
Brighter, Whiter, Ouch!
Treating whitening-induced dentin hypersensitivity.
As interest in cosmetic dentistry, particularly whitening treatments, continues to rise, tooth sensitivity remains a prevalent condition.
Both professional and over-the-counter whitening treatments can cause dentin hypersensitivity and may lead to discontinuation or delay of whitening procedures.
Dentin hypersensitivity is a common ailment. A study of patients in five private practices found that more than 57% experienced dentin hypersensitivity, particularly patients between the ages of 30 and 39.1 While painful and irritating, dentin hypersensitivity is often a manageable condition. However, patients may not think their symptoms are worth mentioning at regular examinations, particularly because the pain can be intermittent. Proactively discussing, diagnosing, and treating dentin hypersensitivity are important elements of providing complete oral health care.
DEFINITION
Dentin hypersensitivity affects one in five adults in the United States, typically those between the ages of 20 and 50, with a peak in adults between the ages of 25 to 39.1,2 Patients with periodontal diseases are at particularly high risk; between 72% and 98% of periodontal patients experience sensitivity.3
Most frequently observed on the premolars, dentin hypersensitivity occurs when tubules at the exposed dentin surface lead to sharp pain when exposed to a stimulus or trigger.2,4 Patients often describe this pain as short and sharp, with common triggers including:5
- Hot or cold air,
- Hot or cold beverages,
- Acidic foods and beverages, and
- Sweet or sugary foods and beverages.
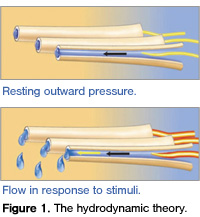
According to the hydrodynamic theory, which is based on the flow of fluid found within the dentinal tubules, tooth sensitivity occurs when a stimulus or trigger is applied to a tooth surface with open or patent dentinal tubules (Figure 1). Fluid movement within the tubules changes the pressure on the nerve endings within the pulp, and creates a nerve response triggering a sensation of pain.4 Patients will often modify their behavior instead of seeking treatment by avoiding certain drinks, foods, and behaviors. If patients are not aware that they are suffering from dentin hypersensitivity, they often simply live with the pain.
 All patients can suffer from sensitivity to some degree. As a result, early screening for those with potential for advanced dentin hypersensitivity is essential. Dentin hypersensitivity is more prevalent in women than in men; research suggests 42% of women in North America suffer from sensitivity compared to 31% of men.4 Aside from patients who self-report sensitivity, talking to patients who have a diet high in citrus fruits, carbonated beverages, and sports drinks can assist in early sensitivity detection.
All patients can suffer from sensitivity to some degree. As a result, early screening for those with potential for advanced dentin hypersensitivity is essential. Dentin hypersensitivity is more prevalent in women than in men; research suggests 42% of women in North America suffer from sensitivity compared to 31% of men.4 Aside from patients who self-report sensitivity, talking to patients who have a diet high in citrus fruits, carbonated beverages, and sports drinks can assist in early sensitivity detection.
CAUSES
Dentin hypersensitivity is often triggered by professionally dispensed and over-the-counter whitening treatments. In this case, sensitivity occurs when the chemical by-products of carbamide and hydrogen peroxide used in whitening treatment passes through the enamel and dentin and into the pulp. Consequently, many practitioners recommend patients to discontinue or alter whitening treatments as recommended by the whitening manufacturer.
Additional causes of dentin hypersensitivity may include gingival recession with rapid loss of the dentinal smear layer. Loss of tooth enamel and the resulting opening of the dentinal tubules due to abrasion, attrition, or erosion can also factor into dentin hypersensitivity.6 Periodontal diseases and bruxism can also lead to sensitivity in some patients.
When determining if dentin hypersensitivity is the cause of a patient’s pain, triggers must be ruled out. These may include caries, pulpitis, cracked or chipped teeth, and/or problematic restorations. While these may be causing the patient to experience sensitivity, the treatment protocol differs considerably.
TREATMENT OPTIONS
Once a patient’s history and symptoms are collected and the causes of sensitivity have been narrowed or determined, the next step is to begin administering the recommended therapy.
Antisensitivity dentifrice products containing 5% potassium nitrate (KNO3) can be recommended as a first line of treatment. Potassium nitrate works to relieve sensitivity by depolarizing the nerves that innervate the dentinal tubules. Potassium ions from the KNO3 diffuse through the dentinal tubules to the nerve endings in the pulp cavity and stop the repolarization of the nerve fibers, leaving the nerve in a resting state and relieving pain. Within 2 weeks of use, an antisensitivity dentifrice with 5% KNO3 can relieve pain from dentin hypersensitivity. Using a dentifrice containing potassium nitrate is a noninvasive and affordable treatment option that can replace a patient’s everyday toothpaste.
Chairside treatments also are an option, and can be enhanced by patient-applied treatments. For example, highly-concentrated fluoride varnishes or lacquers can be used, and are often most successful for moderate cases when combined with a desensitizing dentifrice.7 For patient ease and/or preference, highly concentrated fluoride varnishes or laquers can also be used with mouthguards, particularly when treating multiple teeth.6 Products containing amorphous calcium phosphate and arginine bicarbonate may also be effective in treating hypersensitivity.
WHITENING-RELATED SENSITIVITY TREATMENT
Both dentist-dispensed and over-the-counter whitening products contain peroxide (typically carbamide or hydrogen peroxide), which works to whiten tooth enamel.
A recent study conducted in dental offices demonstrated that patients who brushed with an antisensitivity dentifrice containing the maximum amount of KNO3 two times daily, 2 weeks before and 2 weeks during professional whitening treatment experienced significantly less sensitivity compared to a control group using regular toothpaste.8 Not only were these patients more satisfied with their whitening experience, but they were also more willing to repeat whitening treatments in the future. Whitening results were not affected by the desensitizing toothpaste.8
CONCLUSION
All patients who are undergoing a tooth whitening treatment are at risk for sensitivity. In some cases, the pain is severe enough that the patient delays or even discontinues the treatment, which can result in dissatisfaction. Fortunately, many treatment options exist for decreasing sensitivity. Therefore, discussing the potential for sensitivity with whitening patients before beginning treatment is imperative to a positive outcome.
REFERENCES
- Irwin CR, McCusker P. Prevalence of dentine hypersensitivity and plaque in a general dental population. J Ir Dent Assoc. 1997;43:7-9.
- Gillam DG, Aris A, Bulman JS, Newman HN, Ley F. Dentin hypersensitivity in subjects recruited for clinical trials: clinical evaluation, prevalence and intra-oral distribution. J Oral Rehabil. 2002;29:226-231.
- Chabanski MB, Gillam DG, Bulman JS, Newman HN. Clinical evaluation of cervical dentine sensitivity in a population of patients referred to as specialist periodontology department: a pilot study. J Oral Rehabil. 1997;24:666-672.
- Addy M. Detine hypersensitivity: new perspectives on an old problem. Int Dent J. 2002;52:367-375.
- Zero D. Erosion—chemical and biological factors of importance to the dental practitioner. Int Dent J. 2005;55:285-290.
- Kielbassa AM. Dentine hypersensitivity: simple steps for everyday diagnosis and management. Int Dent J. 2002;52:394-396.
- Hansen EK. Dentin hypersensitivity treated with a fluoride-containing varnish or a light-cured glass-ionomer liner. Scand J Dent Res. 1992;100:305-309.
- Haywood, VB, Cordero R, Wright K, et al. Brushing with a potassium nitrate dentifrice to reduce bleaching sensitivity. J Clin Dent. 2005;16:17-22.
From Dimensions of Dental Hygiene. June 2007;5(6): 24, 26.

