
A Complementary Approach
Dimensions speaks with David W. Paquette, DMD, MPH, DMSc, about the relevance of locally delivered antibiotics in the treatment of periodontal patients.
Q. Locally delivered antimicrobials have come a long way since their introduction in the 1980s, yet many clinicians are still confused about the difference between antibiotics and antiseptic agents. Can you explain the difference?
A. Antibiotics have a specificity to their action, either bactericidal (killing action) or bacteriostatic (limiting growth). They interact with bacteria to either lyse (destroy) the cells or cell walls or to limit the bacteria’s metabolic pathway or cell division.
Antiseptics are more nonspecific in their interaction with bacteria. They can inhibit bacteria growth or attachment. Chlorhexidine is a classic antiseptic agent that has limited specificity. It limits cell attachment and inhibits growth but it is much less potent than an antibiotic, such as doxycycline or minocycline.
The main difference between antibiotics and antiseptics lies in the potency and the specificity of their interactions with bacteria.
 Q. What is the mechanism of action of locally delivered antibiotics?
Q. What is the mechanism of action of locally delivered antibiotics?
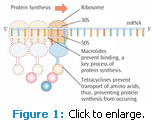
A. Locally delivered doxycycline and minocycline (both in the tetracycline family of antibiotics) inhibit the protein synthesis of bacteria, limiting bacteria growth. Tetracycline-related antibiotics reduce bacteria growth by ceasing protein synthesis in bacteria. Bacteria and human cells conduct protein synthesis on structures named ribosomes. In bacteria, tetracycline crosses the membranes and builds up in the cytoplasm. Tetracycline then binds to one place on the ribosome and prevents an important RNA interaction that turns off the lengthening protein chain (Figure 1). Tetracycline does not damage human cells because it does not accumulate in high enough concentrations to interfere with protein synthesis.
Tetracycline is a family of antibiotic that is traditionally classified as bacteriostatic. However, because doxycycline and minocycline are applied locally in high concentrations, there is enough antibiotic present in the crevicular fluid or in the pocket to kill bacteria (Table 1).1 Antiseptic agents, such as chlorhexidine, use a blocking adherence of the bacteria and/or some minor cell wall changes to limit infection.
Q. Are there any concerns regarding the systemic effects of these antibiotics?
A. Locally delivered antibiotics have gone through rigorous testing before reaching the market. They underwent Phase II and Phase III clinical trials in humans before they received Food and Drug Administration approval (see Table 2).2 They are classified as drugs, which means their absorption, distribution, metabolism, and excretion (pharmokinetics) are extensively documented.
 Another concern regarding the systemic effects of locally delivered antibiotics is whether the drug affects an opportunistic shift in the flora in the oral cavity or in the gut. Locally delivered antibiotics undergo critical evaluation to ensure they do not cause any adverse events related to pathological changes in the oral cavity.
Another concern regarding the systemic effects of locally delivered antibiotics is whether the drug affects an opportunistic shift in the flora in the oral cavity or in the gut. Locally delivered antibiotics undergo critical evaluation to ensure they do not cause any adverse events related to pathological changes in the oral cavity.
When locally delivered antibiotics are used according to their approved labels, there isn’t need for concern regarding their systemic effects. They result in very low systemic concentrations or exposures of the antibiotic when the serum levels are evaluated. The bottom line is this: these products are safe.
The beauty of local antibiotic use is that the antibiotics have primarily a local effect with high concentrations locally and very low concentrations released systemically. Clinicians should always read the label for complete safety information and contraindications.
Q. What should we advise patients who are concerned about developing resistance to antibiotics?
A. These locally delivered antibiotics have low resistance formation. Once placed, there is usually a marked depression in the flora of the bacteria subgingivally. There is often a short-term increase (2 weeks to 3 months) in resistant organisms. In general, locally delivered antibiotics can be repeatedly administered within a 6-month window. There are no data that indicate these agents cause any sort of long-term resistance formation.
In general, clinicians should use these drugs prudently. Locally delivered antibiotics are just one strategy used in the treatment of chronic periodontitis. They do not take the place of good scaling and root planing. Clinicians still need to debride patients as meticulously as possible to break up the biofilm. Locally delivered antibiotics are an addition to this strategy, particularly for use in pockets that have failed to respond to treatment. Repeated administration of locally delivered antibiotics is safe (within a 9-month period, according to the Phase III trials), but clinicians should assess the success of administration before continuing their use.
Q. How should clinicians judge whether the use of locally delivered antibiotics is a success in their patients?
A. I think clinicians are moving away from absolute change in pocket depth as the primary criterion of success. With the use of locally delivered antibiotics, we need to evaluate periodontal stability and reduction of risk of future breakdown. The Phase III trials for locally delivered antibiotics measured mean differences in treatments, which turned out to be quite small—a fraction of a millimeter. But this is not indicative of how patients may respond to this treatment. Some patients may experience significant reductions in pocket depth while others may see no improvement. These mean changes are averages across hundreds of patients within a single group. Clinicians should focus on trying to stabilize the disease process, reassessing patients who are receiving locally delivered antibiotics at 3-month or 4-month intervals. If the desired response has not been achieved at 4 months, readministration may be indicated to increase the likelihood of improvement. The ultimate goal of treatment is to move the patient into a maintenance schedule.
Clinicians should not continuously use locally administered antibiotics in all patients at every visit. In general, clinicians will reach for locally delivered antibiotics when a flare-up occurs. Locally delivered antibiotics are not for whole mouth treatment but rather strategic placement in trouble spots.
Q. Are there specific patient populations that may respond best to the use of locally delivered antibiotics?
A. Data do indicate that locally delivered antibiotics are very effective in patients who have more severe disease; patients with difficult-to-treat areas, such as furcations and posterior sites; and in smokers.3 The most efficacious use of locally delivery antibiotics comes down to prudent treatment planning and risk assessment.
Adjunctive locally administered antibiotics are indicated for patients with localized areas of disease and when there is concern about the level of inflammation or access problems for either patient or clinician. Patients with systemic problems, such as diabetes and cardiovascular disease, may also benefit. Intensive treatment—including scaling and root planing, locally delivered antibiotics, and the extraction of hopeless teeth—may improve systemic outcomes, such as markers of inflammation in the serum. In my opinion, if clinicians are trying to limit oral inflammation in patients, the use of locally delivered antibiotics is helpful.
The views expressed in this interview are those of David W. Paquette, DMD, MPH, DMSc
REFERENCES
- Wilder R, Ryan M. Chemotherapeutics in the treatment of periodontal diseases. Dimensions of Dental Hygiene. 2010;8(6):44-48.
- Glossary of clinical trials terms. Available at: http://clinicaltrials.gov/ct2/info/glossary. Accessed May 25, 2011.
- Paquette DW, Oringer R, Lessem J, Offenbacher S, Genco R, Persson GR, Williams R. Locally delivered minocycline microspheres for the treatment of periodontitis in smokers. J Clin Periodontol. 2003;30:787-794
From Dimensions of Dental Hygiene. June 2011; 9(6): 34, 36, 38.

