
Exploring the Connection
The relationship between respiratory diseases and oral health.
This course was published in the October 2009 issue and expires October 2012. The author has no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- Explain the rationale for identifying and reducing the risk factors for respiratory diseases.
- Describe the pathogenesis of the link between periodontitis and respiratory disease.
- Explain the relationship between oral health and respiratory diseases, including pneumonia, chronic obstructive pulmonary disease, and asthma.
- Identify the preventive oral health care measures to prevent and/or reduce the severity of respiratory diseases.
- Discuss the role of the oral health professional in clinical care, community instruction, and interprofessional communication.
More than 35 million Americans suffer from some type of respiratory disease—ranging from acute pulmonary infections, such as pneumonia, to chronic lung conditions, such as chronic obstructive pulmonary disease (COPD) and asthma.1 When all lung diseases are combined, they account for one in every six deaths in the United States, making respiratory diseases the third most common cause of death among Americans.1
Since the publication of Oral Health In America: A Report of the Surgeon General in 2000 and the National Call to Action to Promote Oral Health in 2003, there has been considerable interest in exploring the potential connections between a wide variety of systemic conditions and oral health.2,3 Although the link between respiratory diseases and oral health has not received the publicity of other health conditions, a substantial and growing body of literature shows an association between oral health and specific respiratory diseases. For example, two recent systematic reviews of the literature document an association between pneumonia and poor oral health status.4,5
Research shows that intensive oral hygiene care coupled with professional oral care can be effective at reducing both the occurrence and severity of certain respiratory diseases.4,5 For example, a systematic review by Sjogren et al identified that frequent toothbrushing and the pre-operative use of 0.12% or 0.2% chlorhexidine mouthrinse or gel reduced nosocomial respiratory tract infections.6 Thus, dental hygiene care has the potential to reduce both the initiation and severity of common respiratory infections when dental hygienists complete a thorough oral health assessment and identify and address threats to good oral health in their patients most at risk for respiratory diseases.
PATHOGENESIS OF THE LINK
Two mechanisms best describe the potential causal link between periodontal diseases and respiratory disease. The first action centers on the direct presence of both pulmonary and periodontal pathogens in plaque biofilm and in reservoirs in the oral cavity. Specific bacteria identified as risk factors for pneumonia, such as Streptococcus pneumoniae, Haemo philus influenzae, Staphylococcus aureus, and Enterobacter (see Figures 1 through 4), have been found throughout the mouth in a variety of oral secretions and in transtracheal aspirates from infected lung sites. Bacterial pneumonia can be traced to the aspiration and/or inhalation of bacterial colonies from the mouth and oropharynx to the upper airway.4
The second mechanism focuses on the pathogenesis of periodontitis—specifically the enzymes that facilitate adherence of respiratory pathogens in pulmonary airways and destroy protective salivary tooth pellicle. In addition, cytokines released as part of the inflammatory process of periodontitis boost adhesion receptors on the mucosa, which results in increased respiratory pathogen colonization.5
Since close examination of the pathogenesis identifies these two major risk factors—including levels of oral bacteria and presence of periodontitis— patients who are at risk and also patients with current acute and chronic respiratory conditions should be targeted for more frequent and intensive dental hygiene care.
ACUTE RESPIRATORY DISEASES
Pneumonia is a general diagnostic term used to describe serious infection in the lungs from more than 30 different causes. The most common causes are viruses, bacteria, mycoplasmas (a type of bacteria without cell walls, which makes them resistant to many common antibiotics), fungi, and other agents. Pneumonia was the number one cause of death in the United States until 1936 when antibiotics were instituted as a routine part of care. However, pneumonia remains a serious infection, especially as a complication to pre-existing lung disease or other conditions in addition to a primary disease diagnosis.
In 2004, pneumonia and influenza combined ranked as the eighth leading cause of death in the United States, with 60,207 people dying of pneumonia in 2004.7 In 2005, pneumonia accounted for 717,000 hospital discharges in women at a rate of 47.4 per 10,000 patients, and for 651,000 hospital discharges in men at a rate of 44.9 per 10,000 patients.7 In addition to the greater number of women affected by pneumonia, individuals age 65 and older are disproportionately affected at the rate of 221.3 per 10,000 patients.7
Pneumoccal pneumonia is the most serious form of pneumonia, and is caused by the bacteria Streptococcus pneumoniae, which accounts for 25% to 35% of all community-acquired pneumonia. The onset of pneumoccal pneumonia can vary from gradual to sudden, and symptoms include chills, chest pain, sweats, cough with rust- or green-colored mucus, and increased breathing and pulse rates.8
About half of pneumonia cases are thought to be viral in origin and tend to cause less severe illness than pneumonia caused by bacteria. Symptoms of viral pneumonia tend to mimic influenza and include headache, dry cough, fever, muscle pain, and weakness.8 Mycoplasmas have characteristics of both bacteria and viruses, and produce more mild and widespread symptoms of pneumonia, most commonly a cough. Mycoplasmas are responsible for many cases of pneumonia among school-age children and cause approximately 15% to 50% of all adult cases of pneumonia.8
The risk for community-acquired pneumonia infections is highest among women; the elderly; those who have pre-existing health conditions, such as COPD, diabetes, and congestive heart failure; those who are immune suppressed, such as people who have HIV disease; and those undergoing cancer therapy. These same patients are at high risk for hospital- acquired pneumonia, which accounts for 15% of all hospital-associated infections, most commonly in the intensive care unit (27% of all infections) and the coronary care unit (24% of all infections).9 Unfortunately, mortality rates are 20% to 33% for hospital-acquired pneumonia, which underlines the serious nature of pneumonia infections. The risk is particularly high for patients who are ventilator dependent, which is the most common risk factor for nosocomial pneumonia infections.9 The incidence of ventilator-associated pneumonia may be as high as 78%, and is described as the most common hospital-acquired infection among patients who require ventilation.4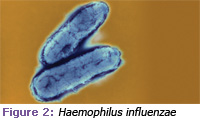
CHRONIC RESPIRATORY DISEASES
COPD is a chronic respiratory disease characterized by an obstruction of airflow in the lungs, Americans died from COPD—making it the fourth leading cause of death in the United States.10
Asthma is a common chronic lung disease that causes tightness in the chest, shortness of breath, coughing, and wheezing. Approximately 22 million Americans have asthma.11 Although asthma has not been classically included within the definition of COPD, many adults who experience asthma earlier in life are now being dually diagnosed with COPD, and the number of those patients dually diagnosed with both COPD and asthma is increasing.11
RESPIRATORY DISEASES AND ORAL HEALTH
Two systematic literature reviews have been published regarding the association between oral health and respiratory diseases.4,5 They provide a more complete picture of the associations between oral health and pneumonia, COPD, and asthma.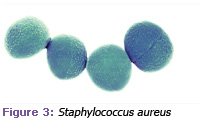
In the first systematic literature review on respiratory diseases and oral health published in 2003, Scannapieco et al selected a total of 30 studies, and demonstrated that the oral cavity may provide a reservoir of bacteria for lower airway infections, especially for hospitalized patients and medically complex patients.5 The findings also suggested that improved oral hygiene measures can reduce the incidence of pneumonia.5 Regarding COPD and asthma, this study analysis found that poor oral hygiene and smoking status were statistically associated with chronic respiratory diseases.5
Azarpazhooh et al selected 19 studies for the second systematic literature review, which was published in 2006.4 The authors evaluated the evidence to support a fair association between pneumonia and oral health, drawing on evidence from well-designed cohort and case control studies.4 These authors identified dental decay and the presence of cariogenic bacteria in addition to periodontal pathogens as significant risk factors for aspiration pneumonia. They also found that patients’ dependence on caregivers to complete oral hygiene procedures was a significant risk factor associated with pneumonia.4 Azarpazhooh et al concluded that there was poor evidence to support an association between COPD and oral health because of small sample size and poor control selection. However, all four studies selected for the systematic review showed a potential association between COPD and periodontal diseases, and the authors recommended further, well-designed research to build on these previous studies.4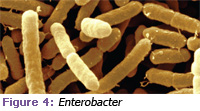
ORAL CARE INTERVENTIONS
Both systematic literature reviews also included a review of interventional studies designed to measure the effectiveness of enhanced oral hygiene in relation to occurrence and/or progression of respiratory diseases. As part of the systematic review, Scannapieco et al completed a meta-analysis of combined data from five intervention trials and concluded that the oral hygiene intervention significantly reduced occurrence of pneumonia in institutionalized subjects.5 In a review of 10 clinical research trials, Azarpazhooh et al concluded that there was a good level of evidence that improved oral hygiene and the provision of professional oral care reduce the occurrence and/or progression of respiratory disease in high-risk elderly adults in intensive care units and nursing facilities.4 Oral hygiene activities varied among the studies and included toothbrushing; use of 0.12% and/or 0.2% chlorhexidine gluconate rinse and/or gel; use of nonabsorbable PNV solution (polymyxin B sulfate, neomycin sulfate, vancomycin hydrochloride); application of 1% povidone iodine; and placement of orabase with gentamicin/colostin/vancomycin 2%. No standard protocols for oral hygiene and/or professional oral care were identified through the research literature selected for review.
Two additional systematic reviews have been published regarding oral hygiene practices and respiratory diseases. In the first of the two reviews published in 2007, Berry et al12 focused on intensive oral health care for patients receiving mechanical ventilation. Although the authors found 55 published articles, they did not find high level evidence from either randomized controlled trials or systematic reviews, and as such, were limited in their evidence-based recommendations for clinical nursing practice.12 Berry et al recommended that standard protocols be developed and tested in multicenter trials in order to provide evidence in standard protocols for oral hygiene and professional care in hospitals and institutional settings.12 They advised clinicians to continue their emphasis on routine, consistent, and thorough oral hygiene procedures in the absence of specific evidence-based protocols.
In a second systematic review published in 2008, Sjogren et al selected 15 articles for analysis.6 Although the authors noted a wide variety in the design and quality of the studies, they concluded that oral hygiene had positive preventive effects on reducing pneumonia and other respiratory infections in elderly patients who were either hospitalized or were nursing home residents. Most significant, the authors concluded that approximately one in 10 cases of death from pneumonia among elderly nursing home residents may be prevented by improving oral hygiene.6
IMPLICATIONS FOR DENTAL HYGIENE CARE
This research confirms the central role of thorough, frequent oral hygiene and professional oral health care for promoting good oral health as well as respiratory health. Dental hygienists should be encouraged to work with patients to identify and reduce risk factors that will limit the initiation and progression of both acute and chronic respiratory diseases. Given the significant economic, social, and health care burdens that respiratory diseases place on individuals and the population overall, dental hygiene care must be viewed as a cost-effective and easily accessible intervention critical for patients who are most at risk for respiratory diseases. In addition to giving specific attention to both mechanical and chemotherapeutic regimens, dental hygienists should include tobacco cessation counseling as an integral part of the care they provide to patients given the comorbidity of smoking as risk factors for both periodontal disease and COPD.
Patients who have chronic respiratory diseases pose particular challenges for dental hygienists in planning and managing the most appropriate levels of dental hygiene care. Although further research is needed to clarify the best practices for dental hygiene care, especially regarding procedures that generate dental aerosols, Agado and Bowen provide practical and realistic recommendations for alterations in the dental hygiene process of care for patients who have COPD and periodontitis.13 For example, the authors recommend alterations in the assessment, treatment, and education phases of care to include monitoring breathing status, blood pressure, and seating position, as well as assessment of smoking status and routine oral cancer examinations as essential components of assessment.13 Regarding specific dental hygiene treatment, the authors recommend that both the use of pre-procedural antiseptic mouthrinse and high volume evacuation should be implemented during care, especially when ultrasonic instru mentation is indicated.13
Access to patients who are most at risk for acute respiratory diseases poses an additional challenge for dental hygienists. Although great strides have been made in incorporating routine oral care procedures among hospitals and institutional settings as well as increasing access to dental hygiene services in these facilities, many challenges remain. Berry et al noted a paucity of standardized, evidence-based oral hygiene care protocols available in the nursing environment.12 Elliot-Smith recommends a collaborative approach for dental hygiene and nursing, and provides examples of dental hygienists and dentists who work with nursing colleagues to develop and implement oral hygiene protocols, especially with caregivers in institutional and home settings.14 Given the potential significant impact that routine oral hygiene and dental hygiene care can have in reducing the burden of acute and chronic respiratory diseases, it is critical for dental hygienists to move beyond the traditional venue of care to work with caregivers, nurses, and other health care professionals to increase not only the quality of oral health, but general health as well.
Photo credits: Figure 1: Science Source / Photo Researchers, Inc; Figure 2: A. Dowsett, Health Protection Agency / Photo Researchers, Inc; Figure 3: SPL / Photo Researchers, Inc; Figure 4: SciMAT / Photo Researchers, Inc.
REFERENCES
- American Lung Association. Diseases A to Z. Available at www.lungusa.org/site/c.dvLUK9O0E/b.33316. Accessed August 31, 2009.
- Oral Health in America: a Report of the Surgeon General. Rockville, Md: United States Department of Health and Human Services. NIH Publication No 00-4713; 2000.
- National Call to Action to Promote Oral Health. Rockville, Md: United States Department of Health and Human Services, Public Health Service, National Institutes of Health, National Institute of Dental and Craniofacial Research. NIH Publication No 03-5303; 2003.
- Azarpazhooh A, Leake JL. Systematic review of the association between respiratory diseases and oral health. J Periodontol. 2006;77:1465-1482.
- Scannapieco FA, Bush RB, Paju S. Associations between periodontal disease and risk for nosocomial bacteria pneumonia and chronic obstructive pulmonary disease. A systematic review. Ann Periodontol. 2003;8:1, 54-69.
- Sjogren P, Nilsson E, Forsell M, Johansson O, Hoogstraate J. A systematic review of the preventive effect of oral hygiene on pneumonia and respiratory tract infection in elderly people in hospitals and nursing homes: effect estimates and methodological quality of randomized controlled trials. J Am Geriatric Soc. 2008;56:2124-2130.
- DeFrances CJ, Hall MJ. 2005 National Hospital Discharge Survey. Advance Data From Vital and Health Statistics. 2007;385:1-19.
- American Lung Association. Pneumonia Fact Sheet. Available at: www.lungusa.org/site/apps/nlnet/content3.aspx?c=dvLUK9O0E&b=2060321&content_id={08C669B0-E845-4C9C-8B1E-285348BC83BD}¬oc=1. Accessed August 31, 2009.
- Leu HS, Kaiser DL, Mori M, Woolson RF, Wenzel RP. Hospital-acquired pneumonia. Attributable mortality and morbidity. Am J Epidemiol. 1989;129:1258-1267.
- American Lung Association. Chronic Obstructive Pulmonary Disease (COPD) Fact Sheet. Available at: www.lungusa.org/site/apps/nlnet/content3.aspx?c=dvLUK9O0E&b=2060053&content_id={EE451F66- 996B-4C23-874D-BF66586196FF}¬oc=1. Accessed August 31, 2009.
- Cardarelli WJ. Asthma: are we monitoring the correct measures? Popul Health Manag. 2009 Mar 26. [Epub ahead of print].
- Berry AM, Davidson PM, Masters J, Rolls K. Systematic literature review of oral hygiene practices for intensive care patients receiving mechanical ventilation. Am J Crit Care. 2007;16:552-562.
- Agado B, Bowen DM. Does the link between COPD and periodontitis affect dental hygiene treatment? Access. 2009;23:4,19-21.
- Elliott-Smith S. Finding a collaborative link, treating periodontal and respiratory diseases. Access. 2009;23:4,16-18.
From Dimensions of Dental Hygiene. October 2009; 7(10): 54-57.



