Update on Tuberculosis
Oral health professionals need to remain up to date on infection control protocols related to TB transmission in order to best protect themselves and their patients.
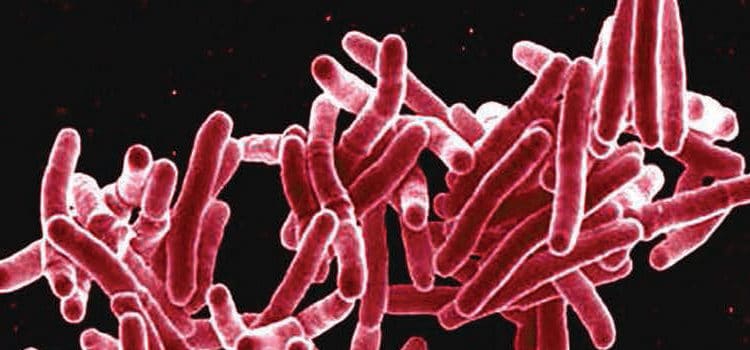
Tuberculosis (TB) is an infectious disease caused by Mycobacterium tuberculosis, which are a pathogenic bacterial species of small, aerobic particles (Figure 1).1 TB is spread through direct person-to-person contact via airborne transmission. Most commonly presenting as a pulmonary infection, the tubercle bacilli invade the lungs, multiply, and cause inflammation. Less commonly, extrapulmonary TB infection can spread through the circulatory or lymphatic systems to other parts of the body, such as lymph nodes, bones, urinary tract or genitals, brain, skin, or as generalized infection.2 Individuals with active TB disease generally present with an acute cough persisting 3 weeks or longer, pain in the chest, hemoptysis (coughing up blood or sputum), weakness or fatigue, weight loss, no appetite, chills, fever, and night sweats.1,2
In 2015, more than 10 million people worldwide developed TB and another 1.8 million died of the disease.3 According to the United States Centers for Disease Control and Prevention (CDC), over the past two decades, the US has made progress in eliminating TB. Recent data, however, show that the prevalence of TB in the US leveled off at three cases per 100,000 individuals during 2013 to 2015.4 According to the World Health Organization, the total number of reported TB cases in the US between 2013 and 2015 was 9,563. Of those cases, 66.2% occurred in foreign-born individuals.3
The incidence of untreated latent TB disease infection (LTBI), in which individuals have M. tuberculosis but are not considered infectious and do not exhibit symptoms, is on the rise.1,4 The bacterium M. tuberculosis can lie dormant in the body for several years.1 Individuals with LTBI may also present with normal chest X-rays and a negative sputum smear.1,2 In response to the increase in LTBI cases, one of the US Department of Health and Human Services’ Healthy People 2020 global health goals is to reduce the rate of TB infection among foreign-born individuals living in the US from 20.4 cases per 100,000 to 14 cases per 100,000.5
ETIOLOGY AND PATHOPHYSIOLOGY
Pulmonary TB is spread through direct person-to-person contact via airborne transmission, not through direct contact such as handshaking.1 Transmission only occurs when an active M. tuberculosis infection is present.1,6 Factors influencing the likelihood of transmission are an exposed individual’s susceptibility (immune system status); infectiousness of an individual with TB disease; environmental factors affecting the concentration of M. tuberculosis pathogens; and, proximity, frequency, and duration of exposure.4 Once infected, the incubation period may occur over 3 months to 6 months.1,2,6 Individuals with active TB disease must receive treatment for several weeks before coming in close contact with others.1–3,6
The bacterium can live undetected in individuals with LTBI for years until a TB skin test (TST)?or blood test, called an interferon gamma release assay (IGRA), detects it or active TB develops.1,2 About 5% to 10% of those diagnosed with LTBI develop active TB disease within the first 2 years of infection.1 This activation can occur in individuals who never received treatment for LTBI and later develop comorbidities or an immunosuppressive disease, such as HIV. Surgeries and medical procedures can also activate LTBI.7,8
DIAGNOSIS
When recording health histories, oral health professionals need to be able to recognize the signs and symptoms of TB, particularly its onset and duration, risk factors, past exposures, associated test results, and whether recommended LTBI treatment was completed. The two tests used to diagnose TB are the TST and the IGRA. Both tests can indicate active or latent TB infection, including any past exposure. While more costly, the IGRA is not affected by prior Bacillus Calmette–Guérin (BCG) vaccine, which is commonly administered in countries where TB is a significant health problem.1,2,7,9 The IGRA looks for the body’s response to specific TB antigens not present in other forms of mycobacteria and BCG.1,6,7,10 The IGRA is generally not recommended for people with recent exposure to M. tuberculosis, children younger than 17, and immunocompromised individuals.1,2
A positive TST or IGRA result does not indicate whether the person has LTBI or if it has progressed to TB disease.8,11,12 Additional diagnostic tests, such as chest radiographs, sputum samples, and a clinical examination, are imperative to definitively diagnose TB disease.1,13 If an individual has a positive TST or IGRA but does not have active TB disease, he or she is diagnosed with LTBI.1
TREATMENT CONSIDERATIONS
Detecting TB disease early and supporting patient adherence to the prescribed anti-TB drug regimen is crucial to preventing drug resistance and re-treatment.9 The current treatment for TB disease is a first-line, anti-TB agent cocktail of oral drugs that includes isoniazid, rifampicin, ethambutol, pyrazinamide, rifabutine, and rifapentine.5,14 The drugs regimen is taken for 6 months or longer. Rapid, second-line drugs are not as practical, as they require injection and are expensive.1,5,15
Globally, TB has become resistant to many of the most effective first-line therapeutic drugs, such as isoniazid and rifampicin.8 This multidrug-resistant TB (MDR-TB) strain emerged due to the lack of adherence to TB antibiotic therapies either because of noncompliance or inadequate drug supply.8,11 Extensively drug-resistant TB has now emerged, although extremely rare in the US, that has a cure rate of only 28%.1,2,6,9,13 This strain is problematic because it is resistant to both first- and second-line therapeutic drugs.1-3 Early detection and treatment are the best course of action in preventing all forms of drug-resistant TB.1,3,9,10
A new treatment for drug-resistant TB has been used successfully in 18 countries.15,16 The regimen consists of a shortened treatment with a 4-month to 6-month intensive phase (with four second-line drugs) and a continuation phase (with two second-line drugs). The entire treatment duration lasts only 9 months to 12 months. The cost is substantially less per patient compared to other drug regimens.9,12,15,16
Directly observed therapy is used to mitigate noncompliance, particularly with drug-resistant strains of TB.1,5 Essentially, a trained observer—usually a health care worker—meets with a patient daily or several times a week to observe whether the patient is complying with treatment and monitors any adverse side effects or drug interactions for the duration of treatment.2 New drugs are being developed for drug-resistant TB strains that show promise.6 However, their ability to reach the most vulnerable populations worldwide remains to be seen.6
INFECTION CONTROL PROGRAM
Every dental setting should have written infection prevention and control procedures that are regularly reviewed. The CDC released a revision of the 1994 Guidelines for Preventing the Transmission of Mycobacterium Tuberculosis in Health-Care Settings in 2005. The revision added dental health care personnel and dental staff members to the health care workers who should be included in a TB surveillance or screening program.1
The CDC recommends assigning an infection prevention and control administrator within the work environment.1 The designated individual should ensure that TB safety standard precautions and procedures are followed, as well as provide written policies and training for all employees.5 Signs depicting cough etiquette should be displayed, in addition to the provision of masks and facial tissues, to prevent the potential spread of disease throughout a clinic. When hiring dental personnel, their LTBI screening and treatment histories must be monitored, as well as whether they have been exposed to active TB disease within the past year.1 Additionally, the administrator’s role entails conducting annual risk assessments and providing personnel training on infection control.
Every dental setting should conduct two types of annual risk assessments to identify the overall TB risk level. A dental setting’s risk classification identifies the number of active TB cases that are encountered within the office annually, including any dental personnel who may have been exposed to M. tuberculosis.1 A general dentist’s office that encounters a few active TB cases per year would be an example of a low-risk setting; a public health setting that serves populations affected by HIV/AIDS or homelessness might be a moderate- or high-risk setting.
A community awareness risk assessment can be accomplished by contacting the local health department to discern the likelihood of encountering TB in a particular area.1 Dental personnel who have volunteered in dental settings with high-risk patients or recently traveled to a county with a high TB-burden should refer to the TB risk classification published by the CDC to determine the required need and frequency of testing for TB disease.1 Both assessments assist the dental setting in the development of office infection control practices.1
Patients or exposed oral health professionals are considered noninfectious when they produce three negative acid fast bacilli (AFB) smears collected in 8-hour to 24-hour intervals, complied with TB treatment for 2 weeks or longer, and their symptoms have improved clinically (coughing markedly improved, no fever).1 When considering an employee’s return to work or the safe scheduling of patients, the best course of action is to receive a medical clearance from the individual’s physician.1
Patients with active TB disease should be dismissed until the aforementioned guidelines have been met and a medical clearance is granted by a physician. Moreover, individuals with suspected symptoms should be dismissed and referred to the health department for TB testing. Urgent dental care with a suspected or active TB case should be provided in a health-care setting that has the capacity to offer an Occupational Safety and Health Administration (OSHA) standard respiratory airborne infection isolation room and fitted N-95 respirators, as regular surgical masks do not filter small M. tuberculosis aerobe particulates.1,15,16
Oral health professionals need to comprehensively review all medical, dental, and social histories of patients with TB, including any chest radiographs and immunization records.1,10,17 The 2007 American Dental Association health history form provides a useful template to screen patients for both active TB and LTBI.18 The form asks whether patients have active TB, persistent cough for more than 3 weeks, cough that produces blood, and/or exposure to anyone with TB. If any of these questions elicits a “yes” response, the patient should be immediately referred.18
Patients with a history of TB should be asked about the history of their disease, including exposure and treatment completion.19,20 Health histories should include questions about recent travel abroad, especially visits to developing countries.17 Prior arrangements should be made if a patient needs a translator. All OSHA-recommended infection control practices should be strictly followed, including the use of personal protective equipment.2
Until a patient diagnosed with TB has finished treatment or is no longer coughing, the use of ultrasonic scalers or air polishers is contraindicated.1,2 Patients with active TB should not be seen for any dental procedures in a setting without OSHA-regulated environmental controls, until the health care professional treating them for TB infection has confirmed they are no longer infectious.
As more dental hygienists work in expanded practice settings, they must develop working relationships with their local health departments to determine the community TB risks within the designated population they are serving. An interdisciplinary approach is needed to care for patients who have postponed dental care due to active TB infection. Clinicians must also consistently update patients’ health records, review relative correspondence, and document any changes.
CONCLUSION
Dental professionals must establish and adhere to proper in-office infection control standards and policies in order to prevent M. tuberculosis transmission to clinicians and patients. Dental hygienists have many important roles to fulfill concerning TB disease, especially pertaining to prevention and screening. Because TB diagnostic methods and pharmaceutical developments are evolving, dental staff must stay abreast of these changes and utilize the most current procedures for best practice.
REFERENCES
- Centers for Disease Control and Prevention. Tuberculosis (TB). Available at: cdc.gov/tb/education/corecurr/pdf/corecurr_all.pdf. Accessed November 22, 2016.
- Cleveland JL, Robison VA, Panililio AL. Tuberculosis epidemiology, diagnosis and infection control recommendations for dental settings. J Amer Dent Assoc. 2009;140:1092-1099.
- World Health Organization. WHO Global Tuberculosis Report 2016. Available at: apps.who.int/iris/bitstream/10665/250441/1/9789241565394-eng.pdf?ua=1. Accessed November 22, 2016.
- Medecins Sans Frontieres. TB Briefing Paper: An Overview of MSF’s Programmatic Use and Clinical Research With New TB Treatment Regimens October 2016. Available at: msfaccess.org/sites/default/files/TB_ISSUEBRIEF_NEW-DRUGS_2016_EN.pdf. Accessed November 22, 2016.
- Centers for Disease Control and Prevention. Leveling of Tuberculosis incidence—United States, 2013-2015. Available at: cdc.gov/mmwr/volumes/65/wr/mm6511a2.htm. Accessed November 22, 2016.
- United States Department of Health and Human Services. Healthy People 2020 Topics and Objectives: Immunization and Infectious Diseases. Available at: healthypeople.gov/2020/topics-objectives/topic/immunization-and-infectious-diseases/objectives. Accessed November 22, 2016.
- Merte JL, Kroll CM, Collins AS, Melnick AL. An epidemiologic investigation of occupational transmission of Mycobacterium tuberculosis infection to dental health care personnel. J Amer Dent Assoc. 2014;145:464-471.
- Jacobsen KH. Introduction to Global Health. 2nd ed. Burlington, Massachusetts; Jones & Bartlett: 2014.
- Van Cutsem G, Isaakidis P, Farley J, Nardell E, Volchenkov G, Cox H. Infection control for drug-resistant tuberculosis: Early diagnosis and treatment is key. Clin Infect Dis. 2016;62:S238-S243.
- Centers for Disease Control and Prevention. Latent tuberculosis infection: A guide for primary health care providers. Available at: cdc.gov/tb/publications/ltbi/treatment.htm. Accessed November 22, 2016
- Garcia MJ, Lopez MR. Editorial commentary: Do have strategies to improve the preventive treatment of latent tuberculosis infection? Clin Infect Dis. 2016;62:1401-1402.
- Centers for Disease Control and Prevention. Questions and answers about TB. Available at: cdc.gov/tb/publications/faqs/qa_latenttbinf.htm. Accessed November 22, 2016.
- World Health Organization. The End TB Strategy. Available at: who.int/tb/post2015_TBstrategy.pdf. Accessed November 22, 2016.
- National Institute of Allergy and Infectious Diseases. Tuberculosis treatment. Available at: niaid.nih.gov/diseases-conditions/tb-treatment. Accessed November 22, 2016.
- World Health Organization. WHO recommendations on the use of the SL-LPA. Available at: who.int/tb/Factsheet_SLLPAfinal.pdf. Accessed November 22, 2016.
- World Health Organization. The Shorter MDR-TB Regimen. Available at: who.int/tb/Short_MDR_regimen_factsheet.pdf. Accessed November 22, 2016.
- The Joint Commission. OSHA and Worker Safety: Helping Health Care Workers to Breathe Easy. Available at: jcrinc.com/assets/1/7/Environment_of_Care_March_2016_JCR.pdf. Accessed November 22, 2016.
- American Dental Association. 2007 ADA Health History Form. Available at: ebusiness.ada.org/productcatalog/product.aspx?ID=117. Accessed November 22, 2016.
- Occupational Safety and Health Administration. Safety and Health Topics: Tuberculosis. Available at: osha.gov/SLTC/tuberculosis/standards.html. Accessed November 22, 2016.
- Von Delft A, Dramowski A, Sifumba Z, Mosidi T, Ting TX, Von Delft D, Zumla A. Exposed, but not protected: More is needed to prevent drug-resistant tuberculosis in healthcare workers and students. Clin Infect Dis. 2016;62:S275-S279.
From Dimensions of Dental Hygiene. December 2016;14(12):18–20.

