
Visual Acuity Is Key to Successful Patient Outcomes
Using magnification to enhance their visual acuity allows dental hygienists to more effectively identify periodontal problems and conduct accurate preventive and nonsurgical periodontal procedures.
The profession of dental hygiene is visually demanding. During clinical patient care, a dental hygienist relies on optimal visual acuity to conduct thorough periodontal assessments, interpret radiographs, and deliver appropriate preventive and therapeutic care. According to the American Optometric Association, an individual with 20/20 vision can clearly see and distinguish objects at 20 feet.1 In dental hygiene clinical care, however, normal 20/20 vision does not necessarily provide a clear or sharp visual of the oral cavity.
The distance from the clinician’s eye to the oral cavity is approximately 15 to 22 inches.2 This distance, in addition to the gradual decline in visual acuity due to aging, impacts the clarity and sharpness of the clinician’s vision.2,3 The average age of a clinically practicing dental hygienist is 42. Considering this, clinicians need to be aware of technologies available to reduce visual deficiencies and decrease eyestrain.2,3
Loupe Systems
Loupes are one of the most affordable ways to enhance a dental hygienist’s visual acuity. Their greatest advantage is the enhancement of indirect vision, which supports more precise instrumentation, leading to positive patient outcomes post-scaling and root planing as well as reduced risk of cementum removal and root gouging.4-7 Loupes also reduce visual deficiencies — especially for clinicians older than age 40.4-7
Galilean and Keplarian prismatic loupes are the most common systems used in dental hygiene. The more popular and traditionally used Galilean loupes consist of one objective convex lens and one concave lens. Galilean loupes have a magnification range limited to 3.5x or less. The lower magnification allows first time magnification users to easily adapt to loupe vision. Galilean loupes are also lightweight and simple in design, making them a popular choice among clinicians who prefer direct vision.8
Keplarian loupes consist of two or more convex lenses with a prism in between. The prism allows the Keplarian loupe to offer an edge-to-edge clarity and a greater magnification depth of 3.5x to 8.0x. To accommodate this, Keplarian loupes have long barrels and are heavier in weight.
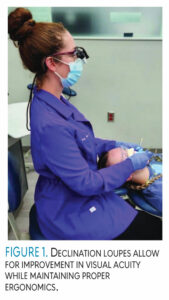
More advanced loupes have been designed to provide the clarity and intense magnification of the Keplarian loupe. Deflection loupes or prism loupes (Figure 1) are designed to improve both visual acuity and musculoskeletal heath, while still providing the necessary optical demands for periodontal procedures. The deflection loupe mimics a single reflex camera with its internal optical design and a prism that reflects light through two faces, so it can flip the image to appear upright.
Deflection loupes enable dental hygienists to reduce neck tilt to 20° or less, ultimately enabling the spine to stay appropriately aligned and straight. Unlike traditional Keplerian loupes, these loupes are lightweight, come in varying magnifications of 3.0x to 10.0x, and offer a wide field of vision.
Headlights
The use of LED coaxial illumination coupled with loupes further enhances a dental hygienist’s visual acuity. The illumination allows the clinician to efficiently and effectively work in the small, constrained, dark oral cavity. This illumination improves visual acuity to detect periodontal issues and carious lesions all while continuing to maintain good posture.9 Many of these headlights utilize color-neutral LED lights, which emit the lowest blue light for eye protection.
Concerns of cross contamination arose during the SARS-CoV-2 pandemic because the clinician must manually turn the headlight on and off. Manufacturers responded with touch-free headlights activated by the head movement or hand wave of the operator.
Many touchless systems have eliminated the need for clinicians to wear the traditional heavy battery pack and cord. Fluorescence-activating headlights with specially filtered loupes allow dental hygienists to identify poor restorative and sealant margins, enamel demineralization, bacterial contamination, supra-and subgingival calculus, and accumulation of active periodontal bacteria around natural teeth and implants.10
Dental Operating Microscope
Introduced in 1981 primarily for endodontic procedures, the dental operating microscope (DOM) allows the clinician to use multiple magnification levels while maintaining the appropriate amount of shadow-free illumination for higher magnification of up to 25x and limits the need to adjust posture.11,12 In comparison to loupes and headlights, the illumination of the DOM is far more superior because of its coaxial path of light being parallel to the path of vision.11
The DOM offers enhanced visual acuity, improvement in quality of treatment, optimal clinician comfort, and decrease of iatrogenic damage to the root surface.11 Another benefit is its ability to take photos and videos during procedures with the use of a beam splitter.11 This capability improves patient-dental hygienist communication in regards to oral hygiene instruction and results in higher acceptance of treatment plans for needed periodontal procedures.
The DOM is becoming more popular among periodontal practices and, thus, dental hygienists. A recent study showed the use of the DOM during nonsurgical periodontal therapy resulted in an overall greater pocket reduction at 4 weeks, improved attachment of the periodontal ligament, and a decrease in pro-inflammatory cytokine production at the root surfaces than nonsurgical periodontal therapy done without DOM magnification.13 Unfortunately, the DOM’s high cost, large size, and need for training may impede its integration into practice.11
Periodontal Endoscope
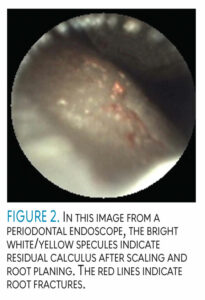 The periodontal endoscope is unique in that it enhances the direct visualization of the following: clinical root, subgingival calculus, and biofilm deposits in both shallow and deep periodontal pockets; periodontal-supporting structures; and biofilm and excess cement on implants (Figure 2).14
The periodontal endoscope is unique in that it enhances the direct visualization of the following: clinical root, subgingival calculus, and biofilm deposits in both shallow and deep periodontal pockets; periodontal-supporting structures; and biofilm and excess cement on implants (Figure 2).14
Early models of the periodontal endoscope used a 0.99 mm fiber optic bundle that enabled root magnification of 24x to 48x.14 Advancements in this technology have improved allowing for magnification of up to 100X and 160K resolution.15
The fiber optic bundle is covered and inserted into an explorer-like instrument that helps guide the periodontal endoscope into the gingival sulcus.14 This allows for the image of subgingival structures to be viewed on a display screen by the clinician as the explorer moves around the subgingival anatomy of the tooth.14
Studies have shown that the visualization and magnification properties of a periodontal endoscope vastly improve dental hygienists’ calculus detection and removal skills on wide tooth and root surfaces and as well as enable the easy detection of root surface caries.16,17 The periodontal endoscope enables meticulous subgingival calculus removal that otherwise would need to be removed by flap surgery. The use of this visualization technology not only enhances the dental hygienist’s visual acuity during periodontal therapy, but also may improve patients’ periodontal health.
Conclusion
Dental hygienists rely heavily on their vision to provide optimal oral healthcare. Using magnification to enrich their visual acuity enables dental hygienists to better manage periodontal issues and perform precise preventive and nonsurgical periodontal procedures to improve oral health outcomes.
References
- American Optometric Association: Visual Acuity: What is 20/20 Vision? Available at: aoa.org/healthy-eyes/vision-and-vision-correction/visual-acuity?sso=y. Accessed May 16, 2024.
- Wilkins E. Clinical Practice of the Dental Hygienist. 14th ed. Burlington, Massachusetts: Jones and Bartlett Learning; 2023: 123.
- Mayo Clinic: Presbyopia. Available at: mayoclinic.org/diseasesconditions/presbyopia/symptoms-causes/syc20363328#:~:text=Presbyopia%20is%20the%20gradual%20loss,worsen%20until%20around%20age%2065. Accessed May 16, 2024.
- Hoerler SB, Branson BG, High AM, Mitchell TV. Effects of dental magnification lenses on indirect vision: a pilot study. J Dent Hyg. 2012;86:323-330.
- Arnett MC, Gwozdek AE, Ahmed S, et al. Assessing the use of loupes and lights in dental hygiene educational programs. J Dent Hyg. 2017;9:15-20.
- Corbella S, Taschieri S, Cavalli N, et al. Comparitive evaluation of the use of magnification loupes in supragingival scaling procedures. J Invest Clin Dent. 2018;9:e12315.
- Perrin P, Ramseyer ST, Eichenberger M, Lussi A. Visual acuity of dentists in their respective clinical conditions. Clin Oral Investig. 2014;18:2055-2058.
- Aldosari MA. Dental magnification loupes: and update of the evidence. J Contemp Dent Pract. 2021; 22:310-315.
- Ari T, Ari N. The performance of ICDAS-II using low-powered magnification with light-emitting diode headlight and alternating current impedance spectroscopy device for detection of occlusal caries on primary molars. ISRN Dent. 2013;2013:276070.
- Teier L, Figueiredo JAP, Blatz MB. Fluorescence-enhanced theragnosis: a novel approach to visualize, detect, and remove caries. Compend Contin Educ Dent. 2021;42:460-465.
- Bud M, Jitaru S, Lucaciu O, Korkut B, Dumitrascu-Timis L, Ionescu C, Cimpean S, Delean A. The advantages of the dental operative microscope in restorative dentistry. Med Pharm Rep. 2021;94:22-27.
- Gutmann JL. Historical perspectives on the use of microscopes in dentistry. J Hist Dent. 2017;65:20-27.
- Liao H, Zhang H, Xiang J, et al. The effect of the surgical microscope on the outcome of root scaling. Am J Transl Res. 2020:12: 7199-7210.
- Wright HN, Mayer ET, Lallier TE, Maney P. Utilization of a periodontal endoscope in nonsurgical periodontal therapy: A randomized, split-mouth clinical trial. J Periodontol. 2023;94:933-943.
- Kuang Y, Hu B, Chen J, et al. Effects of periodontal endoscopy on the treatment of periodontitis: A systematic review and meta-analysis. J Am Dent Assoc. 2017;148:750–759.
- Osborn JB, Lenton PA, Lunos SA, et al. Endoscopic vs. tactile evaluation of subgingival calculus. J Dent Hyg. 2014;88:229–236.
- Naicker M, Ngo LH, Rosenberg AJ, et al. The effectiveness of using the perioscope as an adjunct to non-surgical periodontal therapy: Clinical and radiographic results. J Periodontol. 2022;93:20–30.
From Dimensions of Dental Hygiene. June/July 2024; 22(4):16-19

