Expanding the Dental Hygiene Scope of Practice
Over the past decade, legislatures across the United States have grappled with scope of practice issues for health professions, including dental hygiene.
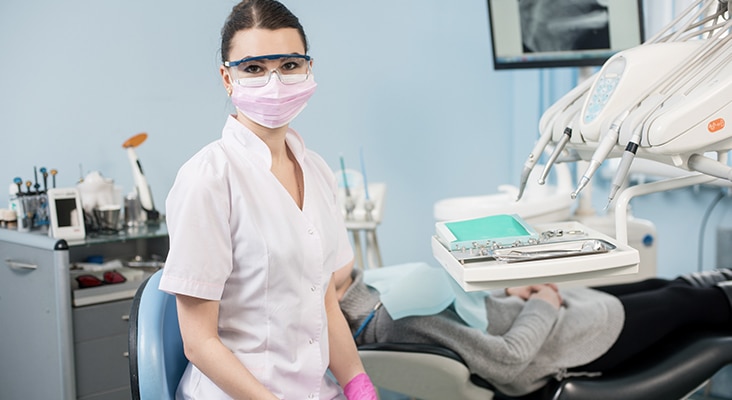
Over the past decade, legislatures across the United States have grappled with scope of practice issues for health professions, including dental hygiene. Almost every state has provided new permissions or enabled conditions for broader practice in response to new technology, improved science, novel dental materials, or alternative methods for delivery of care. Downstream effects of these changes include opportunities for innovative dental hygiene practice. In addition, the fundamental shift in health care delivery away from the medical paradigm of identifying and treating existing disease toward early intervention in prevention of disease processes has had collateral effects on dentistry and dental hygiene. Dental hygienists’ competencies are grounded in patient education, motivational interviewing, and preventive and prophylactic clinical services. This expertise has positioned the profession to play a pivotal role in efforts to improve the oral health of the US population. Dental hygienists are now more commonly viewed as primary preventive oral health specialists with separate and critical responsibilities in the oral health care continuum of care.
Photo Credit: anatoliy_gleb./ iStock / Getty Images Plus
Other Avenues of Care
Dental hygiene has evolved from a somewhat limited role in private dental practices to multiple functions in a variety of dental, medical, educational, and social service provider organizations. While many dental hygienists continue to offer important services in private practice settings, an increasing number are embracing opportunities for expanded practice. These broader opportunities offer different ways in which dental hygienists can serve patients and provide new portals of entry for patients to the oral health care delivery system. One critical function for dental hygienists is to act as a first point of patient contact with oral health services, providing referral to and consultation with other members of clinical dental teams. The emergence of team-based service delivery in oral health care represents an environmental shift that encourages more flexible use of the competencies of various health professions to enable high-quality, high-value, and efficient patient-centered services. Dental hygienists working in skilled nursing facilities consult closely with medical and nursing staff and in school-based programs, they work with administrative staff, nurses, and teachers. Teledentistry teams often include dental hygienists, as well as information technology staff who are critical to delivering remote consultation services. The skills needed by dental hygienists to work effectively with different professional disciplines are similar to those needed to provide compassionate patient care, including communication and interpersonal skills, flexibility, conflict management, cultural awareness, empathy, ethics, and critical-thinking and problem-solving skills.
Photo Credit: artisteer./ iStock / Getty Images Plus

Legislative Roadblocks
A fundamental change to the effective use of dental hygienists is the ability to provide clinical services with less direct oversight in settings other than traditional dental practices. Legislators and regulators recognize that the traditional delivery system is not designed to meet the needs of underserved populations and that barriers to obtaining oral health services are overcome when services are delivered in community settings where patients are commonly found.
Photo Credit: xavierarnau./ iStock / Getty Images Plus

Care Delivery
These changes appear to be impacting care delivery. According to the School-Based Health Alliance National School Based Health Care Census, an analysis of 20 years of census data found that the proportion of school-based health centers (2,584 in 2016-2017 academic year) that employed oral health professionals in the health clinic increased from 9% in 2001-2002 to 28% in 2016-2017. School districts throughout the US without fixed clinics are collaborating with mobile dentistry providers to meet the needs of children with limited access to oral health services. For example, a dental hygienist-owned nonprofit organization, Future Smiles, provides services in approximately 50 schools in Nevada using a mixed model of care delivery. In some schools, care is provided in dental chairs within the school during the academic year; in others, dental hygienists use portable equipment.5 Two of the school campuses have separate buildings for fixed operatories where dental hygiene services are provided on a year-round basis. Approximately 5,000 children receive clinical services annually and another 20,000 children receive oral health education.
Photo Credit: maroke./ iStock / Getty Images Plus

Public Health
Public health dental hygiene practice is available in almost every state, although the pathways to the designation, allowable services, and required levels of supervision vary by jurisdiction. Public health dental hygiene is defined differently across states; it may take the form of collaborative practice, a limited access permit, an extended care permit, or expanded practice dental hygiene. For example, dental hygienists may qualify for independent practice in Colorado and Maine, unsupervised practice with an expanded practice permit in Oregon, stepwise extended care permits in Kansas, public health dental hygiene in Massachusetts and Nebraska, collaborative practice in New Mexico, and alternative practice in California. These agreements enable qualified dental hygienists to offer direct access to patients who have not had a recent dental visit and to provide a full range of educational, preventive, and prophylactic dental hygiene services in the community.
Photo Credit: Hibrida13./ iStock / Getty Images Plus

New Workforce Models
Several states have enabled new oral health workforce models, generically labeled as dental therapy, which allow professionals who have trained in an accredited curriculum and program and passed clinical and written examinations to provide basic restorative services, primary tooth extractions, and preventive oral health services to underserved patients. In Minnesota, an advanced dental therapist may also carry a dental hygiene license and provide a broad range of preventive and restorative services including pulpotomies on primary teeth and tooth extractions under the general supervision of a dentist. Maine, Vermont, Arizona, New Mexico, Nevada, and Connecticut have also passed legislation enabling dental therapy licenses to dental hygienists who will be required to pursue further education and training for licensure.

