 MARKFGD/ISTOCK/GETTY IMAGES PLUS
MARKFGD/ISTOCK/GETTY IMAGES PLUS
The Use of Acupuncture to Ease Musculoskeletal Pain
Evidence supports the effectiveness of this type of traditional Chinese medicine in the management of work-related pain.
The high prevalence of musculoskeletal disorders (MSDs) among oral health professionals is a key barrier to long and rewarding careers. In fact, MSDs are one of the main causes of early retirement from the profession.1 The very nature of dentistry predisposes many clinicians to develop MSDs. While prevention is integral to tackling this problem, for many it is already too late. What should oral health practitioners do if they are already experiencing pain?
In healthcare and, more specifically, the dental field, MSDs are one of the most critical occupational health concerns affecting clinicians.2 The prevalence of chronic musculoskeletal pain among dental hygienists is estimated at 64% to 93%.2 Complementary and alternative medicine therapies, or more recently named complementary health approaches (CHA) by the National Center for Complementary and Alternative Medicine (NCCIH), are practices or products used to treat different conditions and can be helpful in managing chronic MSDs.3 According to the NCCIH, alternative medicines are defined as “using a nonmainstream approach in place of conventional medicine” and are split into two subgroups: natural products or mind and body practices. Acupuncture, massage, chiropractic care, meditation, and yoga are examples of mind and body practices.4 This article focuses on the use of acupuncture to address musculoskeletal pain in oral health professionals.
EFFECTS OF MUSCULOSKELETAL DISORDERS
Pain caused by MSDs may present as a variety of symptoms such as tingling, numbness, swelling, burning, and limited range of motion to the neck and extremities. In turn, these symptoms can cause even the most dedicated oral health professional to miss work. It is estimated that MSDs are responsible for one-third of the sick time taken by dental hygienists.5
MSD pain not only affects the professional lives of healthcare professionals, but also their personal lives. In a 2013 study of dental hygienists, in almost every body region that was examined except the forearm, 312 of the 624 respondents reported that the pain affected their day-to-day life.6 Dental hygienists may be “working through the pain” and intensifying the damage. A 3-year longitudinal study reported that the effects of MSDs begin as early in the career as dental hygiene school.7 Dental hygiene students are far more likely to be impaired by MSDs than students enrolled in other health science programs. When comparing the clinical physical demands of dental hygiene students with other health science majors, dental hygiene students appeared to be at higher risk for MSDs.7 Nondental hygiene health science majors are not subjected to the same type of repetitive movements and static postures. In addition to the direct effects of pain, MSDs can contribute to job dissatisfaction, diminished quality of work, and early burnout.8
![]() ACUPUNCTURE
ACUPUNCTURE
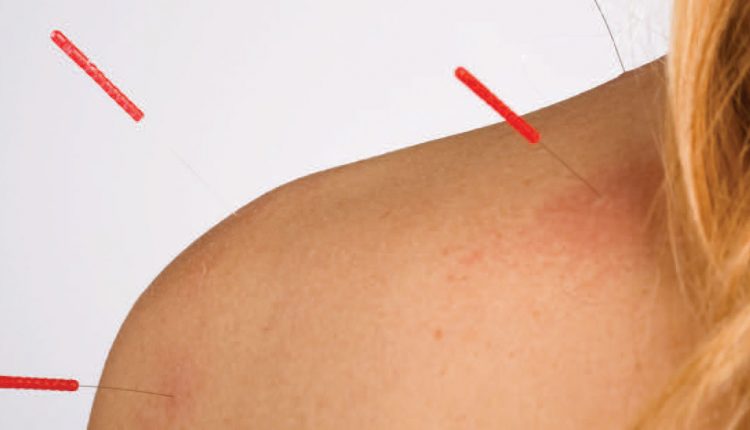
Acupuncture is one of the oldest and most utilized healing treatment systems in the Chinese culture.9 It is considered safe, and most patients experience it as relaxing and calming. The basic principle of acupuncture involves the insertion of thin metal needles into the patient at specific points in the body to alleviate pain and promote general well-being.10 Qi is considered the prominent construct of acupuncture. It refers to energy or “life force” that is essential for healing and health.11 It is believed that pain and illness occur when the flow of qi is blocked. Acupuncture needles are placed in an effort to open qi channels throughout the body and restore health.10
The popularity of acupuncture has been increasing in the West, and is used to treat a variety of issues, such as musculoskeletal pain, headache, cold sensitivity, anxiety, and depression. Sessions typically last from 30 minutes to 40 minutes, and the average course of treatment lasts for 10 sessions.10 The acupuncturist palpates the patient to determine the position of the specific points where the needles will be inserted. While acupuncture charts can serve as a guide for placement, each patient varies in exact point location. These points may also change from session to session as the muscles begin to loosen up.11 During insertion of the needles, the acupuncturist guides them until they are perceived to be grabbed by the tissues or until the patient experiences the sensation known as “de qi.” This term describes a mixture of symptoms including soreness, heaviness, and distention.10 Side effects of acupuncture treatment are typically minor and temporary, and may include needling pain, bruising, hematoma, and dizziness.10,12
Acupuncture is designed to modulate the immune system and the inflammatory response, which may be helpful in resolving inflammation involved in the entrapment of the median nerve in carpal tunnel syndrome. Studies have shown that short-term acupuncture can be more efficacious than ibuprofen in decreasing clinical and electrophysiological symptoms of mild to moderate carpal tunnel syndrome.13 A systematic review and meta-analysis concluded that acupuncture improved chronic low back pain.14
Evidence supports the effectiveness of acupuncture in the treatment of pain, both chronic and acute. The outcomes of acupuncture can be separated into the effects immediately following one treatment or the collective, or cumulative, effects of multiple treatments over time. Current research shows that acupuncture needles can release adenosine when inserted into trigger points.15 This alters fibroblast organization and the free connective tissue layer. Just one treatment with acupuncture can assist in the release of opioid peptides. Immediately following the treatment, the microcirculation in the skin is reduced due to sympathetic nervous system activation, leading to an increase in blood flow to the skin and muscles. Varying durations of cumulative treatments with acupuncture appear to exert differing effects on the brain vs immediate treatment. Cumulative treatments indicate a type of desensitizing response over time, which could play a role in the reduction of chronic pain over multiple treatments.15
What causes patients to pursue acupuncture over allopathic medicine for pain management? One qualitative study from New Zealand found that most people turned to acupuncture when they felt their needs were not being met by conventional healthcare.16 Participants thought their medical providers had only addressed the symptoms but not the true cause of their pain. They also listed the over prescription of pharmaceuticals and concerns of adverse side effects as reasons for seeking out alternative forms of pain management.
Acupuncture is also different from other forms of medicine because of its practitioner/patient collaborative approach. Patients are able to support their treatment between sessions by applying moist heat to the area being treated and performing daily stretches.11 Chan et al9 noted that the bond developed between patients and their acupuncturists is an important part of the healing process. If patients were not happy with their acupuncturist, they were often not satisfied with the results of their treatment.9
DENTAL APPLICATION
Dental hygienists are more likely to use CHAs than the general public (80.7% vs 38.3%).17 This is likely due to the high percentage of oral health professionals who experience work-related chronic pain and must manage that pain in order to be efficient employees. Acupuncture is perceived as effective for pain control with fewer side effects.9
In a study on the use of CHAs for work-related pain among dental hygienists, 84% of the participants used acupuncture for conditions, such as musculoskeletal pain, and reported significant decreases in chronic lower back pain.17 Those who solely used CHAs, such as acupuncture, were more likely to report satisfaction with their careers than those who used more conventional therapies. Another study showed the use of acupuncture was beneficial for the treatment of carpal tunnel syndrome, a common ailment among dental hygienists, by way of immune modulators and anti-inflammatory effects in the entrapped median nerve in the carpal tunnel.13
CONCLUSION
MSDs present a significant burden to oral health professionals. The high prevalence of MSDs among this population warrants concern not only for occupational health but also for career longevity. Acupuncture could be considered a viable treatment option for oral health professionals experiencing pain, as it targets specific muscle group instead of just providing symptom relief.
REFERENCES
- Valachi B. Practice Dentistry Pain-Free. Portland, Oregon: Posturedontics Press; 2008.
- Hayes M, Cockrell D, Smith DR. A systematic review of musculoskeletal disorders among dental professionals. Int J Dent Hyg. 2009;73:159–165.
- Chismark A, Asher GN, Stein MB, Tavoc T, Curran AE. Use of complementary and alternative medicine for work-related pain correlates with career satisfaction among dental hygienists. J Dent Hyg. 2011;8:273–284.
- Chismark AM, Hung AW. Complementary health approaches to reduce musculoskeletal pain. Journal of the California Dental Hygienists’ Association. 2015;33(1):19–22.
- Humann P, Rowe DJ. Relationship of musculoskeletal disorder pain to patterns of clinical care in California Dental Hygienists. J Dent Hyg. 2015;89:305–312.
- Hayes MJ, Smith DR, Taylor JA. Musculoskeletal disorders and symptom severity among Australian dental hygienists. BMC Research Notes. 2013:250.
- Hayes MJ, Smith DR, Taylor JA. Musculoskeletal disorders in a 3 year longitudinal cohort of dental hygiene students. J Dent Hyg. 2014;88:36.
- Lietz J, Kozak A, Nienhaus A. Prevalence and occupational risk factors of musculoskeletal diseases and pain among dental professionals in Western countries: a systematic literature review and meta analysis. PLoS One. 2018;13:e0208628.
- Chan K, Siu JY, Fung TKF. (2016). Perception of acupuncture among users and nonusers: a qualitative study. Health Mark Q. 2016;33:78–93.
- Staykova-Pirovska Y, Despotova-Toleva L. Acupuncture and some common diseases in general practice. Available at: http://tru.uni-sz.bg/tsj/Vol.14,%20N%204,%202016/Y.Pirovska.pdf. Accessed August 24, 2020.
- Finando S, Finando D. An introduction to classical fascia acupuncture. Available at: heightshealthcare.com/An_Introduction_to_Classical_Fascia_Acupuncture_1_.pdf. Accessed August 24, 2020.
- Chung A, Bui L, Mills E. Adverse effects of acupuncture. Can Fam Physician. 2003;49:985–989.
- Ural FG, Ozuturk GT. The acupuncture effect on median nerve morphology in patients with carpal tunnel syndrome: an ultrasonographic study. Available at: http://search.pedro.org.au/ search-results/record-detail/50812. Accessed August 24, 2020.
- Xiang A, Cheng K, Shen X, Xu P, Liu S. The immediate analgesic effect of acupunture for pain: a systematic review and meta-analysis. Evid Based Complement Alternat Med. 2017;2017:3837194.
- Kim SY, Min S, Lee H, et al. Changes of local blood flow in response to acupuncture stimulation: a systematic review. Evid Based Complement Alternat Med. 2016;2016:9874207.
- Jakes D, Kirk R. How and why patients use acupuncture: an interpretive phenomenological study. J Prim Health Care. 2015;1;7:124–129.
- Chismark A, Asher GN, Stein MB, Tavoc T, Curran AE. Use of complementary and alternative medicine for work-related pain correlates with career satisfaction among dental hygienists. J Dent Hyg. 2011;85:273–284.
From Dimensions of Dental Hygiene. September 2020;18(8):22-25.

 ACUPUNCTURE
ACUPUNCTURE