varying distances on the root surface.6 Without proper instrumentation, these areas can encourage plaque adherence, potentially causing periodontal lesions. In addition to developmental anomalies, the narrow anatomy of the anterior teeth make it challenging to find instruments that fit tight tissue.
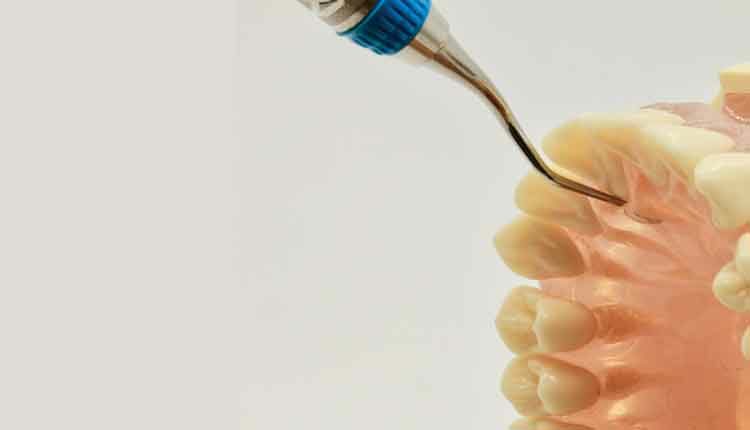
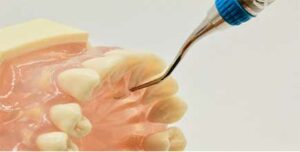
Mini- and micro-mini-bladed Gracey curets can be inserted to the base of a narrow, tight anterior palatal pocket along the midline of the tooth using a straight vertical stroke (Figure 2). This can be done with very straight curets such as mini- or micro-mini-bladed Gracey 1/2, 5/6, or 7/8 curet using an opposite-arch or same-arch hand rest. With a same-arch fulcrum, the bend of the shank of mini- and micro-mini-bladed Gracey 13/14 curets are superior for deep periodontal pockets, recession, and palatal version access. The upper shank of the 13/14 Gracey design extends in the palatal direction to allow the terminal shank to align with the palatal surfaces of the root (Figure 3).
DEEP PALATAL SURFACES OF MAXILLARY MOLARS
The root morphology of maxillary molars includes concavities leading into the furcation areas and a palatal root that is usually convex; however, it could contain shallow concavities.7 The maxillary molars have long and bulky palatal roots, and a deep palatal developmental groove may be present, making it difficult to instrument with traditional instruments.
To best adapt to these surfaces, a mini- or micro-mini-bladed Gracey 7/8 or 13/14 curet can be inserted along the midline of the tooth with vertical strokes. The toe is directed toward the distal surfaces. Roll the instrument blade when entering toward the distal surface to adapt and cover the distolingual line angles. Be sure to adapt the terminal shank to the surface being scaled. This technique can be accomplished at a 2 o’clock clinician position with the patient chin-up and a same-arch fulcrum (Figure 4).
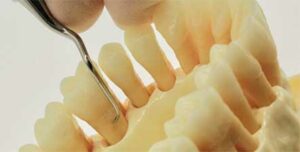
the palatal depression at a 2 o’clock clinician position. Vertical strokes are implemented.© Michaela Nguyen, RDH, BSDH, MS
MAXILLARY BUCCAL FURCATIONS
Furcations of the maxillary molars are more often periodontally involved than those of the mandibular molars. Buccal furcations of the maxillary first molars are the most frequently affected, followed by the mesial and distal furcations.8 Therefore, instruments that adapt well into furcations are vital to prevent periodontal diseases in high-risk root surfaces.
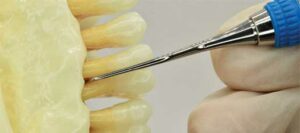
distobuccal root of buccal furcation for maxillary right first molar with an opposite-arch fulcrum. © Michaela Nguyen, RDH, BSDH, MS
A single or combination of mini- or micro-mini-bladed Gracey curets can debride all aspects of a buccal furcation of maxillary molars. A straight shanked micro-mini-bladed Gracey 1/2 or mini-bladed Gracey 1/2 , 5/6, or 7/8 curet can be used with vertical strokes to scale both mesial and distal surfaces of the root surfaces of the buccal furcation. Ideally, an extraoral fulcrum should be used in order to extend the instrument for proper angulation, especially if the furcation is periodontally involved (Figure 5 and Figure 6).
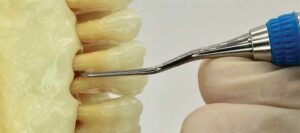
For buccal furcations of the second and third molars, a combination of the mini- or micro-mini-bladed 11/12 and 13/14 Gracey curets should be used to improve angulation and adaptation when instrumenting more posteriorly with intraoral, same-arch, or extraoral opposite-arch fulcrums. To finish scaling a buccal furcation, the roof or entrance of the furcation can be lightly scaled with a mini- or micro-mini-bladed Gracey 13/14 curet utilizing a same-arch fulcrum (Figure 7). Adapt the terminal shank with the long axis of the buccal surface of the molar and swing the handle slightly toward the buccal surface so the angle of the toe is open to activate a short finger-flexing scooping-out technique of the soft and hard deposits that reside on the floor of the furcation. More tenacious deposits may require an adjustment from light- to moderate- scooping strokes.
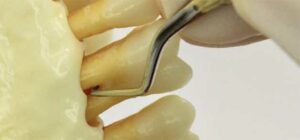
the buccal furcation of the maxillary right first molar by swinging out the handle slightly with a same-arch, palm-down fulcrum.© Michaela Nguyen, RDH, BSDH, MS
CONCLUSION
The mini- and micro-mini-bladed Gracey curets enable access in areas previously too difficult to reach with standard instruments. These mini-bladed curets also come in both finishing and rigid designs, and can be used for both calculus removal and light finishing scaling for periodontally involved patients—especially those with tight pockets and concavities. Mini-bladed curets also provide an alternative to finishing with slim power instruments. These Gracey curets should be considered when treating and/or maintaining periodontally involved patients with depressions, deep pockets, and tight tissue.
REFERENCES
- Zappa U, Smith B, Simona C, Case D, Kim W. Root substance removal by scaling and root planing J Periodontol. 1991;62:750–754.
- Leknes K, Lie T, Boe O, Selvig K. A correlation study of inflammatory cell mobilization in response to subgingival microbial colonization. J Periodontol. 1997;61:67–72.
- Profili F, Sparabombe S, Smith AT, D’Isidoro O, Quaranta A. The effect of miniaturized manual versus mechanical instruments on calculus removal and root surface characteristics: an in vitro light microscopic study. Clin Exp Dent Res. 2019;5:519–527.
- Newman M, Takei H, Klokkevold P, Carranza F. Newman and Carranza’s Clinical Periodontology. 13th ed. St. Louis: Elsevier/Saunders; 2019.
- Bowen DM, Pieren JA. In: Dental Hygiene: Theory and Practice. Darby M, Walsh M, eds. 5th ed. St. Louis: Elsevier; 2019.
- Karunakaran J, Fenn S, Jayaprakash N, Ragavendran N. Successful surgical management of palatogingival groove using platelet-rich fibrin and guided tissue regeneration: a novel approach. J Pharm Bioallied Sci. 2017;9(Suppl 1):S268–S273.
- Hodges K. Hand instrumentation of first molar teeth. Dimensions of Dental Hygiene. 2018;16(5):16–18.
- Cattabriga M, Pedrazzoli V, Wilson TG. The conservative approach in the treatment of furcation lesions. Periodontol 2000. 2000;22:133–153.
From Dimensions of Dental Hygiene. February 2021;19(2):16-18, 21.

