
Breaking Down Barriers
Improving access to oral health care is critical to people living with HIV.
This course was published in the August 2010 issue and expires August 2013 The authors have no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- Understand the importance of oral health for people living with HIV.
- Discuss the barriers to oral health care experienced by those living with HIV
- Describe the strategies and goals of the Special Project of National Significance to expand access to oral health care for underserved
- populations living with HIV disease.
- List common HIV-related oral conditions.
- Discuss rapid HIV testing in the oral health care setting.
People living with HIV have more unmet oral health care needs than the general population.3 They also have more unmet oral health care needs than unmet medical needs.4 People of color, especially women and those without dental insurance, are less likely to receive dental care than others living with HIV.5 Understanding the structural and personal barriers to oral health care for people living with HIV is key to finding interventions that reduce these impediments.
Among people living with HIV, factors contributing to poor access to oral health care mirror those of other vulnerable populations. These include financial barriers4 and structural barriers, such as provider availability, discrimination, fear of dental treatment, and low patient interest in seeking care.6 With nearly half of all expenditures for dental care coming out of patients’ pockets,7 a lack of dental insurance has a major impact on access to care. For low-income individuals, including many living with HIV/acquired immune deficiency syndrome (AIDS), Medicaid is the only source of dental insurance, yet only 60% of people who receive Medicaid benefits live in states that cover adult dental care.8 Research suggests that only 29% of adult Medicaid enrollees visited a dental office in the past year, compared to 44% of adults aged 19 years to 64 years in the general population.4
Access to oral health screening, preventive care and maintenance, and treatment of oral health problems are critical components of basic HIV care. Individuals who receive regular diagnostic and preventive oral health care are less likely to require restorative, endodontic, periodontal, and surgical treatment.9 As such, addressing the obstacles to receiving oral health care and finding innovative ways to overcome them are integral to improving the health and quality of life for the approximately 1 million people living with HIV in the United States.10
SPNS PROJECT
In 2006, the Health Resources and Services Administration (HRSA) HIV/AIDS Bureau, which is part of the US Health and Human Services Department, launched a Special Project of National Sig nificance (SPNS) to expand access to oral health care for underserved populations living with HIV. HRSA is funding 15 demonstration projects, eight in rural areas and seven in urban areas, in addition to a multisite evaluation and technical assistance center, to develop and document strategies for expanding access to oral health care. The HRSA funding will continue for 5 years. The goals of this initiative are to expand access to HIV oral health care services through innovative models, and to disseminate program outcomes to the broader health care community in order to encourage providers and communities to increase access to oral health care for people living with HIV.
Table 1 provides a list of the demonstration projects and the innovative approaches they are implementing to provide oral health care to people living with HIV. Many use a team approach to identify and treat oral manifestations of HIV.5 The HIV medical clinics have adopted a multidisciplinary approach by incorporating oral health care services into their programs. Some programs are strengthening relationships between oral health care and medical care by providing training programs for health care providers and case managers. Other strategies include the use of mobile dental clinics, community college dental hygiene programs, and transportation services, in addition to the establishment of satellite clinics and dental reimbursement models. The Lane Community College program in Eugene, Ore, is of particular significance to the dental hygiene profession because it provides comprehensive oral health care to people living with HIV while also offering valuable hands-on training for dental hygiene students.
- Xerostomia
- Candidiasis
- Oral hairy leukoplakia
- Linear gingival erythema
- Necrotizing ulcerative periodontitis
- Kaposi’s sarcoma
- Oral warts
- Herpes simplex virus
- Aphthous ulcers
- Neutropenic ulcers
One of the program’s major challenges is providing a comprehensive model of oral health care, including access to the full range of dental specialty care, such as periodontics, endodontics, and oral and maxillofacial surgery. Some programs bring specialty providers onsite or contract with dental specialists for referral services. Other programs hire patient navigators or dental case managers to help patients access specialty care. The employment of peer outreach workers, patient navigators, and case managers in oral health care settings is a new approach.
ACHIEVING SUSTAINABILITY
The ultimate success of this initiative depends on program sustainability. There are two main components of sustainability: establishing community-wide consensus that oral health care is a vital part of overall HIV care; and identifying the financial resources that will continue to support the sites beyond the grant period. The programs are exploring ways to attain financial viability, such as: applying for status as a federally-qualified community health center; maximizing reimbursement through Medicaid; requesting funds from the Ryan White Comprehensive AIDS Resources Emergency (CARE) Act, the largest federally funded program for people living with HIV/AIDS; and seeking reimbursement from private insurance. Some program directors are generating new lines of business to help support HIV oral health care or learning to maximize patient revenues through decreasing “no-show” rates and maximizing clinical capacity.
IMPLICATIONS FOR DENTAL HYGIENISTS
The dental hygienist plays a role in both the management of oral health problems for people living with HIV and in the early diagnosis of the virus. Patients living with HIV are at risk for a variety of oral health problems, such as xerostomia and aphthous ulcers. Since the introduction of highly active anti-retroviral therapy (HAART), the oral manifestations of HIV have changed. The occurrence of candidiasis has decreased because HAART boosts white blood cell counts and lowers viral loads.11 However, the side effects include xerostomia and oral warts.2 If untreated, xerostomia can increase levels of tooth decay and infections of the mouth. Receiving the appropriate dental treatment is paramount to this population because oral health problems can make it difficult to chew or swallow. Maintaining a healthy nutritional status and ensuring the ability to take HIV medications are key factors in sustaining overall health for people living with HIV.2
In patients who are unaware of their HIV status, the dental hygienist may be the first health care provider to notice the oral symptoms of HIV.13 In the past when patients exhibited oral symptoms of HIV, the dental hygienist’s only option was to refer them to their primary care physician or to an HIV testing site. In 2006, the Centers for Disease Control and Prevention (CDC) updated its recommendations to include HIV testing as part of routine medical care.14 The oral health care setting is viable for outpatient testing as more people visit a dental office over a 1-year period than a traditional medical setting.15 This provides a great opportunity for the dental hygienist who identifies systemic changes in the oral cavity to offer screening and referrals to medical care. Dental offices currently screen for other medical conditions, such as high blood pressure and diabetes. With the development of oral diagnostics, the opportunities to screen for systemic disease will increase.
Early identification of HIV infection and subsequent referral to appropriate medical care results in better health outcomes and improved quality of life. Increasing people’s awareness of their HIV status may also help reduce secondary transmission rates.

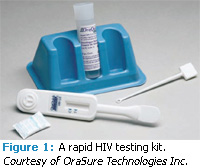
The dental hygienist can now screen for HIV using a saliva sample and a rapid HIV testing kit (see Figure 1). The saliva sample is placed on the test strip. If HIV antibodies are present, they adhere to the antigen contained in the test strip. The results are presented visually through a display that is similar to a home pregnancy test.16 The CDC encourages the use of rapid testing to increase the number of people not only tested, but who actually receive their results. Many individuals who present for traditional testing do not return for their results. With rapid testing, results are available in about 20 minutes.
Dental hygienists need training to correctly administer the test and to provide the appropriate counseling and referral services to medical care. The rapid HIV test is a preliminary test and patients with positive results must be referred for a confirmatory test. Patients who receive a positive test should also be advised about risk reduction behavior and their ability to spread the HIV infection.17
CONCLUSION
Improving access to oral health care is key to maintaining overall health in people living with HIV. The dental hygienist is well-suited to provide essential oral health care services to this population, to recognize changes in the oral cavity that may be related to HIV infection, and to offer chairside education not only about traditional preventive measures for promoting and maintaining oral health, but also in addressing the oral and medical needs of people living with HIV. The expanding role of the dental hygienist in the management of the HIV epidemic should include rapid testing in dental facilities, counseling, and referrals to HIV medical care and other support services.
REFERENCES
- Clinical guidelines for the primary care practitioner. In: Promoting Oral Health Care for People with HIV Infection. New York: New York State Department of Health AIDS Institute; 2001.
- Cherry-Peppers G, Daniels CO, Meeks V, Sanders CF, Reznik D. Oral manifestations in the era of HAART. J Natl Med Assoc. 2003;95(Suppl):21S-32S.
- Marcus M, Freed JR, Coulter ID, et al. Perceived unmet need for oral treatment among a national population of HIV-positive medical patients: social and clinical correlates. Am J Public Health. 2000;90:1059-1063.
- Coulter ID, Marcus M, Freed JR, et al. Use of dental care by HIV-Infected medical patients. J Dent Res. 2000;79:1356-1361.
- Dobalian A, Andersen RM, Stein JA, Hays RD, Cunningham WE, Marcus M. The impact of HIV on oral health and subsequent use of dental services. J Public Health Dent. 2003;63:78-85.
- Guay AH. Access to dental care: solving the problem for underserved populations. J Am Dent Assoc. 2004;135:1599-1605.
- Badner VM. Ensuring the oral health of patients with HIV. J Am Dent Assoc. 2005;136:1415-1417.
- Freed JR, Marcus M, Freed BA, et al. Oral health findings for HIV-infected adult medical patients from the HIV Cost and Services Utilization Study. J Am Dent Assoc. 2005;136:1396-1405.
- Achieving an HIV-free Generation: Recommendations for a New American HIV Strategy. Presidential Advisory Council on HIV/AIDS. Available at: www.comminit.com/en/node/220156/347. Accessed July 10, 2010.
- AIDS.ORG. How many people have HIV? Available at: www.aids.org/info/how-many-have-hiv-and-aids.html. Accessed July 9, 2010.
- Shiboski CH, Cohen M, Weber K, Shansky A, Malvin K, Greenblatt RM. Factors associated with use of dental services among HIV-infected and high-risk uninfected women. J Am Dent Assoc. 2005;136:1242-1255.
- Reznik DA. Perspective oral manifestations of HIV disease. Top HIV Med. 2005;13:143-148.
- Reznik D, Bednarsh H. HIV and the dental team. Dimensions of Dental Hygiene. 2006;4(6):14-16.
- Branson BM, Handsfield HH, Lampe MA, et al. Revised recommendations for HIV testing of adults, adolescents, and pregnant women in health-care settings. MMWR Recomm Rep. 2006;55(RR14):1-17.
- Cleveland JL. Integrating rapid HIV screening into routine dental care. Presented at: Summit on Oral Health Care, HIV and AIDS; October 3, 2008; New York.
- Greenwald JL, Burstein GR, Pincus JP, Branson B. A rapid review of rapid HIV antibody tests. Curr Infect Dis Rep. 2006;8:125-131.
- CDC. HIV counseling with rapid tests. Available at: www.cdc.gov/hiv/pubs/rt-counseling.htm. Accessed July 13, 2010.
From Dimensions of Dental Hygiene. August 2010; 8(8): 20-22, 25.



