
Treating Patients After Weight Loss Surgery
While bariatric surgery is effective in reducing the health risks associated with excess weight, it also presents challenges to oral and systemic health.
EDUCATONAL OBJECTIVES
After reading this course, the participant should be able to:
- Discuss the prevalence of obesity and bariatric surgery in the United States.
- Describe potential dental complications following weight loss surgery.
- Identify treatment recommendations to optimize postsurgical oral health care.
As the prevalence of obesity continues to grow in the United States, more people are choosing to undergo bariatric surgery to lose weight and reduce the health risks associated with excess weight.1,2 Post-surgery, patients are at increased risk of systemic and oral complications. They must also adhere to strict dietary changes.1–4 Dental professionals should be prepared to address these side effects, as well as collaborate with other health care professionals to closely monitor the health of these patients.5–7
SURGICAL POSSIBILITIES
Obesity is defined as a body mass index (BMI) equal to or greater than 30 kg/m.2,3 Today, 32.2% of the American adult population is considered obese and 4.8% are classified as morbidly obese (BMI equal or greater to 35 kg/m).8 Over the past few years, bariatric surgery has increased more than 600%, making it one of the most rapidly increasing fields in modern health care.1 There are two main types: restrictive surgery and malabsorption surgery. Restrictive surgery includes gastric banding, vertical banded
gastroplasty, and sleeve gastrectomy. The second and most common—encompassing between 70% and 75% of all bariatric surgeries—is malabsorption surgery known as Roux-en-Y gastric bypass (RYGB) surgery.3,9
During RYGB surgery, a part of the stomach is stapled or banded to create a small stomach pouch. A Y-shaped portion of the small intestine is then attached to the pouch to allow food to bypass the duodenum and first portion of jejunum (Figure 1).1 Bypassing the duodenum leads to mineral malabsorption2– 5,10,11 and permanent alteration of the gastrointestinal tract. RYGB surgery is the most effective weight loss procedure because the restrictive mechanism promotes early satiety and decreases the amount of food ingested,3 while the nonabsorptive component limits nutrient intake to promote weight loss.1 However, RYGB surgery also requires dietary changes that can create negative side effects.3
MALNUTRITION
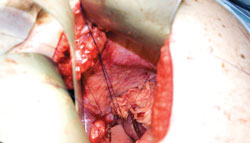
Because the duodenum and proximal jejunum are main absorption sites for most vitamins, their subsequent bypass created by RYGB surgery leads to nutrient deficiencies.2–5,10,11 Protein, iron, calcium, vitamin D, vitamin B12, vitamin A, vitamin K, zinc, and vitamin C are often deficient in patients post-bariatric surgery. 2–5,10,11 These deficiencies can negatively impact the immune system and bone turnover rate, as well as increase the risk of periodontal diseases.
Protein deficiency occurs in 13% to 18% of patients after surgery.11 Common symptoms include brittle hair and hair loss, decrease in pigmentation of hair and scalp, rash and desquamation, lethargy, generalized edema, and delayed healing.12 Protein also plays an important role in the maintenance of bone
structure.9
The incidence of vitamin D deficiency may be as high as 63% in patients 1 year to 4 years post-bariatric surgery.11 Vitamin D is essential for calcium absorption, stimulation of osteoblast activity, and normal bone mineralization. 9 Thus, those with a deficiency are at increased risk of osteoporosis.9 Additionally, studies have correlated calcium deficiency to alveolar bone resorption, which may predispose this population to periodontal disease.13 Vitamin B12 is deficient in 12% to 33% of patients up to 3 years post-surgery.1,11 This deficiency is also associated with the risk of osteoporosis and anemia.11 Oral supplementation alone does not prevent deficiency, and these patients may need subcutaneous or intramuscular injections in order to correct the deficiency.1,3
Vitamin C is frequently deficient among this patient population because it is absorbed in the jejunum. This deficiency can cause delayed healing, and lead to gingivitis and increased
gingival inflammation.14
PERIODONTAL DISEASES
Patients who undergo bariatric surgery and subsequent weight loss experience both positive and negative effects in the periodontium. The immune systems of overweight and obese
people secrete more of the cytokines interleukin-6 (Figure 2) and TNF-alpha (Figure 3), raising their risk of periodontal diseases.15 Patients who have significant weight loss post-surgery experience a decrease in the proinflammatory response and an increase in anti-inflammatory mediators.16 This results in decreased levels of periodontal inflammation. Although more research is needed, this association between bariatric surgery and positive immunological changes indicates that bariatric surgery, along with professional oral health care, may help resolve obesity-related periodontal disease.
Because the nutritional deficiencies experienced post-surgery put bone health at risk, this patient population is vulnerable to periodontal diseases within months of the weight loss procedure.17 This bone loss is attributed to nutrition-related metabolic bone disease, such as osteoporosis.2 In osteoporosis, the bone becomes more porous and susceptible to fracture.18 Healing following dental treatment is negatively impacted by nutritional deficiencies, possibly due to decreased osteoblast activity.10,13 Davies et al found that bone mineral density decreased 4.9% at the hip, 5.7% at the trochanters (part of the femur that connects to the hip), 3% at the neck, and 2.1% throughout the body among patients post-bariatric surgery.11 A correlation has also been found between a decrease in bone mass density at
the hip or spine and tooth loss.7
Vitamin D deficiency can develop in as little as 8 weeks after RYGB surgery, putting bone health at risk. As patients lose weight, their parathyroid hormone levels rise and both calcitonin and 25-hydroxyvitamin D levels decrease. This leads to secondary hyperparathyroidism, 9,10,13 where parathyroid glands become enlarged and hyperactive. Dietary hyperparathyroidism negatively impacts alveolar bone by increasing bone turnover.13 An extremely low level of vitamin D and calcium may trigger removal of calcium from bone, including alveolar bone.12,19 This results in a weakening of the tooth attachment apparatus and possibly tooth loss.19
DENTAL CARIES
After bariatric surgery, patients are instructed to consume three portions of dairy; two portions of meat; and five portions of vegetables, legumes, and fruits every day.3 Because patients eat so frequently, they are at increased risk of plaque accumulation.2 Many patients do not comply with these guidelines and instead consume soft, calorie-dense foods that are easier to digest—raising their risk of dental caries.1,4 As many as 37% of patients post-RYGB surgery consume an increased amount of carbohydrates.
18 Mariscano et al found that 6 months post-surgery, 25% of patients who had undergone bariatric surgery had more decayed teeth than before surgery.17 The predominately carbohydrate diet causes the salivary pH to decrease.4 Xerostomia may also develop due to decreased water consumption, which can
increase caries activity, as well as the risks of periodontal diseases and tooth wear.2
DENTAL EROSION
One of the most common side effects of RYGB surgery is an increase in acidity levels of the mouth due to vomiting and gastro-esophageal reflux disease (GERD).4 After RYGB surgery, 79% of patients reported vomiting as the most frequent symptom,4 with 56% vomiting at least once per week 6 months after surgery.17 This may be caused by the inability of food to pass through the connection between the small stomach pouch and the jejunum.1 Vomiting may also develop in patients who eat too fast, overeat, or inadequately chew food.1,17
Chronic gastric reflux may place the bariatric patient at risk for both medical and dental complications due to inflammation, ulceration, and hyperproliferative changes to the
squamous epithelium of the esophagus, which may increase the risk of gastric and esophageal cancer.2,10 Between the gastric reflux and meal pattern changes, patients are at increased risk of dental erosive lesions.2,4,10,17 As gastric acid flows into the oral cavity, it helps demineralize vulnerable tooth surfaces.4 The decreased pH of the oral environment associated with gastric reflux, in concert with dietary xerostomia, may lead to dental erosive lesions and hypersensitivity.4 Premolars and incisors are the most vulnerable in this patient population, with lesions and pain localized primarily on facial surfaces.4 Close interprofessional collaboration between dental and health care providers throughout recovery can help improve outcomes.
TREATMENT
Patients who have undergone bariatric surgery have special oral health care needs. To reduce the risk of caries, remineralization protocols should be implemented. Dental sealants should be placed in deep pits and fissures that are at risk of decay or incipient lesions. Salivary pH levels should be monitored and neutralized through dietary and chemotherapeutic measures.
To decrease plaque accumulation, patients need to be educated on effective removal methods. Because patients need to eat small meals frequently throughout the day, a prolonged acidic oral environment is created that may be compounded by xerostomia. After a single exposure to sugar, the plaque pH may not return to normal for 3.5 hours or longer.20
Patients, therefore, require frequent counseling to reinforce and ensure plaque control efficiency. The daily use of topical fluorides (over-the-counter or prescription) is extremely helpful in caries protection.21 Fluoride may be delivered in-office and at-home through customized fluoride trays. Calcium phosphate and arginine bicarbonate/calcium carbonate technologies can be used to protect teeth from decay and erosion, to restore minerals, prevent sensitivity, and buffer against acid.22,23 Hypersensitivity can
be addressed with toothpastes containing potassium nitrate or an in-office application of sensitivity gel or fluoride varnish. Xylitol can also help prevent dental caries through biofilm management,24 but it may cause increased gastric gas production, which should be considered with patients who have GERD.25
Many patients who have undergone bariatric surgery are dehydrated due to the decreased gastric capacity.1,2 Patients need to drink 1 cup of fluid over the course of an hour and swallow beverages slowly.12 If the patient experiences xerostomia due to dehydration, dry mouth rinses, salivary substitutes, and moisturizing gels should be considered. Behaviors that reduce saliva, such as the consumption of caffeine, alcohol, and/or marijuana, should be avoided.
The patient’s periodontal condition should dictate post-surgical recare intervals, which are typically every 3 months to 4 months. The use of a daily antimicrobial agent to control
periodontal pathogens and fungal organisms is recommended.26 Probing depths should be taken at every appointment to monitor changes in bone level. Digital dental imaging
should also be used to document health status and educate patients about their oral health status. With visual support tools, patients may be more motivated to adopt oral hygiene improvements. Intraoral and extraoral screening should include monitoring the thyroid and parathyroid and checking for lesions related to xerostomia, low pH, and vomiting. Oral cancer screening, as well as saliva screening for immunoglobulins and electrolytes, pathogenic bacteria, and pH levels, may all be beneficial.
Nutritional support should be considered at every dental visit, along with regular consultations between the dental hygienist and dietitian, so that compatible and consistent dietary plans are implemented and goals are reinforced. By monitoring nutrients presurgically and at periodic intervals post-operatively, physicians will be able to detect malabsorption issues.9 Patients should be advised that vitamin supplementation is required daily.9,12 While weight loss is occurring, calcium and vitamin D supplementation should be recommended to protect the patient’s bones.9 Studies show that vitamin D and calcium supplementation results in reduced alveolar bone loss and gingival inflammation and/or attachment loss.12,19 Calcium supplementation, when combined with magnesium in a 2:1 ratio, increases production of calcitonin, which inhibits osteoclast activity and decreases the risk of bone resorption.12 The intake of magnesium also decreases the risk of secondary hyperparathyroidism.12
Patients’ health histories should be reviewed at each appointment with special attention paid to medication usage and any related side effects. Dental professionals should encourage
patients to receive regular examinations, blood work, and bone scans from their primary care physicians. Blood work is recommended preoperatively,at 3-month to 6-month intervals postoperatively for the first 2 years, and then annually thereafter.27
Dental hygienists can help coordinate and encourage successful networking of allied professionals during all phases of surgical weight loss. Dental hygienists often maintain longstanding
relationships with patients, have access to general and oral health pre-surgical data, can institute early pre-surgical counseling, and provide ongoing monthly support
at 3-month to 4-month intervals.
CONCLUSION
Although RYGB surgery decreases the risk of weight-induced diseases,16 it is not without significant side effects, including those that affect oral health. Although bariatric surgery is being performed more frequently, all of the risks associated with restrictive and malabsorption procedures are still unknown. Both pre- and post-bariatric surgery patients need to be carefully monitored. Patient management presents challenges because of the multitude of overlapping risk factors, however, a multidisciplinary approach—along with preventive oral health care—will increase the likelihood of improved health and quality of life for patients who have undergone bariatric surgery.
ACKNOWLEDGEMENTS
PHOTOGRAPHY: LIFE IN VIEW / SCIENCE PHOTO LIBRARY
FIGURE 2: PASIEKA/SCIENCE PHOTO LIBRARY; FIGURE 3: SCOTT CAMAZINE/SCIENCE PHOTO LIBRARY
REFERENCES
- Shikora S, Kim JJ, Tarnoff, ME. Nutrition and gastrointestinal complications of bariatric surgery. Nutr Clin Pract. 2007;22:29–40.
- de Moura-Grec PG, Marsicano JA, Rodrigues LM, de Carvalho Sales-Peres SH. Alveolar boneloss and periodontal status in a bariatric patient:a brief review and case report. Eur J Gastroenterol Hepatol. 2012;24:84–89.
- Donadelli SP, Junqueira-Franco MVM, deMattos Donadelli CA, et al. Daily vitamin supplementation and hypovitaminosis after obesity surgery. Nutrition. 2012;28:391–396.
- Barbosa CS, Barbério GS, Marques VR, BaldoVde O, Buzalaf MA, Magalhães AC. Dentalmanifestations in bariatric patients: review of literature. J Appl Oral Sci. 2009;17:1–4.
- Lemieux-Charles L, McGuire WL. What do we know about health care team effectiveness? A review of the literature. Med Care Res Rev.2006;63:263–300.
- Rich MW, Beckham V, Wittenberg C, Leven CL,Freedland KE, Carney RM. A multidisciplinary intervention to prevent the readmission of elderly patients with congestive heart failure. NEngl J Med. 1995;333:1190–1195.
- Shine KI. Health care quality and how to achieve it. 2002;77:91–9.
- Wucher H, Ciangura C, Poitou C, Czernichow S.Effects of weight loss on bone status after bariatric surgery: association between adipokines and bone markers. Obes Surg. 2008;18:58–65.
- Williams SE, Cooper K, Richmond B, Schauer P. Perioperative management of bariatric surgery patients: focus on metabolic bone disease. CleveClin J Med. 2008;75:333–338.
- Boyd LD, Moravec LJ. Bariatric surgery and implications for oral health: a case report. J DentHyg. 2011;85:166–176.
- Davies DJ, Baxter JM, Baxter JN. Nutritional deficiencies after bariatric surgery. Obes Surg.2007;17:1150–1158
- Furtado LC. Nutritional management afterRoux-en-Y gastric bypass. Br J Nurs.2010;19:428–436.
- Lü?tfio?lu M, Sakallio?lu U, Sakallio?lu EE,Bari? S, Gü?rgör P. The impact of dietary induced hyperparathyroidism on healthy and diseased periodontia: an experimental study in rats. J Clin Periodontol. 2012;39:264–271.
- Bal BS, Finelli FC, Koch TR. Origins of and recognition of micronutrient deficiencies after gastric bypass surgery. Curr Diab Rep.2011;11:136–41.
- Brandacher G, Winkler C, Aigner F, et al.Bariatric surgery cannot prevent tryptophan depletion due to chronic immune activation inmorbidly obese patients. Obes Surg. 2006;16:541–548.
- Miller GD, Nicklas BJ, Fernandez A. Serial changes in inflammatory biomarkers after Rouxen-Y gastric bypass surgery. Surg Obes Relat Dis.2011;7:618–624.
- Mariscano JA, de Moura-Grec PC, Belarmino,LB, et al. Interfaces between bariatric surgery andoral health: a longitudinal survey. Acta Cir Bras.2011;26(Suppl):79–83.
- Heling I, Sgan-Cohen HD, Itzhaki M, et al.Dental complications following gastric restrictive bariatric surgery. Obes Surg. 2006;16:1131–1134.
- Miley DD, Garcia MN, Hildebolt CF, et al. Crosssectional study of vitamin D and calcium supplementation effects on chronic periodontitis.J Periodontol. 2009;80:1433–1439.
- Kleinberg I, Jenkins GN. The pH of denta lplaques in the different areas of the mouth before and after meals and their relationship to the pH and rate of flow of resting saliva. Ach Oral Biol. 1964;9:493–516.
- Taybos G. The management of xerostomia.Inside Dentistry. Available at:www.dentalaegis.com/id/2009/06/periodontics the-management-of-xerostomia. AccessedDecember 19, 2012.
- Kleinberg I. SensiStat. A new saliva-based composition for simple and effectivet reatment of dentinal sensitivity pain. DentToday. 2002;21:42–47.
- Chow L, Wefel JS. The dynamics of de- and remineralization. Dimensions of DentalHygiene. 2009;7(42):44–46.
- Söderling E, Isokangas P, Pienihäkkinen K,Tenovuo J. Influence of maternal xylitol consumption on acquisition of mutans streptococci by infants. J Dent Res.2000;79:882–887.
- Storey D, Lee A, Bornet F, Brouns F.Gastrointestinal tolerance of erythritol and xylitol ingested in a liquid. Eur J Clin Nutr. 2007;61:349–354.
- DePaolo LG, Spolarich AE. Safety and efficacyof antimicrobial mouthrinses in clinical practice. JDent Hyg. 2007;81(Suppl):13–25.
- Hammer HF. Medical complications ofbariatric surgery: focus on malabsorption and dumping syndrome. Dig Dis. 2012;30:182–186.
From Dimensions of Dental Hygiene. January 2013; 11(1): 52–55.



