
Xerostomia and Oral Disease
Xerostomia or perceived dry mouth has been described as “the symptom that acts like a disease.”
This course was published in the November 2011 issue and expires November 2014. The author has no commercial conflicts of interest to disclose. This 2 credit hour self-study activity is electronically mediated.
EDUCATIONAL OBJECTIVES
After reading this course, the participant should be able to:
- Define xerostomia.
- Discuss the properties of saliva.
- Identify different causes of xerostomia.
- Detail the complications of xerostomia.
- Explain the strategies for reducing oral diseases related to xerostomia.
Xerostomia or perceived dry mouth has been described as “the symptom that acts like a disease.”1 The perception of dry mouth may be attributed to both salivary and nonsalivary causes.2,3 True dry mouth is associated with salivary gland hypofunction.3 The most common cause of xerostomia is the chronic use of medications that alter neural control of salivation, resulting in glandular hypofunction.4,5 Xerostomia, however, may also be associated with psychological conditions, such as depression and anxiety. This association is especially problematic because these conditions are commonly treated with medications that cause salivary hypofunction.6
Living with a dry mouth poses significant challenges for both patients and clinicians. The symptoms of xerostomia can cause patients to experience difficulties with routine activities of daily living. Patients with xerostomia often experience changes in taste that directly influence their food choices, which may lead to problems of the oral hard and soft tissues, as well as poor nutrition. Physical difficulties due to loss of oral lubrication make it difficult or impossible to chew certain foods, and may make wearing dental prostheses uncomfortable or traumatic to the oral tissues. Swallowing may be challenging, increasing the need to drink more fluids while eating, and raising the risk of choking due to the inadequate breakdown of foods. Loss of lubrication may also contribute to digestive problems.
Patients may begin to avoid interpersonal situations that involve meals because of difficulties with eating, leading to social isolation and depression. For others, xerostomia is mainly an annoyance that causes chronic discomfort.
Untreated salivary hypofunction also leads to a multitude of oral diseases such as caries, fungal infections, and gingival disease. Patients may also experience increased viral infections and traumatic lesions of the oral mucosa. Managing daily oral hygiene becomes a greater task for people with xerostomia, especially for those who cannot change the contributing factor(s) that cause the condition.
NEURAL CONTROL OF SALIVATION
During resting conditions, the average adult secretes approximately 500 ml (about 2 cups) of saliva in 24 hours. Most secretions are mucous-based, and are secreted almost entirely during waking hours. Little secretion occurs during sleep.7,8 The total daily secretion of saliva ranges from 800 ml to 1,500 ml, with an average value of 1,000 ml. 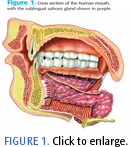
Secretion of saliva is regulated by both divisions of the autonomic nervous system in response to mechanical stimulation (eg, chewing, speaking, and muscle movement) or chemical stimulation (eg, gustatory or taste sensation). Stimulated and unstimulated flow rates vary in response to the degree or intensity of stimulation, circadian rhythms, demand (eg, initiation of digestion), and the health status of the individual. Flow rate and salivary composition also differ by type and duration of stimulation.4,9
Stimulation of the parasympathetic nervous system, which initiates digestion, produces the fluid component of saliva that is high in volume and ions, but relatively low in protein. This watery saliva is known as serous saliva, which is formed by parenchymal cells and secreted by the parotid glands. Parasympathetic stimulation also produces vasodilatation of the blood vessels supporting the salivary glands (Figure 1) as a part of salivary secretion.10 Parasympathetic effects on salivation are stronger and last longer to aid in the breakdown of the bolus of food in preparation for swallowing and digestion.4,9
Conversely, excitation of the sympathetic nervous system produces a flight-or-fight response, producing saliva that is high in proteins, but low in volume. Sympathetic stimulation has a direct effect on glandular cells, resulting in the formation of a more concentrated saliva that contains more mucous and extra enzymes, but also causes vasoconstriction of the blood vessels that supply the glands, reducing rate of secretion.10 Sympathetic stimulation also inhibits flow rate due to central nervous system influences from the higher centers of the brain that control the salivary centers, thereby diminishing reflex activity.10 The texture and consistency of this saliva is rope-like and thick with mucous, and is known as mucinous saliva. Sympathetic stimulation of the submandibular and sublingual glands produces some serous, but mostly mucinous secretions that make the mouth feel sticky to some and dry to others. An example of this sensation is the dry mouth that is perceived while feeling anxious or frightened.
The submandibular glands and sublingual glands are often referred to as mixed because of their ability to secrete both serous and mucinous saliva; however, the mucinous form dominates. The sublingual glands secrete very little to the overall production of saliva, while the minor salivary glands in the labial mucosa secrete approximately 10% of the overall volume of mucinous saliva, which is essential for maintaining oral mucosal integrity and lubrication.9 Because salivation is controlled by the nervous system, any diseases that alter the number of receptors stimulated by neurotransmitters, the function of these receptors, or signal transduction and neurocommunication may affect salivary function.11
Table 2. Drug Classes Associated with Xerostomia17
• Anorexiants
• Anti-inflammatory analgesics
• Antiacne agents
• Antinauseants
• Antianxiety agents
• Antipsychotics
• Anticholinergics/antispasmotics
• Bronchodilators
• Anticonvulsants
• Decongestants
• Antidepressants
• Diuretics
• Antidiarrheals
• Drugs used to treat Parkinson’s disease
• Antiemetics
• Muscle relaxants
• Antihistamines
• Narcotic analgesics
• Antihypertensives
• Sedatives
PROPERTIES OF SALIVA
Saliva is a highly complex body fluid that is associated with numerous critical physiologic functions (Table 1). Saliva is the first digestive enzyme in the gastrointestinal tract and is essential to overall digestion. It is also necessary for good taste sensation, as the fluid helps carry flavors from foods and beverages to the taste bud receptors that then relay information for central taste perception. The fluid also helps with overall oral cleansing following eating.9
Saliva contains a variety of mucins, which are glycoproteins that lubricate mucous membranes, and protect tissues from injury and ulceration during eating, speaking, and performing oral hygiene, and while wearing oral appliances and prosthetic devices. Mucins protect against dehydration and limit microbial adhesion and colonization of microorganisms to oral tissues.8 They also prevent penetration of some carcinogens, toxins, viruses, and irritants through the oral mucous membranes, and encourage soft tissue repair, in addition to maintaining salivary viscoelasticity.12
Bicarbonate and phosphate are electrolytes that serve as salivary buffers for regulating both oral and biofilm pH. Buffers are important for two reasons: first, they neutralize the acidic environment produced by acidogenic organisms, which limits demineralization of tooth enamel; and second, they reduce bacterial colonization by altering their preferred acidic environment.
Bicarbonate is the primary buffer at high flow rates, and calcium and phosphate keep the saliva saturated with hydroxyapatite.9 Other important oral buffers include urea and ammonia.
Saliva maintains balance of the oral ecosystem with immunologic, nonimmunologic, and antimicrobial processes to prevent microbial colonization and reduce bacterial adherence to the teeth and oral tissues.13 Both the acquired pellicle and the dental plaque biofilm contain proteins derived from saliva that aid in controlling pathogenesis of oral diseases.14 There are several mechanisms that help prevent tissue destruction and oral disease caused by pathologic bacteria that reside in the oral cavity.
First, the action of continuous salivary flow clears the mouth of pathologic bacteria, as well as food particles that provide a source of fuel and metabolic support for these organisms. Second, saliva contains numerous products that help kill bacteria. Third, saliva contains large amounts of protein antibodies that also destroy bacteria.7,16 Finally, saliva is essential to maintaining the structural integrity of tooth enamel by limiting demineralization and promoting remineralization. The primary factors that affect enamel hydroxyapatite are the free concentrations of salivary calcium, phosphate, and fluoride, and the level of oral pH.14–16 Salivary fluoride levels offer a caries-protective effect, although basal fluoride levels in saliva are normally very low. Exposing the oral cavity to fluoride increases salivary fluoride level, which gradually diminishes according to the rate of flow and the volume of saliva before and after swallowing.16 By far, the caries-protective effects of saliva are attributed to rate of flow and the ability of saliva to clear the oral cavity of food substances that fuel bacterial growth. All of these factors provide protection of the enamel from demineralization.8,14–16
DRUG-INDUCED XEROSTOMIA
There are multiple etiologies for xerostomia, but medication use is the most frequent cause. More than 500 different drugs induce dry mouth as a side effect (Table 2).17 Older adults are most affected due to the synergistic effects of taking multiple medications. Clinicians, however, should be aware that children also experience drug-induced xerostomia, especially those who are taking neuropsychiatric medications for depression, anxiety, obsessive-compulsive disorders, and medications for attention deficit hyperactivity disorder (ADHD). Both stimulated and unstimulated salivary flow rates decrease when the number of medications taken is increased.4,18,19
The most common mechanism of drug-induced xerostomia is alteration of the neural pathways that stimulate salivary gland secretion.5 Because parasympathetic nerves demonstrate a cholinergic (para sympathetic) action on salivation leading to an increase in fluid volume, anticholinergic drugs reduce the volume of serous saliva. Common anticholinergic drugs include some antihypertensives, antihistamines, antidepressants, antipsychotics, antiemetics, anti spasmotics, and drugs that treat Parkinson’s disease.4,9
Sympathetic stimulation of salivation produces less volume, and viscous, mucinous saliva. Drugs that mimic the sympathetic nervous system include decongestants, bronchodilators, appetite suppressants, and amphetamines used to treat ADHD.4 Drugs may also exert their neural effects in the frontal cortex of the brain by stimulating adrenoreceptors that inhibit central salivary nuclei.4,18 Salivary flow also may decrease in the presence of drugs that vasoconstrict the blood supply to the glands.18,20
Other mechanisms of drug-induced xerostomia are not neurally-mediated. Inhaled medications cause the sensation of dryness due to a topical effect without actually reducing flow. Diuretics may produce symptoms of dryness without any alteration in flow, such as loop diuretics, or true dehydration due to loss of fluid volume and electrolytes.5,18,20
Many drugs used for chemotherapy cause changes in both salivary flow rates and composition. Severity of xerostomia varies with the type and number of agents used and the duration of treatment. Exactly how antineoantineoplastic drugs damage salivary tissues is unknown; however, increased salivary drug concentration and prolonged contact with the oral epithelium is associated with low salivary flow rates. Chemotherapy causes systemic immunosuppression that decreases the concentration of salivary immunoglobulins, which leads to microbial overgrowth, manifesting as mucositis and oral infections.4,9
Radiation to the head and neck area also alters salivation, as salivary gland tissue is highly sensitive to its effects. The degree of xerostomia is dose-dependent and is also related to the amount of salivary gland tissue affected. Every effort must be made to spare a portion of the salivary glands, especially the parotid glands, whenever possible to avoid long-term oral complications. Salivary flow from glands on the contralateral side may increase in an attempt to compensate for what has been lost on the affected side. Recovery of the less radiosensitive mucous glands is helpful for residual lubrication after treatment. After radiation, saliva turns yellowish-brown in color and is more viscous. Buffering capacity is greatly reduced, resulting in a more acidic pH; this environment encourages microbial overgrowth and increased oral disease.
The risk of post-irradiation caries is a life-long concern for patients who have undergone cancer treatment.4,9
SALIVARY GLAND DISEASE
When assessing the medical history of a patient with xerostomia, other potential causes must be considered. First, the clinician should investigate whether a neurological condition or impairment, such as stroke or residual nerve damage from an injury, maybe causing or contributing to the problem. Palpation of the salivary glands may reveal enlargements or irregularities in shape, requiring additional evaluation to detect and diagnose salivary tumors.
Human immunodeficiency virus (HIV) salivary gland disease affects up to 8% of individuals infected with the virus, and most frequently affects the parotid glands.4 Clinicians will observe bilateral parotid enlargement and patients will typically report xerostomia. These complications usually arise late in the course of HIV infection, but are occasionally among the first signs of HIV disease. Infection in the glands may also contribute to the enlargement; however, enlargement may also be caused by Kaposi’s sarcoma and nonHodgkin’s lymphoma associated with HIV infection. Many of the antiretroviral medications used to treat HIV infection also cause xerostomia.4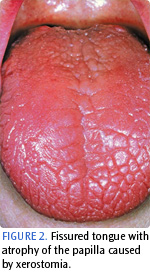
Hepatitis C salivary gland disease affects up to 33% of individuals infected with the virus, and xerostomia is the predominant symptom.4 Histologically, tissue changes in the glands closely resembles those observed with Sjögren’s syndrome, but with less inflammation.4
Autoimmune diseases are also closely associated with salivary gland disease, especially Sjögren’s syndrome, which is characterized by an intense lymphocytic infiltration of the exocrine glands. Lymphocytic infiltration destroys the salivary glands, which decreases production and secretion of fluids. Symptoms of Sjögren’s syndrome include chronic dry eyes and mouth. International diagnostic criteria for Sjögren’s syndrome include measures of salivary gland inflammation and autoantibodies in the serum. Persistent glandular swelling is a characteristic sign of this disease, but may also indicate the presence of lymphoma or bacterial infection. The xerostomia reported by this population is the direct result of local salivary tissue inflammation and fibrosis due to lymphocytic invasion; however, there is also autoimmune-mediated interference with both neurotransmitter and receptor function. Biopsy of the minor labial salivary glands further confirms the diagnosis. Interestingly, these biopsies reveal that as much as 50% of the acinar cells remain intact, thus allowing patients to benefit from salivary-stimulating medications.21,22
Many autoimmune diseases are associated with salivary gland disease and xerostomia, including thyroiditis, rheumatoid arthritis, chronic graft versus host disease, amyloidosis, and cystic fibrosis.4,23,24 Type 1 diabetes also contributes to xerostomia because elevated A1C levels and fasting blood glucose levels lead to increased glucose clearance by the kidneys, resulting in dehydration.25
COMPLICATIONS OF XEROSTOMIA
Loss of lubrication. The loss of lubrication leads to oral discomfort, oral ulcerations and trauma, and occasionally oral pain. Patients experience difficulties with normal oral function, especially eating, swallowing, and speaking.
Soft tissue changes. Loss of the protective properties of salivary mucins leads to parched, friable oral mucosa; dryness and chapping of the lips; cracking at the corners of the mouth; and a fissured tongue with atrophy of the papilla (Figure 2). Fingers and dental instruments often stick to the oral mucosa. The parotid glands may be enlarged and tender to palpation. Palpation of the ductal openings of the glands produces little or no secretion. Aphthous ulcerations may also be present. Soft tissue changes may be exacerbated by opportunistic infections caused by Candida albicans, leading to symptomatic geographic tongue, mucosal and pharyngeal fungal infections, and angular cheilitis.2
Oral infections. Loss of the antibacterial, antifungal, and antiviral properties of normal saliva results in numerous oral infections. Parotid saliva contains proteins that demonstrate antifungal effects against C. albicans. As such, fungal infections are common and frequently recurrent among patients with xerostomia.26 Salivary and mucosal antibodies, including salivary mucins, naturally protect oral tissues from viral infections caused by herpes simplex virus, and even HIV.27,28 Loss of antibacterial activity coupled with the drop in oral pH encourages growth of the oral biofilm and creates a favorable environment for Gram-negative bacteria associated with gingival disease. If already present, gingival disease may progress in extent and severity.2
Dental caries. Loss of buffering capacity drops the pH of the oral cavity and dental plaque biofilm. This, along with the loss of natural mechanical cleansing of salivary flow, significantly increases the risk of dental caries. As salivary flow decreases, clearance of oral sugars and other products needed for bacterial metabolic support is prolonged, plus, bacteria are able to adhere to the teeth more readily. With hypofunction, saliva is less able to protect the teeth from the acid attack of cariogenic bacteria, such as Lactobacillus and Streptococcus mutans, and significant caries activity often develops, predominately on exposed root surfaces.15,16 Root caries is the leading cause of tooth loss and poor quality of life among older adults, and half of all individuals older than 75 are affected.29,30
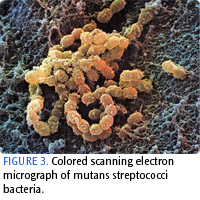
Bacteria that cause dental caries are transmissible, primarily between mother and child.31 Acidogenic bacteria in biofilm are capable of metabolizing fermentable carbohydrates from food sources into organic acids. These acids dissolve the calcium and phosphate minerals in the tooth structure in demineralization. S. mutans (Figure 3) is more involved during the early stages of demineralization, while Lactobacillus (Figure 4) is more evident as the lesion progresses.38 In patients with root caries, levels of S. mutans and Lactobacillus are increased. In patients with no caries, S. mutans is less common and Lactobacillus, which is associated with disease, is notably absent. Many other organisms, however, are associated with root caries, including: Veillonella parvula, Veillonella dispar, Selenomonas noxia, Campylobacter gracilis, Selenomonas putigena, and Fusobacterium nucleatum.32
 |
 |
Salivary protective factors and fluoride stop the demineralization process and help promote remineralization. Saliva buffers the acids and supplies the minerals needed to replace the calcium and phosphate ions that were dissolved. Five critical variables are needed for successful remineralization to occur: 1) high salivary and biofilm pH; 2) high salivary and biofilm calcium levels; 3) high salivary and biofilm phosphate levels; 4) presence of salivary proteins that regulate hydroxyapatite crystals; and 5) presence of the required organic and inorganic matrix.33 In patients with xerostomia, many of these properties are lacking, and both demineralization and caries activity continue to progress. “Snow-capped” cusp tips and white spot lesions are evident.2
Table 3.Factors that increase the risk of caries development.34
• High titers of cariogenic bacteria
• Poor oral hygiene
• Prolonged nursing (bottle or breast)
• Poor family dental health
• Developmental or acquired enamel defects
• Genetic abnormality of teeth
• Many multi-surface restorations
• Chemotherapy or radiation therapy
• Eating disorders
• Drug or alcohol abuse
• Irregular dental care
• Cariogenic diet
• Active orthodontic treatment
• Presence of exposed root surfaces
• Restoration overhangs and open margins
• Physical or mental disability with inability to perform proper oral health care
• Low socioeconomic status
• Xerostomia caused by medication or disease
In addition to bacterial challenge, current research is looking closely at other factors that increase caries susceptibility. Caries is a highly complex disease process that is multi-factorial, with genetic and environmental factors contributing to the known microbial challenge/acid production mechanism. Immune system modulation and local immunological processes in saliva also play key roles in determining the course and severity of the disease.32 Table 3 includes a list of common risk factors.34
A genetic variant in taste sensitivity that increases the desire for sweets, for example, may elevate the risk of caries. Individuals with low taste sensitivity are less susceptible to caries.35,36 Genetic variants also have been discovered for proteins that are critical to proper enamel formation. Those possessing this rare genetic trait have suboptimal enamel structure and increased age-adjusted caries experience.37,38 Variations in immune response genes and a variety of genes that modulate salivary immune function increase caries susceptibility as an individual ages.39,40 It is possible that these genetic differences will be used as markers for caries risk in the future.32
Given the high prevalence of root caries among older adults, the question of age as a risk factor for caries has been explored. Age alone is not a risk factor; however, other agerelated immunologic and behavioral factors may increase caries risk. Immune function declines with age, reducing production of systemic and salivary immunoglobulins, which would otherwise offer protection.41 Medication use leads to hypofunction and altered chemical composition of saliva without altering immune function.42,43 Multiple studies have demonstrated that older adults with medication-induced xerostomia have more caries, more dental restorations, more prostheses, and more tooth loss, due to higher levels of S. mutans and Lactobacillus.44,45 Chronic use of medications that contain sugar as a sweetener also contributes to risk.46 Salivary flow, however, remains stable as an otherwise healthy person ages.47
Assessment tools are available that assess caries risk (Table 4), as well as xerostomia risk, such as the Xerostomia Inventory and the American Dental Hygienists’ Association Hyposalivation Screening Tool.34,48,49 Salivary test kits may also be used chairside to assess risks related to flow rate and salivary pH. These tools can help clinicians determine a patient’s level of caries risk and plan preventive and therapeutic interventions to reduce these risks.
STRATEGIES FOR REDUCING ORAL DISEASE RISK: FLUORIDE
Fluoride is an essential component of any caries control program.50 Fluoride, when available at the crystal surface during an acid challenge, inhibits demineralization. Contained either in biofilm fluid adjacent to enamel crystals or root dentin, fluoride diffuses through channels in the biofilm to increase the fluoride content of the early lesion—preventing further mineral loss. Buffers in saliva raise oral pH in response to acids produced by bacteria from dietary carbohydrates, inhibiting further mineral loss.50 As such, fluoride increases enamel acid resistance. Minerals and fluoride in saliva can then assist with remineralization—fluoride ions adsorb onto the crystal surface and attract and react with calcium and phosphate ions. At higher concentrations, fluoride exhibits antibacterial properties against acidogenic bacteria by crossing the cell membrane and altering enzyme activity essential to growth and survival. Fluoride helps inhibit enolase, an enzyme used by bacteria to metabolize carbohydrates.51
Current evidence shows that topical fluoride products are effective at preventing caries, and that additional benefits are obtained when adding another topical fluoride product with regular use of a fluoridated dentifrice.52 Efficacy of caries reduction is similar between dentifrices, mouthrinses, gels, and varnishes.62 Patients who struggle with self-care may particularly benefit from the addition of a fluoride mouthrinse. Mouthrinses are easy to use, and research shows that patients will readily incorporate them into daily self-care routines.53
Overexposure to both topical and systemic fluoride increases the risk of dental fluorosis. Recent data reveal an increase in prevalence of dental fluorosis over the past two decades, although the degree of fluorosis is still very mild.54 This increase is most likely linked to greater exposure to community fluoridated water and fluoridated dentifrice. Regardless of this risk, water fluoridation is the most cost-effective method for delivering fluoride to a community at large.55
Popular commercially-available topical fluoride products are listed in Table 5. There are also several over-the-counter mouth rinses formulated specifically for patients with xerostomia that contain sodium fluoride, including ACT® Total Care Dry Mouth Rinse (Chattem Inc), Biotene® (GlaxoSmithKline), and Colgate® Dry Mouth Relief (Colgate Oral Pharmaceuticals).
NONFLUORIDE PRODUCTS FOR REMINERALIZATION
Fluorides are the most efficacious caries-reducing products on the market today.52,56 New remineralization products are being used, however, to provide calcium and phosphate ions for precipitation into the carious lesion that, ideally, will not precipitate onto the tooth surface or increase supragingival calculus formation. These products include amorphous calcium phosphate (ACP); casein phosphopeptides (CPP)-ACP (Recaldentâ„¢); calcium sodium phosphosilicate (NovaMin®); and tri-calcium phosphate. More research is necessary to determine the efficacy of these ingredients.
SONIC TOOTHBRUSHING
Research shows that sonic toothbrushing increases salivary flow rate in patients with xerostomia.57 Brushing with a sonic toothbrush (Sonicare®, Philips Oral Healthcare) has also been shown to enhance the diffusion of fluoride through S. mutans biofilms in vitro. Another study showed that subjects with medication-induced xerostomia had significantly lower numbers of incipient and frank root caries after brushing for 1 year with a sonic toothbrush compared to subjects who brushed with a manual toothbrush.58
POLYOLS
Polyols, such as xylitol and sorbitol, are nonfermentable sugar alcohols that decrease dental caries. They inhibit S. mutans in the presence of oral sugars, limiting bacterial growth and reproduction. Polyols also reduce biofilm levels and raise salivary pH, allowing calcium and phosphate to precipitate into demineralized areas. Xylitol has been shown to reduce maternal-infant transmission of S. mutans.59 Caries reduction also improves when sucrose is replaced with a sugar substitute in a cariogenic diet. The recommended dose for caries protective effects is approximately 6 grams per day; caution must be used with higher doses because polyols are not digested and may result in gastrointestinal distress.
ARTIFICIAL SALIVA
Over-the-counter saliva substitutes provide temporary relief from xerostomia. Most contain carboxymethylcellulose, which simulates the viscosity of natural saliva. Many contain glycerin as a humectant and coating agent that provides lubrication, and some include xylitol, sorbitol, and/or fluoride for added caries protection. All are alcohol-free and sugar-free. These products are affordable, but compliance may be problematic due to the limited duration of improvement of symptoms, taste, viscosity, and inconvenience of frequent dosing.
CHLORHEXIDINE
Chlorhexidine has been tested as an antimicrobial agent against S. mutans for short-term use as a component of a comprehensive caries management program. To date, the best evidence of anticaries efficacy has been reported with chlorhexidine varnishes, followed by gels and mouthrinses.60 The evidence about their efficacy, however, is limited and somewhat inconclusive. Additional data are needed to examine long-term effects. Because chlorhexidine is only available in mouthrinse form in the United States at this time, it is not recommended as an agent of choice for caries prevention.80
NUTRITIONAL COUNSELING
Ingestion of sugary foods increases caries risk. Frequency of sugar exposure is more important than the quantity of sugar consumed.61 Minimizing snacking and sugar intake is an important strategy to decrease the nutritional supply for acidogenic bacteria. Avoidance of sticky foods is especially important, because sticky and chewy textures adhere to the teeth longer, especially in pits and fissures. Consumption of acidic beverages also weakens tooth structure and lowers salivary and biofilm pH. Proper oral hygiene is essential to clean the teeth following ingestion of these substances.
Other factors also contribute to dietary risks. Older adults with root caries tend to ingest a greater number of meals each day in addition to having a higher sugar intake. These individuals also have higher counts of Lactobacillus, reduced salivary buffering capacity, and decreased salivary flow.62
SUMMARY
Xerostomia is associated with significant challenges to oral function and may adversely impact quality of life. Complications of xerostomia include difficulties with eating, speaking, swallowing, and wearing oral appliances. Patients with xerostomia are at increased risk of numerous oral diseases—most notably, dental caries. Dental professionals must be aware of the multifactorial nature of this oral condition, conduct a comprehensive risk assessment, and determine appropriate preventive and therapeutic interventions to improve oral health and ability to function.
FIGURE 1 PHOTO CREDIT: BO VEISLAND/PHOTO RESEARCHERS INC
FIGURE 2 PHOTO CREDIT: JAMES STEVENSON/PHOTO RESEARCHERS INC
PHOTO CREDIT: FIGURE 3. DAVID SCHARF/PHOTO RESEARCHERS INC; FIGURE 4. SCIMAT/PHOTO RESEARCHERS INC
REFERENCES
- Ettinger RL. Review: xerostomia: a symptom which acts like a disease. Age Ageing. 1996;25:409–412.
- Fox PC. Differentiation of dry mouth etiology. Adv Dent Res. 1996;10:13–16.
- Dawes C. Physiologic factors affecting salivary flow rate, oral sugar clearance, and the sensation of dry mouth in man. J Dent Res. 1987;66(Suppl):648–653.
- Porter SR, Scully C, Hegarty AM. An update of the etiology and management of xerostomia. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2004;97:28–46.
- Närhi TO, Meurman JH, Ainamo A. Xerostomia and hyposalivation: causes, consequences and treatment in the elderly. Drugs Aging. 1999;15:103–116.
- Bergdahl M, Bergdahl J. Low unstimulated salivary flow and subjective oral dryness: association with medication, anxiety, depression and stress. J Dent Res. 2000;79:1652-1658.
- Guyton AC, Hall JE. Secretory functions of the alimentary tract. In: Textbook of Medical Physiology. 10th ed. Philadelphia: WB Saunders Co; 2000:740–742.
- Humphrey SP, Williamson RT. A review of saliva: normal composition, flow, and function. J Prosthet Dent. 2001;85:162–169.
- Jensen SB, Pedersen AM, Reibel J, Nauntofte B. Xerostomia and hypofunction of the salivary glands in cancer therapy. Support Care Cancer. 2003;11:207–225.
- Garrett JR. The proper role of nerves in salivary secretion: a review. J Dent Res. 1987;66:387–397.
- Enwonwu CO. Ascorbate status and xerostomia. Medical Hypothesis. 1992;39:53–57.
- Tabak LA, Levine MJ, Mandel ID, Ellison SA. Role of salivary mucins in the protection of the oral cavity. J Oral Pathol. 1982;11:1–17.
- Mandel ID. The role of saliva in maintaining oral homeostasis. J Am Dent Assoc. 1989;119:298–304.
- Edgar WM. Saliva: its secretion, composition and functions. Br Dent J. 1992;172:305–312.
- Dowd FJ. Saliva and dental caries. Dent Clin North Am. 1999;43:579–597.
- Langerlöf F, Oliveby A. Caries-protective factors in saliva. Adv Dent Res. 1994;8:222–238.
- USP DI® Drug Information for the Healthcare Professional. 26th ed. Englewood, Colo: Micromedix Inc; 2006.
- Sreebny LM, Schwartz SS. A reference guide to drugs and dry mouth. Gerodontol. 1997;14:33–47.
- Närhi TO, Meurman JH, Ainamo A, et al. Association between salivary flow rate and the use of systemic medication among 76-, 81- and 86-year old inhabitants in Helsinki, Finland. J Dent Res. 1992;71:1875–1880.
- Atkinson JC, Shiroky JB, Macynski A, Fox PC. Effects of furosemide on the oral cavity. Gerodontol. 1989;8:23–26.
- Wall GC, Magarity ML, Jundt JW. Pharmacotherapy of xerostomia in primary Sjögren’s syndrome. Pharmacotherapy. 2002;22:621–629.
- Fox RI, Stern M. Sjögren’s syndrome: mechanisms of pathogenesis involve interaction of immune and neurosecretory systems. Scand J Rheumatol Suppl. 2002;116:3–13.
- Chang CP, Shiau YC, Wang JJ, Ho ST, Kao CH. Decreased salivary gland function in patients with autoimmune thyroiditis. Head Neck. 2003:25:132–137.
- Jensen JL, Uhlig T, Kvien TK, Axell T. Characteristics of rheumatoid arthritis patients with self-reported sicca symptoms: evaluation of medical, salivary and oral parameters. Oral Diseases. 1997;3:254–261.
- Moore PA, Guggenheimer J, Etzel KR, Weyant RJ, Orchard T. Type I diabetes mellitus, xerostomia, and salivary flow rates. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2001;92:281–291.
- Pollock JJ, Denepitiya L, MacKay BJ, Iacono VJ. Fungistatic and fungicidal activity of the human parotid salivary histidine-rich polypeptides on Candida albicans. Infect Immun. 1984;44:702–707.
- Heineman HS, Greenberg MS. Cell protective effect of human saliva specific for herpes simplex virus. Arch Oral Biol. 1980;25:257–261.
- Fox PC, Wolff A, Yeh CK, Atkinson JC, Baum BJ. Saliva inhibits HIV-1 infectivity. J Am Dent Assoc. 1988;116:635–637.
- Saunders RH, Jr., Meyerowitz C. Dental caries in older adults. Dental Clin North Am. 2005;49:293–308.
- Ingle NA, Chaly PE, Zohara CK. Oral health related quality of life in adult population attending the outpatient department of a hospital in Chennai, India. J Int Oral Health. 2010;2:45–55.
- Tanzer JM, Livingston J, Thompson AM. The microbiology of primary dental caries in humans. J Dent Educ. 2001;65:1028–1037.
- Gati D, Vieira AR. Elderly at greater risk for root caries: a look at the multifactorial risks with emphasis on genetics susceptibility. Int J Dent. 2011;2011:647168.
- Mäkinen KK. Sugar alcohols, caries incidence, and remineralization of caries lesions: a literature review. Int J Dent. 2010;2010:1–23.
- American Dental Association Council on Scientific Affairs. Professionally applied topical fluoride. J Am Dent Assoc. 2006;136:1151–1159.
- Lin BP. Caries experience in children with various genetic sensitivity levels to the bitter taste of 6-n-propylthiouracil (PROP): a pilot study. Ped Dent. 2003;25:37–42.
- Wendell S, Wang X, Brown M, et al. Taste genes associated with dental caries. J Dent Res. 2010;89:1198–2002.
- Deeley K, Letra A, Rose EK, et al. Possible association of amelogenin to high caries experience in a guatemalan–mayan population. Caries Res. 2008;42:8–13.
- Patir A, Seymen F, Yildirim M, et al. Enamel formation genes are associated with high caries experience in Turkish children. Caries Res. 2008;42:394–400.
- Ozturk A, Famili P, Vieira AR. The antimicrobial peptide DEFB1 is associated with caries. J Dent Res. 2010;89:631–636.
- Srivastava A, Wang J, Zhou H, Melvin JE, Wong DT. Age and gender related differences in human parotid gland gene expression. Arch Oral Biol. 2008;53:1058–1070.
- Taub DD, Murphy WJ, Longo DL. Rejuvenation of the aging thymus: growth hormone-mediated and ghrelin-mediated signaling pathways. Curr Opin Pharmacol. 2010;10:408–424.
- Leslie MD, Glaser MG. Impaired salivary gland function after radiotherapy compounded by commonly prescribed medications. Clin Oncol. 1993;5:290–292.
- Moore PA, Guggenheimer J. Medicationinduced hyposalivation: etiology, diagnosis and treatment. Compend Contin Educ Dent. 2008;29:50–55.
- Peker I, Alkurt MT, Usalan G. Clinical evaluation of medications on oral and dental health. Int Dent J. 2008;58:218–222.
- Rindal DB, Rush WA, Peters D, Maupomé G. Antidepressant xerogenic medications and restoration rates. Community Dent Oral Epidemiol. 2005;33:74–80.
- Ciancio SG. Medications’ impact on oral health. J Am Dent Assoc. 2004;135:1440–1448.
- Fischer D, Ship JA. Effect of age on variability of parotid salivary gland flow rates over time. Age Ageing. 1999;28:557–561.
- American Dental Hygienists’ Association. ADHA Hyposalivation Tool. Available at: www.adha.org/downloads/Hyposalivation.pdf. Accessed October 10, 2011.
- Thomson WM, Chalmers JM, Spencer AJ, Williams SM. The Xerostomia Inventory: a multiitem approach to measuring dry mouth. Community Dent Health. 1999;16:12–17.
- Featherstone JD. Prevention and reversal of dental caries: role of low level fluoride. Community Dent Oral Epidemiol. 1999;27:31–40.
- Featherstone JD. The science and practice of caries prevention. J Am Dent Assoc. 2000;131:887–899.
- Marinho VC. Cochrane reviews of randomized trials of fluoride therapies in preventing dental caries. Eur Arch Paediatr Dent. 2009;10:183–191.
- Darby M. Antimicrobial mouthrinses in contemporary dental hygiene practice: the take home message. J Dent Hyg. 2007;81(Suppl):1–3.
- Beltrán-Aguilar ED, Barker L, Dye BA. Prevalence and severity of dental fluorosis in the United States, 1999-2004. NCHS Data Brief. 2010;53:1–8.
- Truman BI, Gooch BF, Sulemana I, et al. Reviews of evidence on interventions to prevent dental caries, oral and pharyngeal cancers, and sports-related craniofacial injuries. Am J Prev Med. 2002;23(Suppl):21–54.
- Rethman MP, Beltran-Aguilar ED, Billings RJ, et al. Nonfluoride caries-preventive agents: a systematic review and evidence-based recommendations. J Am Dent Assoc. 2011;142:1065–1071.
- Papas A, Singh M, Harrington D, RodrÃguez S, Ortblad K, de Jager M, Nunn M. Stimulation of salivary flow with a powered toothbrush in a xerostomic population. Spec Care Dentist. 2006;26:241–246.
- Papas AS, Singh M, Harrington D, Ortblad K, de Jager M, Nunn M. Reduction in caries rate among patients with xerostomia using a power toothbrush. Spec Care Dentist. 2007;27:46–51.
- Maguire A, Rugg-Gunn AJ. Xylitol and caries prevention—is it a magic bullet? Br Dent J. 2003;194:429–436.
- Autio-Gold J. The role of chlorhexidine in caries prevention. Oper Dent. 2008;33:710–716.
- Burt BA, Eklund SA, Morgan KJ, et al. The effects of sugars intake and frequency of ingestion on dental caries increment in a three-year longitudinal study. J Dent Res. 1988;67:1422–1429.
- Faine MP, Allender D, Baab D, Persson R, Lamont RJ. Dietary and salivary factors associated with root caries. Spec Care Dentist. 1992;12:177–182.
From Dimensions of Dental Hygiene. November 2011; 9(11): Special CE Insert.




