The Biology Behind Periodontal Disease Phenotypes
The standard clinical periodontal examination begins with the evaluation of clinical and radiographic signs and symptoms to determine the extent and severity of gingival and periodontal tissue damage.
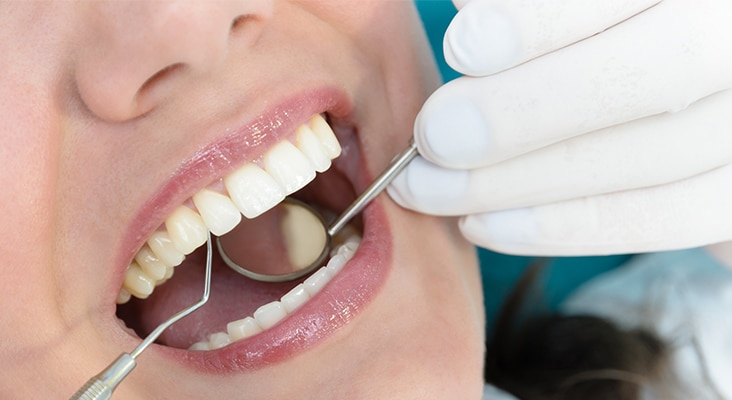
The standard clinical periodontal examination begins with the evaluation of clinical and radiographic signs and symptoms to determine the extent and severity of gingival and periodontal tissue damage. With this, the clinical presentation of periodontal disease, or clinical phenotype, follows clinical features of inflammation, redness, edema, and bleeding on probing, and loss of periodontal attachment, as evidenced by probing depth, attachment level, gingival recession, and alveolar bone loss. These recognized techniques alone are insufficient. The limited success of prognosis in periodontal disease progression in some patients is due to the clinical appearance not reflecting the biology at the biofilm–gingival interface.
Photo Credit: oneblink-cj / iStock / Getty Images Plus
Chronic Inflammation
Chronic adult periodontitis is a bacterially induced chronic inflammatory disease that destroys the attachment apparatus supporting the teeth. Experimental evidence implicates bacterial plaque as the primary etiological factor for initiating periodontitis. Concomitantly, specific periopathogenic bacteria and immune-inflammatory mechanisms are involved in periodontitis in complex interactions. In the model of periodontal pathogenesis including this concept, the bacteria activate an immune-inflammatory mechanism. This adversely affects the host control of the bacterial challenge, as well as the remodeling of osseous and gingival structures. Various environmental and genetic factors are changing the clinical appearance of periodontal disease in a patient.
Photo Credit: Staras / iStock / Getty Images Plus
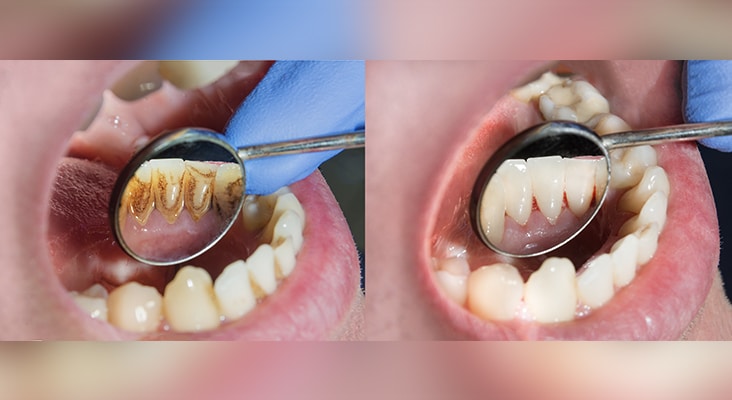
Gingivitis Prevention
Effective and persistent removal of dental plaque is conditional to achievement and maintenance of oral health. According to the nonspecific plaque hypothesis, any reduction of the noxious load of plaque and its bacterial byproducts adjacent to gingiva will reduce gingivitis. As supragingival plaque matures and progresses to subgingival plaque, any decrease in bacterial deposits will prevent gingivitis. The maintenance of noninflamed gingiva will help prevent chronic periodontitis. As the dental biofilm accumulates, oral hygiene helps to control the amount of bacterial deposits on the dental structures and their apical migration. This constitutes primary gingivitis prevention.
Photo Credit: undefined undefined / iStock / Getty Images Plus

Mouthrinse Solutions
Bisbiguanide compounds, like chlorhexidine gluconate and alexidine, are the most effective mouthrinse ingredients used to inhibit plaque formation, especially after mechanical removal of the biofilm. Mouthrinses containing essential oils (thymol, menthol, eucalyptol, and methyl salicylate), as well as those with cetylpyridinium chloride have been shown to be effective in decreasing supragingival plaque and gingivitis. While not an antiseptic, mouthrinse containing delmopinol helps to prevent plaque from adhering to the teeth and gingiva.
Photo Credit: AndreyPopov / iStock / Getty Images Plus

Interdental Cleaners
While patients may have an interdental aid preference, factors such as gingival biotype; anatomy of the embrasure between teeth; tooth location in the dental arch and alignment; and patient’s dexterity, motivation, and compliance should be considered when giving interproximal oral hygiene instructions. Most studies show improvement of plaque scores when comparing patients using interproximal brushes with the use of floss.
Photo Credit: Chalabala / iStock / Getty Images Plus

Patient Education
Research asserts that one single oral hygiene instruction by a dental professional can positively affect the prognosis of periodontitis in a patient for about 6 months afterward. This is in congruence with the 3-month to 6-month recare interval. This confirms the importance of patient education by oral health professionals in the prevention of periodontal diseases.


[…] post The Biology Behind Periodontal Disease Phenotypes appeared first on Dimensions of Dental […]