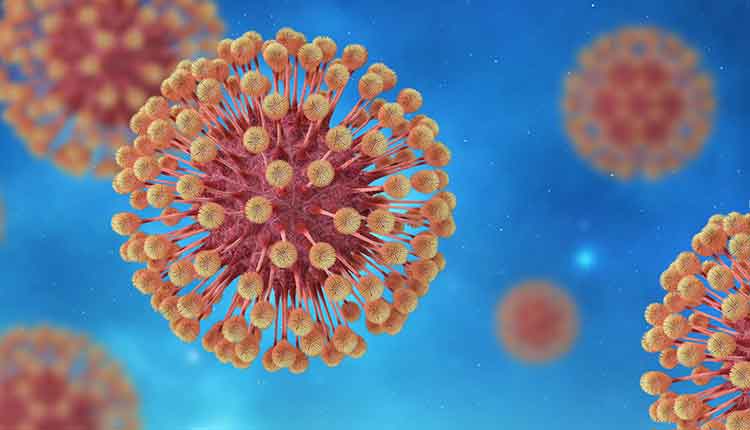
There are more than 100 known herpes viruses, and herpes simplex virus type 1, or HSV-1, is one among the eight known to infect humans. The word “herpes” is a Greek word meaning “to creep or crawl” and its use is in reference to the spreading nature of the symptomatic lesions. HSV-1 causes infections in the mucocutaneous areas of the orofacial region, such as the lips, referred to as herpes labialis but commonly known as “cold sores” or “fever blisters.” Intraoral herpetic lesions may be confused with other ulcerative conditions. Further, uncertainty may exist concerning when to treat patients who present with viral infections such as HSV-1. Therefore, the focus of this paper is to describe the pathogenesis, diagnosis, clinical presentation, and treatment of HSV-1 as oral health professionals will most likely encounter patients seeking treatment while presenting with this condition.
Photo Credit: photoman / iStock / Getty Images Plus

Prevalent Infection
HSV-1 infections are quite common and most often acquired during childhood. Among United States adults, almost 90% are exposed to HSV-1 by the time they are 50. Between 2005 and 2010, the percentage of HSV-1 seroprevalence in the US was 53.9, which is more than three times higher than the seroprevalence of HSV-2. HSV-1 prevalence among women (50.9%) is higher than for men (45.2%).
Photo Credit: privetik / iStock / Getty Images Plus

Viral Evolution
HSV-1 belongs to the alpha (α) herpesvirus subfamily, which also includes other neurotropic viruses such as HSV -2 or genital herpes, and the varicella-zoster virus, which causes chickenpox and shingles. HSV-1 uses the human host for survival and replication. Its typical cellular level life cycle steps are adsorption, penetration, uncoating, replication, assembly, and release. HSV-1 stages can vary among the infected cells wherein the virus can be in latency in some cells and in the replication stage in other infected cells.
Photo Credit: Elitsa Deykova / iStock / Getty Images Plus

The Clinical Course
HSV-1 can cause either primary or reactivation infections. The clinical course of this oral infection depends on age, immune status of the host, and anatomic site of involvement. Primary HSV-1 is manifested in children usually between the ages of 6 months and 5 years as acute (or primary) herpetic gingivostomatitis. Adolescents and adults may also develop acute gingivostomatitis, but it can be less severe, and is more often associated with posterior pharyngitis. HSV infections (primary and recurrent) occurring in immunocompromised individuals tend to be more severe, prolonged, widespread, and more likely to recur.
Photo Credit: syahrir maulana / iStock / Getty Images Plus

Detection and Diagnosis
The diagnosis of oral HSV-1 is typically made by the appearance and location of lesions and patient history. However, not all lesions are readily apparent. The differential diagnosis for primary symptoms includes impetigo, streptococcal pharyngitis, erythema multiforme, acute necrotizing ulcerative gingivitis, Behcet syndrome, herpangina, pemphigus vulgaris, candidiasis, hand-foot-and-mouth disease, herpes zoster, and syphilis. The differential diagnosis for intraoral recurrent herpes is aphthous ulcers. Herpetic lesions tend to have prodromal symptoms, multiple lesions, vesicles precede ulcers, and the location of the lesions are the palate and gingiva. Aphthous stomatitis, in contrast, tends to be single vs coalescing, larger, and almost exclusively on nonkeratinized mucosa such as the buccal mucosa, alveolar mucosa, or floor of the mouth.
Photo Credit: privetik / iStock / Getty Images Plus
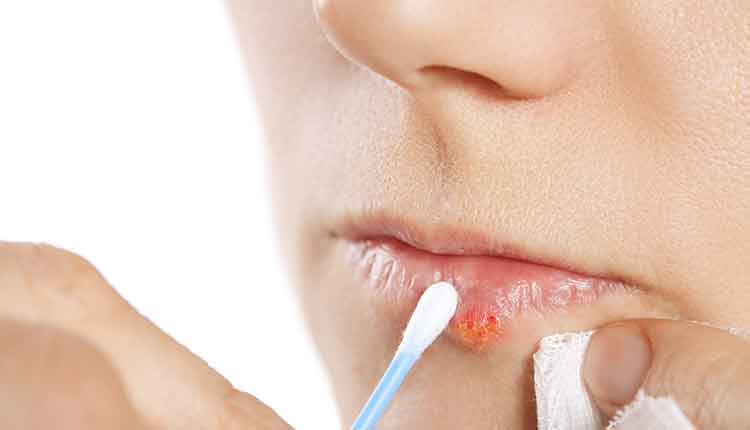
Addressing Herpes Infections
Most HSV-1 infections are self-limiting and resolve within 7 days to 14 days. Treatment consists of over-the-counter products and prescription antiviral medications. These therapies are most beneficial if provided during the prodromal stage within 24 hours to 48 hours of lesion onset. These medications shorten the duration and severity of the infection, but do not eliminate the virus from the body. Supportive therapy, including fluids, rest, and analgesics, are important adjuncts for individuals experiencing primary HSV-1.
Photo Credit: miljko / iStock / Getty Images Plus
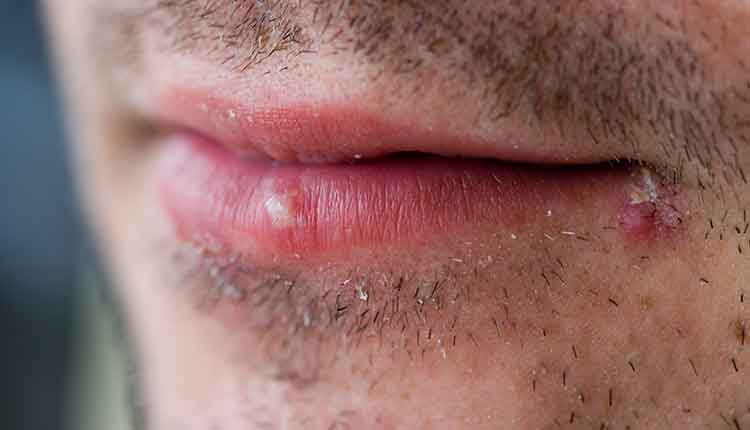
Medical History
Most dental histories include a section that asks about a history of sores or ulcers in the mouth. If a patient answers positively to this question or presents with lesions that appear to be herpetic in nature, oral health professionals should document the location, frequency, and duration of lesions; symptoms associated with those lesions; known triggers; disease course; treatment rendered; complications associated with the lesions and/or treatment; and overall medical history that might correlate with the oral condition. If atypical lesions are found or recurrent intraoral herpes is present in an immunocompromised patient, further diagnostic investigation is warranted using laboratory analysis, and the patient should be referred to an appropriate dental or medical specialist with expertise in this area.
Photo Credit: budgetstockphoto / iStock / Getty Images Plus
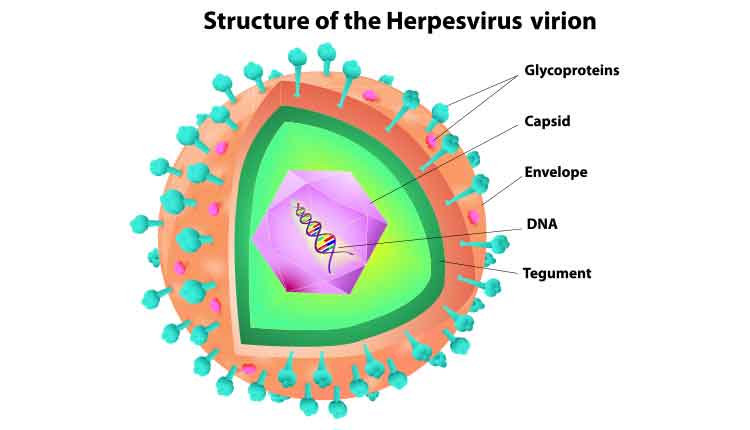
Deferring Treatment
Elective dental and dental hygiene treatment should be deferred for patients who present with active herpetic lesions. Treatment may be uncomfortable and the patient is at risk for the spread of infection or re-infection. Treatment should be postponed until the lesions are completely healed. Oral health professionals are at risk of infection through aerosolization of the virus during dental procedures. Examples of occupational herpetic infections among oral health professionals include herpetic whitlow and herpes keratitis.
Photo Credit: ttsz / iStock / Getty Images Plus

When Team Members Are Infected
If a member of the dental team has an orofacial herpes infection, limit treatment to those patients who are immunocompetent; cover the lesion area with a suitable mask and use a facial shield; change gloves frequently if the hand is brought anywhere near the team member’s mouth; and inform the patient of the team member’s condition and get his or her consent to treat. Herpetic whitlow is highly infectious; therefore, dental team members with this condition should not work until the lesions are healed. In the case of herpes keratitis, viral shedding is high.
Photo Credit: designer491 / iStock / Getty Images Plus
Possibility of Laser Therapy
Lastly, laser treatment has been used to manage recurrent herpes labialis. A review of the literature examining the efficacy of lasers revealed that laser phototherapy appears to decrease pain and the interval of recurrences. High power lasers may also be beneficial in draining vesicles. Other advantages include the absence of drug interactions and side effects. However, none of the laser therapies completely eliminate the virus or recurrence. Additional studies are needed that address efficacy of laser therapy in terms of duration of viral shedding, viral inactivation, and interval of recurrence. Oral health professionals must recognize that while the lip lesion may have been lased, the nature of the virus is such that active virus may be present in the saliva, leaving the patient vulnerable to intraoral infection if elective treatment is rendered.

