Air Polishing Basics
Air polishing as a device to remove extrinsic stain and dental plaque biofilm from the teeth first became available in 1976.
Air polishing as a device to remove extrinsic stain and dental plaque biofilm from the teeth first became available in 1976. The device operates through the movement of pressurized air via the powder bowl, which forces a stream of air and powder toward an outlet, where it then combines water with the air and powder to form a slurry. The abrasiveness of the slurry is influenced by the powder particle size, shape, and hardness, measured on the Mohs scale of mineral hardness from 1 to 10. Hardness is determined by whether a substance can be scratched by another substance of known hardness. A score of 1 is represented by talc and 10 by diamond. The effectiveness of air polishing is increased by higher air pressure and water settings.
Photo Credit: rendeep / iStock / Getty Images Plus

Sodium Bicarbonate Powder
A specially formulated version of sodium bicarbonate was the original powder used in air polishing devices and is still the most common powder on the market today. While sodium bicarbonate is nontoxic and water soluble, early evaluations of its effect on hard and soft tissues resulted in recommendations for use on enamel, but not on cementum and dentin. Sodium bicarbonate encompasses particle sizes up to 250 μm, with an average size of 74 μm and a Mohs hardness index of 2.5. With these characteristics, studies demonstrated that it could be used safely and effectively on enamel. Studies examining the use of sodium bicarbonate for air polishing, however, showed extensive loss of root surface when used on cementum and dentin. The larger and harder the particle impacting the root surface, the greater the erosion of cementum or dentin through the increased size of the defects created. More recent studies have confirmed the same results with sodium bicarbonate air polishing.
Photo Credit: Geo-grafika / iStock / Getty Images Plus

Restorative Materials
A further consideration is the care that must be taken when air polishing restorative materials. Sodium bicarbonate air polishing may erode the surface of restorative materials, resulting in a rough, dull appearance. Yet at least one study has found that sodium bicarbonate air polishing was less abrasive to amalgam, composite, and ceramic surfaces than piezoelectric ultrasonic devices. When considering the results of studies evaluating the effects of air polishing on restorative materials, consideration must be given to the fact that these are invariably conducted as in vitro studies. Air polishing is more effective than rubber cup polishing when cleaning the tooth surface prior to etching for sealant placement, resulting in enhanced bond strength. Once placed, however, air polishing of sealants should be avoided as it can lead to loss of sealant material.
Photo Credit: ayo888 / iStock / Getty Images Plus

Less Abrasive Than Prophylaxis
Despite these limitations, supragingival air polishing is beneficial for patients undergoing routine prophylaxis because supragingival polishing with prophy paste is more abrasive than the use of air polishing powder. Prophy paste contains pumice, which has a Mohs hardness index of 6. Air polishing is also less time consuming than removing stain and plaque biofilm with the traditional rubber cup polish and hand instrumentation. The decrease in appointment time may increase patient comfort and acceptance of the procedure and result in less operator fatigue.
Photo Credit: rekemp / iStock / Getty Images Plus

Glycine Powder Air Polishing
Glycine powder air polishing (GPAP) was developed for use in subgingival air polishing. As such, a powder was needed that would not damage root surfaces. Glycine is an amino acid with a particle size of 20 μm and a Mohs hardness index of 2.1 Research has shown that glycine powder is significantly less abrasive than sodium bicarbonate powder when used on root surfaces. It is also less damaging to restorative materials. GPAP use results in minimal erosion of the gingival tissues at the time of treatment compared to sodium bicarbonate powder air polishing or hand instrumentation.
Photo Credit: cdascher / E+
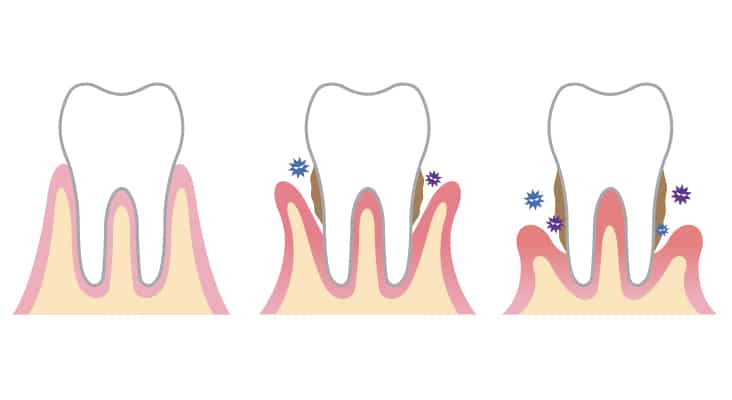
Periodontal Maintenance
Supra- and subgingival air polishing does not remove calculus and, therefore, is not a replacement for ultrasonic and/or hand instrumentation. However, plaque biofilm disruption is a critical aspect of periodontal maintenance appointments. The ability of GPAP to effectively remove subgingival plaque biofilm compared to hand instrumentation adds an alternative modality for this procedure to the dental hygienist’s armamentarium. In addition, a study comparing GPAP to ultrasonic instrumentation during maintenance therapy found that GPAP was equally as effective in reducing periodontal bacteria immediately and 2 days after treatment in patients with moderately deep pockets (5 mm to 8 mm). Furthermore, both treatments demonstrated significant reductions at 2 months in clinical parameters: bleeding on probing, pocket depth, and attachment levels.
Photo Credit: yomogi1 / iStock / Getty Images Plus
Deciding Which Modality to Employ
When considering which modality to employ during periodontal maintenance, several other factors should be considered. A treatment time of 5 seconds per site is recommended with GPAP to ensure that gingival erosion is minimal. Subgingival air polishing requires, in addition to the proper powder selection, the use of a nozzle specifically designed for subgingival insertion. The improper adaptation of handpieces designed for supragingival air polishing can lead to iatrogenically induced facial emphysema when air is introduced into the subcutaneous tissues. Symptoms include facial swelling, tenderness, and pain. Patient acceptance of the procedure has been evaluated in a systematic review that included nine studies, six of which compared GPAP to either hand instrumentation or an ultrasonic device. The conclusion was that patients experienced less discomfort during treatment with air polishing devices compared with hand instruments or ultrasonics.


I use the Hu-Friedy Air Flow Plus powder which uses erythritol. Erythritol has smaller particles than glycine.
“New PLUS powder from Hu-Friedy offers comfortable and efficient supra and subgingival biofilm disruption, as well as light to moderate stain removal. Made from erythritol, a sugar alcohol with a grain size of just 14 microns, PLUS powder is safe to use on virtually all surfaces, including soft or hard tissue, restorative materials, orthodontic appliances, and implants.”