Screening for Sleep Apnea
Obstructive sleep apnea is a medical condition receiving escalated attention due to its associated dangers that range from systemic diseases to fatigue-related accidents.
Obstructive sleep apnea is a medical condition receiving escalated attention due to its associated dangers that range from systemic diseases to fatigue-related accidents. Approximately 5.9 million United States adults are diagnosed with this condition, whereas an estimated 23.5 million cases remain undiagnosed. The latter may be attributed to minimal sleep disorder training across many health care fields. This public health issue calls for dental professionals to increase their familiarity with obstructive sleep apnea, and implement screening protocols and an interprofessional approach to patient care. Doing so can contribute to early sleep apnea diagnosis and treatment that result in improved health outcomes.
Photo Credit: cherrybeans / iStock / Getty Images Plus

Definition
The most common type of sleep apnea, obstructive sleep apnea is characterized by partial or complete narrowing of the pharyngeal airway during sleep. It is defined as a condition in which there is a decrease of oxygen intake (hypopnea) or temporary cessation of breathing (apnea). This chronic, multifactorial, and potentially life-threatening disorder is associated with a reduction in oxygen levels, increased carbon dioxide in the bloodstream, and numerous medical conditions. Obstructive sleep apnea increases the risk of morbidity and mortality, which underscores the need for interprofessional collaboration in diagnosing and managing this condition. Diagnosis and appropriate treatment can also improve coexisting health conditions.
Photo Credit: courtneyk / E+

Risk Factors
Risk factors include age, obesity, gender, hormones, pregnancy, and lifestyle. Prevalence increases with age and plateaus after 60. Obesity affects a large number of individuals with obstructive sleep apnea. A common characteristic of obesity is excess adipose tissue in the head and neck region that contributes to airway obstruction. Due to differences in anatomy and physiology, sleep apnea is more common in men than women. Hormonal changes are associated with prevalence; for example, compared with premenopausal women, a larger number of post-menopausal women have been diagnosed with this condition. Post-menopausal women who do not use hormone replacement therapy are at increased risk. Pregnant women have increased risk, especially during the third trimester when weight gain is greatest.
Photo Credit: SolStock / E+

Symptoms
Symptoms can manifest when the patient is sleeping or awake. Smoking can cause an inflammatory reaction of the pharynx that reduces the airway; similarly, alcohol and sedative use can reduce muscle activity, worsening the symptoms. When sleeping, affected individuals may experience nonrestorative sleep characterized by feelings of insufficient rest. Choking, insomnia, restlessness, unsettling dreams, gastroesophogeal reflux, nocturia, drooling, and excess perspiration are also reported symptoms. Affected individuals may complain of excessive daytime sleepiness.
Photo Credit: Merlas / iStock / Getty Images Plus
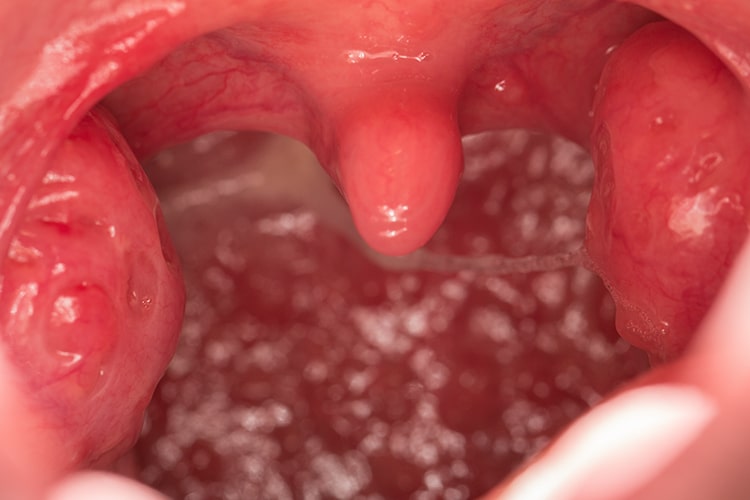
Clinical Features
Frequent clinical findings include a wide tongue that sits toward the tonsil region and a narrow, high-vaulted palate. These anatomical characteristics can reduce the airway passage. A narrow hard palate can decrease nasal airflow. Additional intraoral findings include an elongated soft palate and enlarged uvula, tonsils and adenoids—features that can narrow the airway. Erosion attributed to GERD can occur. Bruxism and edentulism are also linked to this sleep disorder. Affected patients usually grind their teeth and clench their jaw after experiencing an apneic episode. Edentulism can cause a reduction of lower face height, anterior rotation of the mandible, and an unnatural position of the tongue—all of which contribute to airway obstruction.
Photo Credit: PobladuraFCG / iStock / Getty Images Plus

Treatment
Continuous positive airway pressure (CPAP) is the gold standard for treatment, especially in more severe cases. Use of a CPAP facemask improves quality of life, daytime sleepiness, cognitive function, and blood pressure. One of the main issues with this treatment is a lack of patient compliance. Although oral health professionals cannot diagnose obstructive sleep apnea, they can play a part in the fabrication of oral appliances to treat the disorder. Oral appliances are the treatment option most suitable for mild-to-moderate cases. Most commonly used are mandibular-repositioning devices designed to hold the mandible in a forward position, enlarge the area posterior to the tongue, and reduce collapse of the pharynx and palate. Tongue-retaining devices are splints that hold the tongue in place to maintain an open airway.
Photo Credit: grandriver / E+

Therapy and Lifestyle Changes
Myofunctional therapy consists of exercises that target the oral and oropharyngeal structures. Research demonstrates that myofunctional therapy reduces AHI levels by approximately 50% in adults and 62% in children. Additionally, it improves oxygen saturation, snoring, and the adverse outcomes related to sleepiness. Lifestyle modifications are geared toward risk-factor management. Exercise and a healthy diet are encouraged for weight loss; similarly, tobacco cessation and reduced alcohol intake can decrease symptom severity. When the disorder is related to sleep position, positional therapy is recommended to prevent sleeping in a supine position.

