
Etiology of Noncarious Cervical Lesions
As the prevalence of these lesions increases, understanding the roles of abrasion, erosion, and abfraction is key to effectively preventing further destruction of the tooth surface.
As the number of older adults in the United States continues to grow, this change in patient demographics will profoundly affect the practice of dental hygiene. Not only are there more older adults, but they are also retaining more of their natural teeth than ever before. The risk of alveolar bone loss; gingival recession, which can lead to exposed cervical and root areas of the teeth;1 and tooth wear all increase with age. The confluence of these factors raises the risk of noncarious cervical lesions.
NONCARIOUS CERVICAL LESIONS
The phrase “noncarious cervical lesion” (NCCL) describes cervical lesions caused by abrasion, erosion, and abfraction.2–6 While some NCCLs may be identifiable as abrasion, erosion, or abfraction because their etiology is apparent at the moment of examination, many NCCLs are caused by a combination of these etiological factors.1–9 Addy and Shellis4 found that abrasion, erosion, and abfraction most likely interact with each other as opposed to each one acting alone. They note that the erosive damage to hard tissues caused by abrasion may be the most significant relationship in occlusal and cervical wear.4
NCCLs have a variety of clinical presentations, including wedge-shaped, disc-shaped, or very irregular.7 The shape of some NCCLs may be associated with their etiology.8 Abfraction lesions are often sharply wedge-shaped. Lesions caused by abrasion are typically wide, rounded, and disc-shaped, and erosive lesions are broad but more shallow than those caused by abfraction or abrasion.10
ABRASION
Abrasion is the abnormal loss of tooth substance that results from mechanical or friction forces between the tooth and an abrasive medium, such as the particles in prophylaxis paste or toothpaste.1,7 Abrasion often manifests as a disc-shaped lesion that creates a “V” shaped area at the cervical/gingival portion on the facial tooth surface. Abrasion is also attributed to improper brushing techniques. However, if patients are using a soft or extra-soft bristled toothbrush, this is unlikely.8 There is a body of evidence dating back to the 1960s that shows toothbrushes may create very small changes in the tooth surface.9–17 But these changes are minute—measured in microns—as opposed to the extreme cervical wear that is sometimes attributed to toothbrush abrasion.16 A 2007 systematic review found that there is not enough data to support or negate a relationship between toothbrushing and gingival recession.17
Ashcroft and Joiner concluded that the evidence does not support an association between exposed dentin and toothbrush abrasion.1 Dental professionals must be careful when suggesting to patients that they are “brushing too hard.” Many may in fact be using a recommended toothbrushing method, a mildly abrasive or nonabrasive toothpaste, and a soft or extra soft toothbrush. Based on the Mohs hardness numbers of enamel and abrasive particles, the abrasives in toothpaste are more likely responsible for wear on tooth enamel than toothbrush bristles.
EROSION
Erosion is the abnormal loss of tooth substance caused by a chemicomechanical action, but not from acids associated with bacteria.1,7 Exposure to acid caused by gastric reflux and habits, such as the habitual sucking of lemons and frequent vomiting, cause erosion.18–20 A significant number of erosive lesions are seen in children and teens who consume acidic soft drinks, sports drinks, and energy drinks. In the United States, soft drink consumption increased 300% between the late 1970s and the late 1990s.21 Whitening toothpastes that rely on chemical bleaching processes can also contribute to erosive NCCLs.22
Erosion causes a loss of luster of the enamel on the lingual surfaces of the teeth. Oral exposure to stomach acid causes a shallow thinning, beginning at the cervical portion of the tooth and progressing coronally. Erosion from the ingestion of acid-containing soft drinks may cause pitting of the cervical facial enamel or a loss of enamel luster with a chalky decalcification of the enamel surface.21,22
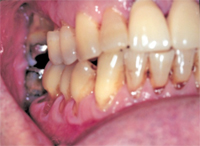
ABRASION AND EROSION COMBINED
Abrasion can be accelerated by erosion, as the combined effect of abrasion and erosion is greater than either process on its own.23–25 In one study that compared abrasion and erosion, the outcome of the two processes combined was 50% greater than the outcomes from either of the processes alone.25 In a literature review on NCCLs, Bartlett and Shaw8 concluded that there is overwhelming evidence from clinical and laboratory studies that abrasion and erosion are linked to NCCLs, yet data also support the theory that NCCLs are caused specifically by abrasion or erosion alone.
ABFRACTION
Abfraction is the third category of NCCLs. Abfraction lesions appear wedge-shaped at the cervical portion of the tooth with sharp internal and external angles (Figure 1).26 Abfraction lesions can be seen on facial and lingual surfaces on both anterior and posterior teeth. Lee and Eakle,26 and Grippo27 coined the term “abfraction” (derived from Latin words “ab,” meaning “away” and “fractio,” meaning “breaking”),8,27,28 and defined it as the “pathological loss of tooth substance caused by biomechanical loading forces.”26–32
As stated previously, many dental professionals have ascribed the etiology of NCCLs to toothbrush abrasion if another cause was not readily apparent. However, there are NCCLs that cannot be explained by toothbrush abrasion or erosion. In the early 1980s, McCoy31,32 questioned the role of toothbrush abrasion in what was then referred to as “cervical erosion.” McCoy used information gleaned from engineering studies and postulated that it was tensile stresses that caused the notches in the cervical portion of the teeth. Two other investigators, Lee and Eakle26 also hypothesized that it was the tensile stresses from occlusal forces from mastication and malocclusion that were in fact responsible for the etiology of the NCCLs. They suggested the concentration of tensile stresses from eccentric occlusion result in the disruption of the chemical bonds between the hydroxyapatite crystals in enamel and dentin, resulting in a deformation or fracture of the hard tooth structures at the cervical portion of the tooth, and that water molecules could invade the broken hydroxyapatite chemical bonds. The water and additional small molecules penetrate between the prisms of the hydroxyapatite crystals and prevent the chemical bonds from being reestablished when the stress is relieved.
In summary, abfraction occurs in the presence of eccentric occlusion or malocclusion. Abnormal forces create alternating or cyclic tensile and compressive stresses, which lead to a weakening in the enamel and dentin.28 After the fatigue limit is reached, there is a breaking in the enamel placed on the tension at the cervical portion of the tooth, which is the most stressed zone, resulting in abfraction or wear.
THE ROLE OF DENTAL HYGIENISTS
The direct etiology of NCCLs may be unclear, but it is paramount to long-term oral health that all NCCLs are recorded in the patient record and their etiology discussed with the patient. These lesions are not always symptomatic but if they are causing problems, such as sensitivity to changes in thermal conditions or to acidic foods, treatment may be in order. Treatment can range from the application of fluoride varnish to restorative care. Plaque retention, which can lead to dental caries, and dentinal hypersensitivity may result from NCCLs, and both will benefit from a range of fluoride therapies—from professionally-applied products to prescription fluoride dentifrices for at-home use.
If patients have detrimental oral habits, such as sucking on lemons or chewing on hard objects, dental hygienists need to encourage them to discontinue the habit in order to prevent the deleterious, cumulative effects of abrasion, erosion, and abfraction. The role of drinking beverages containing large amounts of sugar and acid in NCCLs should also be discussed. Patients need to understand that consuming these drinks can cause devastating effects in the oral cavity, including tooth loss, and create the need for expensive restorative treatments.
Lastly, dental hygienists need to know which oral hygiene products patients are using. If patients with NCCLs are using whitening products, whether chemical or abrasive, the result will likely increase sensitivity. Equally important is discovering the brand of toothpaste the patient uses and determining its level of abrasivity. Patients with NCCLs should use a nonabrasive dentifrice. The prevalence of NCCLs is growing, largely due to the rising numbers of older adults in current populations. Dental hygienists are well-equipped to intercept these noncarious lesions and provide appropriate education, prevention, and treatment.
REFERENCES
- Aschcroft AT, Joiner A. Tooth cleaning andtooth wear: a review. J Engineering Tribiology.2010;224:539–549.
- Hempton TJ, Ovadia R, McManama JC, BonacciFJ. Addressing cervical class V lesions. Dimensionsof Dental Hygiene. 2010;8(3):48–51.
- Grippo JO, Simring M, Schreiner S. Attrition,abrasion, corrosion and abfraction revisited: anew perspective on tooth surface lesions. J AmDent Assoc. 2004;135:1109–1118.
- Addy M, Shellis RP. Interaction betweenattrition, abrasion, erosion in tooth wear. MonogrOral Sci. 2006;20:17 –31.
- Harpenau LA, Noble WH, Kao RT. Diagnosisand management of dental wear. J Calif DentAssoc. 2011;39:225–231.
- Wood ID, Kassir ASA, Brunton PA. Effect oflateral excursive movements on the progressionof abfraction lesions. Oper Dent. 2009;34:273–279.
- Roberson TM, Heymann HO, Swift EJ.Sturdevant’s Art and Science of OperativeDentistry. 5th ed. Philadelphia: Mosby; 2006:292.
- Bartlett DW, Shaw P. A critical review of noncariouscervical (wear) lesions and the role ofabfraction, erosion and abrasion. J Dent Res.2006;85:306–312.
- Perez Cdos R, Gonzalez MR, Prado NAS,Ferreira de Miranda MS, de Andrade Macedo M,Fernandes BMP. Restoration of noncariouscervical lesions: when, why and how. Int J Dent.2012;2012:687058.
- Reyes E, Hildebolt C, Langenwalter E, Miley D.Abfraction and attachment loss in teeth withpremature contacts in centric relation: clinicalobservations. J Periodontol. 2009;80:1955–1962.
- Manly RS, Wiren J, Manly PJ, Keene RC. Amethod for measurement of abrasion of dentinby toothbrush and dentifrice. J Dent Res.1965;44:533–540.
- Bjorn H, Lindhe J. On the mechanics oftoothbrushing. Odontol Revy. 1966;17:9–16.
- Bjorn H, Lindhe J, Grondhal HG. The abrasionof dentine by commercial dentifrices. OdontolRevy. 1966;17:109–120.
- Volpe AR, Mooney R, Zumbrunnen C, Stahl,D, Goldman HM. A long term clinical studyevaluating the effect of two dentifrices on oraltissues. J Periodontol. 1975;46:113–116.
- Sanges G, Gjermo P. Prevalence of oral softand hard tissue lesions related to mechanicaltooth cleansing procedures. Community DentOral Epidemiol. 1976;4:77–83.
- Bergstrom J, Lavstedt S. An epidemiologicapproach to toothbrushing and dental abrasion.Community Dent Oral Epidemiol. 1979;7:57–64.
- Rajapakse PS, McCracken GI, Gwynnett E,Steen ND, Guentsch A, Heasman PA. Does toothbrushing influence the development andprogression of non-inflammatory gingivalrecession? A systematic review. J Clin Periodontol.2007;34:1046–1061.
- Dynesen AW, Bardow A, Petersson B, NielsenLR, Nauntofte B. Salivary changes and dentalerosion in bulimia nervosa. Oral Surg Oral MedOral Pathol Oral Radiol Endod. 2008;106:696–707.
- Scheutzel P. Etiology of dental erosion—intrinsic factors. Eur J Oral Sci. 1996;104:178–190.
- Lussi A. Dental erosion from diagnosis totherapy. Monographs in Oral Sci Basel Karger.2006;20:1–8.
- Borjian A, Ferrari CC, Anouf A, Touyz LZ. Popcolaacids and tooth erosion: an in vitro, in vivo,electron-microscopic, and clinical report. Int JDent. 2010;2010:957842.
- Lussi A, Hellwig E. Risk assessment andpreventive measures. Monogr Oral Sci.2006,20:190–199.
- Davis WB, Winter PJ. The effect of abrasionon enamel and dentine after exposure to dietaryacid. Br Dent J. 1980;148:253–256.
- Assopardi A, Bartlett DW, Watson TF. SheriffM. The measurement and prevention of erosionand abrasion. J Dent Res. 2001;29:395–400.
- Eisenburger M, Shellis RP. Addy M.Comparative study of wear of enamel inducedby alternating and simultaneous combinations ofabrasion and erosion in vitro. Caries Res.2003;37:450–455.
- Lee WC, Eakle WA. Possible role of tensilestress in the etiology of cervical erosive lesions ofthe teeth. J Prosthet Dent. 1984;52:374–380.
- Grippo JO. Abfractions: a new classification ofhard tissue lesions of teeth. J Esthet Dent.1991;3:14–19.
- Palmer B. Abfraction: A Literature Review andHypothesis. Available at: www.brianpalmerdds.com/hypothesis_abfractions.htm. AccessedSeptember 24, 2012.
- Litonjua LA, Andreana S, Bush PJ, Cohen RE.Noncarious cervical lesions and abfractions. A reevaluation.J Am Dent Assoc. 2003;134:845–850.
- Grippo JO, Simring M, Coleman TA.Abfraction, abrasion, biocorosion, and theenigma of noncarious cervical lesions: a 20-yearperspective. J Esthet Rest Dent. 2012;24:10–23.
- McCoy G. The etiology of gingival erosion. JOral Implantol.1982;10:361–362.
- McCoy G. On the longevity of teeth. J OralImplantol.1983;11:248–267.
From Dimensions of Dental Hygiene. October 2012; 10(10): 50-52.

