Reversing Caries Lesions With SDF
Recently, silver diamine fluoride (SDF) emerged as a new chemotherapeutic option for caries management in the United States. SDF has long been used in Japan, Australia, and Argentina in caries prevention, and the value of silver ions to treat dental caries has been known for more than a century.
New Chemotherapeutic Option
Recently, silver diamine fluoride (SDF) emerged as a new chemotherapeutic option for caries management in the United States. SDF has long been used in Japan, Australia, and Argentina in caries prevention, and the value of silver ions to treat dental caries has been known for more than a century. SDF currently is designated by the US Food and Drug Administration as a treatment for dentinal hypersensitivity in adults. The application of SDF to treat caries is considered an off-label use, similar to fluoride varnish. As with other forms of off-label use, however, clinicians should use their professional judgment when choosing SDF for caries prevention.
Photo Credit: Lighthaunter / iStock / Getty Images Plus

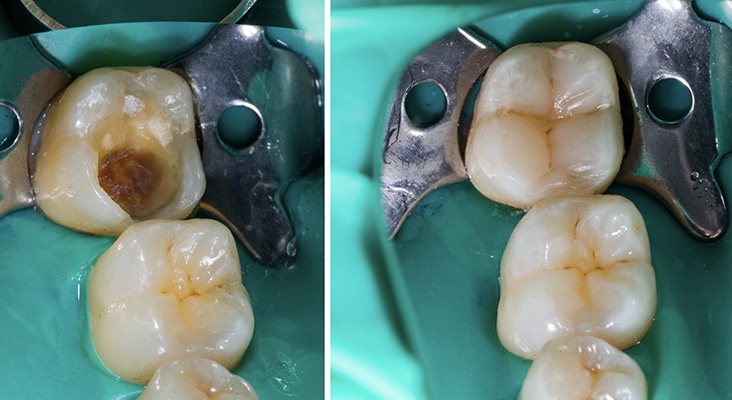
Decreasing Lesion Depth
SDF is an inexpensive and colorless topical agent used to treat and prevent dental caries. Silver is a substantive antimicrobial that limits the reinvasion of cariogenic bacteria after application. The fluoride ions promote remineralization. Upon application of SDF to a decayed surface, a silver-protein conjugate layer forms, which increases resistance to acid dissolution and enzymatic digestion. Treated lesions will increase in mineral density and hardness as lesion depth decreases.
Photo Credit: jabkitticha / iStock / Getty Images Plus
Evidence Base
Several randomized clinical trials evaluated the efficacy of SDF in treating dental caries. Two studies in children demonstrated 91% to 93% caries arrest after 2 years to 3 years of biannual application. Two studies showed 65% to 79% arrest after 2 years to 2.5 years with an annual application. A dose-response relationship was seen, with better outcomes accompanying a higher frequency of application. Reapplication appears to provide additional benefits, as after 1 year, the caries arrest rate plummeted without reapplication and increased with reapplication. Thus, oral health professionals may want to observe the effects of SDF rather than prescribe conventional restorative dentistry prematurely. Studies have reported better caries prevention with an annual application of SDF compared with other topical medicament treatments, such as four times per year applications of fluoride varnish or chlorhexidine varnish.
Photo Credit: Lin Shao-hua / iStock / Getty Images Plus
SDF Placement
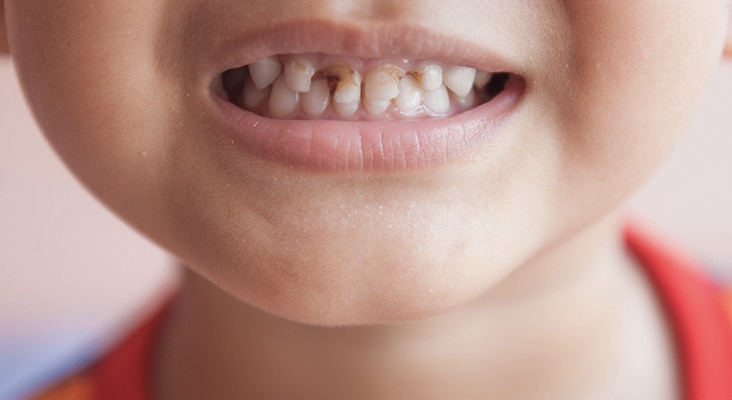
Before placing SDF, oral health professionals should consider whether a patient is appropriate for this treatment. As mentioned earlier, SDF is used “off label” for arresting caries, especially among those in certain populations. SDF will likely benefit patients diagnosed with salivary dysfunctions, those with special health care needs, the underserved, medically compromised individuals, and those with severe early childhood caries. SDF may also be useful for treating lesions that would otherwise be difficult or impossible to treat using traditional methods.9 Furthermore, SDF is likely useful in the enamel pits and fissures surfaces of patients at high caries risk who may not be able to tolerate conventional sealants. SDF can also be used in conjunction with sealants when a lesion is suspected but has not been visualized.
Photo Credit: Primz / iStock / Getty Images Plus

Key Considerations
Clinicians should also consider if repeated SDF application is appropriate. For example, when treating a patient who is not likely to return for a follow-up evaluation and treatment, clinicians need to consider the following options:
- No SDF placement.
- Place SDF only once with the understanding the patient may not return for subsequent applications.
- Place SDF and glass ionomer cement (GIC) sealant/restoration during the same appointment.
Photo Credit: Jummie / iStock / Getty Images Plus
Contraindications
For a tooth that is symptomatic, partially necrotic, or otherwise pulpally involved, SDF may not be beneficial and immediate traditional treatment may be a better approach. With careful application, SDF will not go beyond treated sites, but patients and providers should be aware that SDF will cause stinging if it contacts soft tissue ulcerations or lacerations. Using conventional GIC restorative materials for light curing is not needed and may help reduce SDF’s discoloration effects upon light curing, which is required for resin modified glass ionomer and composite. In situations when patient behavior necessitates short treatment times, a light-cured resin modified glass ionomer may be more appropriate instead of a pure conventional glass ionomer because setting with a light may be faster. Light curing after SDF placement can increase the darkening of the lesion and resin-based restorative materials, but it will not make it as dark as amalgam.
Photo Credit: ChrisGorgio / iStock / Getty Images Plus
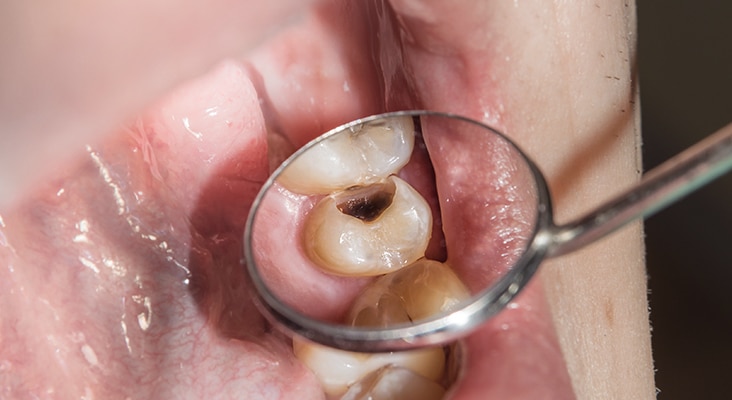
Application
Arresting a caries lesion with SDF may be beneficial when traditional methods are not likely to be successful. In the case of a patient with multiple caries lesions that cannot be immediately restored, SDF can slow the disease process and decrease sensitivity until definitive restorative care can be performed. Repeated application of SDF may help preserve tooth structure. In such cases, reapplication has been recommended at least biannually until a tooth exfoliates, is extracted, or the tooth is restored. In situations where restorations are not an option, repeated applications of SDF may be the best option.

