 URILUX / E+
URILUX / E+
Study Finds Oral Palate Differences in Patients With Schizophrenia
New research from the University of Nevada, Reno School of Medicine (UNR Med) and University of Maryland School of Dentistry (UMSOD) suggests patients with deficit schizophrenia have a wider oral palate than people with other forms of the disease, as well as those without the mental disorder.
New research from the University of Nevada, Reno School of Medicine (UNR Med) and University of Maryland School of Dentistry (UMSOD) suggests patients with deficit schizophrenia have a wider oral palate than people with other forms of the disease, as well as those without the mental disorder. These findings may lead to a deeper understanding of the neuropsychiatric condition.
The study, “An Early Developmental Marker of Deficit Versus Nondeficit Schizophrenia,” published in Schizophrenia Bulletin suggests the development of patients with deficit schizophrenia begins to change from other groups with schizophrenia as early as the end of the first trimester of pregnancy. “These findings may lead to future research that could potentially reduce the number of individuals who experience this devastating neuropsychiatric condition,” says study coauthor Gary D. Hack, DDS, an associate professor in the Department of Advanced Oral Sciences and Therapeutics at UMSOD.
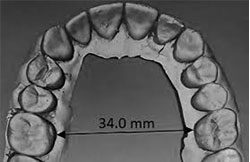
Hack and the study’s lead author Brian Kirkpatrick, MD, chair of UNR Med’s Department of Psychiatry and Behavioral Sciences, worked with an international team on oral palate research comparing individuals with schizophrenia who had or did not have deficit features. Wider palates were only observed in patients with deficit schizophrenia and not in controls or patients with nondeficit schizophrenia. The palate difference in the deficit patients may reflect abnormal brain development during the prenatal period, according to Hack.
Additionally, these physical orofacial differences in patients with schizophrenia suggest the whole-body model of this illness is a more appropriate model to present to patients, family members, and students. This is associated with cardiovascular disease, diabetes, reduced life expectancy, and minor physical anomalies. Individuals with schizophrenia also have been found to have different bacteria in their oral cavities than those without the illness. This suggests changes in the oral microbiome might be associated with the psychiatric illness—which could offer a new tool for diagnosis.
“Our research findings broaden the thinking about the many complex factors that are operating as our brain and face develop, and enhance the holistic nature of human health,” says Hack. “In the meantime, we hope that together as dentists and psychiatrists we can collaborate to improve the dental experience for this population of patients that already faces numerous social and financial barriers, as well as oral health issues.”

