 BET_NOIRE/ISTOCK/GETTY IMAGES PLUS
BET_NOIRE/ISTOCK/GETTY IMAGES PLUS
Ultrasonic Instrumentation Technique for First Molar Teeth
Successful instrumentation of first molar teeth is integral toachieving and maintaining periodontal health.
First molar teeth present a challenge for clinicians’ professional care and patients’ self-care. Not only do first molars demonstrate complex anatomy, they are at increased risk for increased probing depths, clinical attachment loss, and bone loss when compared with single-rooted and more anterior teeth.
The root anatomy of first molar teeth was reviewed in the article “Hand Instrumentation of First Molar Teeth,” in the May issue of Dimensions of Dental Hygiene.1 Also, ultrasonic tip selection was discussed in the article ”Ultrasonic Insert/Tip Selection for First Molar Teeth’” in the July issue of Dimensions.2 Knowledge about the root concavities and furcation anatomy of these molars is crucial for providing nonsurgical periodontal therapy (NSPT) and periodontal maintenance (PM) for patients with periodontitis.
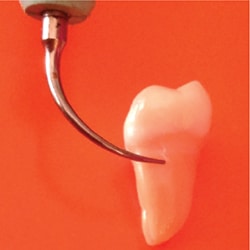
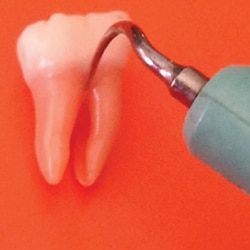
Three key issues for correct ultrasonic instrumentation for periodontal debridement of first molar teeth are: how much of the tip the operator applies, the angle at which the tip is adapted, and the lateral force. First, up to 4 mm of the working end of a magnetostrictive insert can be adapted (Figure 1). With a piezoelectric tip, 2 mm to 3.5 mm should be adapted. Unfortunately, adapting a greater surface area could create burnished calculus, incomplete deposit removal, and inefficient instrumentation. Conversely, the use of less than the active area may cause root surface striations and/or sensitivity.
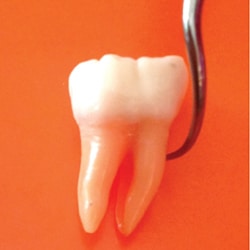
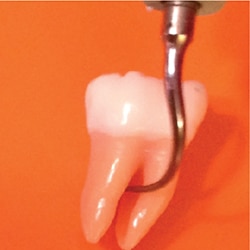
The second key factor is the use of the proper angle of the active tip to the root, which should be maintained at 0° to 15°. Because of the significant crown and root curvatures of first molars, 0° is nearly impossible; a 10° to 15° angle is more feasible (Figure 2). This 15° tip-to-root angle is ideal because angulation greater than 15° results in loss of root substance.3,4 The most damage to root surfaces (eg, defect depth) was found with increased tip angulation.3,4
The third factor is the force used with the tip. The lightest force possible, without causing burnishing, should be used to remove the deposit. Use of heavier lateral force can cause root structure removal.3,4 Clinicians should let the instrument’s vibratory action remove the deposit. If necessary, the low power setting can be adjusted to medium or medium high. There is a relationship between tip angulation, lateral force, and power setting, and each can be adjusted to meet the clinical needs of the patient.3,4
CONCAVITIES
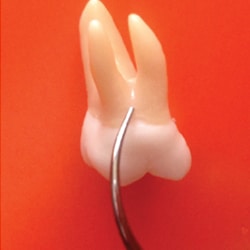
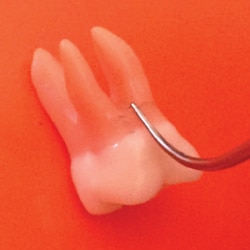
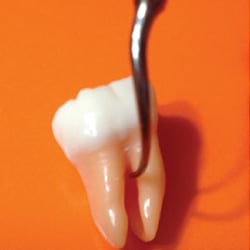
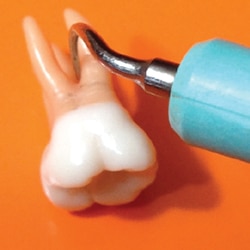
Adjacent to the maxillary first molar buccal furcation entrance and the mandibular first molar buccal and lingual furcation entrances is a significant concavity, which needs to be maneuvered to remove plaque biofilm and calculus. This concavity is about 0.5 mm to 1 mm deep and necessitates rolling the ultrasonic tip into the concavity to reach its depths (Figure 3). There are two ways to approach these concavities with magnetostrictive units. One is to adapt the back of the working end within the concavity (Figure 4). The other is to adapt the side of the working end to the concavity (Figure 3). With piezoelectric units, the sides of the tip are used.
The maxillary first molar tooth has concavities on the mesial and distal surfaces extending from the cementoenamel junction (CEJ) to the entrance to the mesial or distal furcation, depending on the level of attachment. The mandibular first molar usually has a significant longitudinal concavity on the mesial surface extending throughout the middle one third of the root that does not reach the tooth’s CEJ or apex. These concavities might also contain developmental grooves. The distal of the mandibular first molar usually does not have a concavity; therefore, this entire surface is convex.
Knowing where the root concavities lie is essential to effective periodontal instrumentation. Often deposits fill these concavities. If this is the case, the root might feel smooth and mistakenly be assumed to be clinically free of plaque biofilm and calculus.
FURCATON INVOLVEMENT
Furcation involvement indicates molars are at increased risk of tooth loss compared with other teeth.5,6 In fact, a retrospective study revealed that severe periodontitis in those aged 30 to 45 started between the ages of 22 and 28.7 Thus, furcation involvement occurs in both young and older adults. Furcation involvement on the first molars necessitates concentration on a very focused area. The anatomical structures and the position of the gingival margin will be considered.
Typically, loss of bone in furcation areas has been classified by the extent of horizontal involvement: Class I, II, or III.8 The clinician will have a clear picture of the horizontal depth needed for effective instrumentation if a furcation probe is used to measure the loss of tissue.
The residual periodontal support on each root of the furcated molars can also be assessed via a vertical classification.9 Tarnow and Fletcher10 established the initial system with subclassifications based on probable vertical depth from the roof of the furcation in millimeters (A = 1 mm to 3 mm, B = 4 mm to 6 mm, C= 7 mm or greater). Tonetti et al9 modified this system based on the extent of attachment/bone loss in relation to the root length (A = coronal third, B= middle third, C= apical third).
Assessing loss of attachment in the furcation relates to the anatomy. In fact, both horizontal and vertical furcation bone loss are associated with increased risk of tooth loss during PM.5 Furcation involvement is more likely in molars where the entrance to the furcation area is closer to the gingival margin and, thus, the microbial assault.5 The maxillary molar furcation entrances are located only 4 mm on the buccal, 3 mm on the mesial, and 5 mm on the distal from the CEJ. The mandibular molar furcation entrances are only 3 mm on the buccal and 4 mm on the lingual from the CEJ.
One of the greatest advantages of ultrasonic instrumentation in exposed furcations is the rounded and thin surface area of ultrasonic instruments/tips (UITs) that emits energy from various sides of the tip. This energy emitted from multiple sides adapts to more surface area at one time than a curet, which could be beneficial in the roof of a furcation.
The buccal and lingual openings on both first molar furcations are narrow (ie, 1 mm or less) indicating the need for a very thin tip. The roof of a furcation is best approached by applying the side or back of the working end (Figure 5). This same principle applies to instrumentation inside the furcation. An exception would be a very exposed furcation where there is room to adapt the ultrasonic in varying orientations.
The inside of the exposed furcation can be treated in two steps. First, the mesial surface of the distal root is debrided (Figure 6) and second, the distal surface of the mesial root is treated (Figure 7). With a deep horizontal and/or vertical exposure of the furcation, it is important to have memorized the anatomy of the inside of the roots.1 Each root on maxillary and mandibular first molar teeth manifests a concavity on the interior of the mesial or distal root, and the interior of the lingual/palatal root in the case of maxillary teeth. Therefore, rolling and pivoting are indicated to reach inside the concavities in the interior of an exposed furcation area (Figure 8). In this instance, a surgical diamond-coated UIT might be useful depending on philosophy, experience, and the ability to view the area with an endoscope. Also, UITs designed for furcations with a 0.8 mm ball end are available for entering furcations, as well as for developmental grooves and concavities.
Throughout NSPT and PM, ultrasonic instrumentation should be supplemented with hand instrumentation to aid in effectiveness. Both root anatomy and proper technique must be considered for prevention and maintenance of periodontitis. Caring for first molar teeth is important to achieving and maintaining periodontal health.
![]() REFERENCES
REFERENCES
- Hodges KO. Hand instrumentation of first molar teeth. Dimensions of Dental Hygiene. 2017;15(12)14–16.
- Hodges KO. Ultrasonic insert/tip selection for first molar teeth. Dimensions of Dental Hygiene. 2018;15(7):48–49.
- Flemmig TF, Petersilka GJ, Mehl A, Hickel R, Klaiber B. The effect of working parameters on root substance removal using a piezoelectric ultrasonic scaler in vitro. J Clin Periodontol. 1998;25:158–163.
- Flemmig TF, Petersilka GJ, Mehl A, Hickel R, Klaiber B. Working parameters of a magnetostrictive ultrasonic scaler influencing root substance removal in vitro. J Periodontol. 1998;69:547–553.
- Nibali L, Sun C, Akcali A, et al. The effect of horizontal and vertical furcation involvement on molar survival: A retrospective study. J Clin Periodontol. 2018:45:373–381.
- Johansson KJ, Johansson CS, Ravald N. The prevalence and alterations of furcation involvements 13 to 16 years after periodontal treatment. Swedish Dental Journal. 2013:37(2):87–96.
- Thorbert-Mros S, Cassel B, Berglundh T. Age of onset of disease in subjects with severe periodontitis: A 9- to 34-year retrospective study. J Clin Periodontol. 2017;44:778–773.
- Hamp S, Nyman S, Lindhe J. Periodontal treatment of multirooted teeth. Results after 5 years. J Clin Periodontol. 1985;2;126–135.
- Tonetti MS, Christiansen AL, Cortellini P. Vertical subclassification predicts survival of molars with class ii furcation involvement during supportive periodontal care. J Clin Periodontol. 2017;44:1140–1144.
- Tarnow D, Fletcher P. Classification of the vertical component of furcation involvement. J Periodontol. 1984;55:283–284.
From Dimensions of Dental Hygiene. October 2018;16(10):56,58.


Great article, love the reference to the 3 important factors. Adaptation, Angulation & Activation! Always enjoy your articles, thank you!