
Elevate Patient Comfort and Confidence in Gingival Grafting
Incorporate a palatal stent technique using thin plastic vacuform material and collagen to enhance patient comfort, control bleeding, and ensure predictable outcomes in gingival grafting procedures.
In this age of advanced technology and high patient expectations, it can be useful for clinicians to support the benefits of gingival grafts, and express confidence the procedure can be both beneficial and comfortable. This will help alleviate patient concerns, because a gingival graft is one of the most predictable surgical procedures in periodontics.1
Providers who embrace this technique in gingival grafting can deliver more complete care, and patients can start telling positive stories instead of negative ones. By making a palatal stent out of a thin plastic vacuform material and covering the wound under the plastic with collagen, clinicians and patients can enjoy predictable, evidence-based results in both comfort and healing. The technique is as follows:
- Assure patients of the benefits (namely, increased comfort and diminished chance of postoperative bleeding) derived from the palatal stent.
- Take a maxillary impression at the consultation appointment and pour a model.
- Make a vacuform stent with 0.20-mm material prior to the surgical appointment.
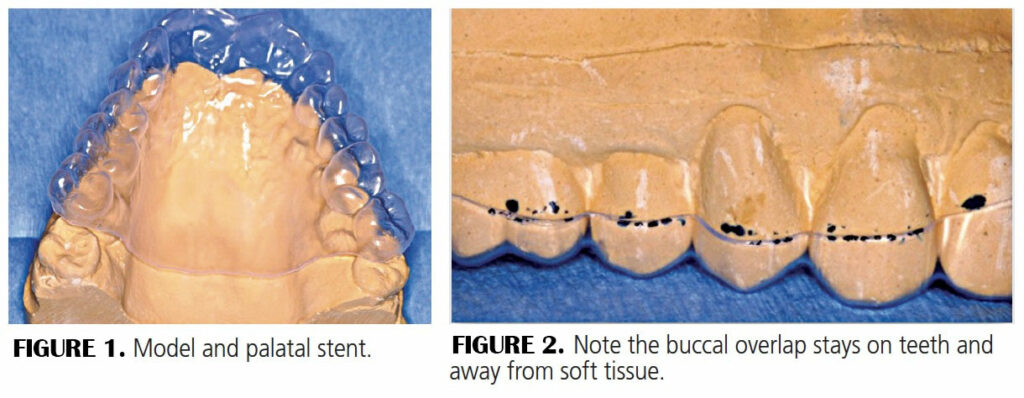
- Trim the plastic to avoid the soft palate, as with a denture, and trim to overlap on the buccal surfaces of teeth only 2 to 3 mm to stay off the soft tissues (Figure 1 and Figure 2). Trimming to avoid the soft palate will ensure the gag reflex will not come into play.
- At the surgical appointment, check the fit before starting the procedure to ensure the trimming was accurate.
- After surgery, place two layers of the collagen material of choice over the donor site, and cover it with the stent. Make certain the stent contacts and gently holds the collagen in place (Figure 3).

Besides significantly less pain, a major benefit is that collagen will result in almost immediate clotting. Consequently, since the stent holds the collagen against the donor site, bleeding is visibly under control before the patient leaves the office. In addition, with the knowledge the collagen will remain in place overnight, clinicians can be confident they have eliminated one serious potential complication of a graft from the palate — namely, postoperative bleeding from the donor site.
Postoperative instructions for the patient (which should always be given in writing) are:
- Leave the stent in until the next morning.•
- At that time, remove it and resume brushing and flossing as normal, but avoid the graft sites (both donor and recipient). Let the patient know it is OK if the collagen falls out.
- Leave the stent in full time for the first week, removing it only for brushing and flossing.
- After the first week, use the stent while eating and sleeping until feeling comfortable without it.
- At this point, the stent is only used for palatal comfort (if and when needed). It will not affect the outcome if used less frequently.
- If a second graft is planned, ask the patient to save the stent.
Discussing grafting techniques to help patients understand the benefits will result in greater acceptance, and higher levels of patient comfort, compliance, and satisfaction. In turn, clinicians can improve patients’ periodontal health and achieve better restorative results by predictably preventing recession in areas where the gingiva may be thin.
A careful and thoughtful explanation of the approach described here should help overcome possible patient objections to gingival grafting. This method might also enhance relationships between general dentists and periodontists by sharing this technique tip if they are not already using it.
Reference
- Hagorsky U, Bissada N. Clinical assessment of free gingiva graft effectiveness on the maintenance of periodontal health. J Periodontol. 1980;51:274–278.
This information originally appeared in Kohner J. Maintaining palatal comfort following gingival grafting. Decisions in Dentistry. 2020;6(10):10-12.

